* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Common Clinical Syndromes: Diarrhea
Survey
Document related concepts
Transcript
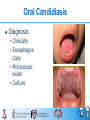
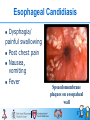
Digestive Tract Diseases in HIV-infected Children HAIVN Harvard Medical School AIDS Initiative in Vietnam 1 Learning Objectives By the end of this session, participants should be able to: Diagnosis and treatment of oral candidiasis Describe the most common causative pathogens of diarrhea in HIV-infected children Describe clinical manifestations and diagnosis of diarrhea Develop a treatment plan for diarrhea in an HIV-infected child 2 Oral Candidiasis 3 Oral Candidiasis Common seen in severe stage of immunodeficiency Usually persistent and refractory Form: • multiple white • easily removable patches • pseudomembranous plaques Place • • • • Tongue Gums Buccal and pharyngeal mucosa Esophagus 4 Oral Candidiasis Diagnosis: • Clinically • Eosophagos copy • Microscopic exam • Culture 5 Esophageal Candidiasis Dysphagia/ painful swallowing Post chest pain Nausea, vomiting Fever Spsuedomembrane plaques on eosopaheal wall 6 Treatment Topical: • Clotrimazole (Dartarin cream) • Ketoconazole • Nystatin Systemic: Medication Duration Oral candidiasis: 7-10 days •Fluconazole: 3-6mg/kg BID •Itraconazole:3-6 mg/kgBID Esophageal candidiasis: 2 weeks 7 Source: National guidelines 3003, 2009 Overview of Diarrhea 8 Definition Diarrhea is defined as having loose or watery stool at least 3 times per day, or more frequently than normal Acute diarrhea Persistent diarrhea or Chronic diarrhea < 14 days >14 days 9 WHO 2009. Diarrhea: why children are still dying and what can be done Epidemiology Diarrhea is the second leading cause of death among children less than 5 years old Diarrhea occurs more frequently in HIV-infected children than in HIVnegative children, with more severe and persistent episodes WHO 2009. Diarrhea: why children are still dying and what can be done 10 Prevalence of Diarrhea in HIV-infected Children 23.5-100% Thailand (52.7% average) Nigeria 75% Children’s Hospital 1 Vietnam Hospital of tropical diseases 9% 60% (2003) 33-49% (2006) Etiology (1) The most common diarrheal pathogens in children include: • Rotavirus • Bacterial agents In addition, HIV-infected children are susceptible to other less common pathogens: • Protozoans • Parasites • Mycobacteria WHO 2009. Diarrhea: why children are still dying and what can be done 12 Etiology (2) HIV-associated Pathogens: occurs in severely immunosuppressed children Cryptosporidium infection MAC infection Abdominal TB lymph node infection Cytomegalovirus (CMV) • CMV-associated Colitis 13 Etiology (3) Other causes are noninfectious etiologies: • HIV-associated malabsorption • Lactose intolerance • Medication side effects: Didanosine (ddI), buffer form Protease inhibitors (PI): • Lopinavir/ritonavir • Ritonavir 14 Pathogenesis (1) Factors that contribute to susceptibility to diarrhea in HIVinfected children: • • • • young age malnutrition undernourishment immunocompromised status 15 Pathogenesis (2) Micronutrient deficiency increases risk of mortality several fold Diarrhea is transmitted through: • Fecal-oral route • Contaminated food and water • Person-to-person 16 How Do You Diagnose Diarrhea? 17 Diagnosis: Overview Recognize diarrhea is important as delayed diagnosis and treatment would result in patient mortality Focus on history can classify the diarrhea, its severity, and its possible causes Physical exams are also important to assess illness severity 18 Diagnosis: Overview (2) In children <2 • acute watery, non-bloody diarrhea with vomiting is usually due to viral pathogens In older children • viral diarrhea is still common • bacterial diarrhea should also be considered In immunosuppressed children • diarrhea may be due to HIVassociated pathogens 19 Diagnosis: History (1) Onset: acute, subacute Duration: how long Number of bowel movements a day Stool characteristics • Profuse • Watery • Semi-form • Mucous • Bloody 20 Diagnosis: History (2) Associated symptoms: • Fever, vomiting, abdominal pain. • Other household members with diarrhea Other history: • Medications (ARVs, other drugs) • Food/water intake • Other OI that may cause diarrhea 21 Assessing: Level of Dehydration Action A Look at: •Condition Well alert B C Restless, irritable Lethargic, unconscious •Eyes Normal Sunken Sunken •Thirst Normal drink, no thirsty Thirsty, drink eagerly Drinks poorly or unable to drink Feel: Goes back skin pinch quickly Goes back slowly (<2 s) Goes back very slowly (>2 s) Decide If there are ≥ 2 signs: some dehydration If there are ≥ 2 signs: severe dehydration No dehydration Symptoms/Signs Associated with Dehydration Mental status Thirst Heart rate Quality of pulses Breathing Eyes Tears Mouth and tongue Skinfold Capillary refill Extremities Urine output 23 Common Diseases Shigellosis • Fever, abdominal pain, scraping • Bloody mucous stool, frequent bowel movement • Stool microscopic observation: erythrocytes, leucocytes • High, prolonged fever, pulse-tem discordance, may presented as sepsis Salmonellosis • Watery stool, bloody stained stool • Culture: stool/blood 24 Common Diseases HIV-associated • Cryptosporidia Microsporida Isospora Infection • • • CMV colonitis • • • Watery, frequent stools, no blood, large volume Rapid weight loss, commonly no fever Vomiting, nausea, abdominal pain Stool microscopic stain: Fever, Abdominal pain Bloody stools May have CMV infection in other organs (esophagus, lungs, liver) 25 CMV-associated Colitis Sigmoidoscopy: disseminated unspecific rash, submucous bleeding and ulcer • Histology: inclusion body in intracytoplasma 26 Common diseases HIV-associated • Persistent or recurrent fever • Persistent or recurrent diarrhea Disseminated MAC Infection/ Abdominal Lymphnode TB • Abdominal pain • Weight loss or no weight gain • Fatigue, sweats • Anemia, leukopenia, low platelet • TB: ultrasound image, may have pulmonary TB 27 Laboratory Tests 28 Overview In general, most diarrheal illness does not require laboratory testing However, in cases of severe or persistent diarrhea, the following tests may be useful: • • • • CBC Electrolytes Renal functions Blood culture 29 Stool Study Stool microscopic exam: WBC, RBC, O&P Stain: AFB, Modified AFB Antigen detection: • Rotavirus antigen • C. difficile toxin Stool culture: • Bacteria • Mycobacterium species Chronic diarrhea not responsive to usual therapy: Sigmoidoscopy, Colonoscopy 30 Treatment Fluid replacement and feeding!!! 31 Fluid Replacement Action A Condition Well alert Eyes Thirst Normal Normal drink, no thirsty Feel: skin pinch Decide Treatment B C Restless, irritable Sunken Thirsty, drink eagerly Lethargic, unconscious Sunken Drinks poorly or unable to drink Goes back quickly Goes back slowly (<2 s) Goes back very slowly (>2 s) No dehydration If there are ≥ 2 If there are ≥ 2 signs: some signs: severe dehydration dehydration Can be treated at home Hospitalized necessary Hospitalized 32 necessary Treatment at Home Give the child more fluid than usual • Fluid replacement: low osmolality oral rehydration solution (ORS) or home made solution <2 years old: 50-100 ml after each watery stool Older child: 100-200 ml Zinc supplement: • younger than 6 months: 10mg daily; • 6 months and older: 20 mg daily for 2 weeks Continue feeding: • Breast feeding: continue and more frequently • Formula feeding: every 3 hours • Soft food: continue with addition of milk 33 Treatment at Home When to return • • • • • • • Begins passing frequent, watery stools Has repeated vomiting Becomes very thirsty Is eating or drinking poorly Develops a fever Has blood in the stool Does not get better in 3 days 34 Inpatient Treatment (1) For mild and moderate dehydrated cases, admission to the hospital is necessary Oral rehydration: 75 ml/kg for 4 hours • Monitor if the ORS given appropriately • Assess during and after 4 hours, if any sign of severe dehydration detected, IV replacement is needed Zinc supplement: after first 4 hours as treatment at home Feeding: • encourage breast feeding whenever possible • Other: as treatment at home 35 Inpatient Treatment (2) For severe dehydrated IV rehydration with lactate ringer/normal saline solution If IV not available: nasogastric tube can be used to give ORS Oral rehydration in addition Correction of acidosis, electrolyte repletion Zinc supplement and feeding when possible 36 Pathogenic Treatment 37 Shigellosis Salmonellosis (bloody stool) Ciprofloxacin: 15 mg/kg/day BID x 5 days Norfloxacin: 15 mg/kg/day BID x 5 days Cephalosporin 3th gen • Ceftriaxone: 50 mg/kg IV x 5 days For H.histolytica: • Metronidazole: 50 mg/kg/day TID x 5 days 38 HIV-associated Pathogens ARV is the common treatment Cryptosporidia •Azitromycin: 10 mg/kg/day x 10 days •Plus Paromomycin: 25-35 mg/kg/day Microspora •Albendazole 10 mg/kg/day x 3 days Isospora CMV colitis •Gancyclovir IV 10 mg/kg x 14-21 days then 5 mg/kg/day x 5-7 weeks Disseminated •Clarithromycin: 7.5-15 mg/kg twice MAC daily Plus •Ethambutol 15-25 mg/kg daily Plus •Rifampicin 10-20 mg/kg daily 39 TB •TB therapy Case Study A 2-year-old child comes to your OPC for follow-up His mother mentions to you that he has been having diarrhea for the last 2 days He has 5-6 stools per day. The stool is watery, non-bloody, without mucous The mother thinks he also runs a fever because his forehead feels hot to the touch His most recent CD4: 25%, 500cps/ml He’s not yet on ARV 40 Key Points Diarrhea is common in HIV-infected children and needs aggressive treatment Most common pathogens are viruses, bacteria and local circulating agents OIs causing diarrhea include TB, MAC, cryptosporidia and CMV 41 Thank you! Questions? 42