* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download needle emg examination of the foot
Survey
Document related concepts
Transcript
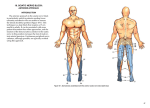
NEM AA P HO RKS WO N O I T OT A N I AM HE FO X E G OF T M E E L D NEE MD , o r o Del T MD . R David A. Park, Tracy AMERICAN ASSOCIATION OF NEUROMUSCULAR & ELECTRODIAGNOSTIC MEDICINE 2621 Superior Drive NW Rochester, MN 55901 (507) 288-0100 [email protected] www.aanem.org AMERICAN ASSOCIATION OF NEUROMUSCULAR & ELECTRODIAGNOSTIC MEDICINE Workshop handouts are prepared as background didactic material to complement a hands-on workshop session. This workshop handout was originally prepared in September 2000 and revised in September 2008. The idea and opinions in this publication are solely those of the author(s) and do not necessarily represent those of the AANEM. Copyright © September 2000 AMERICAN ASSOCIATION OF NEUROMUSCULAR & ELECTRODIAGNOSTIC MEDICINE 2621 Superior Drive NW Rochester, MN 55901 Needle EMG Examination of the Foot David R. Del Toro, MD Department of Physical Medicine and Rehabilitation Medical College of Wisconsin Milwaukee, Wisconsin Tracy A. Park, MD Medical Rehabilitation Associates Milwaukee, Wisconsin INTRODUCTION The intrinsic muscles of the foot are affected by a wide variety of neurogenic disorders, including peripheral polyneuropathy, lumbosacral radiculopathy/plexopathy, and entrapment/compression mononeuropathies of the sciatic, deep peroneal, and tibial nerves. Although this discussion addresses the technical aspects of needle electromyography (EMG) examination of the foot, the approach to this technique will be presented in terms of entrapment neuropathies within the foot. Needle EMG examination of the intrinsic muscles of the foot is perhaps the most under-utilized of all the tools available to electrodiagnostic medicine (EDX) consultants. There are several reasons for this. One is that several published articles have reported the common occurrence of prolonged insertional activity in the intrinsic foot muscles of normal subjects.7,8,27 These findings were refuted by Dumitru et al in a later study, which found true abnormal spontaneous activity in 2% of 50 healthy, asymptomatic subjects.7 A second reason is that many EDX consultants believe that needle examination of the foot muscles isprohibitively painful to the patient. However, most EDX consultants routinely insert needle electrodes into a variety of hand muscles, even though this procedure often elicits more pain in the hand muscles than it does in the foot muscles. And finally, many EDX consultants are uncomfortable with the technique and interpretation of needle EMG examination of the foot muscles. This is because, in the majority of institutions, there is so little time and attention dedicated to this topic by residency/fellowship training programs and continuing medical education programs. This workshop addresses the last of these reasons, with the hope that the participants will develop an understanding of the anatomic principles, electrophysiologic approach and technique, and clinical interpretation of needle EMG examination of the foot. ANATOMY With the exception of the extensor digitorum brevis (EDB), which is innervated by the deep peroneal nerve (L5/S1), the intrinsic muscles of the foot receive their nerve supply from three branches of the tibial nerve: the medial plantar nerve (MPN), the lateral plantar nerve (LPN), and Baxter’s nerve (more formally referred to as the inferior calcaneal nerve or the 1st branch of the LPN). All of these tibial nerve branches carry fibers from the S1 and S2 nerve roots. Tibial Nerve At the level of the medial malleolus, the tibial nerve lies within the tarsal tunnel, deep to the flexor retinaculum (Figure 1), and is encased within a tunnel along with the remainder of the tibial neurovascular bundle. There is a distinct compartment for the tibial nerve within the upper tarsal tunnel which is a site of potential compression of the tibial nerve itself or one or more of the tibial nerve branches. This compartment is formed by the calcaneal attachment of the deep aponeurotic segment of the flexor retinaculum.24 2 Needle EMG Examination of the Foot In 93 - 95% of feet, the MPN and LPN branch off the tibial nerve within the tarsal tunnel.6,12 (For the purposes of EDX testing, it is helpful to think of the tibial nerve as actually having 4 terminal branches: the MPN, the LPN, Baxter’s nerve, and the medial calcaneal nerve.19) The first three of these carry motor fibers and are described below. The fourth branch (the medial calcaneal nerve) is purely sensory and will not be discussed here. In the lower tarsal tunnel, still at the level of the calcaneus, the tunnel for the tibial nerve divides into upper and lower calcaneal chambers that are separated by the interfascicular septum. (Figure 1) The interfascicular septum is actually a segment of the deep fascia of the abductor hallucis extending towards its attachment to the medial aspect of the calcaneus. The upper calcaneal chamber contains the MPN, while the lower calcaneal chamber houses the LPN. These calcaneal chambers represent a second site of entrapment of the individual plantar nerves. Although Baxter’s nerve initially enters the lower chamber, it follows a different course from that of the plantar nerves, veering to penetrate the posterior aspect of this chamber and traveling laterally across the foot anterior to the calcaneus.24 Therefore, unlike the plantar nerves, Baxter’s nerve does not tend to be entrapped in the calcaneal chambers. Medial Plantar Nerve (MPN) After exiting the upper calcaneal chamber, the MPN travels into the sole of the foot via the abductor canal,24 which is formed by the attachment of the abductor hallucis to the talus and navicular.16,17,21 The abductor canal is another known entrapment site of the MPN.16,17,21 The MPN innervates the abductor hallucis, flexor hallucis brevis (medial and lateral heads), flexor digitorum brevis, and 1st lumbrical. Lateral Plantar Nerve (LPN) The LPN leaves the lower calcaneal chamber and passes into the sole of the foot through its own abductor canal, which (like that of the MPN) is formed by the attachment of the abductor hallucis to the talus and navicular. The abductor canal of the LPN is a potential entrapment site for this nerve as well. The LPN then passes in an oblique fashion laterally and distally across the foot, sandwiched between the flexor digitorum brevis (on the plantar side) and the quadratus plantae (on the dorsal side).24 After piercing the lateral intermuscular septum, the LPN divides into its terminal superficial and deep branches, opposite the base of the 5th metatarsal.24 The LPN provides motor innervation to the quadratus plantae, flexor digiti minimi brevis, flexor hallucis brevis (lateral head), adductor AANEM Workshop hallucis, all interossei, and the second through fourth lumbricals.24 It should be noted that the medial branch of the deep peroneal nerve may frequently send motor twigs to the dorsal interossei.1 MCN Baxter’s nerve Figure 1: Schematic drawing of the medial aspect of a right foot, illustrating the tarsal tunnel and the tibial nerve with its four terminal branches. (TN, tibial nerve; MCN, medial calcaneal nerve; Baxter’s nerve; QP, quadratus plantae muscle; LPN, lateral plantar nerve; MPN, medial plantar nerve; IFS, interfascicular septum; AH, abductor hallucis muscle; FR, flexor retinaculum). Baxter’s Nerve (Inferior Calcaneal Nerve; 1st branch of LPN) Baxter’s nerve, originally named the inferior calcaneal nerve when it was first described by Roegholt in 1940,22 has also been referred to as “the first branch of the lateral plantar nerve,”23 “the muscle branch of the lateral plantar nerve,”19 or “the nerve to the abductor digiti quinti.”11 In the upper tarsal tunnel, Baxter’s nerve arises either from the tibial nerve prior to the MPN/LPN bifurcation, or from the LPN itself just after its origin.24 After passing through the posterior segment of the lower calcaneal chamber, Baxter’s nerve heads inferiorly between the deep fascia of the abductor hallucis and the underlying quadratus plantae.24 As it passes the quadratus plantae, Baxter’s nerve takes a sharp turn toward the lateral side of the foot. It follows a horizontal and transverse course immediately anterior to the medial aspect of the calcaneal tuberosity while passing between the overlying flexor digitorum brevis and the underlying quadratus plantae.24 (Figure 2) Baxter’s nerve can be compressed between the quadratus plantae and abductor hallucis,2,4,20,23 or by a heel spur at the medial AANEM Workshop Needle EMG Examination of the Foot calcaneal tuberosity.4,16,20,26 (In the authors’ experience, Baxter’s nerve is the most commonly entrapped nerve in the foot.) Baxter’s nerve always terminates with motor branches to the abductor digiti quinti pedis, and may send motor branches to the quadratus plantae and flexor digitorum brevis.2,5,18,20,23 3 interossei (10.5% in the second; 2.6% in the third).1 Either or both DPN branches can become entrapped beneaththe inferior extensor retinaculum, causing the socalled ‘anterior tarsal tunnel syndrome.’ Baxter's Nerve Figure 3: Schematic drawing of the terminal course of the deep Figure 2: Schematic drawing of the posterior view of the heel showing how Baxter’s nerve can be entrapped between the abductor hallucis and the medial edge of the quadratus plantae. At this site, Baxter’s nerve is particularly vulnerable to excessive traction during pronation. (Used with permission from Schon LC, Baxter DE. Heel pain syndrome and entrapment neuropathies about the foot and ankle. In: Gould JS, editor. Operative foot surgery. Philadelphia: WB Saunders; 1994. p 193.) peroneal nerve (DPN). Note that the DPN typically divides above the inferior extensor retinaculum into a medial branch, which innervates the first dorsal web space, and a lateral branch, which innervates the extensor digitorum brevis. (Adapted with permission from Liveson JA. In: Peripheral neurology: case studies in electrodiagnosis, 2nd edition. Philadelphia: FA Davis; 1991. p 53.) Deep Peroneal Nerve NEEDLE EMG EXAMINATION OF SELECTED FOOT MUSCLES After branching from the common peroneal nerve just distal to the fibular neck, the deep peroneal nerve (DPN) courses between the muscle layers of the anterior compartment on its way to the foot. The DPN then divides into medial and lateral branches 1.3 cm proximal to the ankle joint.12 Both of these branches then pass deep to the inferior extensor retinaculum. (Figure 3) The medial branch supplies cutaneous innervation to the first dorsal web space, while the lateral branch provides the motor innervation to the extensor digitorum brevis. (Figure 3) In addition, the edial branch of the DPN may frequently provide some innervation to the dorsal interossei.1 A recent anatomic study reported a 92.1% incidence of DPN motor branches to the first dorsal interosseus pedis, with the incidence falling off sharply in a medial-to-lateral manner in the remaining dorsal Needle EMG examination of various intrinsic foot muscles is a useful tool in the EDX consultant’s armamentarium and can yield extremely valuable information to assist in developing the EDX impression. Unfortunately, most EDX consultants are comfortable with needle EMG examination of only a couple of the intrinsic foot muscles (i.e., extensor digitorum brevis and first dorsal interosseus pedis). Even widely used reference books for needle EMG techniques include only a very limited number of intrinsic foot muscles.10 The following section will describe in detail how to perform needle EMG examination of numerous intrinsic foot muscles along with their most likely peripheral innervation pattern. 4 Needle EMG Examination of the Foot Due to individual variation in dexterity and coordination of the different intrinsic foot muscles, an EDX consultant may not always be able to evaluate the selective voluntary recruitment of early individual motor units (i.e., first-, second-, or third-order motor units). However, one should be able to elicit multiple voluntary motor units and possibly evaluate the interference pattern of these motor units by simple telling the patient, “Try to wiggle your toes.” First Dorsal Interosseus Pedis (FDIP) The first dorsal interosseus pedis (FDIP) is innervated by the LPN (although it often receives a branch from the DPN as well).1 For needle EMG examination of the FDIP, the needle electrode is inserted into the first dorsal web space immediately proximal to the first and second metatarsal heads, with the tip angled slightly toward the heel. (Figure 4) This angle will direct the EMG needle into the mid-shaft level of the metatarsals, where the space between these bones is the widest. The first muscle encountered by the needle electrode in this space will be the FDIP. To confirm needle electrode placement into the FDIP, the patient can recruit this muscle by attempting resisted abduction and/or flexion of the first and second toes. Needle EMG examination of the FDIP should then proceed with investigation of the muscle’s insertional activity, spontaneous activity, motor unit recruitment, and motor unit action potential morphology. Figure 4: Needle electrode placement for EMG examination of first dorsal interosseus pedis (FDIP). The needle electrode is inserted into the first dorsal web space immediately proximal to the first and second metatarsal heads, and is angled toward the heel. This angle will direct the EMG needle into the mid-shaft level of the metatarsals, where the space between these bones is the widest. Fourth Dorsal Interosseus Pedis (Fourth DIP) The fourth dorsal interosseus pedis (fourth DIP) is innervated by the LPN, exclusively. Needle electrode insertion is similar to the FDIP technique, with the electrode inserted into the fourth dorsal web space immediately proximal to the fourth and fifth metatarsal heads. (Figure 5) Again, the needle electrode AANEM Workshop is angled toward the heel to direct it into the space between the metatarsal shafts. The first muscle encountered by the needle electrode in this space will be the fourth DIP. Needle electrode placement is confirmed by having the patient recruit the fourth DIP with resisted abduction and/or flexion of the fourth and fifth toes. Alternatively, the EDX consultant can place a finger between the fourth and fifth toes and then have the patient attempt resisted adduction of these toes. Needle EMG examination of the fourth DIP can then proceed in the usual fashion as described for the FDIP. Figure 5: Needle electrode placement for EMG examination of fourth dorsal interosseus pedis (fourth DIP). The needle electrode is inserted into the 4th dorsal web space immediately proximal to the fourth and fifth metatarsal heads. The needle electrode is angled toward the heel to direct it into the space between the metatarsal shafts. Flexor Digiti Minimi Brevis (FDMB) The flexor digiti minimi brevis (FDMB) is the short flexor of the little toe. Like the fourth DIP, it is exclusively innervated by the LPN. The needle electrode is inserted at the lateral aspect of the forefoot at the midpoint of the 5th metatarsal shaft. (Figure 6) The needle tip should pierce the thinner dorsal skin (immediately superior to the border of the plantar skin). The needle electrode is directed across the foot, just inferior to the 5th metatarsal shaft. Needle electrode placement is confirmed by having the patient flex the toes. Needle EMG examination of the FDMB can then proceed in the usual fashion as described for the FDIP. Abductor Digiti Quinti Pedis (ADQP) The abductor digiti quinti pedis (ADQP) is always innervated by Baxter’s nerve.19 For needle EMG examination of the ADQP, the needle electrode tip is inserted at (or up to about 0.5 cm superior to) the junction of the dorsal and plantar skin (so the tip pierces the thinner dorsal skin, and not the thick plantar skin) and approximately 1 to 2 fingerbreadths proximal to the base of the 5th metatarsal. (Figure 7) The electrode shaft should be directed posteriorly at about a 45-degree angle, an orientation that will guide it into the bulk AANEM Workshop Needle EMG Examination of the Foot of the ADQP muscle belly. The needle electrode is then advanced until insertional activity of the muscle is detected. Needle electrode placement in the ADQP is confirmed by having the patient abduct and/or flex the fifth toe against resistance. If the patient is unable to do this, the examiner can place a finger against the lateral side of the fifth toe and have the patient externally rotate the foot against this resistance; the ADQP should contract automatically in order to stabilize the fifth toe. Needle EMG examination of the ADQP then proceeds in the usual manner. 5 Abductor Hallucis (AH) The abductor hallucis (AH) is innervated by the MPN. Needle EMG examination of the AH begins with palpation of the muscle belly just posterior and inferior to the navicular tuberosity. The needle electrode is inserted about 2 cm posterior to the navicular tuberosity, at (or immediately superior to) the junction of the dorsal and plantar skin. (Figure 8) The electrode shaft can be directed posteriorly (at about a 45-degree angle) or slightly distally. When advancing the needle electrode, one must be cognizant of the medial and lateral plantar nerves which are nearby but deep to the AH. After observing insertional activity of the muscle, the EDX consultant can confirm needle electrode placement by having the patient attempt abduction and/or flexion of the first toe. Alternatively, the examiner can place a finger against the lateral side of the first toe and have the patient internally rotate the foot against this resistance; the AH should contract automatically in order to stabilize the first toe. Needle EMG examination of the AH an then proceed in the usual fashion. Figure 6: Needle electrode placement for EMG examination of flexor digiti minimi brevis (FDMB). The needle electrode is inserted at the lateral aspect of the forefoot at the midpoint of the 5th metatarsal shaft. The needle tip should pierce the thinner dorsal skin (immediately superior to the border of the plantar skin).The needle electrode is directed across the foot, just inferior to the 5th metatarsal shaft. Figure 7: Needle electrode placement for EMG examination of Figure 8A and 8B: Needle electrode placement for EMG abductor digiti quinti pedis (ADQP). The needle electrode tip is inserted at (or immediately superior to) the junction of the dorsal and plantar skin (so the tip pierces the thinner dorsal skin) and approximately 1 to 2 fingerbreadths proximal to the base of the 5th metatarsal (see mark in figure). The electrode shaft should be directed posteriorly at about a 45-degree angle, an orientation that will guide it into the bulk of the ADQP muscle belly. examination of abductor hallucis (AH). The needle electrode is inserted about 2 cm posterior to the navicular tuberosity, at (or immediately superior to) the junction of the dorsal and plantar skin (the needle tip piercing the thinner dorsal skin). The electrode shaft can be directed posteriorly at about a 45-degree angle (A), or slightly distally (B). When advancing the needle electrode, one must be cognizant of the medial and lateral plantar nerves which are nearby but deep to the AH. 6 Needle EMG Examination of the Foot AANEM Workshop Figure 9A and 9B: Needle electrode placement for EMG examination of extensor digitorum brevis (EDB). The needle electrode tip is inserted into the lateral edge of the EDB at the midpoint of the muscle belly (A). If there is little or no palpable EDB muscle mass, the needle electrode is inserted about 2 cm posterior and 2 cm superior to the base of the fifth metatarsal. The bellies of the EDB lie lateral to and deep to the tendons of the extensor digitorum longus. An attempt should be made to explore all four muscle bellies by directing the needle electrode in a very shallow angle medially across the foot (B), thereby allowing the needle to pass just deep to the long extensor tendons. Extensor Digitorum Brevis (EDB) The extensor digitorum brevis (EDB) is innervated by the DPN. Prior to needle electrode insertion, the EDB muscle mass is palpated to determine its lateral edge. The needle electrode tip is inserted into the lateral edge of the EDB at about the midpoint of the muscle belly. (Figure 9) If there is little or no palpable EDB muscle mass, the needle electrode is inserted about 2 cm posterior and 2 cm superior to the base of the fifth metatarsal. The bellies of the EDB lie lateral to and deep to the tendons of the extensor digitorum longus. An attempt should be made to explore all four bellies by directing the needle electrode in a very shallow angle medially across the foot, thereby allowing the needle to pass to the long extensor tendons, where the two most medial bellies are located. Needle electrode placement into the EDB is easily confirmed by having the patient gently and slowly extend the toes. Needle EMG examination of the EDB can then proceed in the usual manner. DISCUSSION The needle EMG examination of intrinsic foot muscles is critical in the EDX evaluation of the foot. 14,25 Unfortunately, several published and widely recognized studies have reported abnormally prolonged insertional activity in the intrinsic muscles in a significant percentage of normal feet.7,8,27 However, none of these studies have been able to demonstrate spontaneous activity, in the form of sustained positive sharp waves or fibrillation potentials, in the intrinsic foot muscles of any normal subjects. In fact, a more recent study by Dumitru et al7 examining the AH and EDB in 50 healthy asymptomatic subjects demonstrated “truly abnormal” spontaneous single muscle fiber discharges (i.e., fibrillation potentials and positive sharp waves) in only 2% (1/50 feet). To explain the findings in the previous studies,7,8,27 Dumitru et al concluded: “It is likely that the previously reported high prevalence of spontaneous activity in healthy persons resulted from not fully appreciating the similarity between innervated and denervated spontaneous single muscle fiber discharge configurations.” 7 In addition, none of these earlier studies have included nerve conduction studies (NCS) on the nerves of the ‘normal’ feet to assess for subclinical or asymptomatic nerve dysfunction.7,8,27 However, despite the flaws in these reports, many EDX consultants avoid performing needle EMG examination on intrinsic foot muscles, since they are uncertain of how to interpret any observed abnormalities or how such abnormalities might be diagnostically useful. The authors have consistently found needle EMG abnormalities (i.e., sustained positive sharp waves and fibrillation potentials) to be the most frequent ‘positive’ finding in the electrophysiologic evaluation of patients with suspected entrapment neuropathies in the foot−‘positive’ not in a random manner, but in a logical way that ‘fits’ the clinical presentation. This experience supports the theory that axonal degeneration is the pathologic mechanism for tarsal tunnel syndrome.14 Furthermore, the authors have found needle EMG examination to be both more specific and AANEM Workshop Needle EMG Examination of the Foot more sensitive than NCSs for diagnosing entrapment neuropathies in the foot. Because the needle EMG abnormalities that have been reported in asymptomatic feet have been quite mild, more prominent findings (i.e., 1+ or greater abnormal spontaneous activity in the form of sustained positive sharp waves and/or fibrillation potentials) must be demonstrated to indicate denervation beyond what would be considered normal ‘wear and tear.’ Additionally, the clinical significance of any abnormal EMG findings in a given intrinsic foot muscle should be corroborated by studying the same muscle in the unaffected foot: asymmetric findings would suggest a focal pathology rather than normal ‘wear and tear’. Just as important as the performance of the needle EMG examination of the intrinsic foot muscles is the decision of which muscles to explore in a given patient. It must be realized that examining a single muscle (e.g., the abductor hallucis) to ‘screen’ for the presence of tarsal tunnel syndrome is grossly inadequate, since more distal entrapment of individual tibial nerve branches is a frequent cause of symptoms resembling tarsal tunnel syndrome. Also, neurogenic symptoms in the foot are often vague and poorly localized, so these factors are not always reliable in guiding the examiner to the involved nerve. Adding to this limitation is the fact that entrapment neuropathies in the foot rarely result in complaints of weakness; instead, the symptoms are typically numbness, pain, and/or paresthesias. Therefore, weakness is virtually eliminated as a basis for choosing which intrinsic foot muscles to explore. Because intrinsic foot muscles often have needle EMG abnormalities in clinical conditions other than a nerve entrapment in the foot, such as a peripheral polyneuropathy and lumbosacral radiculopathy, it is important to expand the scope of the needle EMG examination to investigate these other possibilities. Abnormalities in a given nerve distribution or muscle should lead to evaluation of intrinsic muscles supplied by a different nerve, and possibly the intrinsic muscles of the opposite foot. Limb muscles proximal to the foot, as well as the lumbosacral paraspinal muscles, may also need to be explored, depending on the overall clinical picture. Ultimately, like any other electrophysiologic information, the results of the needle EMG examination of the intrinsic foot muscles must be considered in conjunction with the patient’s clinical presentation. The history, physical examination, NCSs, and needle EMG examination must all come together to create a logical ‘fit,’ one that makes anatomic and physiologic sense. 7 REFERENCES 1. Akita K, Sakamoto H, Sato T. Lateromedial and dor soplantar borders among supplying areas of the nerves innervating the intrinsic muscles of the foot. Anat Rec 1999;255(4):465-470. 2. Arenson DJ, Cosentino GL, Suran SM. The inferior calcaneal nerve: An anatomical study. J Amer Podiatry Assoc 1990;70:552-560. 3. Baxter DE, Pfeffer GB, Thigpen M. Chronic heel pain:Treatment rationale. Orthop Clin North Amer 1989;20:563-569. 4. Baxter DE, Pfeffer GB. Treatment of chronic heel pain by surgical release of the first branch of the lateral plantar nerve. Clin Orthop Rel Res 1992;279:229-236. 5. Baxter DE, Thigpen M: Heel pain. Operative results. Foot Ankle 1984;5:1625. 6. Dellon AL, Mackinnon SE. Tibial nerve branching in tarsal tunnel. Arch Neurol 1984;41:645-646. 7. Dumitru D, Diaz CA, King JC. Prevalence of denervation in paraspinal and foot intrinsic musculature. Am J Phys Med Rehabil 2001;80:482-490. 8. Falck B, Alaranta H. Fibrillation potentials, positive sharp waves and fasciculation in the intrinsic muscles of the foot in healthy subjects. J Neurol Neurosurg Psychiatr 1983;46:681-683. 9. Gatens PF, Saeed MA. Electromyographic findings in the intrinsic muscles of normal feet. Arch Phys Med Rehabil 1982;63:317-318. 10. Geiringer SR. Anatomic Localization for Needle Electromyography. Hanley & Belfus, Philadelphia, 1993. 11. Hamm JT, Sanders M. Anatomic variations of the nerve to the abductor digiti quinti muscle. Foot Ankle 1987;8:123. 12. Havel PE, Ebraheim NA, Clark SE, Jackson WT, DiDio L. Tibial nerve branching in the tarsal tunnel. Foot Ankle 1988;9:117-119. 13. Horwitz MT. Normal anatomy and variations of the peripheral nerves of the leg and foot. Arch Surg 1938;36:626-636. 14. Kraft GH. Tarsal tunnel entrapment. In: Course E: Entrapment neuropathies. AAEE Ninth Annual Continuing Education Course, Boston. September 25, 1986, pp 13-18. 15. Mackinnon SE, Dellon AL, Daneshvar A. Tarsal tunnel syndrome: Histopathologic examination of a human posterior tibial nerve. Contemp Orthop 1984;9:43-48. 16. Murphy PC, Baxter DE. Nerve entrapment of the foot and ankle in runners. Clin Sports Med 1985;4:753-76368. 17. Oh SJ, Lee KW. Medial plantar neuropathy. Neurology 1987;37:1408-1410 18. Park TA, Del Toro DR. Case report: isolated inferior calcaneal neuropathy. Muscle Nerve 1996;19:106-8. 19. Park TA, Del Toro DR. Electrodiagnostic evaluation of the foot. Phys Med Rehabil Clin N Amer 1998;9:871-896. 20. Przylucki H, Jones CL. Entrapment neuropathy of muscle branch of lateral plantar nerve. J Amer Podiatry Assoc 1981;71:119-124. 21. Rask MR. Medial plantar neurapraxia (“jogger’s foot”): Report of 3 cases. Clin Orthop Rel Res 1978;134:193-195. 22. Roegholt MN. Een nervus calcaneus inferior als overbrenger van de pijn bij calcaneodynie of calcanensspoor en de daaruit volgende therapie. Ned Tijdschr v Geneeskd 1940;84:1898. 23. Rondius JJ, Huson A. The first branch of the lateral plantar nerve and heel pain. Acta Morphol Neerl Scand 1986;24:269. 24. Sarrafian SK. Anatomy of the Foot and Ankle. Philadelphia, JB Lippincott Company, 1983. 25. Spindler HA, Reischer MA, Felsenthal G. Electrodiagnostic assessment in suspected tarsal tunnel syndrome. Phys Med Rehabil Clin N Amer 1994;5:595-612. 26. Tanz SS. Heel pain. Clin Orthop 1963;28:169-177. 27. Wiechers D, Guyton JD, Johnson EW. Electromyographic findings in the extensor digitorum brevis in a normal population. Arch Phys Med Rehabil 1976;57:84-85. NEM AA P HO RKS WO N O I T OT A N I AM HE FO X E G OF T M E E L D NEE MD , o r o Del T MD . R David A. Park, Tracy AMERICAN ASSOCIATION OF NEUROMUSCULAR & ELECTRODIAGNOSTIC MEDICINE 2621 Superior Drive NW Rochester, MN 55901 (507) 288-0100 [email protected] www.aanem.org AMERICAN ASSOCIATION OF NEUROMUSCULAR & ELECTRODIAGNOSTIC MEDICINE