* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 1. dia
Human leukocyte antigen wikipedia , lookup
Immune system wikipedia , lookup
Globalization and disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Adaptive immune system wikipedia , lookup
Germ theory of disease wikipedia , lookup
Graves' disease wikipedia , lookup
Systemic lupus erythematosus wikipedia , lookup
Anti-nuclear antibody wikipedia , lookup
Innate immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Myasthenia gravis wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Autoimmune encephalitis wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Sjögren syndrome wikipedia , lookup
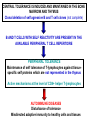
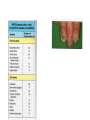
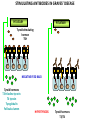
Autoimmune diseases CENTRAL TOLERANCE IS INDUCED AND MAINTAINED IN THE BONE MARROW AND THYMUS Clonal deletion of self agressive B and T cell clones (not complete) B AND T CELLS WITH SELF REACTIVITY ARE PRESENT IN THE AVAILABLE PERIPHERAL T CELL REPERTOIRE PERIPHERAL TOLERANCE Maintenance of self tolerance of T-lymphocytes against tissuespecific self proteins which are not represented in the thymus Active mechanisms at the level of CD4+ helper T-lymphocytes AUTOIMMUNE DISEASES Disturbance of tolerance Misdirected adaptive immunity to healthy cells and tissues PERIPHERAL TOLERANCE IMMUNE RESPONSES ARE NOT INITIATED IN THE PERIPHERY Normal tissue cells do not express MHC class II NO SIGNAL 1. for CD4+ Th activation Normal tissue cells do not express co-stimulatory molecules and do not produce T cell differentiating cytokines NO SIGNAL 2. for CD4+ Th activation Migration of naive T lymphocytes to normal tissues is limited Antigen presenting cells are not activated in normal tissues NO SIGNAL 3. PERIPHERAL TISSUES TOLERIZE THEMSELVES FACTORS INVOLVED IN THE PATHOMECHANISM OF AUTOIMMUNE DISEASES • Lack of AICD – mediated clonal deletion – Mutation in Fas or FasL • • • • Block of anergy – Induced by tissue necrosis or local inflammation breaking T cell anergy by increased B7 expression Novel Th epitóp self reactive B cell activation drug induced hemolytic anemia Inefficiency of regulatory T cell function Molecular mimicry – cross reactivity of pathogenic and self proteins • Polyclonal lymphocyte activation – LPS, szuper antigens • Immunologically previledged sites Demage of anatomical barriers – Post-traumic uveitis ANY CHANGE DISTURBING THE PHYSIOLOGICAL THRESHOLD AUTOIMMUNE DISEASES • Chronic inflammatory conditions • Repair mechanisms cannot compete with tissue destruction caused by the immune system • Variety of symptoms and of target tissues • Mechanisms of recognition and effector functions are the same as those acting against pathogens and environmental antigens • Both genetic and environmental factors are involved in the predisposition to autoimmune diseases – HLA class I and II and other genetic factors affect susceptibility • Runs in families and varies between populations • C1, C2 or C4 deficiency predisposes to systemic lupus erythematosus (SLE) – Environmental factors • Goodpasture’s syndrome – autoantibodies to type IV collagen, glomerulonephritis, smokers develop pulmonary hemorrhage as well • Symphathetic ophtalmia – provoked by damage • Infection – Wegener’s syndrome – antibodies to proteinase-3 of neutrophil granules results in destruction of small blood vessels primarily in the lung Any infection can induce granulocyte activation and exposure of the autoantigen Frquency of autoimmune diseases is elevated in vomem Tolerance : Role of genetic and environmental factors Practically all autoimmune diseases Involve some T-cell defects In the absence of T cell help autoreactive B cells ate trapped in the T-cell zone and die Defective central tolerance: Autoimmune PolyEndocrinopathy Candidiasis-Ectodermal Dystrophy (APECED), AIRE deficiency (Finnish population) Heterogenous disease: Candida albicans infection hypothyroidism hypogonadism and infertility vitiligo (depigmentation of the skin) alopecia (baldness) pernicious anemia chronic active autoimmune hepatitis Regulatory inhibit the activation of autoreactive T-cells IPEX: Immune dysregulation, Polyendocrinopathy, enteropathy, and X-linked syndrome FoxP3 deficiency ASSOCIATIONS OF HLA ALLOTYPE WITH SUSCEPTIBILITY TO AUTOIMMUNE DISEASE Disease HLA serotype Relatív risk Sex ratio Women/male Ankylosing spondylitis B27 87.4 0.3 Acute anterior uveitis B27 10.04 <0.5 Goodpasture’s syndrome DR2 15.9 ~1 Multiple sclerosis DR2 4.8 10 Graves’s disease DR3 3.7 4-5 Myasthenia gravis DR3 2.5 ~1 Systemic lupus erythematosus DR3 5.8 10 - 20 DR3 and DR4 3.2 ~1 Rheumatoid arthritis DR4 4.2 3 Pemphigus vulgaris DR4 14.4 ~1 Hashimoto thyroiditis DR5 3.2 4-5 Insulin dependent diabetes mellitus Maximum 20% of predisposed people develop the disease environmental factors TISSUE-SPECIFIC AUTOIMMUNE DISEASES Endocrine glands • Tissue-specific proteins are not expressed in other cells • Vascularized tissues, secrete hormone to the blood – Easy access to the immune system • Impaired function of a single type of epithelial cells • Thyroid gland – Hashimoto’s thyroiditis • no thyroid hormone production – hypothyroid • CD4+ T cells and antibodies against thyroglobulin and microsomal proteins – Graves’ disease • Antibodies to TSH receptor – hyperthyroid • Negative feedback regulation is not functional • CD4+ Th2 cells and antibodies against the muscle of eye – bulding eyes • Islets of Langerhans in pancreas – Insulin-dependent diabetes • T cells against insulin, glutamic acid decarboxylase GAD – Insulin-resistant diabetes • Antagonistic antibodies to insulin receptor • Adrenal gland – Addison’s disease – chronic adrenal gland hypofunction • Lymphocyte infiltration STIMULATING ANTIBODIES IN GRAVES’ DISEASE PITUITARY PITUITARY Tyroid stimulating hormon TSH NEGATIVE FEED BACK Tyroid hormons T3 triiodine tyronin T4 tyroxin Tyroglobulin Folliculus lumen HYPERTYROSIS Tyroid hormons T3/T4 BLOCKING AUTO – ANTIBODIES IN MYASTENIA GRAVIS NEURO-MUSCULAR JUNCTION MIYSTENIA GRAVIS Nerve impulse Nerve impulse Acetilcholin receptor Muscle Internalization NO Na+ influx NO muscle contraction MANIFESTATION OF TYPE III HYPERSENSITIVITY IN SLE Facial, malar "butterfly" rash with characteristic shape across the cheeks. Discoid lupus erythematosus (DLE) involves mainly just the skin, it is relatively benign compared to systemic lupus erythematosus (SLE). In either case, sunlight exposure accentuates this erythematous rash. A small number (5 to 10%) of DLE patients go on to develop SLE (usually the DLE patients with a positive ANA). Here is a more severe inflammatory skin infiltrate in the upper dermis of a patient with SLE in which the basal layer is undergoing vacuolization and dissolution, and there is purpura with RBC's in the upper dermis (which are the reason for the rash).