* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download surrogacy chapter 2
Designer baby wikipedia , lookup
Donor Sibling Registry wikipedia , lookup
Anovulation wikipedia , lookup
Semen quality wikipedia , lookup
Female infertility wikipedia , lookup
Infertility wikipedia , lookup
In vitro fertilisation wikipedia , lookup
Egg donation wikipedia , lookup
Embryo transfer wikipedia , lookup
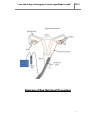
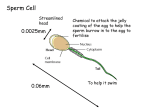
“Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Chapter – II Surrogacy and Elements Involved Human reproduction is a form of sexual reproduction resulting in the conception of a child through sexual intercourse between man and woman. During intercourse, the interaction between the male and female reproductive organs results in fertilization of woman’s ovum by the male sperm resulting into childbirth after the gestation period.1 Approximately, 84 % of women conceive within one year of having irregular unprotected sexual intercourse, which has been brought to 92 % after two years and 93 % after three years. For women upto 25 years old, the cumulative conception rate is 60 % during first six months and 85 % during one year, but conception rates for women aged over 35 years is less than half of this.2 As opined by Dr. Anirudh Singh, surrogacy is opted by most of the people because of their complicated medical conditions and not merely out of their convenience. A woman may have ovaries but no uterus, which means that she can produce healthy eggs but is unable to conceive. She may also have undergone the process of hysterectomy, i.e., removal of the uterus, owing to some uterinal disease; she may be affected by the effects of chemical or mechanical contraception, such as pelvic inflammatory disease associated with the use of an intra-uterine device, or by the effects of sexually transmitted diseases; spontaneous or induced abortion.3 1 http://www.shrishtiivf.com/Reproduction.htm; last visited on 15/05/2013, time: 09:00 am (IST), place: Meerut, (UP), India. 2 Infertility Treatments for Women: A Review of the Bio-medical Evidence, The Women’s Health Council, Ireland, Full Report, 2009, p.17. 3 This information is based upon a discussion with Dr. Anirudh Singh of Dr. Singh Test Tube Baby Centre, Opp. DIG Residence, Near Circuit House, Civil Lines, Meerut (UP). Page | 1 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Page | 2 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Page | 3 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Wider causes of infertility may include alcohol and tobacco consumption, use of illicit drugs, environmental and industrial pollutants, stress, nutritional imbalance, hormonal disorders, effect of physico-chemical alterations in habitats, pesticides, pollutants, mutagens in human body through consumption of food sprayed with herbicide, insecticide etc.4 In the opinion of the researcher, some fertile couples may also seek the services of a surrogate mother in situations when the female cannot physically bear a pregnancy, or when she is affected by a heart condition or chronic spontaneous abortion, or when she may transmit a harmful genetic or other congenital condition to the child she might conceive. Some of the problems may be solved by in-vitro fertilization, coupled with ovum donation resulting in the childbirth through the process of surrogacy. The successful rates of childbirth are as a result of natural IVF cycles, where pregnancy rates have been reported varyingly between 0 and 30 % after embryo transfer. 5 This is most likely because the natural cycle depends solely upon the development of a dominant follicle. As a result, ovarian stimulation was developed to generate more follicles and therefore, more oocytes produced, replacing the natural cycle of IVF. This in turn increases the probability of a successful pregnancy. However, IVF as practiced today is complex, time-consuming and expensive. It generates much stress and side effects such as ovarian hyper-stimulation. Thus, there has been a revival of interest in natural cycle of IVF treatment in recent years. The aim of medically assisted conception is to overcome the barriers preventing spermatozoa from encountering oocytes in infertile couples. The origins of such technologies can be traced to attempts to fertilize human oocytes outside the body. The invitro fertilization of human oocytes was accomplished only in 1944 by Rock & Menkin.6 Since then, the procedures for handling gametes have been refined and have led to various techniques for the transfer of either gametes or embryos to the woman. Infertility Treatments for Women: A Review of the Bio-medical Evidence, The Women’s Health Council, Ireland, Full Report, 2009, p.19. 5 https://www.inkling.com/read/padubidri-shaws-textbook-gynecology-15th/chapter-17/infertility-andsterility; last visited on 25/05/2013, time: 10:00 am (IST), place: Meerut, (UP), India. 6 Rock J. and Menkin M.F., In vitro Fertilization and Cleavage of Human Ovarian Eggs, 1944, pp.100-105. 4 Page | 4 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2.1 2015 Stages of Normal Reproduction in Women and Men: Normal reproduction is a complex process that involves a series of steps. For women, the steps include: a) Coordination between the hypothalamus, pituitary, and ovary to allow development of usually, a single dominant egg (called oocyte); b) Preparation of the lining of the uterus (called the endometrium) to receive an embryo; c) Release of the egg (ovulation) from the ovary; d) Capture of the egg by the fallopian tube; e) Interaction with sperm within the tube resulting in fertilization; f) Transport of the fertilized egg (zygote) through the tube and into the uterine cavity, as the zygote divides and becomes a multi-cell embryo; and g) Implantation of the embryo into the endometrium, and development of the placenta.7 For men, the steps include: a) The first step in fertility is the production of gonadotropin releasing hormone (GnRH) in the hypothalamus, which prompts the pituitary gland to manufacture follicle stimulating hormone (FSH) and luteinizing hormone (LH); b) FSH maintains sperm production and LH stimulates the production of the male hormones; c) Both the sperm and the male hormone production occur in the two testicles, or testes, which are contained in the scrotal sac; d) The production of sperm in the seminiferous tubules within each testicle. The head of the sperm contains DNA and when combined with the egg’s DNA creates a new individual. The tip of the sperm head is the portion called the ‘acrosome’, which enables the sperm to penetrate the egg. The mid-section contains ‘mitochondria’, which supplies the energy to the tail to move. The tail moves with whip-like 7 This information is based upon a discussion with Dr. Anirudh Singh of Dr. Singh Test Tube Baby Centre, Opp. DIG Residence, Near Circuit House, Civil Lines, Meerut (UP). Page | 5 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 movements back and forth to propel the sperm towards the egg. In this process, the sperm have to reach the uterus and the fallopian tube in order to fertilize a woman’s egg.8 Conditions that affect any of these processes reduce the chances of conception in a given cycle; if the condition is chronic, it can lead to the clinical condition of infertility. Infertility is not a sexual disorder. Rather, it is a condition of the reproductive system that can be caused by a number of factors occurring in both men and women. The male reproduction is hormonally driven, requiring a normal functioning of hypothalamus and pituitary gland. The male sperms are continually produced throughout a man’s lifetime. During spermatogenesis and transport through the male reproductive tract, the male spermatozoa are transformed into a highly specialized cell with its own motility and enzymatic capacity to penetrate the egg. Epididymal function must be normal and the accessory glands must be functional to produce normal seminal plasma. An intact nervous system is also required to permit penile erection and normal ejaculation. But in case of any problem in the process of reproduction, it is considered a problem related to infertility and this is the time when one may plan to go for surrogacy. Hence, before looking into the legal implications of the notion, it is essential to discuss the factors responsible for the same. 2.2 Infertility in Men: Male infertility can be due to many reasons such as oligospermia (few sperms), non-motile sperms, azoospermia (lack of sperms) and androgen disorders which has serious debilitating effects on the libido. Male infertility can be divided into: a) Ejaculation Failure: - Ejaculatory failure is the inability to ejaculate. It has a variety of causes, including pelvic nerve damage from diabetes mellitus, multiple sclerosis or abdominal-pelvic surgery and spinal cord injury. It is important to distinguish ejaculatory 8 This information is based upon a discussion with Dr. Anirudh Singh of Dr. Singh Test Tube Baby Centre, Opp. DIG Residence, Near Circuit House, Civil Lines, Meerut (UP). Page | 6 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 failure from the inability to achieve an erection, premature ejaculation and retrograde ejaculation (ejaculating into the bladder and not into the penis). Rectal probe electroejaculation is a commonly performed technique that may enable patients to produce an ejaculate capable of achieving a pregnancy. With rectal probe, the doctor electrically stimulates the pelvic sympathetic nerves to induce a reflex ejaculation from which semen is collected. b) Ejaculatory Duct Obstruction: - Ejaculatory duct obstruction is diagnosed in approximately 10 percent of men without sperm in the ejaculate. Usually caused by stones, cysts or scar tissue blocking the prostate ducts, the condition is treated with a simple outpatient procedure that involves removing portions of the ducts. Significant improvements in semen quality occur in 70 percent of patients, which are associated with a 20 percent to 30 percent pregnancy rate.9 c) Varicocele: - The varicocele is defined as dilated and twisted veins within the scrotum, similar to varicose veins in the legs, and is basically a consequence of upright posture. A varicocele can be found in 42 percent of infertile men and has an unquestioned statistical association with infertility. However, 15 percent of normal fertile men also have a varicocele. Varicocele surgery to bind off the twisted veins will improve semen quality in roughly 67 percent of patients, with improvement most likely to be an increase in the sperms’ ability to move spontaneously rather than sperm quantity.10 The pregnancy rate following varicocele repair is approximately 40 percent, with pregnancy occurring at an average of nine months after surgery. The varicocele remains the most correctable factor when poor semen quality is discovered. Problems with sperm production are by far the most common of the three, and can be detected during semen analysis.11 9 http://www.fertilityindia.com/male_infertility_and_vasectomy_reversal.php; last visited on 02/07/2013, time: 08:00 am (IST), place: Meerut, (UP), India. 10 http://www.ucsfhealth.org/conditions/infertility_in_men/causes.html; last visited on 02/07/2013, time: 08:30 am (IST), place: Meerut, (UP), India. 11 http://umm.edu/health/medical/reports/articles/infertility-in-men; last visited on 02/07/2013, time: 09:00 am (IST), place: Meerut, (UP), India. Page | 7 2015 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2.3 Infertility in Women: Maternal age is the most significant factor related to a woman’s ability to conceive. While many women today are waiting to become pregnant, the ovary’s ability to produce normal, healthy eggs declines with age, increasing the risk of chromosomal abnormalities and unsuccessful implantation and pregnancy. The likelihood for successful pregnancy begins to decrease in women in their early 30s. While this decline is initially quite minimal, as the years pass the rate of decline increases and begins to rapidly accelerate around age 37 to 38, with an acute fall beyond 42 years of age. Other factors, such as endometriosis and uterine fibroids can also play a vital role in infertility, though many women with these conditions conceive healthy children without trouble. Medical practitioners recommend that women who have crossed the age of 35 should have a fertility evaluation after attempting pregnancy for six months. Couples under the age of 35 should consider evaluation if they do not conceive after trying for a year.12 Causes of Infertility in Women: Normally, a woman may have regular menstrual periods, defined as regular cycles occurring every 21 to 35 days, which always indicates that she ovulates regularly. Ovulation of the egg occurs approximately 2 weeks before the start of the next period. If a woman has cycles at intervals of greater than 35 days, it may indicate that she is not ovulating an egg periodically. Ovulation of the egg is essential for pregnancy. It is a cause of infertility, if menstrual cycles are infrequent or irregular in a couple attempting pregnancy. One of the major cause of this may be the age of the woman, which is the most significant factor related to her ability to conceive. But in addition to age, there are a number of conditions that can interfere with a woman’s fertility, including endometriosis, polycystic ovarian syndrome, pituitary tumors and pelvic inflammatory disease etc. Infertility Treatments for Women: A Review of the Bio-medical Evidence, The Women’s Health Council, Ireland, Full Report, 2009, p.17. 12 Page | 8 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 a) Endometriosis: It is a chronic condition characterized by the growth of endometrial tissue in areas other than uterine cavity, commonly in the pelvic cavity, including the ovaries. It occurs when tissue from the membrane lining the uterus, called the endometrium, grows outside the uterus. Approximately, 10 % of the infertile couples are infected with endometriosis and between 20 to 30 percent of infertile women are estimated to have this condition. This tissue acts just like the endometrium in accumulating blood in the monthly menses period, but it has no place to shed the blood at the end of the cycle. It can cause irregular bleeding between menstrual cycles. The accumulation of tissue and blood can lead to inflammation, scarring and other problems. Symptoms include pain and cramping before and during periods, pain during intercourse, fatigue, diarrhea, constipation, nausea and infertility. Endometriosis can be treated with drugs or surgery to remove the cysts, which includes hysteroscopy, which is a procedure that allows the doctor to look inside the uterus in order to diagnose and treat the causes of abnormal bleeding. Hysteroscopy is done using a hysteroscope, a thin lighted tube that is inserted into the vagina to examine the cervix and inside of the uterus.13 b) Polycystic Ovarian Syndrome: In polycystic ovarian syndrome (PCOS), there is a long term inability to release eggs to the uterus, where they can be fertilized — a process called ovulation. Elevated insulin levels stimulate excess production of the hormone androgen, which cause some of the unfertilized eggs to disintegrate, leading to inconsistent or no ovulation. Most women with PCOS have multiple benign cysts in their ovaries. Symptoms include irregular ovulation and menstrual periods, obesity, insulin resistance, acne and excessive hair growth. PCOS, the number one cause of infertility, occurs in about 26 percent amongst the white women aged 18-25 in United Kingdom. PCOS is diagnosed by: (a) irregular or absent ovulation; (b) clinical and/or bio-chemical signs of excess androgen and (c) polycystic ovaries. Its treatments include weight loss, medications including hormones, medications to treat the insulin resistance associated with PCOS, or surgery to remove a Infertility Treatments for Women: A Review of the Bio-medical Evidence, The Women’s Health Council, Ireland, Full Report, 2009, pp-15-16. 13 Page | 9 2015 “Law and Policy on Surrogacy: A Socio-Legal Study in India” portion of the ovary or to drill holes in the ovary with a laser to reduce androgen production.14 c) Pituitary Tumors: Pituitary tumors can lead to destruction of some of the hormone-secreting cells in the pituitary gland, causing cessation of menstrual periods in women and reduced sperm production in men. Because of their location, these tumors also can cause visual field defects. Pituitary tumors are diagnosed by measuring hormone levels in the blood and urine, from MRI or CT scans of the brain and by visual field tests. Treatments include surgical removal of the tumor, radiation therapy, hormone replacement therapy etc. d) Pelvic Inflammatory Disease: Pelvic inflammatory disease (PID) in the female reproductive organs often occurs after a sexually transmitted disease such as gonorrhea or a chlamydia infection, or after miscarriage, abortion or childbirth. It can cause inflammation and permanent scarring of the fallopian tubes, abdominal pain and tenderness, fever and an unpleasant-smelling in vaginal discharge. Repeated attacks may occur with or without reinfection. About 20 percent of infertility is attributed to scarring from PID. PID usually is diagnosed during a pelvic examination, although samples of discharge may be analyzed. Antibiotics are the usual treatment. Surgery or in-vitro fertilization (IVF) is used to treat infertility resulting from PID.15 e) Additional Factors: These include: (1) Behavioural Factors: - It is well known that certain personal habits and lifestyle factors impact health. Many of these may limit a couple’s ability to conceive. These include: cigarette smoking, which lowers the sperm counts in men and increases the risk of miscarriage, premature birth and low birth weight babies for women. Smoking by either partner reduces the chance of conceiving with each cycle, either naturally or by IVF, by one-third. The next factor is alcohol. Alcohol intake greatly Infertility Treatments for Women: A Review of the Bio-medical Evidence, The Women’s Health Council, Ireland, Full Report, 2009, pp-14-15. 15 http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3831061/; last visited on 05/07/2013, time: 10:00 am (IST), place: Meerut, (UP), India. 14 Page | 10 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 increases the risk of birth defects for women and, if present in high levels in the mother’s blood it may cause Fetal Alcohol Syndrome. Alcohol also affects sperm counts in men. The third factor includes drugs, such as marijuana and anabolic steroids, which may impact sperm counts in men. Cocaine use in pregnant women may cause severe retardations and kidney problems in the baby and is perhaps the worst possible drug to abuse during pregnancy. It is suggested that recreational drug use should be avoided by the woman, both when trying to conceive and when pregnant. (2) Environmental and Occupational Factors: - The ability to conceive may be affected by exposure to various toxins or chemicals in the workplace or the surrounding environment. Substances that can cause mutations, birth defects, abortions, infertility or sterility are called reproductive toxins. Disorders of infertility, reproduction, spontaneous abortion, and teratogenesis are among the top ten work-related diseases and injuries in the US today. Despite the fact that considerable controversy exists regarding the impact of toxins on fertility, the following four chemicals affect the most while conceiving, i.e., lead; repeated exposure to radiation, ranging from simple x-rays to chemotherapy; ethylene oxide, a chemical used both in the sterilization of surgical instruments and in the manufacturing of certain pesticides. This may cause birth defects in early pregnancy and also has the potential to provoke early miscarriage. The fourth chemical is dibromochloropropane (DBCP), which is found in pesticides, has the ability to cause ovarian problems leading to a variety of health conditions like early menopause that may directly impact fertility.16 16 https://web.stanford.edu/class/siw198q/websites/reprotech/New%20Ways%20of%20Making%20Babies/C ausefem.htm; last visited on 06/07/2013, time: 11:00 am (IST), place: Meerut, (UP), India. Page | 11 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Fertility Treatment Options17: S.No. 1. Fertility Treatment Options Medicines a) Anti-Oestrogens b) Gonadotrophin c) Pulsatile Gonadotrophin Releasing Hormone d) Dopamine Agonists e) Aromatase Inhibitors 2. Surgical Treatments a) Ovarian Drilling b) Fallopian Tube Surgery c) Uterine Surgery d) Surgery for Endometriosis 3. Assisted Reproductive a) IUI (Intra-Uterine Insemination) Technology (ART) b) IVF (In-Vitro Fertilization) c) GIFT (Gamete Intrafallopian Transfer) d) ZIFT (Zygote Intrafallopian Transfer) e) ICSI (Intra-cytoplasmic Sperm Injection) f) Donor Insemination (Eggs or Sperm Donation) g) PGD (Pre-implantation Genetic Diagnosis) h) IVM (In-Vitro Maturation) 4. Other Treatments NaPro Technology (Natural Procreative Technology) Infertility Treatments for Women: A Review of the Bio-medical Evidence, The Women’s Health Council, Ireland, Full Report, 2009, p.27. 17 Page | 12 2015 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2.4 Understanding the Meaning of Assisted Reproductive Technology (ART): - Traditionally, conception occurs through intercourse between a male and female, with the male supplying the sperm and the female providing the eggs. But with the changing times, this special feature of reproduction got destructed, extinguished and infertility was considered as a curse for the individual and for the entire family. When partners discover fertility problems, they opt to a variety of options to bring a child into their lives. They may try to adopt one, or may choose from a variety of medical technologies, one of which is Assisted Reproductive Technology or ART, which is a fertility treatment that enhances a woman’s ability to get pregnant. ART has enabled millions of people (including infertile men and women, single men and women, lesbian, gay, transgender couples etc.) in the world to have biological children who otherwise would not have been able to do so. In India, there has been an unprecedented and unregulated growth of ART clinics providing IVF technology. Within the framework of medical tourism, ARTs are the latest addition to the long list of medical services being offered. Low costs, easy access to the otherwise highly regulated technologies and easy availability of surrogate mothers and gamete donors have made India a favoured destination for these procedures. Page | 13 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Assisted Reproductive Technology (ART) Procedure Page | 14 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Diagram of Egg Retrieval Procedure Page | 15 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Major Events in the History of Medically Assisted Conception18: Major Events in the History of Medically Assisted Conception Year Technique 1878 In vitro fertilization of rabbit and guinea-pig oocytes 1890 First transfer of mammalian embryo from one female to another 1909 Human pregnancy with donor semen 1944 In vitro fertilization of human oocyte 1970 Laparoscopic ovum pick-up 1973 Transient rise in human chorionic gonadotrophin 1978 Successful live birth of human baby by in vitro fertilization and embryo transfer (IVF-ET) in a natural cycle 1980 IVF-ET used for treating unexplained infertility 1981 IVF-ET pregnancy in a clomifene-citrate-stimulated cycle 1981 Laparoscopic collection of human oocytes for IVF-ET under ultrasound guidance 1982 Birth following oocyte and sperm transfer into the uterus 1983 Established pregnancy after transfer of donated embryos fertilized in vitro 1983 Successful cryopreservation of human embryos 1983 Trans-vaginal aspiration of oocytes by culdocentesis 1983 IVF-ET used for the treatment of endometriosis and for infertility of unknown cause 18 Recent Advances in Medically Assisted Conception, Report of a WHO Scientific Group, Geneva 1992, World Health Organization, Switzerland, p.8. Page | 16 2015 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 1984 Intra-uterine insemination with washed semen (IUI) 1984 IVF-ET used for the treatment of immunological infertility 1984 Pregnancy following oocyte donation and IVF-ET in a woman with premature ovarian failure 1984 IVF-ET used for the treatment of male infertility 1984 Pregnancy after gamete intra-fallopian transfer (GIFT) by laparotomy 1984 GIFT by laparoscopy 1985 IVF-ET used for the treatment of hostile cervical factor 1985 Vaginal oocyte collection under ultrasound guidance 1986 Pregnancy after human oocyte cryopreservation 1986 Direct intra-peritoneal insemination (DIPI) 1986 Pregnancy after trans-laparoscopic zygote intra-fallopian transfer (ZIFT) 1987 Pregnancy following pronuclear-stage tubal transfer (PROST) 1987 Ultrasound guided peritoneal oocyte and sperm transfer 1987 Oocyte donation and GIFT as treatment for premature ovarian failure 1987 Catheterization of the fallopian tubes from the vagina 1988 Pregnancy after transfer of multiple sperm under the zona pellucida 1989 Fallopian replacement of eggs with delayed intra-uterine insemination (FREDI) Page | 17 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2.5 2015 Step-by-Step Medical Procedure of Gestational Surrogacy19: Gestational surrogacy is a complicated procedure for the women involved. Both the surrogate and the egg donor (whether the intended mother or a selected donor) prepares for about a month in advance for the embryo retrieval and transfer. Beginning roughly weeks prior to the embryo transfer, the surrogate begins GnRH Agoinst (Lupron®) administration. This is a daily injection for roughly two and a half weeks to suppress ovarian function in order to synchronize the two women’s menstrual cycles. After about a week and a half the surrogate begins to take estrogen and progesterone supplements, administered either vaginally, orally or through injection, to help support the early stages of pregnancy. This continues until the pregnancy test, and possibly several more weeks after pregnancy is established. For the egg donor (whether of the intended mother or not), the process may begin with oral contraceptives for cycles prior to the Assisted Reproductive Technology (ART) cycle. This helps regulate the menstrual cycle, ensuring that GnRH Agonist is administered at the right time. Oral contraceptives may also help prevent ovarian cysts, which can develop during GnRH analogue therapy. About a week after the surrogate begins GnRH Agonist administration, the egg donor begins the same GnRH Agonist administration. For the egg donor, this is done primarily to prevent a premature LH (luteinizing hormone) surge, which could cause the eggs to be released before they are ready for retrieval. An ultrasound is performed around the time of the expected period to examine the ovaries and make sure that there is no cyst. After menstrual bleeding starts, ovarian stimulation also begins to support follicle development. The two hormones necessary for ovulation are Follicle Stimulating Hormone (FSH) and Luteinizing Hormone (LH). These hormones are known as ‘gonadotrophins’. There are a number of medications available to treat infertility that contains gonadotrophins. FSH is a small protein that would be destroyed by digestive enzymes in the stomach if taken orally; therefore, gonadotrophins are given by injection under the skin or into the muscle. Follicle or egg development is monitored using vaginal 19 This information is based upon the interview and discussion with Dr. Anirudh Singh and Dr. Sashee Singh of Dr. Singh Test Tube Baby Centre, Meerut (UP). Page | 18 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 ultrasounds and blood tests, performed frequently to see if medication prescriptions need to be altered. After 7 to 12 days of ovarian stimulation, the egg donor is injected with human chorionic gonadotropin (hCG), a natural hormone that completes the maturation process of the oocytes. Timing is critical, as oocyte retrieval must be performed 34-36 hours after hCG administration. To retrieve the eggs, the egg donor is administered anesthesia as a trans-vaginal ultrasound probe guides a long needle into each follicle. The follicular fluid, oocytes, and granulosa (egg-supporting cells) cells are aspirated from the follicles. The uterus, cervix and fallopian tubes are never penetrated in the procedure. A physician is then required to collect the oocytes and follicular fluid in a test tube and an embryologist locates the oocytes using a microscope. The egg donor is observed after the procedure as medication wears off. She will commonly feel lower abdominal discomfort and have some vaginal spotting for several days, but generally feels fully recovered in one to two days. Eight to 15 oocytes are typically retrieved per patient. In the embryology lab, eggs are then placed on a culture medium to support development of the embryo and mimic the environment of the fallopian tube or uterus. The dishes with eggs are placed in incubators to control the temperature and atmospheric gasses. Sperms are removed from semen collected either that morning from the intended genetic father or from frozen sperm, possibly from a sperm bank. After a few hours in the incubator, the sperms are placed in the culture medium with the eggs and returned to the incubator to develop. Individual sperm can also be injected into each egg using the intracytoplasmic sperm injection (ICSI) technique. The next day, eggs are examined to make sure fertilization has begun. If so far successful, eggs will now be zygotes, a single cell with two nuclei. After five days, embryos should have developed into the blastocyst stage, where an embryo has 80 or more cells. Selection of the best embryos for transfer is based mostly on normal visual appearance, though this does not guarantee a genetically normal embryo. The best appearing embryos are implanted into the surrogate’s uterus using a thin embryo transfer catheter that passes through the surrogate’s cervix to the top of the uterus. The number of embryos implanted depends on the surrogate and egg donor’s age, and on the appearance of the embryos. The more implanted the more likely for a successful attachment, but also higher probability of multiple births. Excess embryos not transferred Page | 19 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 can be frozen. The surrogate begins to take progesterone supplements on the day or day after oocyte retrieval to help prepare the uterine lining for implantation. A pregnancy test is done 9 to 12 days after embryo transfer, and again a few days later if test is positive. If the second test is still positive, she continues with hormonal supplements and has frequent follow-ups with the fertility clinic. After 8 to 10 weeks of pregnancy, the surrogate can begin seeing a regular obstetrician. This technology of artificial insemination involves a woman achieving pregnancy by non-involvement of sexual activity with a male partner, which includes fertilization involving manipulation of gametes/embryos outside the human body and transfer of gametes/embryos into the uterus/womb of the female. Here, the surgical removal of eggs from a woman’s ovaries, combining them with sperm in the laboratory, and returning them to the woman’s body or donating them to another woman for child-bearing, called the surrogate mother takes place. It is a popular technique for artificial procreation used by infertile childless couples. Its relative simplicity has made it an extremely popular method. One would be wondering as to why such kind of artificial means is adopted by women to achieve pregnancy. The reasons are several and could involve her immune system rejecting her partner’s sperm as invading molecules; she may be having issues with the cervix such as cervical scarring, cervical blockage from endometriosis, or thick cervical mucus; if the male partner is impotent, then donor sperm may be used.20 A woman in want of such artificial insemination to achieve pregnancy can obtain sperm from her male partner or from a sperm donor. The sperm is usually obtained through masturbation or through the use of electrical stimulator, although a special condom, known as ‘collection condom’ may be used to collect the semen during intercourse. The sperm provided by a sperm bank is produced by a donor attending the sperm bank’s premises in order to ascertain the donor’s identity on every occasion. The donor masturbates within the premises of the sperm bank and provides an ejaculation in a small container. The contents of the container are usually extended with chemicals in order to provide it for insemination. The sperm is then frozen and isolated for a period of usually six months and the donor is re-tested prior to the sperm being used for artificial 20 http://www.evmshealthservices.org/index.cfm/fuseaction/site.content/type/86923.cfm; last visited on 20/07/2013, time: 11:00 am (IST), place: Meerut, (UP), India. Page | 20 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 insemination. The artificial introduction of sperm into the uterus of a woman usually takes place with the help of a syringe. There are a number of ART techniques adopted such as Intra-Cytoplasmic Sperm Injection (ICSI), Gamete Intra-Fallopian Transfer (GIFT), Zygote Intra-Fallopian Transfer (ZIFT), embryo transfer, In vitro fertilization (IVF) (which is commonly known as “testtube baby technology”) and most importantly and widely used is ‘Surrogacy’, which is not a technique, but an arrangement, is also included under the umbrella term of ART. The ART techniques are discussed as under:21 a) Intra-Cytoplasmic Sperm Injection (ICSI): It is an assisted reproductive technology (ART) used to treat sperm- related infertility problems in both males and females. ICSI is used to enhance the fertilization phase of in-vitro fertilization (IVF) by injecting a single sperm directly into a mature egg. The fertilized egg is then placed in a woman's uterus or fallopian tube. In ICSI, all the steps are similar to the procedure of IVF, except the step of fertilization. Normally in IVF one egg is mixed with 100,000 sperms and one of the sperms fertilizes the egg on its own. In contrast, in ICSI each egg is held and injected with a single live sperm. This micro-fertilization is done with the help of a machine called the Micromanipulator. Similar to IVF, ICSI differs in the fertilization process. Unlike in IVF, where one egg is mixed with 1 lakh sperms, with fertilization taking place on its own, ICSI is a technique where each egg is held and injected with a single live sperm. This micro-fertilization is also done with the help of a machine called the Micromanipulator. For fertilization, ICSI involves the taking up of a single sperm in a fine glass needle which is injected directly into an egg. This egg is then incubated and examined. The embryo is then transferred back into the womb of the woman two or three days after fertilization. In this process, not all the eggs collected will be of a high enough quality or are mature enough to be suitable for injection. In conventional IVF, the eggs and sperm are mixed together in a dish and the sperm fertilizes the eggs naturally. 21 Spar, Debora L., The Baby Business: How Money, Science, And Politics Drive The Commerce Of Conception, 2006 ed. Page | 21 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Following are the circumstances in which ICSI may be appropriate to be used: a) when the sperm count is severely low; b) poor quality of sperms; c) when the sperms are abnormal; d) when the sperm has been recovered directly from the epididymis or the testicles, from the urine or by electro-ejaculation; e) where there are high levels of anti-bodies in the semen; f) when there have been previous fertilization failures. Men who have very few sperm count or no sperm count in their semen, or who have high numbers of abnormal sperms that are unable to fertilize an egg and would previously have had little or no chance of fathering their own genetic offsprings are been offered the facility of ICSI which gives them a real hope of having their own genetically related child.22 b) Gamete Intra-Fallopian Transfer (GIFT): GIFT is an assisted reproductive procedure introduced for the treatment of nontubal infertility. It has been a popular procedure because it results in better pregnancy rates as compared to regular IVF procedure. It involves removing a woman’s eggs, mixing them with sperm and immediately placing them into a fallopian tube, along with the man’s sperm. This technique introduced by endocrinologist Dr. Ricardo H. Asch in 198423, allows fertilization to take place inside the woman’s uterus and solves the problem of unexplained infertility. GIFT was introduced in an era when oocyte recovery was done laparoscopically and therefore, delivering gametes into the fallopian tube did not involve any extra-surgical procedure. Indications for GIFT include endometriosis and male infertility. Ovulation induction with clomiphene citrate combined with hCG and intrauterine insemination (IUI) is used to treat infertility in non-tubal situations. GIFT is a modified version of IVF technology. Like IVF, this procedure involves retrieving an egg from the woman, fertilizing it, and implanting the resulting embryo in 22 http://www.advancedfertility.com/icsi.htm; last visited on 22/07/2013, time: 01:00 pm (IST), place: Meerut, (UP), India. 23 http://embryo.asu.edu/pages/ricardo-hector-asch-1947; last visited on 22/07/2013, time: 04:00 pm (IST), place: Meerut, (UP), India. Page | 22 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 the uterus, here the process goes more quickly. While in traditional IVF, the embryos are observed and raised in a laboratory for 3 to 5 days, in GIFT, the sperm and eggs are just mixed together before being inserted and, with luck, one of the eggs will become fertilized inside the fallopian tubes. It takes, on average, four to six weeks to complete a cycle of GIFT. First, the woman must take a fertility drug to stimulate egg production in the ovaries. The doctor will monitor the growth of the ovarian follicles, and once they are mature, the woman will be injected with Human Chorionic Gonadotropin (hCG). The eggs will be harvested approximately 36 hours later, mixed with the man’s sperm, and placed back into the woman’s fallopian tubes using a laparoscope. Placement of the gametes in the fallopian tubes takes advantage of the protective tubal environment. The tubal environment enhances oocyte maturation and sperm function allowing for better embryo development. The other major advantage of GIFT is better synchronization between the developing embryo and the uterine endometrium as it enters the uterine cavity only by day 5 or 6 as compared to a day 2 or 3 transfer in IVF cycle. A woman must have at least one normal fallopian tube in order for GIFT to be suitable. It is used in instances where the fertility problem relates to sperm dysfunction, and where the couple has idiopathic infertility of which the cause is unknown. Some patients may prefer the procedure to IVF for ethical reasons, since the fertilization takes place inside the body. This is a semi invasive procedure and requires laparoscopy. GIFT is not technically in vitro fertilization because with GIFT fertilization takes place inside the body, not on a petri dish.24 GIFT is an assisted reproductive procedure that involves the following: 1) A woman’s ovaries are stimulated with medications to increase the probability of producing multiple eggs. 2) Eggs are collected through an aspiration procedure. The semen is collected in nontoxic, wide mouthed sterile plastic container. It is advisable to freeze at least 2 semen samples prior to the procedure to ensure availability of a sample if problems with collection occur. 24 http://www.infertile.com/infertility-treatments/gift.htm; last visited on 25/07/2013, time: 08:00 am (IST), place: Meerut, (UP), India. Page | 23 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 3) 2015 The semen is allowed to liquefy before it is examined microscopically to quantify the concentration and percentage of motile sperms. Liquefied semen is washed with human tubal fluid medium supplemented with 8 percent maternal serum. The best quality eggs are then immediately mixed with mobile sperm and placed in a special catheter. 4) The mixture of eggs and sperm are transferred to the woman through a laparoscopic procedure by placing a catheter in the fallopian tube and injecting the egg/sperm mixture. Standard double puncture laparoscopy technique is hereby used. 5) The last step is to watch for early pregnancy symptoms. The fertility specialist will probably use a blood test to determine if pregnancy has occurred. It has been suggested that pregnancy rates would be better if the tube on the side of the dominant ovary, from which maximum number of oocytes were retrieved, was chosen for transfer. GIFT and ZIFT can be used to treat many types of infertility, except in cases where there is damage to or abnormalities of the fallopian tubes. These techniques can also be used in cases of mild male infertility, as long as the sperm is capable of fertilizing an egg. If the woman is not capable of producing eggs that can be used in GIFT, but her partner's sperm is capable of fertilization, they might consider getting eggs from a donor. One reason for using an egg donor is age. Women over 35 are less likely to have viable eggs and more likely to have children with birth defects than younger women. A woman with premature ovarian failure, a condition in which menopause has begun early, might also consider a donor if she wants to carry a child. As with most fertility procedures, success depends on the couple's age and the woman’s egg quality. It is estimated that approximately 25-30% of GIFT cycles result in pregnancy, with a third of those being multiple pregnancies. The First GIFT baby in the UK was Todd Holden born on October 1986. The First GIFT baby in the US was Kaitlynne Kelley born on 28th April, 1987.The first application of this method in Latin Page | 24 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 America was held in Argentina on 13th May, 1986 and was led by Dr. Ricardo H. Asch and the treatment was successfully completed with the birth of Manuel Campo Lopez.25 c) Zygote Intra-Fallopian Transfer (ZIFT): ZIFT is also a modified version of IVF technology. It is an assisted reproductive procedure similar to in-vitro fertilization and embryo transfer, the difference being that the fertilized embryo is transferred into the fallopian tube instead of the uterus. It is an infertility treatment used when a blockage in the fallopian tubes prevents the normal binding of sperm to the egg. Egg cells are removed from a woman’s ovaries and fertilized in-vitro in a petri dish in a laboratory. The fertilized eggs, at this stage called zygotes, which are placed in the fallopian tubes within 24 hours by the use of laparoscopy and because of this the procedure is also referred to as tubal embryo transfer (TET). The woman must have healthy tubes for ZIFT to work. ZIFT is commonly chosen by couples who have failed to conceive after at least one year of trying and who have failed five to six cycles of ovarian stimulation with intrauterine insemination (IUI). ZIFT has been used in infertility situations where at least one fallopian tube is normal and other IVF treatments have failed.26 ZIFT is an assisted reproductive procedure that involves the following steps: 1) A woman’s ovaries are stimulated with medications, especially hormone injections to stimulate the development of the ovarian follicles. 2) Eggs are then retrieved by trans-vaginal needle aspiration through an ultrasound while the patient is under light sedation. 3) Those eggs are fertilized in a laboratory in a procedure identical to IVF. During the ZIFT procedure, fertilized eggs are transferred within 24 hours, as against 3-5 days used in a regular IVF cycle. 25 http://www.sooperarticles.com/health-fitness-articles/pregnancy-articles/gift-gamete-intrafallopiantransfer-its-success-advantages-disadvantages-156706.html; last visited on 25/07/2013, time: 10:00 am (IST), place: Meerut, (UP), India. 26 http://www.womens-health.co.uk/infertility/zift.html; last visited on 27/07/2013, time: 11:00 am (IST), place: Meerut, (UP), India. Page | 25 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 4) 2015 The fertilized eggs are then transferred through a laparoscopic procedure where a catheter is placed deep in the fallopian tube through a very small incision in the abdomen of the intended woman while she is under general anesthesia. 5) The final step is to wait and watch for early pregnancy symptoms. The fertility specialist will probably use a blood test to determine if pregnancy has occurred.27 d) In-Vitro Fertilization (IVF): - 27 http://www.midwestivf.com/treatments/zift.php; last visited on 27/07/2013, time: 01:00 pm (IST), place: Meerut, (UP), India. Page | 26 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 In-vitro fertilization (IVF) is a process by which egg is fertilized by sperm outside the body. IVF is a major treatment for infertility when other methods of assisted reproductive technology have failed. The process involves monitoring and stimulating a woman’s ovulatory process through the use of a drug that enables her to super-ovulate or to produce more eggs in one cycle than she normally does, removing ovum or ova (egg or eggs) by suction through a needle inserted into her ovaries and fertilizing them in a petri dish in a fluid medium in a laboratory with her partner’s or donor’s sperm. The fertilized egg (zygote) is cultured for 2-6 days in a growth medium and is then transferred by a thin catheter through the intended woman’s vagina into her uterus, where it is hoped that it will grow into healthy surrogate baby/babies.28 The first successful birth of a “test tube baby”, Louise Brown, occurred in 1978, who was born as a result of natural IVF cycle where no stimulation was made. Robert G. Edwards, the physiologist developed this therapy and was awarded the Nobel Prize in Physiology or Medicine in 2010.29 The term in-vitro, is derived from the Latin meaning in glass, which is used because early biological experiments involving cultivation of tissues outside the living organism from which they came, was carried out in glass containers such as beakers, test tubes, or petri dishes. Today, the term in-vitro is used to refer to any biological procedure that is performed outside the organism, it would normally be occurring in, to distinguish it from an in vivo procedure, where the tissue remains inside the living organism within which it is normally found. A colloquial term for babies conceived as the result of IVF, i.e., “test tube babies”, refers to the tube-shaped containers of glass or plastic resin, called test tubes that are commonly used in chemistry labs and biology labs in the shallower containers called petri dishes. Unlike the simpler process of artificial insemination, in which sperm is placed in the uterus and conception precedes otherwise normally, IVF involves combining eggs and sperm outside the body in a laboratory, i.e., in a test tube and placing of embryo(s) in the 28 Sher Geoffrey, Virginia Marriage Davis and Stoess Jean, In Vitro Fertilization: The A.R.T. of Making Babies, 3rd ed. 2005, pp. xvii-xviii. 29 http://www.nobelprize.org/nobel_prizes/medicine/laureates/2010/popular-medicineprize2010.pdf; last visited on 28/07/2013, time: 02:30 pm (IST), place: Meerut, (UP), India. Page | 27 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 uterus of the intended woman. IVF is a complex and expensive procedure. Only about 5% of couples with infertility opt for it. However, since its introduction in the U.S. in 1981, IVF and other similar techniques have resulted in more than 200,000 babies.30 IVF may be used to overcome female infertility in the woman due to problems of the fallopian tube, making in vitro fertilization difficult. It may also assist in male infertility, where there is a defect in sperm quality, and in such cases intra-cytoplasmic sperm injection (ICSI) may be used, where a sperm cell is injected directly into the egg cell. This is used when sperm have difficulty penetrating the egg, and in these cases the partner's or a donor's sperm may be used. ICSI is also used when sperm numbers are very low. When indicated, the use of ICSI has been found to increase the success rates of IVF. According to National Institute for Health and Clinical Excellence (NICE) guidelines, IVF is to be used where there is an unexplained infertility for women who have not conceived after 2 years of regular unprotected sexual intercourse. IVF is never considered the first step in the treatment of infertility. Instead, it is reserved for cases in which other methods such as fertility drugs, surgery, and artificial insemination do not work.31 When it comes to infertility, IVF may be an option if either of the couple has been diagnosed with: a) Endometriosis b) Low sperm counts c) Problems with the uterus or fallopian tubes d) Problems with ovulation e) Antibody problems that harm sperm or eggs f) The inability of sperm to penetrate or survive in the cervical mucus g) An unexplained fertility problem 30 http://www.webmd.com/infertility-and-reproduction/guide/in-vitro-fertilization; last visited on 28/07/2013, time: 03:59 pm (IST), place: Meerut, (UP), India. 31 http://www.dailymail.co.uk/health/article-1028430/Infertile-couples-denied-IVF-NHS-postcode-lotterymeans-just-chance.html; last visited on 28/07/2013, time: 05:00 pm (IST), place: Meerut, (UP), India. Page | 28 2015 “Law and Policy on Surrogacy: A Socio-Legal Study in India” There are five basic steps in the IVF and embryo transfer process which includes the following32: 1) Stimulation of Egg Maturation in the Ovaries: This process is also known as ‘ovarian stimulation or ovulation induction’, where a woman takes medications to stimulate the ovaries to make many mature eggs at one time. These medications are given by injection for a period of 8-14 days. Multiple eggs are desired because some eggs will not develop or fertilize after retrieval. Egg development is monitored using trans-vaginal ultrasound to examine the ovaries, and urine or blood test samples are taken to check hormone levels. When the eggs are mature, as determined by the size of the ovarian follicles and the level of estrogen, an HCG injection initiates the ovulation process. The eggs are taken out 34 to 36 hours after the injection by the health care service provider. 2) Egg Retrieval: This process is used to remove the eggs from the ovaries so that they can be fertilized. Eggs are retrieved through a minor surgical procedure that uses ultrasound imaging to guide a hollow needle through the pelvic cavity. Sedation and local anesthesia are provided to reduce and remove potential discomfort. The eggs are removed from the ovaries using a hollow needle, a procedure called follicular aspiration. The steps of egg retrieval involve: a) An ultrasound probe is inserted into the vagina to visualize the ovaries and the follicles, which contain the eggs; b) A needle is inserted through the wall of the vagina to the ovaries; and c) Suction is used to pull the eggs from the ovaries into the needle. 3) Secure the sperm: The sperm usually is obtained by ejaculation is prepared for combining with the eggs. 4) Fertilization: In a process called insemination, the sperm and eggs are placed in incubators located in the laboratory. The incubators enable fertilization to occur. In 32 http://www.nlm.nih.gov/medlineplus/ency/article/007279.htm; last visited on 29/07/2013, time: 09:00 am (IST), place: Meerut, (UP), India. Page | 29 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 some cases where there is a lower probability of fertilization, intra-cytoplasmic sperm injection (ICSI) may be used, where a single sperm is injected directly into an egg using a needle in an attempt to achieve fertilization. The eggs are monitored to confirm that fertilization and cell division are taking place. Once this occurs, the fertilized eggs are considered embryos. About 60 % of IVF in the United States is performed with ICSI. The number of pregnancies from IVF using natural fertilization is about the same as the number resulting from ICSI. The embryos that develop from IVF procedure are then placed into the uterus from 1 to 6 days after retrieval. 5) Embryo Transfer into the Uterus: The embryos are usually transferred into the woman’s uterus from one to six days after retrieval, but in most cases the transfer occurs between two to three days following egg retrieval. At this stage, the fertilized egg has developed into a two-to-four cell embryo. The transfer process involves a speculum33 which is inserted into the vagina to expose the cervix. A predetermined number of embryos are suspended in fluid and gently placed through a tube into the womb. Here the embryo should be implanted into the lining of the uterus 6 to 10 days after retrieval. This process is often guided by ultrasound. The procedure is usually painless, but some women experience mild cramping.34 For IVF to be successful, it typically requires healthy ova, sperm that can fertilize, and a uterus that can maintain a pregnancy. Due to the costs of the procedure, IVF is generally attempted only after less expensive options have failed. IVF is also indicated in cases where any of its expansions is of interest, that is, a procedure that is usually not necessary for the IVF procedure itself, but would be virtually impossible or technically difficult to perform without concomitantly performing methods of IVF. Such expansions ‘Speculum’ means a medical tool for investigating/dilating the opening of body cavity for medical examination of the interior parts. 34 http://www.nlm.nih.gov/medlineplus/ency/article/007279.htm; last visited on 29/07/2013, time: 10:00 am (IST), place: Meerut, (UP), India. 33 Page | 30 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 include pre-implantation genetic diagnosis (PGD) to rule out presence of genetic disorders, as well as egg donation or surrogacy where the woman providing the egg is not the same who will carry the pregnancy to term. The goal of such procedures is to successfully fertilize a human egg, resulting in an embryo. That embryo is then implanted into a woman’s uterus for gestation. Thus, the equation which is understood by the researcher involves: - Egg + Sperm = Zygote Embryo Child The development during this time actually encompasses multiple steps with increasing cell division. Initially the sperm fertilizes one or more eggs, resulting in a zygote. The zygote develops in a blastocyst within a few days. The blastocyst becomes an embryo once it has developed cells to support both the fetus and the placenta. The success rate of IVF procedure depends on a number of factors including patient characteristics and treatment approaches. But it is also important to understand that pregnancy rates are not the same as live birth rates. In the United States, the live birth rate for each IVF cycle is approximately: 30 to 35% for women under age 35 25% for women ages 35 to 37 15 to 20% for women ages 38 to 40 6 to 10% for women ages over 4035 35 http://www.uptodate.com/contents/in-vitro-fertilization-ivf-beyond-the-basics; last visited on 10/08/2013, time: 02:00 pm (IST), place: Meerut, (UP), India. Page | 31 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Step-by-Step Medical Procedure of Gestational Surrogacy Page | 32 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2.6 2015 Third Party Assisted ART: ART has helped many infertile couples to fulfill their dreams of having a child of their own. Innovative techniques have been introduced to achieve pregnancies in various types of infertility and also to improve existing pregnancy rates. However, pregnancy rates are still unacceptably low and the cost of technology is very high. Alternative techniques to ART have been introduced from time to time with the intent of achieving pregnancy while avoiding the high cost of ART. In countries like India, the social pressures on a couple to reproduce are very high and the per capita income is low and no funding is available for treatment, hence, the use of third party assisted ART becomes important to have a child of their own genes. This may involve: a) Sperm Donation: Couples may use donated sperm when a man does not produce sperm or produce very low count of sperms, or if he has a genetic disease. Donated sperms can be used with intra-uterine insemination (IUI) or with IVF. b) Egg/Oocyte Donation: This can be used when a woman does not produce healthy eggs that can be fertilized. An egg donor undergoes ovary stimulation and egg retrieval steps of IVF. The donated egg is then fertilized with a sperm from the woman’s partner and the resulting embryo is placed into the woman’s uterus. This process of egg donation may be helpful for women who have primary ovary insufficiency; have had chemotherapy or radiation therapy; have had surgical removal of the ovaries; were born without ovaries; are carriers of known genetic diseases; are infertile because of poor egg quality. Oocyte donation, unlike its male counterpart of sperm donation, has been a routine clinical treatment, with widespread introduction of IVF. Prior to the advent of IVF, there was neither a source of oocytes for donation to the laboratory nor clinical techniques available to ensure successful fertilization and transfer of the resulting embryos. This technique was first described by Craft in 1982 and later modified by Bucktt and Tan.36 Oocyte donation has now become a widely used treatment for infertility which is due to 36 Buckett WM and Tan SL, Alternative Assisted Conception Techniques, in Brinsden, PR (ed.), A Textbook of In Vitro Fertilization and Assisted Reproduction, 2nd ed. 1999, pp.243-255. Page | 33 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 premature menopause. Oocytes are incubated for 6 hours prior to insemination. Then four to six oocytes and 20,000 sperms are transferred into the uterine cavity in 20 mL culture medium with a normal embryo transfer catheter. Further, a simplification of the procedure entailed transfer of gametes into the uterine cavity without pre-incubation.37 Oocyte with sperm is transferred directly into the uterine cavity. The patients who require donor oocyte fall under two main groups: i. Women with non-functioning ovaries: 1. Premature ovarian failure 2. Ovarian agenesis 3. Bilateral oophorectomy 4. Menopause ii. Women with functioning ovaries: 1. Risk of inheritable genetic disease in children 2. Failed IVF due to poor quality oocytes 3. Inaccessible ovaries38 There is a growing demand for oocyte donation from women in their early 40s who fail to conceive after several cycles of IVF with their own oocyte, resulting into an equal or possibly higher pregnancy rate than through routine IVF procedure. Medically it is proved that women after 40 have better pregnancy rates with donor oocytes. Transfer of fresh embryo results in higher pregnancy rate than that of frozen-thawed embryos. There are also a small but growing number of post-menopausal women desiring pregnancy through oocyte donation. The main sources of oocyte donors include infertile woman’s close friend or relative and infertile patients undergoing IVF treatment, who donate their excess oocytes. The age of the oocyte donor is an important factor in achieving good 37 Ransom MX, Garcia AJ et. al, Direct Gamete Uterine Transfer in Patients with Tubal Absence or Occlusion, Journal of Assisted Reproduction and Genetics, 14 (1), 1997, pp.35-38. 38 http://www.sart.org/detail.aspx?id=1894; last visited on 15/08/2013, time: 10:00 am (IST), place: Meerut, (UP), India. Page | 34 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 pregnancy rate, though the age of the recipient is not that significant. An ideal donor is a woman between the age group of 21 to 35 years, with previous successful pregnancies, is in a stable relationship and has completed her family.39 The advantages attached to this procedure are that it avoids the laboratory cost of IVF-ET and it also avoids the surgical costs because it is performed through a needle injection. But a major disadvantage of this needle injection procedure is that for complete aspiration of fluid, the needle may have to be withdrawn and reinserted a number of times, thus increasing the risk of trauma and infection. c) Surrogate and Gestational Carriers: If a woman is unable to carry a pregnancy to term, she and her partner may choose a surrogate or a gestational carrier. A surrogate motherhood involves a woman bearing the child of another woman. Where the woman cannot produce eggs, the couple enters into a contract with a surrogate, whereby the surrogate is artificially inseminated with the sperm of the male partner of the couple. The surrogate then bears the child to term. The resulting child gets biologically related to the surrogate and to the male partner. Surrogacy can be used when the female of the couple does not produce healthy eggs that can be fertilized. In contrast, a gestational carrier is implanted with an embryo, where the woman willing to have a child of her own, can produce eggs but is unable to carry a child to term. The embryo is externally formed by in-vitro fertilization with husband’s sperm and wife’s ova and thereupon the embryo is implanted in surrogate mother’s womb to bear the child to term. Here the child is not biologically related to the surrogate and the child born would inherit the genetic code of the contracting couple. The surrogate is paid by the couple for renting her womb. This alternative can be used when a woman produces healthy eggs but is unable to carry a pregnancy to its full term. If needed, egg or sperm donation can also be used in this situation. The culture in the West is more tech-savvy with ‘rent or borrow a sperm’ or ‘renta-womb’ kind of lifestyle. People have this mental set up that atleast the baby is made with their own gametes, even though nourished in a rented body and with sisters, sister-in39 Patki, Ameet; Nadkarni, Suprana et al., Oocyte Donation, published in Rao, Kamini A and Chen, Christopher, Endoscopy in Infertility, 1st ed. 2007, pp.382-383. Page | 35 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 laws and even mothers lending their uterus, it finds greater acceptability. Surrogacy is also in culture these days because in the West it is not that easy to adopt a baby owing to tough adoption and paternity laws. In India, most of the women opt to rent out their wombs chiefly because of monetary reasons. These women may also have babies of their own and many of them are not first time mothers. These surrogate mothers are basically financially deprived, whose husbands have either passed away or have left them or do not pay any attention towards the household responsibilities. These women rent their wombs for carrying the child of an infertile couple only as a means to run their family. One surrogate mother received $ 8,000 for the same and relinquished all the rights in the infant to the infants’ parents. This was done by her as she wanted to secure her daughter’s future. India is having 1.2 billion population and has emerged as a preferred destination for a number of couples from around the world who are looking for a low-cost, trouble-free way of becoming parents.40 India has emerged as a hub for medical tourism because of the availability of advanced medical technology, cheap availability of women to bear a child and most importantly lack of legal scrutiny which has ensured commercial surrogacy a boom in Indian markets. This practice is not only attracting the foreign couples to have a surrogate baby in India but is also booming the Indian couples, whether they are infertile or not, the examples are of Bollywood stars Aamir Khan and Shahrukh Khan.41 40 http://www.washingtonpost.com/world/in-india-a-rise-in-surrogate-births-for-west/2013/07/26/920cb5f8efde-11e2-8c36-0e868255a989_story.html; last visited on 17/08/2013, time: 11:59 am (IST), place: Meerut, (UP), India. 41 Shah Rukh Khan opted for surrogacy and Aamir Khan’s wife Kiran Rao opted for surrogacy as Kiran did not want to de-shape her body figure and spoil future prospects of her career. Page | 36 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Example of Bollywood Star Shahrukh Khan Page | 37 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 Example of Sex selection test during surrogacy by Bollywood star Shahrukh Khan Page | 38 “Law and Policy on Surrogacy: A Socio-Legal Study in India” 2015 However, in the absence of a regulation or law on the same, some unscrupulous agents are luring poor, uneducated women into signing surrogacy contracts which are not fully understood by such women. The worry is about the increasing exploitation of poor Indian women who undergo pregnancies to earn money which is a matter of great concern. These surrogate women in the wake of earning money to run their family, undergo pregnancy several times, ruining their health. The other problem relates to legal aspects. The issue of ownership and the rights of commissioning couples and surrogate hosts have largely arisen from surrogacy arrangements because they are unsupervised by expert doctors, counselors, lawyers and most importantly have no binding effect due to the lack of legislative action on it. However, the only legal measures left are the National Guidelines for Accreditation, Supervision and Regulation of ART Clinics in India, issued by the Indian Council of Medical Research in 2005; recommendations of the Law Commission of India42 and the guidelines provided by the Hon’ble Supreme Court through the ratios of its decided cases43, which are insufficient to handle the issue of commercial surrogacy. 42 228th Report of Law Commission of India, Need for Legislation to Regulate Assisted Reproductive Technology Clinics as well as Rights and Obligations of Parties to a Surrogacy, August 2009. 43 Baby Manji Yamada v. Union of India, AIR 2009 SC 84; Jan Balaz v. Anand Municipality and Others, AIR 2010 Guj 21; K. Kalaiselvi v. Chennai Port Trust, Represented by the Chairman, Chennai, W.P.No.8188 of 2012; decided by Madras HC on 4th March, 2013. Page | 39