* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Relative Afferent Pupillary Defect (RAPD)
Visual impairment wikipedia , lookup
Fundus photography wikipedia , lookup
Vision therapy wikipedia , lookup
Eyeglass prescription wikipedia , lookup
Photoreceptor cell wikipedia , lookup
Retinitis pigmentosa wikipedia , lookup
Dry eye syndrome wikipedia , lookup
Blast-related ocular trauma wikipedia , lookup
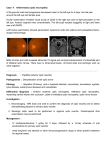
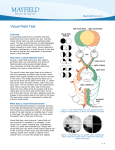
Relative Afferent Pupillary Defect (RAPD) This document is based on the handout from the “Medicine for Finals” course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations. They will complement more detailed descriptions and are not intended to be comprehensive. Most medical students and junior doctors find eyes generally difficult. There are two useful starting points that can make things easier. One is to have a standard scheme for “examine the eyes”. The second is to be familiar with the signs of optic neuropathy. When you have read these notes, have a look at the video demonstration of an afferent pupillary defect. Examine the eyes • Inspection • Visual acuity (monocular for each eye) • Fields • External ocular movements • Fundi • Pupils (brightest light last) including swinging torch test Remember to check visual acuity separately in each eye. If the acuity is reduced, re-check using a pinhole, which corrects for refractive errors. Because a pinhole reduces the amount of light reaching the eye, the object needs to be well illuminated. Further details of visual field testing, external ocular movements and fundoscopy are included in the notes on Neurology. Optic neuropathy: signs • Pale disc • Loss of visual acuity • Loss of red colour vision • Central scotoma • Afferent pupillary defect (the Marcus Gunn pupil) This is a useful list to remember. If you are asked to perform fundoscopy, and there seems to be no obvious abnormality, consider the following three possibilities: a) normal fundi b) pan-retinal photocoagulation- the scars from this are often peripheral and can be missed quite easily c) optic atrophy- the pallor of one disc can be subtle It is always worth comparing one side with the other to see if one disc is paler than the other. If you are in doubt, try “I wonder if one disc is a little pale and would like to check for the other signs of optic neuropathy”. This then gives the examiner the opportunity to ask you about the other signs, which you can then discuss fluently if you know this list. Patients with acute optic neuropathy often notice that colour vision is changed through the affected eye- “things look greeny-blue”. Red colour fibres are the first affected, which is why a red hatpin is most sensitive for testing the central part of the visual fields. Dr R Clarke www.askdoctorclarke.com 1 Swinging torch test • In the good eye, light causes constriction and this is consensual • Release of stimulus from good eye causes dilatation- also consensual • Light in "bad" eye is a weak stimulus: there is a relative afferent defect • Release of the stimulus from the good eye acts consensually causing dilatation of the pupil on the bad (affected) side • It competes with weak afferent stimulus • The result is dilatation of the pupil to light on the affected side It is sometimes hard to know why anyone ever shines a light in a patient’s eyes without doing the swinging torch test. Routinely saying that the pupils react to light is probably a hangover from the days when tertiary syphilis was commoner and it was important to check for Argyll Robertson pupils. These are small, irregular and with a poor response to light, but some response to accommodation (“like a prostitute, will accommodate but not respond”). These days the only situations where shining a light in a patient’s eyes (without the swinging torch test) is helpful is either to confirm death or after a serious head injury: in both of these, you are testing the efferent pathway- parasympathetic fibres from the Edinger Westphal nucleus which hitch-hike with the third nerve and which make the pupil constrict. In live patients, pupil size is related to tonic parasympathetic constrictor tone. When dead, this is lost and the pupils are “fixed and dilated”. With head injury and rising intracranial pressure causing herniation through the tentorium, the long third nerve can be easily stretched- effectively causing a third nerve palsy. This may well be a false localising sign as the primary problem may be away from the anatomical pathway of the third nerve. Loss of papillary constriction may be one of the earliest signs. In patients without head injury, the swinging torch test is the key to detecting problems with the optic nerve ie an afferent defect. The same pupillary response may be observed with chronic glaucoma- where raised pressure damages the optic nerve head (the weak spot in the eyeball). Fundocopy in chronic glaucoma will usually reveal enlargement of the optic cup, not the pale atrophic disc of optic atrophy. Optic atrophy: causes • Demyelination • Trauma • Compression eg pituitary tumour or meningioma • Diabetes • Toxic eg methanol • Secondary to papilloedema Dr R Clarke www.askdoctorclarke.com 2 O ptic neuropathy: term inology O ptic neuropathy O ptic neuritis R etrobulbar neuritis (fundus initially norm al) B ulbar neuritis P apillitis O ptic neuritis with P apilloedem a S ix weeks later O ptic atrophy P rim ary optic atrophy With demyelinating disease, optic neuropathy is a relatively common presentation. The eye is often painful and the patient complains of blurred vision in the affected eye, particularly centrally- “like looking through the bottom of a beer glass”. Red colour vision is lost early- so the world looks bluer through the affected eye. About 80% have retrobulbar neuritis- where initial examination of the fundus is normal. The remaining 20% have a demyelinating plaque right at the front of the optic nerve: this gives the appearance of papilloedema. After about 6 weeks, patients will have recovered most, but not all, of their vision and fundoscopy will then reveal a pale disc- optic atrophy. Sometimes this is called primary optic atrophy- due to a primary problem with the nerve, rather than secondary to papilloedema or tertiary, in association with disease of the retina. Dr R Clarke www.askdoctorclarke.com 3