* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download High values
Compartmental models in epidemiology wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Focal infection theory wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Public health genomics wikipedia , lookup
Infection control wikipedia , lookup
Prenatal testing wikipedia , lookup
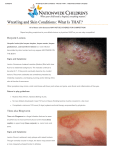
Prof. Elsanousi M Taher BDS, M.Sc., FFDRCSI LIMU SPECIAL TESTS AND LABORATORY INVESTIGATION IN ORAL DIAGNOSOS Why we investigate? For the sake our of the patient To To To To confirm diagnosis exclude a disease or condition manage a patient reassure patient Inadequate diagnosis may lead to: Missed diagnosis Misdiagnosis Bad practice Legal action Superfluous or unnecessary investigations can be: Time consuming Expensive Occasionally Cause dangerous undue anxiety The staff should explain to the patient in simple terms the relevance of investigations he/she asked for For most investigations, there is a normal range 95 % of normal people fit into this range while 5%, though normal, but are out of this range If the results are very different from what is expected and not going with clinical impression, check validity Always Give summary of clinical details to Lab staff Obtain Patient consent Types of investigations: Vitality tests Radiology Hematology Urinalysis Microbiology Biochemistry Immunology or serology Histopathology Teeth Vitality tests/ sensitivity tests: Are used to determine weather the pulp of the tooth is vital or not The tests are not always reliable The results should be evaluated with other findings and symptoms The tooth to be tested should be completely dry and isolated so that the possibility of conduction of stimulus to nerves of gingiva, periodontal ligament is minimized Methods Heat test: application of hot gutta percha to the incisal edge or buccal (cervical area) surface of the tooth Cold test application of ice or ethyl chloride sprayed on a cotton pellet Electrical pulp testing: Preparation of test cavity: when other tests give inconclusive results For more details about the pulp vitality investigation please go back to orofacial pain lecture on semester six Caries activity tests: these tests demonstrate: Caries activity Lactobacillus count Effect of preventive measures commonly used tests are: Snyder test Lactobacillus count Salivary buffer test For more details go the cariology course, preventive course and diagnosis of dental caries in 4th, 5th and 6th semester RADIOLOGY INVESTIGATIONS Imaging techniques: Radiographs: intra-oral Periapical Bitewing occlusal The following points should be observed on interpreting intraoral radiographs: Lamina dura continuity and thickness Periodontal ligament: variation in width Level of alveolar crest Teeth pathology or developmental defects Pulp size and degree of pulp calcification if present Periapical radiolucency Existing restoration Location of calculus Pathological conditions of the jaws Other dental findings Extra-oral: required in the following cases: Suspected bone fracture Suspected salivary calculus To see the extent of a lesion To know the exact location of a lesion, tooth or foreign body Inability to tolerate intraoral films TMJ disorder General jaw screening Extra-oral plain radiographs: Panoramic Lateral Skull projections Facial MJ oblique projections projections Tomography: Computer CT assisting imaging: scan Magnetic resonance imaging Sonography HISTOPATHOLOGY Biopsy: is the surgical removal of living tissue for the purpose of microscopic examination Indications: non healing lesion that fail to respond to treatment Ulcer Extraction socket Gingival tissue Periapical tissue any lesion suspected of being neoplastic or potentially malignant: Leukoplakia Erythroplakia Lump Continue indications for biopsy any surgically excised tissue any tissue spontaneously expelled from the body an intraosseous lesion that that can not be positively identified radiographically Confirmation of some clinical diagnosis: Carcinomas and other malignant lesion Vesiculo-bullous lesions LP Sjögren’s syndrome chronic granulomatous diseases(TB, sarcoidosis, Crohn’s disease (CD) and orofacial granulomatosis (OFG) Lesion causing extreme concern to patient Contraindications for biopsy: Pigmented lesions Lesions that appear purplish and appear to be filled with blood Systemic conditions Precautions in taking biopsy: Adhere to infection control policy Minimum LA manipulation is not to be injected into the lesion (must be 1 cm away) Iodine Avoid Sharp containing antiseptics should be avoided important anatomical structures instrument should be used (not diathermy) Some of the normal surrounding tissue should be included Elliptical Small piece is taken and deep is better than shallow and broad Identify Specimen surgical margins should be fixed immediately in 10 formalin solution Give clinical data including D.D Histopathology: Incisional Excisional Punch Aspiration and cytological Types of biopsy: 1. Excisional: Removal of the entire lesion with adequate margin (in small lesions ≤ 1 cm) In case of almost certain that lesion is benign Used as diagnostic and treatment (avoidance of second operation) 2. Incisional: part of the lesion is removed Select good site (toluidine blue may be used scalpel or punch may be used Include part of adjacent normal looking tissue (may yield more information than lesion itself) 3. Punch biopsy: Tissue punches with Diameter from 0.2-0.6 cm are used Punch biopsy 4. Needle aspiration biopsy Simple and rapid Effective in parotid tumors and LNs with less risk Aspirate may used for: Chemical analysis Microbiological Histopathological used for biopsies in: Lymph nodes Deep seated lesions Parotid lesions Use lidocaine with 1:100,000 epinephrine Select the area of interest and deliver only a few drops of local anesthetic Remove the 4 mm diameter punch instrument from its sterile package Place the cutting edge at a right angle to the biopsy site and twirl the handle, cutting a core about 3 mm deep (for reference, the bevel is around 1 mm) The circular core can be removed in one of two ways: 1. curved scissors or 2. scalpel, #15 blade Grasp the core with tissue forceps, cut out the core and place in the vial of 10% formalin Fill out request forms, provide billing information and send to laboratory PREPARATION OF CYTOLOGY SMEAR • Sample spread on glass slide • Fixed with 70 % alcohol and air dried for 30 minutes • send to lab with clinical details Disadvantages of FNAB: Difficult to interpret Sample may be unrepresentative (false negative) Diagnostic cytology includes: Exfoliative cytology: Microscopic examination of cells that are spontaneously shed from epithelial surfaces or taken by simple scraping, brushing or washing of a lesion Usually they are individual cells Diagnostic criteria depends on nuclear and cytoplasmic features Interventional cytology (FNAB) Sample taken by surgical procedure Diagnostic criteria depends on nuclear features Diagnostic criteria also lies in cytoplasmic as well as nuclear features Exfoliative cytology: Microscopic examination of surface cells that have been removed from oral mucosa by scraping Very useful in some parts of the body (Pap smear for cervical cancer) but of limited value in oral cavity May show dysplastic changes of oral mucosa Recently Smear oral brush biopsy is being used examination may be useful in Candida hyphae demonstration Exfoliative cytology: Indications: Rapid laboratory evaluation In premalignant lesion when patient is not ready for biopsy Multiple premalignant lesions For evaluation of vesicular lesions Exfoliative cytology Advantages: Limited No equipment is needed need for anaesthesia or surgical instruments Short Less time anxiety and fear for the patient Exfoliative cytology Disadvantages: Detects early surface lesions only and give no clue about the underlying tissue In Heavily keratinized lesion the exact nature can not be identified Biopsy is finally essential to establish definitive diagnosis Many times materials are not adequate or not representative Oral brush biopsy: No LA special instrument used to obtain transepithelial specimen containing cells from deep, superficial and intermediate layers of epithelium Computer assisted system is used for analysis and confirmation that all epithelial layers are represented in the sample Specificity and sensitivity are still questionable Pap smear showing cervical cells taken by the brush shown Indications for use: Flat white lesions Red lesions Ulcer margins Ulcerated masses BRUSH BIOPSY Indications for oral Exfoliative cytology: Blister forming viral infections (viral inclusions and multinucleated giant cells) Pemphigus Tzank cells Candidosis and deep fungal infections (hyphae) If Normal biopsy is not possible Contraindications: Clinically obvious malignancy Hyperkeratotic white lesions For suspected malignancy, the cytopathology report may come as: Negative for malignancy This doesn't ensure absence of malignancy, it only say that in the sample submitted, cells didn't show malignant features Suspicious for malignancy Biopsy recommended Positive for malignancy Biopsy is mandatory HEMATOLOGICAL INVESTIGATIONS HEMATOLOGICAL INVESTIGATIONS It includes: Mature blood elements Precursors of blood elements (bone marrow) Chemical constituents of plasma Coagulation factors HEMATOLOGICAL TESTS Complete or Full blood count (CBC or FBC) Frequently requested and very valuable in oral diagnosis and oral med. Includes: Hb estimation % Red cell count Hematocrit PCV White cell count: Total DLC Platelet count Red blood cell indices: • MCV MCH MCHC For visual inspection of blood cells • • Blood film Size : variation in size called Anisocytosis Shape: variation in shape called Poikilocytosis There may be abnormal shape as in Spherocytosis Cells may be: Normocytic Microcytic Macrocytic Immature cells HB content : Normochromic Hypochromic Blood film Bleeding tests ESR Non specific Elevated in chronic inflammatory diseases Blood Normal range ↑ level ↓ level Hb M: 13-18 gm/dL F: 11-16 gm/dL Polycythemia. Myeloproliferative disease. Anemia PCV M: 40-54% F: 37-47% Polycythemia Anemia Dehydration macrocytic anemia MCV 78-99 fl PCV/RBC • Vit B12 and folate deficiency • Liver disease • Alcoholism • Hypothyroidism • Myeloproliferative disorders MCH 27-32 pg Hb/RBC • Iron deficiency anemia • Thalassemia • Chronic disease • Iron deficiency anemia • Thalassemia Blood Normal range MCHC 32-36 gm/DL = Hb /PCV RBCs M 4-6 × 1012/L F 4-5 × 1012/L Polycythemia WBCs 4-10 × 109/L • • • • • ↑ level ↓ level • Iron deficiency anemia • Thalassemia • Sideroplastic anemia Pregnancy Infection Trauma MI Leukemia Anemia / fluid overload • Bone marrow disease • Some infections • Drugs • Idiopathic Blood Normal range ↑ level ↓ level Neutrophils 3× 109/L Pregnancy Bleeding Infection trauma, MI leukemia • Bone marrow disease • Some infections • Drugs • Idiopathic Lymphocytes 2.5 × 109/L Some infections Some infections leukemia, bowel some immune disease defects (AIDS) Eosinophils 0.15 × 109/L Allergy, parasitic infections, lymphoma some immune defects Blood Normal range Platelets 150-400 × 109/L • Thrombocytosis in bleeding ↑ level • Myeloproliferative disease ↓ level • • • • Autoimmune Drugs Leukemia Idiopathic Reticulocytes 0.5-1.5 % of RBCs • Hemolysis • Response to treatment of anemia --------------- ESR ((Nonspecific ) 0-15 mm/h • • • • • • Pregnancy Chronic infection Multiple myeloma CT disease Malignancy Temporal arteritis ----------------- Abnormalities Leukocytosis Leukopenia in TLC and DLC or neutrophilia Eosinophilia Study of WBCs helps in: diagnosis of acute infection Diagnosis of leukemia Feature MI of some other conditions e.g. Causes of Neutrophil leukocytosis: Bacterial Tissue Acute pyogenic infections necrosis as in trauma and MI hemorrhage and Hemolysis Myeloproliferative disorders like leukemia Eosinophila: Allergic reaction and diseases (B. asthma & hay fever) Parasitic infection e.g. amoebiasis Skin disease e.g. psoriasis and pemphigus Monocytosis: Chronic bacterial infection as TB Chronic myeloblastic leukemia and Hodgkin’s disease Lymphocytosis: Acute viral infections: infectious mononucleosis Mumps CMV Herpes infections Chronic bacterial infection like TB and syphilis Chronic lymphocytic leukemia Acute lymphoblastic leukemia Platelets Thrombocytosis Myeloproliferative Following disorders splenectomy Thrombocytopenia Aplastic anemia Leukemia Idiopathic and autoimmune Drugs Hypersplenism Radiation and cytotoxic drugs BLEEDING INVESTIGATIONS FBC and blood film: See the number and shape of platelets To exclude leukemia Coagulation screening Prothrombin time PT Tests extrinsic pathway (Factors VII,X, V, II,I) Normal value 14 ± 2 second Prolonged in: Liver disease Vit K deficiency Warfarin therapy INR is better: 1-1.3 in normal Activated partial thromboplastin time APTT Tests intrinsic pathway mainly (XII,XI,IX,VIII,X) Normal value: 35-40 seconds Prolonged > 50 in: Hemophilia Heparin treatment Thrombin time TT Prolonged > 15 in: Heparin therapy Fibrinogen deficiency and dysfunction e.g. DIC Bleeding time: No need to be done If platelets count is normal In vivo test BLEEDING TIME Platelet aggregation or adhesion test: Used to test dysfunction of platelets if count is normal and BT increased Antiplatelet IgG : as in ITP Coagulation factor assay: VIII IX in hemophilia in hemophilia B vWF in von Welbirand disease Taking history and good clinical examination may give good clues about the bleeding disorders: Site Type History of drugs Alcoholism Liver diseases Please note that most of bleeding disorders in dental patients are due to local factors Blood group and cross-match Serum iron, ferritin, transferrin and serum B12 and red cell folate Hemoglobin electrophoresis : Estimation of fetal Hb (HbF) may be used to help diagnosis of major Thalassemia Diagnosis of sickle cell anemia ELECTROPHORESIS URINALYSIS Urinalysis Simple, cheap, non invasive and widely available Colour: Normally: Clear yellow Dark brown: concentrated urine or bilirubinuria Red: food, blood, refampycin Cloudy: infection Ph: usually acidic Glucose nil except in: DM Pregnancy Renal Head injury Ketones: Ketoacidosis Starvation Proteins: Normally no protein Traces in pregnancy, exercise, drugs Proteinurea may indicate: UTI Nephrotic syndrome and other renal diseases DM Multiple myeloma Amyloidosis Blood (hematuria) Kidney and urinary tract inflammation Tumor Stone Trauma Infective Endocaraditis Bilirubinuria Drugs as phenothiazines Jaundice Protein Glucose URINALYSIS Ketones Health Usually no proteins, but traces can bf found in young and pregnancy Usually no glucose but traces can be found in pregnancy Usually no Disease Renal diseases DM M. Myeloma Amyloidosis Endocaraditis drugs DM Pancreatitis Head injury Hyperthyroidism UDM TRAUMA SATARVATI ON URINALYSIS BILIRUBIN UROBILINO BLOOD GEN Health Usually no Usually Usually no present specially in concentrate d urine Disease Hepatocellular and obstructive Jaundice All types of Genitourinary jaundice disease Bleeding disease Endocaraditis MICROBIOLOGICAL TESTS Used to make a definitive diagnosis and select antimicrobial therapy Do investigation before giving antibiotics Proper collection and transportation of sample Provide the microbiologist with clinical details Collection and transport of sample: Collect appropriate sample As fresh as possible Appropriate transport medium: suitable for suspected microorganism (virus or bacteria) No contamination Microbiological methods: Non cultural methods: Light microscopy Electron microscopy Gene or DNA probing using PCR Cultural methods: using bacterial culture (solid or liquid) or tissue culture for viruses Immunological methods: Detect antibodies Detect antigens Light Microscopy: Very useful Very quick (results within minutes) Inexpensive (LM and stain) Gram stain to classify into G+ and G- bacteria Acid fast stain e.g. Ziehl-Neelsen stain for Mycobacterium tuberculosis Dark field microscopy for spirochetes like TP LM is helpful in the diagnosis of thrush, actinomycosis and AUG EM may be used for viral Smears SMEAR Isolation and identification of the pathogens using culture media: Most common, reliable and universally available in clinical practice Help in diagnosis and choosing proper antibiotic Cultures: For Bacteria and fungi : culture media (usually blood agar; selective or non selective media) For Viruses: tissue culture Bacterial culture: May need transport medias if there would be a delay Avoid contamination if sample is from non sterile part of the body e.g. Oral cavity Swap or needle may be used to collect the sample Oral rinse may be used for oral Candida If anaerobic organisms are suspected deal with sample accordingly Identification of the causative organisms: Colony characteristics in culture plates Growth requirements Biochemical tests Indications for cultures: Management of suppurative lesions As an aid in the diagnosis of candidosis Bacterial culture of complicated odontogenic infections Detection of microbial nucleic acid in clinical specimen (DNA probes): Labelled commercially available fragments of DNA that will hybridize with complimentary sequence of microbial nucleic acid if present in the specimen The sample is first treated to denaturate microbial dsDNA and then the DNA probes added The microbial DNA sequence is multiplied using PCR PCR enable us to detect even small amount of antigens Advantage of DNA probes : Very sensitive Quick No need for culture so very useful in viruses Disadvantage: expensive Not readily available Need well trained staff Serology : Microbes can be identified by detection of their specific antibodies or antigens in the serum or other body fluids Methods of serology Precipitation Agglutination Immunoelectrophoresis Immunofluorescent IMMUNOFLUORESCENT TECHNIQUE It is two stage procedure: Commercially available microbial antigens are incubated with patient’s serum DIF: Fluorescinated or enzyme labeled, animal derived antibody to human immunoglobulins is added to detect antigens using a fluorescent microscopy IDIF: a known antigen is allowed to react with the unknown serum antibody which then detected with fluorescent dye conjugated anti-antibody The different classes of immunoglobulins can identified and quantified to determine: Acuteness of infection if IgM is predominate or there is fourfold rise in IgG level between acute sample and second one taken 10 days later (convalescent sample ) Chronic infection and immunity is assessed by measurements of IgG Very useful for microbes that are difficult to cultivate Blood culture: endocaraditis and septicaemia Some Serological and immunological tests Syphilis screening tests: 1. Tests rely on non specific antibacterial antibodies called reagin 2. a. rapid plasma regain and card test b. VDRL test Definitive tests: a. Treponema pallidum hemagglutination test (TPHT) b. fluorescent treponemal antibody with absorbed serum (FTA-ABA) infectious mononucleosis: Paul-Bunnel test: heterophil Paul-Bunnel antibodies causes sheep RBCs to agglutinate and it is positive for 6 months after infection HIV and AIDS: Rely on detection of antigenic viral components or antibodies formed as in response to HIV infection Western Blot test (antibody test): Patients serum + test strips containing HIV antigens: ELIZA will demonstrate Ag-Ab complexes Viral hepatitis: ELIZA test demonstrate of both the viral antigens and antibodies response of the patient to infection Hepatitis B: Hepatitis B surface antigens (HBsAg): positive in current infection Hepatitis Be antigen (HBeAg): positive in highly infectious cases Hepatitis BcAntigen (HBcAg) positive: indicate infection With hepatitis B virus – earliest response Hepatitis B surface antibodies: appear late and indicate long term immunity against HB infection SEROLOGY OF AUTOIMMUNE DISEASE Diagnosis of autoimmune diseases based on: Clinical features Elevated ESR Decreased A/G ratio Serological tests in some cases Rheumatoid factor: antibodies react with IgG immunoglobulin and the complex cause damage to synovial membrane. This test is positive in rheumatoid arthritis Antinuclear antibodies: (ANA) Fluorescent antinuclear antibody test Indirect immunofluorescence BIOCHEMICAL INVESTIGATIONS Urea, creatinine and electrolytes (U &Es): renal failure : both creatinine and urea are increased Electrolyte disturbance Liver function test LFTs: Used for diagnosis of liver ALT diseases, jaundice and AST biliary tract GGT Alk. Phosphatase Serum Ca, Po4 and alkaline phosphatase Diagnosis of bone diseases Cardiac enzymes: AST Creatine kinase CK Lactate dehydrogenase LD Troponin : very specific and diagnostic Lipids: Cholesterol Triglycerides Lipoproteins Hormones Blood glucose tests Arterial blood gases Biochemical investigations: Blood chemistry: Calcium: Normal: The 9-10.6 mg % 2.3-2.6 mmol/L normal range is controlled by: parathyroid hormone thyrocalcitonin Vitamin D Serum calcium: High values: Hyperparathyroidism Bone metastasis Multiple myeloma Paget’s disease Sarcoidosis Thiazides Hypervitaminosis D Low values: Hypoparathroidism Vitamin D deficiency Renal failure Nephrotic syndrome Phosphorus: Normal: adults 3-4.5 mg % children 4.0-7.0 mg % The normal range is controlled by: parathyroid hormone Vitamin D Phosphorus: High values: Chronic renal disease Healing bones Hypoparathyroidism Hypervitaminosis D Low values: Hyperparathroidism Rickets and Osteomalacia Blood glucose: Normal: 70-100 mg /100 ml 2.8-5 mmol /L High value: DM Cushing's disease Steroid intake Low value: Insulin secreting ? Addison’s disease Malabsorption of carbohydrates Uric acid: Normal: Male: 2.1-7.8 mg % Female: 2.0-6.4 mg % High values: Gout Renal failure Leukemia and lymphoma Starvation, lead poisoning Low values: rare Cholesterol: Normal: 150-250mg % 3.9-7.8 mmol/L High values: cardiovascular disease, biliary obstruction and chronic hepatitis Hypothyroidism uncontrolled diabetes Low values: acute infections Malnutrition Hyperthyroidism Total protein and albumin/globulin ration (A/G ratio): Normal values: Total protein: 6.0-7.8 g % Albumin: 3.2-5.6 g % Globulin: 2.3-3.5 g % A/G ratio 1.5:1 to 2.5:1 Proteins High total proteins: CT diseases; SLE, rheumatoid arthritis Acute liver destruction Multiple myeloma Low values: Malnutrition Malabsorption Anemia Diarrhea Burns Nephrotic syndrome Abnormal A/G ratio: Multiple myeloma Severe liver diseases Billirubin: Normal values: 0.2-1.2 mg % High values: haemolytic anemia biliary obstruction hepatitis malignant liver disease Alkaline phosphatase: Normal values: 30-85 IU/ L High values: obstructive liver disease metastatic carcinoma involving bone Hyperparathyroidism Paget’s disease Osteomalacia rickets Low values: rarely in scurvy, hypophosphatasia and hypothyroidism Blood urea nitrogen: Normal: High 8-18mg % 3.3-6.7 mmol/L values: Renal failure Dehydration Low values Liver disease Nephrotic syndrome Vit B 12 150-800 ng/L High value Liver disease Leukemia Low value Pernicious anemia Gastrectomy Crohn’s disease Ileal resection Strict vegetarian Metformin Folic acid 3-20 microgram/L Red cell folate 120-650 microgram/L Low value Alcoholism Nutritional deficiency Hemolytic anemia Drugs: Phenytoin Methotrexate Sulphasalazine Oral contraceptive pills Serum ferritin Adult male 25-190 ng/mL Adult female 15-99 ng/mL Child mean 21 ng/mL Low value: Iron deficiency Electrolytes: that include; sodium(Na) potassium (K), chloride (CL) and Co2