* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Clinical Features
Survey
Document related concepts
Transcript
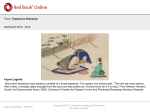
PERIPHERAL VASCULAR DISEASE
Dr .Ghazi F.Haji
Senior lecturer of Cardiology
Al-Kindy College of Medicine/Baghdad university
06/07/2017
1
”Objectives”
Definition
Aetiology
Presentations
Investigations
Management
Acute arterial occlusion
06/07/2017
I
2
Peripheral vascular disease of the lower
extremities
Definition
“Decreased patency” of the arterial supply to the lower
extremities leading to
Chronic ischemic: (Claudication ,critical limb)
Atherosclerotic, Vasculitis,Burger's Disease
(ThromboangiitisObliterans),Extrinsic compression
(neoplasm)
Acute Ischemic : Embolic, Thrombotic”
06/07/2017
3
Risk Factors
Hypertension
Cigarette smokers
Diabetics
Hyperlipidaemia
Increased age
History of other atherosclerotic disease
(coronary artery disease or carotid stenosis)
06/07/2017
I
4
Pathophysiology
“Narrowing of the arterial lumen leads to”
Decreased blood flow resulting in.
Decreased O2 supply leading to
Anaerobic metabolism
Increased Lactic Acid
leading to:
Pain at rest
Poor wound healing
Painful ulceration
06/07/2017
5
Chronic Ischaemia
Intermittent Claudication
Muscle pain which appears during exercise
when there is an inadequate arterial flow
critical limb -Rest Pain
Cold Peripheries
Arterial Ulcers
Wet/dry gangrene
06/07/2017
6
Clinical Presentation
1.
2.
3.
4.
Cramping/burning muscular pain
Localized to a muscle group (calf)
Reproducible
Relieved with rest
Distribution of pain may suggest anatomic
location of disease
06/07/2017
7
Lower Limb Assessment
Features of Chronic Ischemic changes
“Hair loss, shiny appearance & Trophic changes
Pulses: diminished or absent
Bruits:”
Presence of Gangrene
Ulcers
Pallor on elevation and rubor on dependency
(Buerger's sign)
Muscle-wasting
Skin and nails: dry, thin and brittle
Temperature: Often cool
Oedema: un usual
06/07/2017
8
Intermittent Claudication
Differential Diagnosis
06/07/2017
Spinal Stenosis
9
Pain caused by critical Limb
Ischemia
Rest Pain
worse at night
May be present throughout the day and night
Continuous, aching & severe
Located in toes and forefoot.
(Patient hangs the leg over the side of the bed)
06/07/2017
10
INVESTIGATION OF PVD
Assess risk factors:
Fasting lipids & glucose, HbA1c
Non-Invasive
Doppler Ankle/Brachial Index
Invasive
CT Angiogaphy/ MRI
Angiography
06/07/2017
11
06/07/2017
12
Chronic Ischaemia
Conservative Management
STOP SMOKING!
Increasing exercise tolerance
Pharmacotherapy's:
Aspirin 75 mg daily or clopidogrel 75 mg daily
Statins.
The peripheral vasodilator(Pentoxyphylline)
, cilostazol, has been shown to improve walking
distance
ACE I {esp. in Diabetics }&control of DM
Avoidance of minor trauma esp. in those with
neuropathy
06/07/2017
13
Surgical Management
Endovascular options: to increase inflow if
suitable for femoral angioplasty or stenting
Surgical bypass of diseased segment using
vein or prosthetic graft
If un-reconstructable: Try Prostacyclin infusion
(Iloprost)
Last option is amputation
06/07/2017
14
Treatment of critical ischemia
“Ischemic rest pain/ulcer/gangrene”
Angioplasty vs. Surgery
06/07/2017
15
Femoral Angiography
06/07/2017
16
Acute Limb Ischaemia
Embolus
Thrombus
Trauma
06/07/2017
17
Source of Emboli
Heart - 90%
- Arrhythmias, Valvular heart disease
- Prosthetic heart valves, Mural thrombus
post MI, Ventricular aneurysm
Great Vessels (9%)
Atherosclerotic aorta
Other (1%) --Paradoxical
Thrombus--- Thrombus on a pre-existing
atherosclerotic lesion
l
06/07/2017
18
Clinical Features
Pain
Pallor
Parasthesia.
Paralysis
Pulselessness
Perishing Cold
Treatment------ Urgent Treatment
Heparin
Investigations
Intervention
06/07/2017
? Thrombolytic
19
Clinical features
Embolism
Thrombosis in situ
Severity
Complete (no collaterals) Incomplete (collaterals)
Onset
Seconds or minutes
Hours or days
Limb
Leg 3:1 arm
Leg 10:1 arm
Embolic source
Present (usually AF)
Absent
Bruits
Absent
Present
Diagnosis
Clinical
Treatment Embolectomy, warfarin
thrombolysis
06/07/2017
Angiography
-Medical, bypass,
20
Upper limb diseases
1-Arm claudication
2-Atheroembolism (blue finger syndrome).
3-Subclavian steal. When the arm is used, blood is 'stolen'
from the brain via the vertebral artery. This leads to
vertebro-basilar ischaemia, which is characterised by
dizziness, cortical blindness and/or collapse.
06/07/2017
21
Raynaud's phenomenon and Raynaud's disease
Cold (and emotional) stimuli may trigger vasospasm,
leading to the characteristic sequence of digital pallor
due to vasospasm, cyanosis due to deoxygenated blood,
and rubor due to reactive hyperaemia.
06/07/2017
22
Primary Raynaud's phenomenon (or disease):
This affects 5-10% .
Young age women aged 15-30 years may be familial
Not progress to ulceration or infarction
NO significant pain
NO underlying cause .
No investigation is necessary.
The patient should be reassured and advised to avoid
exposure to cold. Long-acting nifedipine may be
helpful
23
06/07/2017
I
Secondary Raynaud's phenomenon (or syndrome)
Occur in older people
Association with connective tissue disease (most
commonly systemic sclerosis or the CREST syndrome, ),
vibration-induced injury (from the use of power tools) and
thoracic outlet obstruction (e.g. cervical rib).
Progress to fingertip ulceration, and necrosis .
Significant pain
Need investigation
Need treatment :avoid exposure to cold
The fingers must be protected from trauma,
Antibiotics requires to treatment infection
Sympathectomy .
Prostacyclin infusions
06/07/2017
24
Burger's Disease
(Thromboangiitis Obliterans)
Clinical Features
- Males <45 years
- Upper and lower limb involvement
- Heavy smokers
- It is most common in those from the Mediterranean and North
Africa. It characteristically affects distal arteries, giving rise to
claudication in the feet or rest pain in the fingers or toes
- Disease also affects the veins, giving rise to superficial
thrombophlebitis
Diagnosis: Angiogram
Major limb amputation is the most frequent outcome if patients
continue to smoke(Choice cigarette or your limb)
06/07/2017
25
Diseases of the aorta
Aneurysm, dissection
Aneurysm: This is an abnormal dilatation of the
aortic lumen; a true aneurysm involves all the layers
of the wall, whereas a false aneurysm does not
06/07/2017
26
06/07/2017
Dr Habib Tareif, FRCSI
27
Aetiology
Atherosclerosis
Hypertension
-Families and genetic factors
-Infection -syphilis (saccular aneurysms) .
aortitis include Takayasu's disease , Reiter's syndrome
giant cell arteritis and ankylosing spondylitis
Marfan's syndrome (autosomal dominant trait and is
caused by mutations in the fibrillin gene on chromosome
15. Affected systems include the skeleton (arachnodactyly,
joint hypermobility, scoliosis, chest deformity and high
arched palate), the eyes (dislocation of the lens) and the
cardiovascular system (aortic disease and mitral
regurgitation).
06/07/2017
28
Types of aneurysm, investigation & treatment
Types : abdominal(mass) ,thoracic(high pressure +aortic
regurgitation)
Investigations:.
Chest X-ray, ultrasound , echocardiography, MRI or CT
Treatment with β-blockers reduces the rate of aortic dilatation
and the risk of rupture.
Elective replacement of the ascending aorta
06/07/2017
29
06/07/2017
Dr Habib Tareif, FRCSI
30
Abdominal aortic aneurysms (AAAs)
AAAs are present in 5% of men aged over 60 years and 80% are
confined to the infrarenal segment.
Men are affected three times more commonly than women.
The usual age at presentation is 65-75y
.
Ultrasound is the best way of establishing the diagnosis and of
following up
CT provides more accurate information about the size and extent
of the aneurysm,.
06/07/2017
31
06/07/2017
Dr Habib Tareif, FRCSI
32
Aortic dissection
A tear of the aortic wall(intima) allows arterial blood to
enter the media, which is then split into two layers,
creating a 'false lumen' alongside the existing or 'true
lumen'. The aortic valve may be damaged and the
branches of the aorta may be compromised.
Disease of the aorta and hypertension are the most
important aetiological factors..
It may also rupture into the left pleural space or
pericardium with fatal consequences..
The peak incidence is in 60-70 y (Occur in younger in
marfan sydrome,pregnancy ,truma )
06/07/2017
Men
are twice as frequently affected as women.
33
06/07/2017
Dr Habib Tareif, FRCSI
34
Types
Aortic dissection is classified anatomically and for
management purposes into type A and type B
( regarding debakey and stanford classification)
Type A dissections account for two-thirds of cases and
frequently also extend into the descending aorta.
06/07/2017
35
06/07/2017
Dr Habib Tareif, FRCSI
36
Factors that may predispose
to aortic dissection
Hypertension (80% of cases)
Aortic atherosclerosis
Aortic coarctation
Collagen disorders (e.g. Marfan's syndrome, Ehlers-Danlos
syndrome)
Fibromuscular dysplasia
Previous aortic surgery (e.g. CABG, aortic valve replacement)
Pregnancy (usually third trimester)
Trauma
Iatrogenic (e.g. cardiac catheterisation, intra-aortic balloon
pumping)
06/07/2017
37
Clinical features
Involvement of the ascending aorta typically gives rise to
anterior chest pain, and involvement of the descending
aorta give rise to intrascapular pain.
The pain is typically described as 'tearing' and very abrupt
in onset; collapse is common..
There may be asymmetry of the brachial, carotid or femoral
pulses and signs of aortic regurgitation. Occlusion of
aortic branches may cause MI (coronary), stroke (carotid)
paraplegia (spinal), mesenteric infarction with an acute
abdomen (coeliac and superior mesenteric), renal failure
(renal) and acute limb (usually leg) ischaemia.
06/07/2017
38
Investigations
The chest X-ray (wide medistinum ,left-sided pleural
effusion )
The ECG -left ventricular hypertrophy in patients with
hypertension, or rarely changes of acute MI (usually
inferior).
Doppler echocardiography ( aortic regurgitation, a dilated
aortic root and, occasionally, the flap of the dissection).
Transoesophageal echocardiography
CT and MRI angiography are both highly specific and
sensitive.
06/07/2017
39
Management
The early mortality of acute dissection is approximately
1-5% per hour so treatment is urgently required.
Initial management comprises pain control and
antihypertensive treatment(labetelol alfa and beta
,sodium nitruoprusside ,nicardipin ,ACEI.)
Endoluminal repair or implanting a stent graft placed
from the femoral artery
Type A dissections require emergency surgery to replace
the ascending aorta.
Type B aneurysms are treated medically unless there is
actual or impending external rupture, or vital organ (gut,
kidneys) or limb ischaemia, as the morbidity and
40
06/07/2017
mortality associated with surgery is very high.
Thank you
Any Questions???