* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download facial nerve and
Survey
Document related concepts
Transcript
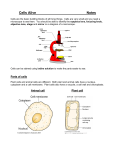
ENT related PN system DR. MOHAMMAD ALSALEM Olfactory nerve (I) Damage can cause an inability to smell (anosmia), a distortion in the sense of smell (parosmia), or a distortion or lack of taste Intensely smelling substances, for example ammonia, may lead to the activation of pain receptors (nociceptors) of the trigeminal nerve that are located in the nasal cavity the nerve (actually many small nerve fascicles) travels up through the cribriform plate of the ethmoid bone to reach the surface of the brain Located in upper 1/3 of nasal cavity in the posteriodorsal recess (inferior surface of the cribriform fossa) + superior part of the nasal septum(10mm) & superiomedial part of superior turbinate primary olfactory neurons; (olphactory receptor neurons) bipolar in shape; non-motile cell has single odor receptor (not specialized as other senses) Lesions to the olfactory nerve can occur because of "blunt trauma", such as coup-contra-coup damage, meningitis, and tumors of the frontal lobe. Decreases in the ability to smell is a normal consequence of human aging, and usually is more pronounced in men than in women Other causes of loss of smell: Upper respiratory tract infection (e.g., sinusitis or the common cold, Nasal polyps, Hypothyroidism Exposure to a chemical that burns the inside of the nose Radiation therapy to the head and neck Kallmann syndrome (hypogonadotropic hypogonadism +anosmia) General features Adaptation to odor can occur within 1-5 min If two odors were mixed the sum of the intensity will be less than the two individually perceived intensities and is dominated by the stronger component. Cross adaptations are present between odors at high concentrations, whereas cross facilitations occur near threshold values Odor association tend to stay longer in the memory than the associations from other senses Olfaction helps two aspects of eating: the recognition of food types and the initiation of digestion Females are better in odor identification than men. Female sense of odor is more acute at ovulation & less during menstruation. Trigeminal Nerve (V) The sensory function of the trigeminal nerve is to provide tactile, proprioceptive, and nociceptive afference to the face and mouth. Its motor function activates muscles of mastication: the masseter, the temporalis and the medial and lateral pterygoids. The other four muscles are the tensor veli palatini, the mylohyoid, the anterior belly of the digastric and the tensor tympani The branch Foramen Compartment Function Ophthalmic Superior orbital fissure Orbital cavity Sensation ( somatic afferent); orbit + face Conveys parasympathetic • from oculomotor (III) via ciliary branch to ciliary muscles • through the lacrimal nerve Maxillary Foramen rotundum Pterygoplatine fossa Mandibular Foramen ovale Infratemporal fossa Sensation : palate + nose + face Conveys parasympathetic from: greater petrosal (VII) To the nose + lacrimal gland Sensation: mandibule + ear Taste via lingual nerve: anterior 2/3 of the tongue (in a communication with chorda tympani) Parasympathetic :parotid gland Motor: muscles of mastication + floor of mouth + tensors THE CORNEAL REFLEX The afferent limb of the reflex is via the nasociliary nerve the efferent limb is via the facial nerve. A pointed wisp of cotton wool should be used. The examiner should ask the patient to look upwards, then resting the hand on the patient's cheek, The wisp should be applied to the lower cornea but taking care not to bring it into vision or a blink reflex will result. The patient will flinch, the eyeball will roll up and the eye will attempt to close. Facial Nerve (VII) The facial muscles include: Occipitofrontalis muscle, Temporoparietalis muscle, Procerus muscle, Nasalis muscle, Depressor septi nasi muscle, Orbicularis oculi muscle, Corrugator supercilii muscle, Depressor supercilii muscle, Auricular muscles (anterior, superior and posterior), Orbicularis oris muscle, Depressor anguli oris muscle, Risorius, Zygomaticus major muscle, Zygomaticus minor muscle, Levator labii superioris, Levator labii superioris alaeque nasi muscle, Depressor labii inferioris muscle, Levator anguli oris, Buccinator muscle, Mentalis Platysma. The platysma is innervated by the facial nerve. Although it is mostly in the neck and can be grouped with the neck muscles by location, it can be considered a muscle of facial expression due to its common innervation. The stylohyoid muscle, stapedius and posterior belly of the digastric muscle Facial Nerve (VII) The facial nerve is made of 10,000 fibers (7000 mylinated motor, 3000 unmylinated sensory & parasympathetic) Location of facial nerve related nucleus: 1 Facial Motor nucleus: in the caudal end of the pons 2 Superior salivatory nucleus 3 Nucleus solitarus: medulla Note that the facial nerve emerge at the ponto-medullary junction The facial nerve is made of: 1. facial nerve proper: input from facial motor nucleus special visceral efferent fibers (motor): (efferent) Posterior belly of digastrics muscle Stylohyoid muscle Muscles of facial expressions (including Masseter muscles) 2. nervus intermedius (nerve of wrisberg) Gives chorda tympani branch, parasympathetic Exists the Brain stem adjacent to the motor branch of the facial nerve Joins the VII nerve as it approaches the Internal auditory canal to form the common Facial nerve •General Visceral motor: input from Superior salivatory nucleus (efferent) •Greater superficial petrosal •Lacrimal gland •Nasal glands •Palatine glands •Chorda tympani Submandibular gland Sublingual gland Minor salivary gland General sensory: input into nucleus solitarus (afferent) Auricular concha External auditory canal Tympanic membrane Special Visceral sensory: (input into nucleus solitarus) (afferent) Greater superficial petrosal :Taste from Soft palate Chordi tympani: Taste from the anterior 2/3 of the tongue Pathway Intracranial part 1-CP < 2-Meatal segment (IAC) Intratemporal/ intrepetrous part (within the fallopian canal) Peri-ganglionic 3-labyrinthine /proximal segment 4-tympanic/ horizontal segment 5-mastoid /vertical segment 6-Extracranial part (parotid) Facial Nerve Paralysis Ramsay Hunt syndrome /Herpes zoster oticus PATHOLOGY The disease is a reactivated varicella zoster infection (chicken pox) from dormant viral particles resident in the geniculate ganglion of the facial nerve and the spiral and vestibular ganglia of VIII Symptoms: • Auricular pain: the 1st symptom to appear • Vesicular Rash: •location: 1.concha 2.posteriomesial surface of the auricle (postauricular) 3.EUC 4.mucosa of the palate 5.anterior 2/3 of the tongue • Facial nerve palsy • VIII may be involved in the form of hearing loss (SNHL), vertigo and or tinnitus. Vestibulocochlear (VIII) Cochlear system Organ of corti: Specialized epithelium (sensory receptor for sound) Located within the inner part of the basilar membrane Hair cells of organ of corti Number of rows Total number Function Afferent innervations % Inner hair cells 1 row 3.000 principal transducer of motion from the basilar membrane to a nerve impulse (Send information about hearing to the brain) 90% Outer hair cells 3 rows up to 5 in humans 12.000 Cochlear amplifier: amplify motion from the basilar membrane at the point of maximum response (which increase sensitivity, frequency & selectivity) controlling and fine tuning mechanisms 10% Summary of the Pathway for sound Sound waves in the air enter the outer ear canal. Vibration of the tympanic membrane is transmitted through the chain of three (3) ossicles (which amplify the sound 20 X) to the oval window. Vibration of the oval window induces pressure waves in the perilymph of the scala vestibuli. Vibration of the vestibular (Reissner's) membrane transfers pressure waves from perilymph to the endolymph of the scala media (cochlear duct). Pressure waves of the endolymph induce the basilar membrane to vibrate, induces a shearing of the apical ends of the hair cells against the tectorial membrane. This will bend the bundle of stereocilia on each hair cell resulting in the bending of the bundle of stereocilia and the opening of mechanically gated ion channels in the membrane of the stereocilia Influx of K+ ions, depolarizing the hair cell, which releases neurotransmitters. This results in an action potential being propagated along nerve fibers of sensory neurons in the spiral ganglion. The vestibular system Components of the vestibular system The semicircular canals are concerned with the rotation the saccule and utricle with gravitation (vertical) Benign positional vertigo One of the most common types of peripheral vertigo BPPV occurs because a semicircular canal has otoconia (originating from the macula of the gravity-sensitive Utricle) either: attached to the cupula (cupulolithiasis) free floating in the endolymph (canalolithiasis) The majority of BPPV is due to debris in the posterior canal, but debris may also enter the horizontal and superior semicircular canals. ESSENTIALS OF DIAGNOSIS 1. Sudden vertigo lasting seconds with certain head positions. 10–20 seconds 2. No associated hearing loss. 3. Characteristic nystagmus (latent, geotropic, fatigable) with Dix-Hallpike test. Primary idiopathic endolymphatic hydrops (known as Ménière’s disease) is of unknown etiology ESSENTIALS OF DIAGNOSIS • Episodic vertigo lasting hours. • Fluctuating hearing loss. • Tinnitus. • Aural pressure. (fullness) Sudden Sensorineural Hearing Loss (SSNHL) Definition: ≥ 30 dB SNHL in at least 3 adjacent frequencies that occurs over ≤ 3 days most commonly no etiology found (idiopathic SSNHL) 85%,theories: viral infection: atrophy of tectorial membrane autoimmune perilymphatic fistula vascular ischemia:reduce O2 tension in stria vascularis DRUGS Temporary vs permenant hearing loss: permanent (hearing loss/vestibular dysfunction): Anti-neoplastic: cistaplatine/carboplatine Amingogylcoside vancomycin temporary (hearing loss): Aspirin Macrolide: erythromycin Quinine Temporary MAQ temporary/permanent: Permanent CAVe Diuretics: can cause both; in neonates it cause permanent hearing loss The main drugs that cause vestibulotoxicity: streptomycin gentamycin minocylcline (tetracycline) Temporary/Permanent Di The glossopharyngeal nerve (IX) Function Afferent fibers Somatic sensation Special sensation Visceral sensation Efferent fibers Visceral Special visceral (branchiogenic) Post 1/3 of tongue, tonsils, soft palate Naso + oropharynx ( pharyngeal plexus) Ear: Ant 1/3 Skin of EUC Internal surface of T.M, Mucosa of middle ear(tympanic plexus) bony part of ET Taste from the post 1/3 of the tongue Carotid body Carotid sinus Presynaptic parasympathetic fibers to parotid gland Motor fibers to stylopharyngeaus muscle Gag reflex: Brisk and brief elevation of the soft palate and bilateral contraction of pharyngeal muscles evoked by touching the posterior pharyngeal wall, the soft palate or posterior part of the tongue It prevents something from entering the throat except as part of normal swallowing and helps prevent choking. Afferent fibers Nerve Glossopharyngeal nerve Efferent fibers Vagus nerve Vagus nerve (X) clinical ENT relations loss of auricular sensation at the concha & anti helex auricular branch pharyngeal branch nasal reguragtaion during swallowing external branch of the superior laryngeal nerve Recurrent laryngeal nerve deviated Uvula dysphagia stridor horsness of voice Aphonia reffered pain from the laryngeal ca paralysed v.c unilateral/ bilateral Vagus nerve relation to the pharynx & larynx Pharyngeal branch which contributes to the pharyngeal plexus*) External branch of the superior laryngeal nerve pharyngeal and palate muscles except tensor palati muscle (trigiminal) stylopharyngeaus (glossopharyngeal) Cricothyroid muscle Recurrent laryngeal nerve all internsix muscle of the larynx except the cricothyroid muscle 1-Pharyngeal muscles: 3 constrictor muscles salpingopharyngeus palatoglossus 2-palate muscle: levator palati muscle palatoglossus palatopharyngeus all intrinsic muscles recieves unilateral innervation except interarytenoid •Somatic motor pathway of the vagus nerve •Pharyngeal plexus is made up of Vagus & Glossopharyngeal & sympathetic plexus •Somatic (cutenous sensation): •Cutenous sensation from the back of the auricle & posterior external auditory canal •General Visceral Sensation: •Common sensation from the larynx & pharynx is to the spinal nucleus of the trigeminal •Special ( taste) Visceral sensation: •Sensation of taste from the pharynx, vallecula, tongue base, epiglottis Hypoglossal Nerve (XII) It receives: •sympathetic fibres from the superior cervical ganglion •some fibres from the vagus •motor roots of Cl and C2 via the ansa cervicalis. Motor fibres derived from the: hypoglossal nucleus itself supply intrinsic & extrinsic muscles of the tongue except the palatoglossus •The fibres derived from the C 1 components supply Suprahyoid muscles XIIth nerve lesion •paralyses one side of the tongue •the larynx also pulls across to the opposite side on swallowing, because the hyoid fails to elevate on the paralyzed side.