* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download PDF
Survey
Document related concepts
Transcript
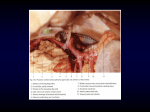
Hindbrain Stroke in Children Caused by Extracranial Vertebral Artery Trauma BY RICHARD A. R. FRASER, M.D., F.R.C.S.(C),* AND SEYMOUR M. ZIMBLER, M.D., F.A.C.S.t Abstract: Hindbrain Stroke in Children Caused by Extracranial Vertebral Artery Trauma • Hindbrain transient ischemic attacks (TIAs) culminating in posterior circulation stroke are described in five children. Atlanto-axial subluxation and angiographical documentation of Cl to C2 level arterial pathology are documented in one patient. Four additional patients with nearly identical clinical presentations, posterior fossa TIAs, stroke and basilar angiographical pathology are reviewed. A mechanical traumatic etiology is suggested. Unexplained transient repeated brain stem and/or cerebellar symptomatology may be due to extracranial vertebral artery stenosis or occlusion by atlanto-axial instability. After appropriate documentation, stabilization may prevent further TIAs or strokes. Additional Key Words vertebrobasilar occlusion Downloaded from http://stroke.ahajournals.org/ by guest on June 15, 2017 DFor many years, neurosurgeons and neurologists, when evaluating patients with cervical spine trauma or congenital anomalies of the cervical spine, have emphasized the direct compressive effects of such lesions on the cervical spinal cord. Occasional patients with cervical spine trauma and injury to the vertebral arteries with subsequent brain stem and cerebellar dysfunction have been reported. 16 All of these patients have been adults. Additional patients have had posterior fossa stroke symptoms following chiropractic cervical spine manipulation. 716 Occlusive cerebrovascular disease in children is uncommon. The overwhelming majority of such patients display lesions in the carotid circulation.17 Only seven children have been reported previously with disease in the posterior cerebral circulation. 1821 Septic emboli occurred in two, while no clearly defined etiology could be identified in the remaining five (table 1). We wish to describe an additional patient, a sixyear-old boy with a history of vertebrobasilar TIAs, which culminated in a major posterior circulation stroke. Cervical spine x-rays and angiographical data lead us to suggest that the cerebrovascular accident in this patient was the result of atlanto-axial subluxation, traumatic deformation of the vertebral arteries and distal embolization to the basilar artery. Clinical and angiographical similarities in other patients suggest a common syndrome. From the * Department of Neurological Surgery, the New York Hospital-Cornell Medical Center, 525 East 68th Street, New York, New York 10021. tDepartment of Orthopedics, Tufts-New England Medical Center Hospital, 171 Harrison Avenue, Boston, Massachusetts 02111. Stroke, Vol. 6, March-April 1975 transient ischemic attack atlanto-axial subluxation extracranial cerebrovascular disease cervical fusion Case Report A six-year-old right-handed boy was first admitted to the Boston Floating Hospital because of gait ataxia and clumsiness of the right upper extremity. During the previous month, he had experienced intermittent nausea, headache, frequent vomiting, dysarthric speech, and clumsiness of the right upper extremity. These symptoms would appear for a day, improve spontaneously, and reappear two to three days later. Because of these symptoms, he had been admitted to another hospital where neurological examination, EEG, brain scan, skull x-rays, and CSF formula were reported as normal. At the time of admission to the Boston Floating Hospital, examination revealed a mild deficit with minor clumsiness of the right hand, bradykinesia, and slow speech. The diagnoses suggested included cerebellar ataxia of infectious or postinfectious etiology. A brain scan (technetium 99) was normal. Skull x-rays on this admission were reported as normal, but closer examination revealed nonfusion of the odontoid and anterior displacement of Cl on C2. While this finding was noted and confirmed on cervical spine tomograms (fig. 1) and flexion and extension films (figs. 2 and 3), its significance and relationship to the current illness were not appreciated and the patient was discharged without cervical stabilization. One day following discharge, the patient awoke with a mild right hemiparesis which, over the ensuing six hours, evolved into a flaccid hemiplegia and prompted his readmission to the Boston Floating Hospital. His parents stated that he had fallen from bed the night before. Examination on the second admission confirmed severely dysarthric speech, inability to gaze to the left of the midline, nystagmus on right lateral gaze, lower motor neuron weakness of the left face, and a virtually complete right hemiplegia. Deep tendon reflexes were absent in the right extremities and a right-sided extensor plantar response was elicited. Dysmetria was apparent in the left upper extremity. Laboratory studies, including hemogram, white blood count, serum electrolytes, and urinalysis, were normal. 153 Downloaded from http://stroke.ahajournals.org/ by guest on June 15, 2017 Not reported Not reported Sudden coma following severe bums and septicemia Two months' intermittent vertigo, ataxia, sudden right hemiparesis, left cerebellar deficit Three months' intermittent vertigo, Not reported fall with occipital fracture one month prior —diplopia, bilateral cerebellar deficit 6 yr, M 7yr, M 18 mo, F 4yr, M 9 yr, M 14 yr, M Dooley et al.19 Fowler20 Fowler20 Ouvrier and Hopkins21 Ouvrier and Hopkins21 Ouvrier and Hopkins21 Coarctation aorta, septicemia, endocarditis, sudden right hemiparesis Sudden coma, decerebrotion without antecedent illness or trauma Not reported Normal Two months' intermittent ataxia, Not reported vertigo, vomiting, transient left hemiparesis, left cerebellar deficit, "jarred" in auto accident eight months previously Eight months' intermittent Normal diplopia, vertigo, followed by sudden right sensory motor disturbance, ataxia, anisocoria 9yr, M Cervical spine x-rays C1-C2 subluxation DeVivo and Farrell18 Clinical presentation One-month transient intermittent vomiting, dysarthria, ataxia, sudden right hemiplegia 6 yr, M Age/<ex Present case Reference Childhood Vertebrobasilar Arfery Occlusion TABLE 1 Terminal basilar artery occlusion Severe dementia, hemiparesis Septic Mechanical? Moderate dysarthria and cerebellar deficit C2 stenosis left vertebral; terminal basilar artery Septic Unknown Mechanical? Died Died Mechanical? Mechanical? Mechanical deformation; probable thrombotic embolus to basilar artery Etiology C1-C2 left vertebral; Severe left C4 stenosis right cerebellar vertebral deficit Distal basilar artery Posterior cerebral artery occlusion C2 stenosis left Horner's syndrome vertebral; right and cerebellar vertebral occlusion deficit of the foramen magnum; basilar and (eft posterior cerebral Right brachial dysmefria C1-C2 occlusion left vertebral; right vertebral "kinked" at C2; left posterior cerebral artery occlusion Result Right hemiparesis, C1-C3 fused Arteriography C1-C2 occlusion left vertebral artery, partial right basilar artery S N HINDBRAIN STROKE IN CHILDREN Downloaded from http://stroke.ahajournals.org/ by guest on June 15, 2017 FIOUII1 Tomogram Cl toC2. Un-united odontoid immediately posterior to arch of Cl. HOSPITAL COURSE The following day, four-vessel angiography was performed, prompted by a diagnostic impression of "arteritis." The presence of atlanto-axial subluxation was not communicated to the neuroradiologist so that the study was performed in the usual hyperflexed position, causing maximum anterior displacement of the atlas. The arteriogram revealed occlusion of the right vertebral artery at the level of C2. Collateral vessels were seen at this level bypassing the occluded portion of the vertebral artery and rejoining the vessel at the rostral border of C2. The right vertebral artery terminated in the posterior inferior cerebellar artery without opacification of the basilar artery (fig. 4). The left vertebral artery demonstrated aneurysmal dilatation at C2. This vessel also terminated in the posterior inferior cerebellar artery without filling of the basilar artery (fig. 5). Carotid injections opacified the rostral tip of the basilar artery and both superior cerebellar arteries and posterior cerebral arteries. Neurosurgical consultation was again requested. It was our impression that the arterial pathology revealed by angiography was the result of mechanical trauma to each vertebral artery as it crossed the transverse foramen of C2. The occlusion of the right vertebral artery and the aneurysmal dilatation of the left was thought to result from chronic intermittent mechanical trauma and stretching of each vessel by the anterior displacement of Cl upon C2. A presumptive diagnosis of a posterior circulation stroke was suggested. It was decided to stabilize the patient externally in halotraction and await maturation of his neurological deficit. One week after admission, he was able to flex and extend the right leg against gravity and demonstrated a flicker of movement in the right toes. Functional improvement occurred in conjunction with active physiotherapy. Strok; Vol. 6. March-April 1975 FlOUtll Cervical spine —flexion Anterior displacement of Cl and united odontoid process. Neurological improvement continued for another four weeks, at which time the patient was ambulatory with a right leg brace and demonstrated proximal movement against gravity in the right upper extremity. The right hand, however, remained plegic. Eye movements were normal. Four-vessel angiography was repeated at this time and revealed no change in the vertebral artery anomalies. These films did demonstrate, however, that the basilar artery had recanalized with filling of the superior cerebellar and posterior cerebral arteries from the posterior circulation. Slight narrowing of the distal basilar artery just proximal to the origin of the superior cerebellar arteries remained (figs. 6 and 7). At this time, a cervical spine fusion of Cl to C3 using wire and iliac bone was performed. The patient was discharged on the tenth postoperative day after an uneventful convalescence. Follow-up at three months revealed little improvement with persistent severe right hemiparesis, most marked in the right upper extremity. Discussion Only seven children have been previously reported with occlusive or stenotic pathology of the vertebrobasilar system.18"21 Review of the case material (table 1) reveals that in five of these patients 15S FRASER, ZIMBLER t f Downloaded from http://stroke.ahajournals.org/ by guest on June 15, 2017 FIOUII4 noun 3 Right vertebral angiogram — lateral view. Occlusion of vertebral artery at C2. collateral supply to Cl segment with distal vertebral filling but termination in the posterior inferior cerebellar artery (PICA). Cervical spine — extension Normal allanlo-axial relationships restored. Distal un-united odontoid has undergone counterclockwise rotation no apparent cause for the vascular pathology could be assigned and all were designated as either a congenital or idiopathic disorder. The remaining two patients had septicemia and obvious septic emboli to many vessels, including the intracranial circulation. Closer attention to this table reveals that four of the remaining five presented with syndromes strikingly similar to the present case. All were male. Intermittent attacks of vertigo, ataxia, and sensory motor disturbances, presumably posterior circulation TIAs, were followed after weeks or months by a sudden stroke-like syndrome of hemiparesis and ataxia. In case 4, a severe fall and a documented occipital fracture preceded the permanent stroke-like syndrome by a month. There was no antecedent trauma in case 3 or 5, but the patient described in case 7 experienced the onset of sudden hemiparesis while walking home from baseball practice where cervical trauma might have occurred. In each of these patients, arteriography revealed stenosis or occlusion of the vertebral arteries of one or both sides at the level of the second cervical vertebra. In addition, incomplete filling of the basilar artery was 156 Left vertebral angiogram — lateral view. Dilatation of vertebral artery at C2. Vessel terminates in left PICA. No filling of basilar artery. S l r o t ; Vol. 6, March-April 1975 HINDBRAIN STROKE IN CHILDREN "V \ Downloaded from http://stroke.ahajournals.org/ by guest on June 15, 2017 i FIOURI 7 Right vertebral angwgram four weeks later — lateral view. Vertebral artery unchanged Basilar artery now opacified, but narrow. Marked stenosis ofbasilar artery just proximal to origin of superior cerebellar artery. present in three. Cervical spine films were normal in one case and not described in the remaining three. These patients all survived with minor to moderate cerebellar and brain stem deficits. It seems apparent that our case is a clear example of a posterior circulation stroke. Serial angiograms revealed an occluded basilar artery which later recanalized concomitant with minor improvement in the patient's neurological deficit. (Anticoagulants were not administered at any time.) We believe that the most reasonable explanation for this vertebrobasilar arterial lesion is traumatic and that repeated anterior subluxation of Cl on C2 caused mechanical deformation and occlusion of both vertebral arteries. Thrombus formation in the deformed vertebral arteries with distal embolization into the basilar artery presumably caused the stroke in our patient. Though no mention was made of cervical spine anomalies in four previously reported patients with almost identical findings, we wonder whether a similar mechanism was playing an etiological role. It is possible, even in the absence of bony anomalies, that mechanical distortion of the vertebral arteries may result from subluxation secondary to laxity of the ligaments connecting the atlas and axis. In Slrok: Vol. 6, March-April 1975 Left vertebral angiogram four weeks later — lateral view. Vertebral dilatation at C2 unchanged Basilar artery now fills tortuously with right vertebral injection. this instance, no radiographical changes would be apparent except on flexion and extension films. Atlanto-axial subluxation with non-union of the odontoid is a frequent congenital anomaly of the spinal column. Previous series of patients with atlanto-axial anomalies do not contain a single example of angiographically documented vertebrobasilar pathology." 2 * Ford2 has described a 17-year-old boy similar to the case reported here. Recurrent posterior circulation TIAs were eventually diagnosed after atlanto-axial instability was discovered and treated by cervical fusion. Unfortunately, this case lacks angiographical documentation. The patient's symptoms were recurrent, transient, and closely resembling those reviewed above; they seem a convincing, if not proved, example of this syndrome. Several patients presenting with brain stem and/or cerebellar deficits due to stroke have been reported following cervical spine trauma1"*' w and an even larger number following chiropractic neck manipulation. 719 In two patients of the latter group, angiography confirmed vertebral artery lesions at the level of the axis,11 similar to those described above. Schneider and Crosby3 have suggested that the vertebral arteries are especially vulnerable to compression at three sites: (1) at any fracture dislocation above C6, (2) at the atlanto-axial level with Cl to C2 compression, and (3) at Cl because of atlanto-axial 1975 FRASER, ZIMBLER Downloaded from http://stroke.ahajournals.org/ by guest on June 15, 2017 dislocation resulting from the occipital condyles sliding forward over the articular facets of Cl. Arteriograms in the present case, in two post-neck manipulation cases,12 and in four children without antecedent trauma18'19'21 revealed similar Cl to C2 arterial pathology, and confirm the potential vulnerability of the vertebral artery at this level. Our patient was treated by fusion of the first three cervical vertebrae when his neurological condition stabilized. This procedure seemed warranted to prevent future additional mechanical trauma to the vertebral arteries and further posterior circulation strokes. Potential cervical cord compression was also prevented. A recent report attempts to define angiographically prognostic indicators in patients with basilar artery occlusion.30 These authors point out that such patients present in two ways: (1) with abrupt onset of coma, often leading to death, or (2) with transient symptoms of brain stem ischemia. The latter patients are a diagnostic problem. These authors also suggest, not surprisingly, that small or absent collaterals from the anterior circulation carry a poor prognosis. Basilar artery occlusion has been regarded in the past as nearly always fatal.31 More recent reports,30'32 however, suggest that survival is the rule. Increased awareness of the syndrome described in this report might lead to documentation of similar pathology in patients with otherwise unexplained repeated transient brain stem and cerebellar symptomatology. Appropriate x-ray studies, including flexion and extension cervical spine films and vertebral angiography, are urged in such cases. These patients represent an additional syndrome of extracranial occlusive cerebrovascular disease, one in which surgical stabilization provides appropriate therapy and removes further risk of stroke. Summary A patient is described with bilateral vertebral artery anomalies at Cl to C2, with occlusion of the basilar artery occurring in conjunction with a posterior circulation stroke. The anomalies are believed to be the result of chronic and repeated atlanto-axial subluxation. Review of the literature provides four previous patients with strikingly similar clinical presentations. All were male and all presented with intermittent symptoms suggestive of brain stem and/or cerebellar dysfunction. All were retrospectively diagnosed as experiencing posterior cerebral circulation transient ischemic attacks, which culminated in a stroke with varying degrees of static neurological deficit. Patients with severe atlanto-axial instability are at risk for posterior circulation injury and possible brain stem stroke. Vertebral artery angiography should be considered in such patients. 158 References 1. Carpenter S: Injury of neck as cause of vertebral artery thrombosis. J Neurosurg 18:849-853, 1961 2. Ford FR: Syncope, vertigo, and disturbances of vision resulting from intermittent obstruction of the vertebral arteries due to defect in the odontoid process and excessive mobility of the second cervical vertebra. Bull Johns Hopkins Hosp 91:168-173, 1952 3. Schneider RC, Crosby EC: Vascular insufficiency of brain stem and spinal cord in spinal trauma. Neurology 9:643656, 1959 4. Schneider RC, Schemm GW: Vertebral artery insufficiency in acute and chronic spinal trauma. J Neurosurg 1 8:348-360, 1961 5. Simeone FW, Goldberg HI: Thrombosis of vertebral artery from hyperextension injury to the neck. J Neurosurg 29:540554, 1968 6. Svechting Rt, French LA: Posterior inferior cerebellar artery syndrome following fracture of cervical vertebra. J Neurosurg 12:187-189, 1955 7. Blaine ES-. Manipulative (chiropractic) dislocations of atlas. JAMA 85:1356-1359, 1925 8. Ford FR, Clark D: Thrombosis of the basilar artery with softenings in the cerebellum and brain stem due to manipulation of the neck. A report of two cases with one post-mortem examination. Reasons are given to prove that damage to the vertebral arteries is responsible. Bull Johns Hopkins Hosp 98:37-42, 1956 9. Green D, Joynt RJ: Vascular accidents to brain stem associated with neck manipulation. JAMA 170:522-524, 1959 10. Kunkle EC, Muller JC, Odom PL: Traumatic brain stem thrombosis: Report of a case and analysis of mechanism of injury. Ann Int Med 36:1329-1335, 1952 11. Lyness SS, Wogman AD: Neurological deficit following surgical manipulation. Surg Neurol 2:121-124, 1974 12. Mahalic T, Farhat SM: Vertebral artery injury after chiropractic manipulation of the neck. Surg Neurol 2:125129, 1974 13. Pratt-Thomas HR, Berger KE: Cerebellar and spinal injuries after chiropractic manipulation. JAMA 133:600-603, 1945 14. Pubek RA: Brain stem vascular accident following neck manipulation. Wis Med J 62:141-143, 1963 15. Schwarz GA, Geiger JK, Spano AV: Posterior inferior cerebellar artery syndrome of Wallenberg after chiropractic manipulation. Arch Int Med 97:352-354, 1956 16. Smith RA, Estridge MN: Neurologic complications of head and neck manipulations: Report of two cases. JAMA 182:528-531, 1962 17. Banker BQ: Cerebral vascular disease in infancy and childhood. J Neuropath Exp Neurol 20:127-140, 1961 18. DeVivo DC, Farrell FW Jr: Vertebrobasilar occlusive disease in children: A recognizable clinical entity. Arch Neurol 26:278-281, 1972 19. Dooley JM, Smith KR: Occlusion of the basilar artery in a 6year-old boy. Neurology 18:1034-1036, 1968 20. Fowler M: Two cases of basilar artery occlusion in childhood. Arch Dis Child 37:78-81, 1962 21. Ouvrier RA, Hopkins IJ: Occlusive disease of the vertebral basilar arterial system in childhood. Dev Med Child Neurol 12:186-192, 1970 22. Bull JM: The syndrome of atlanto-axial dislocation. Clin Proc 1:336-345, 1942 23. Dunbar HS, Ray BS: Chronic atlanto-axial dislocations with Stroke, Vol. 6, March-April 1975 HINDBRAIN STROKE IN CHILDREN 24. 25. 26. 27. late neurological manifestations. Surg Gynec Obstet 113:757-762, 1961 Garber JN: Abnormalities of the atlas and axis vertebrae — congenital and traumatic. J Bone Joint Surg 4 6 A : 17821791, 1964 MacCrae DL: Bony abnormalities in the region of the foramen magnum: Correlations of the anatomic and neurological findings. Acta Radiol 40:335-354, 1953 Paradis GR, Janes JM: Post traumatic atlanto-axial instability: The fate of the odontoid process fracture in 46 cases. J Trauma 13:359-367, 1973 Roberts A, Wickstrom J: Prognosis of odontoid fractures. Acta Orthop Scand 44:21-30, 1973 28. Shatzker J, Rorabeck CH, Daddell JP: Fractures of the dens (odontoid process). An analysis of 37 cases. J Bone Joint Surg 53B:392-404, 1971 29. Nagler W: Vertebral artery obstruction by hyperextension of the neck: Report of 3 cases. Arch Phys Med Rehab 54:237240, 1973 30. Moscow NP, Newton TH: Angiographic implications in diagnosis and prognosis of basilar artery occlusion. Amer J Roentgen 119:597-604, 1973 31. Kubik CS, Adams RD: Occlusion of the basilar artery: A clinical study. Brain 69:6-15, 1946 32. Fields WS, Ratinor G, Weibel J, et al: Survival following basilar artery occlusion. Arch Neurol 15:463-471, 1966 Downloaded from http://stroke.ahajournals.org/ by guest on June 15, 2017 Stroke, Vol. 6, March-April 1975 159 Hindbrain Stroke in Children Caused by Extracranial Vertebral Artery Trauma RICHARD A. R. FRASER and SEYMOUR M. ZIMBLER Downloaded from http://stroke.ahajournals.org/ by guest on June 15, 2017 Stroke. 1975;6:153-159 doi: 10.1161/01.STR.6.2.153 Stroke is published by the American Heart Association, 7272 Greenville Avenue, Dallas, TX 75231 Copyright © 1975 American Heart Association, Inc. All rights reserved. Print ISSN: 0039-2499. Online ISSN: 1524-4628 The online version of this article, along with updated information and services, is located on the World Wide Web at: http://stroke.ahajournals.org/content/6/2/153 Permissions: Requests for permissions to reproduce figures, tables, or portions of articles originally published in Stroke can be obtained via RightsLink, a service of the Copyright Clearance Center, not the Editorial Office. Once the online version of the published article for which permission is being requested is located, click Request Permissions in the middle column of the Web page under Services. Further information about this process is available in the Permissions and Rights Question and Answer document. Reprints: Information about reprints can be found online at: http://www.lww.com/reprints Subscriptions: Information about subscribing to Stroke is online at: http://stroke.ahajournals.org//subscriptions/