* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Nealon, C
Survey
Document related concepts
Transcript
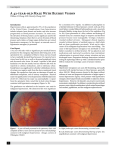
Malignant Hypertension: Is it more common than we think? Cari Nealon, O.D. Abstract This case series describes two patients that presented with ocular complications secondary to malignant hypertension within a three-week period. One presented during the acute phase and the other five months after an undiagnosed crisis. Patient 1: 1. 2. Case History Patient Demographics: 57 year-old African American male Chief complaint: Seeing new black and colored spots in both eyes Ocular history: None (-) glaucoma/ARMD/ocular trauma/ocular surgery Medical history: Hypertension, Chronic Hepatitis C, Type II Diabetes Mellitus, Sleep apnea Medications: Atenolol, HCTZ/Triamterene, Lisinopril Other salient information: The patient has not taken his hypertensive or diabetic medications in over seven months. The emergency department referred the patient to the eye clinic for decreased vision of unknown etiology. His entering blood pressure was 233/149. He was given two IV injections of 10mg hydralazine and one oral dose of 20mg Lisinopril before his eye exam. Pertinent findings Clinical findings Corrected visual acuities were 20/25-2 OD and 20/40+2 OS Extraocular muscle movements, pupils, and color vision were normal OD and OS Slit lamp examination was unremarkable OD and OS Intraocular pressures were normal with readings of 19 mmHg OD and 20 mmHg OS Dilated fundus examination was remarkable for Grade 2 OD and Grade 1 OS optic disc edema, scattered flame hemorrhages and cotton wool spots in all four quadrants OU, 1 disc diameter of macular elevation OS, and moderate vessel tortuosity with nicking and banking defects OD and OS. FDT 24-2 screening visual field was reliable OD and OS. Four superior nasal defects and one superior temporal defect were found OD and two superior nasal paracentral defects OS. Spectralis Optic Disc OCT scans showed optic nerve edema in both OD and OS. Spectralis macular OCT showed normal foveal contour OD and a large area of sub-retinal fluid with associated cystic changes OS Fundus photos were taken to document findings in OD and OS. 3. Physical findings Entering blood pressures at the emergency department were repeatable with readings of 233/149 and 226/150. Blood pressure after the initiation of IV hydralazine was 197/110. Laboratory studies Most recent HbA1c was 6.7 in November 2014. Radiology studies A STAT head CAT scan was performed in the emergency department. No intracranial masses, extra axial collections, hydrocephalus or hemorrhages were found. Differential diagnosis Primary/leading Hypertensive emergency with grade 4 hypertensive retinopathy OU Others Severe non-proliferative diabetic retinopathy 1. Diabetic retinopathy could be contributing but the extremely elevated blood pressure readings and significant amount of cotton wool spots along with flame hemorrhages suggest that hypertension is the primary cause. Patient 2: 1. 2. Case History Patient Demographics: 68 year-old African American male Chief compliant: Mild blurred vision at distance and near in both eyes Ocular history: None (-) glaucoma/ARMD/ocular trauma/ocular surgery Medical history: Hypertension, Chronic sinusitis, Degenerative joint disease, Microscopic hematuria, PTSD, alcohol and cannabis abuse Medications: Nadolol 20mg, Amlodipine besylate 10mg, Lisinopril 40mg, Chlorthalidone 25mg, Meloxicam 15mg, Fluticasone 50mcg 120D nasal inhaler, Gabapentin 300mg Other salient information: He was a new patient to the clinic and his last eye exam was five years ago. Pertinent findings Clinical findings Best corrected visual acuities were 20/25 OD and 20/30 OS Extraocular muscle movements, pupillary testing, FDT screener, and slit lamp examination were unremarkable OD and OS. Intraocular pressures were 15 mmHg OD and 13 mmHg OS Dilated fundus examination revealed trace OS and 1+ OS optic disc edema without disc drusen OU, a small disc hemorrhage OS, and moderate vessel tortuosity with nicking and banking defects OD and OS. 3. Cirrus RNFL OCT showed an average thickness of 82 OD and 77 OS. All quadrants were within normal limits Cirrus 5-line raster OCT through optic nerve head showed trace elevation OD and Grade 1 elevation OS, with prominence superiorly and inferiorly. Fundus photos were taken in both eyes to document findings. Physical findings Blood pressure in eye clinic on 07/28/15: 155/82, pulse 62 Blood pressure on 02/10/15 at primary care exam: 226/107 Laboratory studies Normal Radiology studies Head CAT scan without contrast was performed after the primary care physician was notified of the optic nerve edema. No intracranial masses, extra axial collections, hydrocephalus or hemorrhages were found. Differential diagnosis Primary/leading Optic nerve head edema secondary to prior malignant hypertensive episode OU Others Optic nerve head drusen 1. No visible optic nerve drusen. Buried drusen usually becomes visible in adulthood. 2. 5-line raster OCT showed no hyper-reflective opacities Intracranial space occupying lesion 1. No other neurological signs 2. Head CAT scan was ordered by primary care physician and was unremarkable for masses or acute hemorrhages Idiopathic intracranial hypertension (pseudotumor cerebri) 1. Does not fit the usual demographic – Female, forty years of age or overweight Bilateral optic neuritis 1. Demyelinating – rarely bilateral, no APD present 2. Infectious/inflammatory – no current infections or inflammatory conditions Bilateral NAION 1. Rarely presents bilaterally 2. Optic disc hemorrhage was in the eye with less optic nerve swelling 3. No visual field defect OD and OS Diagnosis and Discussion Both Patient 1 and Patient 2 were diagnosed with malignant hypertension. Patient 1 presented to the eye clinic with the classic presentation of malignant hypertension. He had grade four retinopathy, which is defined by the presence of retinal hemorrhages, cotton wool spots and papilledema. He had acute visual symptoms, which prompted him to seek medical attention. Patient 2 presented with an atypical presentation of malignant hypertension. He was diagnosed with optic nerve edema secondary to a previous hypertensive crisis. Five months prior, the patient’s blood pressure was 226/107 but no further evaluation was initiated. When he presented for his comprehensive eye examination, his fundus findings included bilateral, asymmetric optic disc edema, a small disc hemorrhage, and moderate hypertensive vessel changes. By examining the patient’s vital sign history, we were able to find a possible etiology. A retinal ophthalmologist also examined the patient on the same day and confirmed the tentative diagnosis. Background information Malignant hypertension definitions o A hypertensive crisis is most often diagnosed when systolic blood pressure is greater than 180mmHg and/or diastolic blood pressure is greater than 120mmHg but the values are not definite. It can further be divided into hypertensive urgency or hypertensive emergency, the later meaning that end-organ damage is also present with the elevated blood pressure. o Malignant hypertension is defined as extremely elevated blood pressure with bilateral retinal hemorrhages, and/or exudates, with or without papilledema. Risk factors for hypertensive crisis o Older age, black, male gender, and medicine noncompliance. Symptoms of hypertensive crisis o Many patients are asymptomatic. o If symptoms are present, they can include headache, epistaxis, faintness, and chest pain. Ocular symptoms include a scotoma, diplopia, flashes, visual dimness, or decreased visual acuity. Ocular signs o Retinal lesions can include hemorrhages, cotton wool spots, serous retinal edema, Elschnig spots, and optic nerve edema. Systemic treatment o Immediate referral to an emergency room is warranted. o Hypertensive urgencies are treated with oral medications. o Hypertensive emergencies require an intensive care unit admission and intravenous medications to reduce blood pressure. Systemic and ocular prognosis o Undetected and untreated patients one-year survival rates are between 10-20%. o Five-year survival rates in treated patients are around 70%. o Once treatment is initiated, retinal lesions typically begin to resolve within the first few months. Typically, only Elschnig spots remain visible. o Long-term visual consequences could occur due to the ischemic complications. Treatment/Management Patient 1 o Following examination in the eye clinic, the patient was directed back to the emergency department for further treatment and evaluation. o The ED physician in charge of the patient’s care was contacted and the ocular findings were reported. o The patient received another IV injection of hydralazine following his eye exam and was discharged from the ED once his blood pressure decreased to 182/100. o Due to his long abstinence from medications, Atenolol, HCTZ/triamterene and Lisinopril were discontinued. He was instead started on 50mg of Hydrochlorothiazide. o The patient returned to the eye clinic five days later to be evaluated by the retinal ophthalmologist. Blood pressure was still elevated at 163/113. Visual acuity improved to 20/20-2 OD and was stable at 20/40 OS. Macular OCT showed mild improvement in sub-retinal fluid and cystic changes OS and optic nerve OCT showed mild increase in optic nerve edema OU. Retinal hemorrhages and cotton wool spots were stable OU. o The patient will return to clinic in three weeks for a dilated fundus examination. o If the sub-retinal fluid is still present even with better blood pressure control, a referral for an intravitreal injection of anti-VEGF like bevacizumab (IVB) could be considered. A recent study looked at the efficacy of a single IVB injection in twelve patients with persistent retinopathy following a malignant hypertensive episode. The study concluded that IVB is a safe and effective treatment for persistent retinopathy. Patient 2 o Since the patient was not currently in a hypertensive crisis, he was not referred to the emergency department for an evaluation. o The patient’s primary care physician was notified of the findings. Subsequently, his doctor recommended to increase Nadolol dosage to 40mg and ordered a head CAT scan. o The patient was evaluated by a retinal ophthalmologist the same day and he recommended following up in six weeks with a dilated fundus examination, Humphrey 24-2 threshold visual field, Spectralis OCT through macular and optic nerves. A B-scan will be ordered if necessary to determinately rule out optic nerve head drusen. Bibliography o Aggarwal, Monica, and Ijaz A. Khan. "Hypertensive Crisis: Hypertensive Emergencies and Urgencies." Cardiology Clinics (2006): 135-46. Print. o Downie, Laura E., Lauren A.B. Hodgson, Carly D'Sylva, Rachel L. McIntosh, Sophie L. Rogers, Paul Connell, and Tien Y. Wong. "Hypertensive Retinopathy: Comparing the Keith-Wagener-Barker to a Simplified Classification." Journal of Hypertension (2013): 960-65. Print. o Rodriquez, Maria Alexandra, Siva K. Kumar, and Matthew De Caro. "Hypertensive Crisis." Cardiology in Review 18.2 (2010): 102-07. Print. o Salman, Abdelrahman Gaber. "Intravitreal Bevacizumab in Persistent Retinopathy Secondary to Malignant Hypertension." Saudi Journal of Ophthalmology (2013): 25-29. Print. o Shantsila, Alena, Eduard Shantsila, and Gregory Y.h. Lip. "Malignant Hypertension: A Rare Problem or Is It Underdiagnosed?" Current Vascular Pharmacology CVP (2010): 775-79. Print. o Steinegger, K., C. Bergin, and Y. Guex-Crosier. "Malignant Hypertension: Clinical Manifestations of 7 Cases." Klinische Monatsblätter Für Augenheilkunde Klin Monatsbl Augenheilkd (2015): 590-92. Print. Conclusion Over 65 million Americans have hypertension but only 1-2% of patients present to a clinic during a hypertensive crisis. Many patients are asymptomatic even with severely elevated blood pressure. Ocular symptoms and signs provide an opportunity for malignant hypertensive diagnosis and subsequent treatment. However, ocular manifestations usually regress once blood pressure decreases making retrospective diagnosis difficult. A recent study that retrospectively analyzed seven cases of malignant hypertension argued that even the presence of one retinal lesion and a history of elevated blood pressure, malignant hypertension should be considered. There is a significant difference in mortality rates between treated and untreated malignant hypertensive patients. This makes a detailed ocular examination even more important in patients with hypertension, especially those in the higher risk categories.