* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download THE COMPARISON OF DIALYSIS TYPES` EFFECTS ON HEARING
Survey
Document related concepts
Transcript
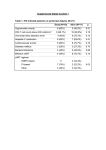
THE COMPARISON OF DIALYSIS TYPES’ EFFECTS ON HEARING ACUITY AND BAER FINDINGS IN PATIENTS WITH CHRONIC RENAL FAILURE Assist. Prof. Sebahattin CÜREOĞLU, MD* Assist. Prof. Üstün OSMA, MD* Research Fellow Zafer ALKAYA, MD* Research Fellow Yasin SARI, MD** Assoc. Prof. Faruk MERIÇ, MD* Prof. İsmail TOPÇU, MD* Assoc. Prof. M.Emin YILMAZ** *Dicle University, School of Medicine, Department of Otorhinolaryngology ** Dicle University, School of Medicine, Department of Nephrology Running Title: Effect of dialysis on hearing in renal failure Key words: Chronic renal failure, hearing loss, hemodialysis, peritoneal dialysis, BAER Corresponding Address: Yrd. Doç. Dr. Sebahattin CÜREOĞLU Dicle Ün.Tıp Fak. KBB Anabilim Dalı, 21280, Diyarbakır- TURKEY E-Mail: [email protected] Total number of pages: 11 1 Abbreviations used: CRF, chronic renal failure; PTA, pure-tone audiometry; TTD, Threshold tone decay test; BAER, Brainstem auditory evoked; SNHL, sensorineural hearing loss. 2 THE COMPARISON OF DIALYSIS TYPES’ EFFECTS ON HEARING ACUITY AND BAER FINDINGS IN PATIENTS WİTH CHRONIC RENAL FAILURE Abstract In this study, the origin of hearing loss in patients with chronic renal failure (CRF) and the effect of dialysis type on hearing loss due to CRF was investigated. For these purposes, 40 patients with CRF ( 20 in hemodialysis and 20 in peritoneal dialysis program) were examined for hearing acuity by pure-tone audiometry (PTA), Threshold tone decay (TTD) test and Brainstem auditory evoked response (BAER). The hearing loss (13 cochlear, 10 retrocochlear in TTD test), was found in 57.5 % of patients. BAER findings showed that III., V. absolute latencies and I-III., III-V interpeak latencies were significantly longer in hemodialysis group than control group. No statistical significance was found between hemodialysis and peritoneal dialysis groups in audiological and BAER findings. Significant changes were not also observed before and after hemodialysis. It is concluded that both cochlea and retrocochlear region are susceptible to the effect of uremia. The type of dialysis has not affected the degree of hearing loss in CRF patients. 3 Introduction Etiology of sensorineural hearing loss (SNHL) seen in CRF patients is contradictory. In the literature, uremic toxins, anemia, electrolyte imbalance, chelating agents used in hemodialysis, ototoxic medications, metabolic imbalances, immune deficiencies, dialysis type, and dialysis frequency were shown responsible for SNHL (1-4). The purpose of this investigation was to evaluate auditory ability and brainstem auditory evoked response (BAER) findings of CRF patients who were treated by dialysis and also the effect of dialysis type on hearing acuity. Patients and methods This study included 40 patients with CRF who were on dialysis medication.The diagnosis of a CRF was based on history, physical examination, laboratory tests, and biopsy study. Since the patients could no longer be maintained conservatively by medication and diet, they were treated by dialysis. Three groups were included in the study; Group I, 20 patients (13 males, 7 females) with CRF taking hemodialysis (14 patients were taking dialysis 3 times a week, 6 patients were taking twice a week); Group II, 20 patients (12 males, 8 females) taking peritoneal dialysis (patients were taking dialysis twice a day); Group III, 20 persons (13 males, 7 females) as control. Patient with a family history of hearing loss, chronic otitis media, ototoxic medication, acoustic trauma and diabetes mellitus, and patients who were over 40 years old to eliminate presbyacusis were excluded from the study. All patients had otoscopic examination before tests to exclude external factors. BUN, creatinin, electrolytes and glucose levels were measured before dialysis. Pure tone audiometry, Threshold tone decay (TTD) test, and 80 dBHL BAER potentials were recorded before and after dialysis. Our standard isolated audiology laboratory was used for 4 tonal, supraliminary test and BAER. 2048 rarefaction click in 10srr/sec were used in BAER. We used Medelec Sapphire 2A equipment for BAER, Madsen OB-822 for audiometry, Amplaid 720 for tympanometry. We considered 250-500,1000 Hz hearing levels as low frequency levels, 2000, 4000, 6000, 8000 Hz levels as high frequency hearing levels. The findings were compared among hemodialysis group, peritoneal dialysis group, and control group. 25 dBHL was accepted normal according to the ISO-1964 standards. In statistical evaluation, ANOVA test and Post hoc Tukey procedure were used to understand which groups are different. Results The mean age of patients was 31,7 (range 17-40 years) in patient’s group, 32.5 in control group. Etiology of CRF in these patients is shown in Table 1. Mean patients’ diseased period was 4 years (1-18) in both peritoneal dialysis and hemodialysis groups. On the basis of test results; in hemodialysis group, (6 patients had cochlear, and 5 had retrocochlear) totally 11 had SNHL. In peritoneal dialysis group, (7 patients had cochlear, 5 had retrocochlear), totally 12 had SNHL. Hearing loss mostly were in high frequencies. TTD test showed cochlear pathology in 13 patients and retrocochlear pathology in 10 patients. Significant prolongation of I. absolute latency in cochlear group was observed when the BAER results of cochlear and retrocochlear groups were compared (p<0.05). Hearing levels in controls were 12.65-/+ 5.64 in low frequencies, and 16.52 -/+ 4.74 in high frequencies. Hearing levels were 20.40 -/+ 13.1 and 31.1-/+ 17.5 in peritoneal dialysis group, and 20.90-/+ 14.1 and 35.0-/+19.0 in hemodialysis group accordingly. There was significant difference in hearing levels between patient’s and control’s group (P<0.01). There was no significant difference in audiometrical findings between hemodialysis and 5 peritoneal dialysis group. There was no significant difference in high frequency and low frequency hearing levels before and after hemodialysis. BAER results are given in Table 2. As seen in Table 2, there was significant difference for III., V. absolute and I-III, III-V interpeak latencies between hemodialysis and control groups. But there was no significant difference among the BAER results of hemodialysis (before and after), and peritoneal dialysis groups. Discussion After the first reported hearing loss in patients with CRF by Diafaley, some authors reported varying degrees of hearing loss (1-8). In our study, hearing loss was found in 23 (57.5%) patients. Patients with CRF have usually high frequency hearing loss 1,6. But Gatland et al. also reported both high and low frequency losses(3). In our study, most of them had high frequency loss, but we also detected low frequency component of hearing loss in patients. The causes and the origin of hearing loss are contradictory. Yassin et al. has proposed a possible common defect in the electrolyte transport through membranes and that hearing loss was correlated with hyponatremia(9). But Kopsa et al. found no correlation between them(4). In our study groups, serum Na, K and Ca levels were normal. It was suggested that when diuretics and aminoglycosides are used together, they may effect stria vascularis and corti organ and cause ototoxicity(10). But none of our patients had used them so we discluded their effect. Because metabolic disease like diabetes mellitus may effect cochlear blood supply, we didn’t take this group to our study. Some authors demonstrated the involvement of both central and peripheral nervous systems, which was already present before hemodialysis and thought that it was 6 possibly due to ureamic neuropathy(11,12). It is reported that the effect of uremia to stria vascularis causes cochlear hearing loss(13). Wigand et al. reported an average hearing loss of 20 dB in a group of ureamic patients, particularly in the higher frequencies, suggesting cochlear involvement(14). The study by Marsh suggests that the acoustic nerve more vulnerable to the effects of uremia(15). Retrocochlear hearing loss is considered to be the result of demyelinization from superior olivary nucleus to inferior colliculus(16,17). But demyelinization in cochleovestibular preganglioner fibers also contributes to retrocochlear hearing loss(17). Our results have shown both cochlear and retrocochlear hearing loss, and 13 patients had cochlear and 10 had retrocochlear pathology according to the TTD test. They also had prolonged absolute III., V. latencies and prolonged I-III, III-V interpeak latencies. Significant prolongation of I. absolute latency in cochlear group was observed when the BAER results of cochlear and retrocochlear groups were compared. Some authors reported that hearing loss got better after dialysis(3,8), but there are some reports showing worsening of hearing(2,7,18). It was shown that prolonged first-wave latency was reported in hemodialysis patients in one study(15), whereas the fifth wave latency was prolonged in another study(19). Gafter et al. showed prolongation of III and V waves latencies in patients with CRF(12). The results of prolonged BAER latencies are in accordance with previous studies which showed delayed prolongation mostly of the later waves III, V and interpeak III-V latency in patients on hemodialysis(12,19). Bazzi et al. did not find any significant differences in the frequency and severity of hypoacousia in the groups with different durations of dialysis(20). Mirahmadi et al. did not find evidence of any worsening of hearing after 7 regular dialysis treatment protracted for 1-5 years(21). Oda et al. has proposed that long term hemodialysis treatment may cause electrolyte, osmotic, and biochemical alterations leading to SNHL(22). In our study, there was no significant difference between pre and post dialysis audiometrical and BAER findings. It was suggested that hemodialysis has caused more hearing deficiency in compare with peritoneal dialysis(2). In our study, hemodialysis group has lower hearing levels in compare with peritoneal dialysis group but it was not significant statistically. By looking at our results, we concluded that there was no difference between hemodialysis and peritoneal dialysis in effecting hearing. BAER findings exhibit no improvement of neural conduction after hemodialysis in patients with CRF. The present study may also suggest that cochlea and retrocochlear region especially the pons and midbrain is more susceptible to the effect of uremia. REFERENCES 1-Kligerman AB, Solangı KB, Ventry IM, Goodman AL, Weseley SA. Hearing impairment associated with chronic renal failure. Laryngoscope 1981;91:583-592. 2-Nikolopoulos TP, Kandiloros DC, Segas JV, Nomicos PN, Ferekidis EA, Michelis KE. Auditory function in young patients with chronic renal failure. Clin Otolaryngol 1997;22(3):222-5. 3-Gatland D, Tucker B, Chalstrey S, Keene M, Baker L. Hearing loss in chronic renal failure-hearing threshold changes following haemodialysis. J R Soc Med 1991;84(10):587-9. 4-Kopsa H, Kotzaurek R, Mitschke H, Schmidt P. Horstorungen bei chronisher Niereninsuffizienz. Mschr. Ohrenheilk. Lar. Rhinol 1972;106: 332-339. 8 5-Mancini ML, Dello-Strologo L, Bianchi PM, Tieri L, Rizzoni G. Sensorineural hearing loss in patients reaching chronic renal failure in childhood. Pediatr Nephrol 1996;10(1):38-40. 6-Morton LP, Reynolds L, Zent R, Rayner BL. Hearing thresholds in CAPD patients. Adv Perit Dial 1992;8:150-2. 7-Kusakari J, Hara A, Takeyama M. The hearing of the patients treated with hemodialysis: A long term follow-up study. Auris Nasus Larynx 1992;19:105-113. 8-Özen M, Sandalcı O, Kadıoğlu A, Agosoğlu N. Audiometry in chronic renal failure before and after intermittent hemodialysis. Proc Eur Dial Transplant Assoc 1974;11:203-209. 9-Yassin A, Badry A, Fatthi A. The relationship between electrolyte balance and cochlear disturbances in cases of renal failure. J Laryngol Otol 1970;84:429-435. 10-Bergstrom L, Jenkins P, Sando I, English GM. Hearing loss in renal disease: Clinical and pathological studies. Ann Otol Rhinol Laryngol 1973;82:555-576. 11-Antonelli AR, Bonfioli F, Garruba V, et al. Audiological findings in elderly patients with chronic renal failure. Acta Otolaryngol Stockh Suppl 1990;476-54-68. 12-Gafter U, Shvili Y, Levi J, Talmi Y, Zohary Y. Brainstem auditory evoked responses in chronic renal failure and the effect of hemodialysis. Nephron 1989; 53:2-5. 13-Bubalo FS, Davidson DD. Recent developments in hereditary nephritis-Alport’s syndrome. Indiana Med 1991;84:860-6. 14-Wigand ME, Meents O, Kreusser H, Heiland A. Cochleovestibular disturbances in renal failure and the influence of diuretics. Audiology 1972;11 (supp):31-35. 9 15- Marsh JT, Brown WS, Wolcott D, Landsverk J, Nissenson AR. Electrophysiological indices of CNS function in hemodialysis and CAPD. Kidney Int 1986;30:957-963. 16-Albert A, Di Paolo B, Capedi P. Evoked potentials in uremia. Contributions to Nephrology 1985;45:60-68. 17-Luciern JC, Anteunu MA, Jacob MV. Hearing loss in a uremic patient: indications of involvement of the VIII.th nerve. J Laryngol Otol 1987;101:492-496. 18-Moffat DA, Cumberworth VL, Baguley DM. Endolymphatic hydrops precipitated by haemodialysis. J Laryngol Otol 1990;104:641-642. 19-Hutchinson JC, Klodd DA: Electrophysiologic analysis of auditory, vestibular and brainstem function in chronic renal failure. Laryngoscope 1982;92:833-843. 20-Bazzii C, Venturini CT, Pagani C, Arrigo G, D’Amico G. Hearing loss in short and long term haemodialysed patients. Nephrol Dial Transplant 1995;10(10):1865-8. 21-Mirahmadi MK, Vaziri ND. Hearing loss in end-stage renal disease- effects of dialysis. J Dial 1980;4:159-162. 22-Oda M, Preciado MC, Quick CA, Paparella MM. Labyrinthine pathology of chronic renal failure patients treated with hemodialysis and kidney transplantation. Laryngoscope 1974;84:1489-1506. 10 Table 1. Etiological factors in patients with CRF. Etiology Case number (n=40) Chronic Pyelonephritis + nephrolithiasis 15 Chronic Glomerulonephritis 10 Amiloidosis Unknown 3 12 11 Table 2. Absolute and interpeak latencies of BAER waves in hemodialysis, Peritoneal dialysis groups and controls . Group I III V I-III Control 1.68 3.80 5.76 2.11 1.96 4.07 Hemodialysis 1.73 3.99 5.97 2.22 1.99 4.22 Peritoneal dialysis 1.70 3.93 5.88 2.20 1.95 4.16 P <0.05* <0.05* >0.05 <0.05* III-V <0.05* I-V (msn) >0.05 *The difference is found between hemodialysis and control groups. 12