* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Cutaneous mycobacterial infections
Survey
Document related concepts
Marburg virus disease wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Tuberculosis wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Leptospirosis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
Transcript
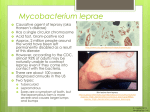
Cutaneous mycobacterial infections Tuberculosis: Definition: It is a chronic Granulomatous communicable disease caused by invasion of the skin by mycobacterium tuberculosis, the same microorganism that is responsible for pulmonary TB, which is an aerobic intracellular acid fast microorganism belongs to the genus mycobacteria that have many species ex; M. bovis. Epidemiology: cutaneous TB is relatively uncommon form of extrapulmonary TB. Even in countries like India & China where pulmonary TB is still common, cutaneous outbreak are rare (0.1%). All ages can be affected especially young age group. Both sexes are affected equally, although lupus vulgaris tends to affect females more. Route of cutaneous infection will be either exogenous inoculation or endogenous (by hematogenous spread or from adjacent infected tissues). Predisposing factors include poverty, crowding, and HIV infection. Pathogenesis & classification: the disease is highly variable in its clinical presentation depending on the immunological status of the patient & the route of inoculation of mycobacteria to the skin. There are 4 major categories of cut. TB.: 1. inoculation from exogenous source: a/ primary inoculation TB ( patient has no immunity) b/ TB. Verrucosa cutis (patient has immunity) 2. Endogenous spread: a/ contiguously: scrofuloderma. b/ autoinoculation TB: TB. Cutis orificialis. 3. haematogenous spread to the skin: a/ military TB ( pt. has no immunity) b/ lupus vulgaris (pt. has immunity) 4. tuberculids: a/ erythema induratum b/ papulo necrotic tuberculid Clinical features: 1. Primary inoculation TB: (tuberculous chancre) develop at the site of inoculation of tubercle bacilli into a tuberculous free individual (pt. with no previous exposure to TB & has no immunity). It occurs chiefly in children, most commonly on the face & extremities. Usually the inoculation occurs on previously traumatized skin. The typical lesion consists of painless red-brown papule that enlarges to form indurated nodule which then ulcerate. Prominent regional lymphadenopathy usually occurs 3-8 weeks later completing the complex. This form of TB also occur at the site of BCG vaccination in previously non-immunized child.( tuberculin test negative) 1 2. TB verrucosa cutis: it develops at the site of entry of TB bacilli into the skin of a 3. 4. 5. 6. person with previous sensitization to TB (immune patient) & tuberculin test strongly positive. The lesion is almost always solitary. It consist of hyperkeratotic papule gradually enlarge by peripheral extension to form hyperkeratotic plague with fissuring at the surface & purulent exudate. Site of involvement include dorsum of hands in adults & ankles & buttock in children. Scrofuloderma: this is TB involvement of skin by direct extension from underlying infected tissues usually TB lymphadenitis. Most frequently cervical lymph nodes. Clinically presented with subcutaneous masses which enlarge to form nodules, suppuration occurs centrally. Temperature of the skin overlying the lesion is not elevated (cold abscess). It heals with characteristic cord-like scar. TB cutis orificialis: is a form of cut. TB that occurs at the mucocutaneous borders of the nose, mouth, vagina, caused by autoinoculation from underlying active visceral TB. It indicates failing resistance to the disease. Lesions are ulcers which are soft, punched out & with undermined edges. Lupus vulgaris: this form most commonly appear at sites distant from the initial infectious focus. About 50% will have evidence of TB elsewhere, so complete evaluation of the pt. is mandatory. Lupus vulgaris is associated with high immunity to TB & most pt. will have positive tuberculin test. Typically, lesion consists of single plague composed of grouped red-brown papules which when blanched with diascopic pressure reveal a pale brow or apple-jelly color. The papules tend to heal slowly in one area to progress to another. The disease is destructive, leaves deforming ugly scars as it slowly progress over years (decades). About 90% of cases, lesions occur over head & neck. Tuberculids: are group of skin eruptions associated with an underlying or silent focus of TB. They represent cutaneous lesions induced by blood dissemination of TB bacilli usually in pt. with strong immunity against TB (positive tuberculin test). Diagnosis: 1. Biopsy: of the skin stained with acid fast stain should be done when history & physical exam. suggest TB. 2. Culture: remain the gold standard for diagnosis & determine the sensitivity of the microorganism to antibiotics. 3. PCR: determine microbacterium DNA in infected tissues. 4. Tuberculin test: this test is designed to detect cell mediated immune response to M.TB it remains the most useful method to identify infected persons. It becomes positive 2-10 weeks after infection, and remains positive for many years although it may wane with age. Test is done by injecting 5 TU (tuberclin units) of purified protein derivative PPF intradermally & then read the result 48-72 hours after the injection. It is considered positive if there is induration of 15 mm or more diameter. Negative or doubtful reaction does not rule out TB specially if history & medical exam. Suggest the disease & also in immune compromised pt. 2 Treatment: HIV testing is recommended in all pt. with TB because they may need a prolonged treatment. Culture to determine the sensitivity of the organism is important because multidrug resistance is common problem in some countries. Treatment starts with 4 drug regime: INH 5mg/kg/day + rifampicin 600mg/day + ethambutol 25/mg/kg/day + pyrizinamide 15-30mg/kg/day continue for 2 months then followed by INH + rifampicin for 6-9 months according to response. Leprosy: Definition: highly infectious chronic Granulomatous disease principally affects the skin & peripheral nerves, caused by mycobacterium leprae which is gram positive, weakly acid fast, obligate intracellular bacilli living in temperature 30-33c (so that it tends to affect the acral cooler parts of the body). Epidemiology: the disease is endemic in India & Far East, it can affect all ages & both sexes & it is highly infectious (50% of the contacts get infection). Incubation period is 2-5 years. Mode of transmission mainly via nasal droplets & secretions of the respiratory tract. Close contact, low social class & poor sanitation are predisposing factors. Pathogenesis: the disease has a spectrum regarding its clinical presentation include: tuberculoid leprosy TL, border line leprosy BL and Lepromatous leprosy LL according to the immune status of the host. In TL, cell mediated immunity is strongly expressed so that the infection is restricted to one or few skin lesions & there is rapid lymphocytic infiltration causing nerve damage. In LL, cell mediated immunity failed to occur, resulting in heavy multiplication of the bacilli which spread & multiply in infected tissue. Nerve damage is slow & gradual, haematogenous spread may occur to any area of the skin & other system like respiratory tract, eyes, testes, small muscles of hands & feet. Nerve damage may lead to anesthesia, muscle weakness, contractures & autonomic dysfunction. Clinical features: 1. Tuberculoid leprosy TL: the typical lesion is large erythematous plague that has well defined borders and flat atrophic center. It is dry, scaly, hairless, anhidrotic (decrease sweating) & anesthetic. The lesion is usually solitary or may be few (less that 3) & they are asymmetrical. Sites include face, trunk & extremities. The nerves proximal to the lesion are enlarged & tender (characteristic sign). Muscle group supplied by these nerves are paralyzed & atrophic. Contractures & foot drop can occur. No systemic symptoms or mucosal lesions. Remission within 3 years can occur without treatment. 2. Lepromatous leprosy LL: lesions consist of either hypopigmented macules or Lepromatous infiltrations (plagues & nodules). They are numerous (hundred) and small, ill defined & confluent. Involvement of skin is diffuse & symmetrical. 3 No change in skin texture, or sweating or sensation & there is no nerve thickening. Progressive hair loss (outer 1/3 of eye brow, then other body hair except scalp hair). The face show diffuse infiltration & waxy appearance (leonine face). Nerve involvement occur later, slowly progressive & give stocking–glove pattern. Systemic and mucous lesions are common. No remission without treatment. 3. Border line leprosy BL: features are in between, he patient can pass to TB or LL according to changes in his immune status (unstable leprosy). Diagnosis: 1. History & clinical exam. (Skin& nerve lesions). 2. Skin biopsy: stained with Fite stain. 3. Slit smear of the skin: smears of tissue fluid taken from the acral parts of the body stained with acid fast stain will be positive in LL and negative in TL. 4. PCR. 5. Lepromin test: determine the immune status of the patient. Positive in TL & negative in LL. 6. Histamine test: detect absent flare. 7. Methacholin test: detect absent sweating. Treatment: TL: (pauci bacillary): Dapson 100 mg/day for 3 years + Refampicin 600/mg/day for 6 months. LL: (multi bacillary): Dapson 100 mg/day for 10 years (in BL) or for life (in LL) + Refampicin 600/mg/day for 3 years. Lerpa reactions: (reaction to antibiotic treatment) are characteristic & abrupt. About 50% of patients experience a reaction after initiation of therapy. There are 2 types: a/ type I reaction: represent an enhanced cell mediated immunity toward mycobacterium lepra. They present with inflammation of preexisting lesions which become swollen, tender & erythematous simulating cellulites. Complication is nerve damage which occurs suddenly, the nerves are swollen & tender. Treatment by systemic steroids prednisolone 40-60mg/day tapered slowly according to response. b/ type II reaction: represent circulating immune complex disease, causing systemic symptoms ex: fever, arthralgia, anorexia with subcutaneous erythematous nodules ( erythema nodosum leprosum) they do not occur on preexisting lesions & are associated with systemic involvement ex: keratitis, nephritis, neuritis,…. Treatment by systemic steroid prednisolone 40-60mg/day tapered slowly or thalidomide 100-400mg/day according to severity. 4