* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download diuretics - Caangay.com
Survey
Document related concepts
Remote ischemic conditioning wikipedia , lookup
Coronary artery disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Jatene procedure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
Heart failure wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
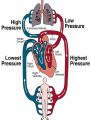
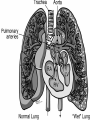
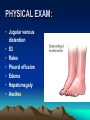
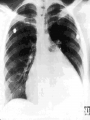
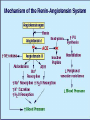
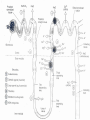
CONGESTIVE HEART FAILURE MA. LENY ALDA G. JUSAYAN, MD HEART FAILURE • Inability of the heart to pump an adequate amount of blood to the body’s needs • CONGESTIVE HEART FAILURE – refers to the state in which abnormal circulatory congestion exists a result of heart failure CAUSES OF HEART FAILURE: • Final common pathway of many kinds of heart diseases – Ischemic, alcoholic, restrictive, hypertrophic – Optimal treatment requires identification of primary & secondary factors leading to CHF – HELPFUL RESULT of dilatation: increases cardiac output – HARMFUL RESULT of dilation: more wall tension, more oxygen is needed to produce any given stroke volume CLASSIFICATION: • SYSTOLIC DYSFUNCTION: – Inadequate force is generated to eject blood normally – Reduce cardiac output, ejection fraction (< 45%) – Typical of acute heart failure – Secondary to AMI – Responsive to inotropics CLASSIFICATION: • DIASTOLIC DYSFUNCTION – Inadequate relaxation to permit normal filling – Hypertrophy and stiffening of myocardium – Cardiac output may be reduced – Ejection fraction is normal – Do not respond optimally to inotropic agents CLASSIFICATION: • HIGH OUTPUT FAILURE – Increase demand of the body with insufficient cardiac output – Hyperthyroidism, beri-beri, anemia, AV shunts – Treatment is correction of underlying cause CLASSIFICATION: • ACUTE HEART FAILURE – Sudden development of a large myocardial infarction or rupture of a cardiac valve in a patient who previously was entirely well, usually predominant systolic dysfunction CLASSIFICATION: • CHRONIC HEART FAILURE – Typically observed in patients with dilated cardiomyopathy or multivalvular heart diseases that develops or progresses slowly PRECIPITATING CAUSES OF HEART FAILURE: • • • • • • • • • Infection Anemia Thyrotoxicosis & pregnancy Arrythmias Rheumatic, viral & other forms of myocarditis Infective endocarditis Systemic hypertension Myocardial infarction Physical, dietary, fluid, environmental & emotional excesses • Pulmonary embolism PULMONARY CONGESTION & RESPIRATORY SYMPTOMS: • Result of dilatation & increasing left ventricular end diastolic pressure, left atrial pressure & capillary pressures – Results to pulmonary vascular congestion & symptoms associated with cough with blood tinged sputum Cont. • EDEMA OF THE BRONCHIAL MUCOSA – Increases resistance to airflow producing respiratory distress similar to asthma (cardiac asthma) Cont: • DYSPNEA – Results from reflexes initiated by vascular distention – Increased rigidity of lungs & impaired gas exchange resulting from interstitial edema – Accumulation of fluid in ALVEOLARS SACS (pulmonary edema) Cont. TACHYCARDIA An early compensatory response mediated by increased sympathetic tone EDEMA compensatory response mediated by the renin angiotensin aldosterone system & by increased sympathetic outflow CARDIOMEGALY a compensatory structural response SYMPTOMS: • Due to inadequate perfusion of peripheral tissues (fatigue, dyspnea) • Elevated intracardiac filling pressures (orthopnea, PND, peripheral edema) PHYSICAL EXAM: • Jugular venous distention • S3 • Rales • Pleural effusion • Edema • Hepatomegaly • Ascites “All the signs of CHF are the consequences of inadequate force of contraction" PATHOPHYSIOLOGY: • STARLING’S LAW “Within limits, the force of ventricular contraction is a function of the enddiastolic length of the cardiac muscle, which in turn is closely related to the ventricular end-diastolic volume.” PATHOPHYSIOLOGY: – Heart failure results in DEPRESSION of the ventricular function curve – COMPENSATION in the form of stretching of myocardial fibers results – Stretching leads to cardiac dilatation which occurs when the left ventricle fails to eject its normal end diastolic volume CARDIAC FAILURE VENOUS PRESSURE CARDIAC OUTPUT SYMPATHETIC ACTIVITY BLOOD PRESSURE RENAL BLOOD FLOW RENIN ANGIOTENSIN II ALDOSTERONE CAPILLARY FILTRATION SODIUM RETENTION EDEMA NEUROHUMORAL ACTIVATION DURING MYOCARDIAL FAILURE MYOCARDIAL FAILURE CARDIAC OUTPUT BLOOD PRESSURE/TISSUE PERFUSION ACTIVATION OF ADRENERGIC SYSTEM ARTERIOLAR CONSTRICTION INCREASED SYSTEMIC VASCULAR RESISTANCE INCREASED RESISTANCE TO EJECTION COMPENSATORY RESPONSES DURING HEART FAILURE: CARDIAC OUTPUT CAROTID SINUS FIRING SYMPATHETIC DISCHARGE RENAL BLOOD FLOW RENIN RELEASE FORCE RATE PRELOAD CARDIAC OUTPUT (VIA COMPENSATION) AFTERLOAD REMODELING Pathophysiology of Cardiac Performance Factor 1. Preload (work or stress the heart faces at the end of diastole) Mechanism Therapeutic Strategy increased blood volume and -salt restriction increased venous tone--->atrial -diuretic therapy filling pressure -venodilator drugs 2. Afterload (resistance against increased sympathetic which the heart must pump) stimulation & activation of renin-angiotensin system ---> vascular resistance ---> increased BP - arteriolar vasodilators -decreased angiotensin II (ACE inhibitors) 3. Contractility decreased myocardial -inotropic drugs (cardiac contractility ---> decreased CO glycosides) 4. Heart Rate decreased contractility and decreased stroke volume ---> increased HR (via activation of b adrenoceptors) CLINICAL MANAGEMENT OF CONGESTIVE HEART FAILURE • OBJECTIVES: Increase cardiac contractility Decrease preload ( left ventricular pressure) Decrease afterload (systemic vascular resistance) Normalize heart rate and rhythm Approaches: Reduce workload of heart 1.Limit activity level reduce weight control hypertension 2. Restrict sodium (low salt diet) 3. Give diuretics (removal of retained salt and water) 4. Give angiotensin-converting enzyme inhibitors (decreases afterload and retained salt and water) 5. Give digitalis (positive inotropic effect on depressed heart) 6. Give vasodilators (decreases preload & afterload) DRUGS USED TO TREAT CONGESTIVE HEART DISEASE: • VASODILATORS – Reduce the preload (through venodilatation), or reduction in afterload (through arteriolar dilatation) or both – Decrease the load of the myocardium DIURETIC AGENTS: • Reduce salt & water retention, thereby reducing ventricular preload INOTROPIC AGENTS: oIncrease the strength of contraction of cardiac muscles DRUGS USED TO TREAT CONGESTIVE HEART FAILURE VASODILATORS -CAPTOPRIL -ENALAPRIL -FOSINOPRIL INOTROPIC AGENTS -DIGOXIN -DIGITOXIN -LISINOPRIL -QUINAPRIL -DOBUTAMINE -HYDRALAZINE -ISOSORBIDE -MINOXIDIL -SODIUM NIITROPRUSSIDE DIURETICS -BUMETANIDE -FUROSEMIDE -HYDROCHLOROTHIAZIDE -METALAZONE -AMRINONE -MILRINONE BASIC PHARMACOLOGY OF DRUGS USED IN CONGESIVE HEART FAILURE: DIGITALIS PHARMACOKINETICS: LIPID SOLUBILITY ORAL AVAILABILITY HALF-LIFE PLASMA PROTEIN BINDING PERCENTAGE METABOLIZED VOLUME OF DISTRIBUTION DIGOXIN DIGITOXIN MEDIUM 75% 40 HRS 20-40 HRS <20 6.3 L/KG HIGH >90% 168 HRS >90 HRS >80 0.6 L/KG PHARMACOKINETICS: -T1/2 is long (40 hrs) -Therapeutic plasma concentration: 0.5-2 ng/ml -Toxic plasma concentration: >2 ng/ml *digitalis must be present in the body in certain "saturating" amount before any effect on congestive failure is noted this is achieved by giving a large initial dose in a process called "digitalization" -after intial dosages, digitalis is given in "maintenance" amounts sufficient to replace that which is excreted to avoid exceeding therapeutic range during digitalization: - the loading dose should be adjusted according to the health of the patient - slow digitalization (over 1 week) is the safest technique - plasma digoxin levels should be monitored METABOLISM & EXCRETION: • Digoxin – not extensively metabolized, 2/3 excreted unchanged in the kidneys • Digitoxin – metabolized in the liver and excreted into the gut via the bile MECHANISM OF ACTION: • Inhibit the monovalent cation transport enzyme coupled Na+, K+ ATPase & increased intracellular Na+ content increases intracellular Ca2+ through a Na+ - Ca2+ exchange carrier mechanism. • Increased myocardial uptake of Ca2+ augments Ca2+ release to the myofilaments during excitation invokes a positive inotropic response MECHANISM OF ACTION: • Produce alterations in the electrical properties of both contractile cells and the specialized automatic cells, leading to increased automaticity & ectopic impulse activity • Prolong the effective refractory period of the AV node slow ventricular rate in atrial flutter & fibrillation PROPERTIES OF CARDIAC GLYCOSIDES: OUABAIN DIGOXIN DIGITOXIN Lipid solubility (oil/water coefficient) Low Medium High Oral availability (% absorbed) 0 75 > 90 Half-life in the body (hrs) 21 40 168 Plasma protein binding (% bound) 0 <20 >80 Volume of distribution 18 6.3 0.6 EFFECTS IN HEART FAILURE: • • • • • • Stimulates myocardial contractility Improves ventricular emptying Increase cardiac output Augments ejection fraction Promotes diuresis Reduces elevated diastolic pressure & volume & end –systolic volume • Reduces symptoms resulting from pulmonary vascular congestion & elevated systemic venous pressure DIGITALIS INTOXICATION: • Serious & potentially fatal complication • Anorexia, nausea & vomiting = earliest signs of digitalis intoxication • Arrythmias: ventricular premature beats, bigeminy, ventricular & atrial tachycardia w/ variable AV block • Chronic digitalis intoxication = exacerbations of heart failure, weight loss, cachexia, neuralgias, gynecomastia, yellow vision, delirium TREATMENT OF DIGITALIS INTOXICATION: Tachyarrythmias: withdrawal of the drug, treatment with beta blocker or lidocaine Hypokalemia: potassium administration by the oral route OTHER POSITIVE INOTROPIC DRUGS USED IN HEART FAILURE: • BIPYRIDINES – Amrinone & Milrinone – Parenteral forms only – Half-life: 2-3 hrs – 10-40% excreted in the urine – MOA: increase inward calcium influx in the heart during action potential & inhibits phosphodiesterase – ADVERSE EFFECTS: nausea, vomiting, thrombocytopenia, liver enzyme changes BETA ADRENOCEPTOR STIMULANTS: • DOBUTAMINE – Increases cardiac output – Decrease in ventricular filling pressure – Given parenterally – CONTRAINDICATIONS: pheochromocytoma, tachyarrythmias – ADVERSE EFFECTS: precipitation or exacerbation of arrythmia DRUGS WITHOUT POSITIVE INOTROPIC EFFECTS USED IN HEART FAILURE: • DIURETICS – Reduce salt & water retention reduce ventricular preload – Reduction in venous pressure reduction of edema & its symptoms, reduction of cardiac size improved efficiency of pump function ANGIOTENSIN-CONVERTING ENZYME INHIBITORS: • Reduce peripheral resistance reduce afterload • Reduce salt & water retention ( by reducing aldosterone secretion) reduce preload • Reduce the long term remodelling of the heart vessels ( maybe responsible for the observed reduction in the mortality & morbidity) VASODILATORS: • HYDRALAZINE, ISDN – Reduction in preload through venodilatation or reduction in afterload through arteriolar dilation or both BETA-ADRENOCEPTOR BLOCKERS: • BISOPROLOL, CARVEDILOL, METOPROLOL – Reduction in mortality in patients with stable Class II & Class III heart failure DIURETICS RENAL TRANSPORT MECHANISM: • PROXIMAL CONVOLUTED TUBULE: – Carries out isosmotic reabsorption of amino acids, glucose and cations – Bicarbonate reabsorption – 40-50% Na reabsorption THICK PORTION OF ASCENDING LIMB OF THE LOOP OF HENLE: • Pumps Na, K & Cl out of the lumen into the interstitium • Provides the concentration gradient for the countercurrent concentrating mechanism • Ca & Mg reabsorption DISTAL CONVOLUTED TUBULE: • Actively pumps Na & Cl out of the lumen nephron • 10 % Na reabsorbed • Ca & Mg reabsorption COLLECTING TUBULE: • Primary site of acidification of urine & aldosterone regulated reabsorption of Na • 2-4 % reabsorbed filtered Na • H2O reabsorption under ADH control DIURETICS • Drugs that increase the rate of urine flow • Increase the rate of Na & Cl excretion • Decrease reabsorption of K, Ca & Mg DIURETICS • CLASSIFICATION: 1. CARBONIC ANHYDRASE INHIBITORS 2. OSMOTIC DIURETICS 3. LOOP DIURETICS 4. THIAZIDE DIURETICS 5. POTASSIUM SPARING DIURETICS • SITE OF ACTION: Proximal tubule Proimal tubule, Loop of Henle, Collecting tubule Ascending limb of the loop of Henle Distal convoluted tubule Collecting ducts CARBONIC ANHYDRASE INHIBITORS: • CLASSIFICATION & PROTOTYPES: ACETAZOLAMIDE (Diamox) – a sulfonamide derivative • MECHANISM OF ACTION: – Inhibits carbonic anhydrase w/c slows the ff. rxn: H + HCO3 H2O + CO2 Necessary for maximum reabsorption of HCO3 from the glomerular filtrate Drug effect occurs throughout the body PHARMACOKINETICS: • • • • Well absorbed after oral administration Onset of action: 30 minutes Duration: 12 hrs Excretion: proximal tubule CLINICAL USES: • • • • • Treatment of glaucoma – major application Urinary alkalinization Epilepsy Acute mountain sickness Correction of metabolic alkalosis TOXICITY: • • • • Hyperchloremic metabolic acidosis Renal stones Renal potassium wasting Drowsiness & paresthesias – large doses LOOP DIURETICS CLASSIFICATION & PROTOTYPES: Furosemide – prototype & sulfonamide derivative Bumetanide- sulfonamide Ethacrynic Acid – phenoxyacetic acid PHARMACOKINETICS: • Rapidly absorbed • Diuretic response is extremely rapid following IV injection • Duration of effect: 2-3 hrs • Half life: dependent on renal function • Excreted in the kidney MECHANISM OF ACTION: • Inhibit the coupled Na+/K+/2Cl transport system in the luminal membrane of the thick asceding limb of the loop of henle reduce NaCl reabsorption • Increase Mg & Ca+ excretion CLINICAL USES: • Treatment of edematous states (CHF & ascites) • Acute pulmonary edema in w/c a separate pulmonary vasodilating action may play a useful additive role • Sometimes used in hypertension if response to thiazide is inadequate but their short duration of action is a disadvantage • Treatment of severe hypercalcemia induced by a carcinoma – less common • Acute renal failure • Hyperkalemia TOXICITY: • Hypokalemic metabolic alkalosis • Hyperuricemia • Hypovolemia & cardiovascular complications • Ototoxicity – important toxic effect of the loop agents • hypomagnesemia THIAZIDE DIURETICS • CLASSIFICATION & PROTOTYPE: – HYDROCHLOROTHIAZIDE – sulfonamide derivative – INDAPAMIDE – new thiazide like agent with a significant vasodilating effect than Na diuretic effect MECHANISM OF ACTION: • Inhibit NaCl transport in the early segment of the distal convoluted tubule ( a site w/c significant dilution of urine takes place) REDUCE THE DILUTING CAPACITY OF THE NEPHRON EFFECTS: • Urinary excretion – Full doses – produce a moderate Na & Cl diuresis hypokalemic metabolic alkalosis – Reduced the blood pressure by reduction of the blood volume but with continued use these agents appear to reduce vascular resistance CLINICAL USE: • Hypertension – major application, for w/c their long duration of action & moderate intensity of action are useful • Chronic therapy for edematous conditions (CHF) another common application • Recurrent renal calcium stone formation can sometimes be controlled with thiazides TOXICITY: • Hypokalemic metabolic alkalosis & hyperuricemia • Chronic therapy is often associated with potassium wasting • hyperlipidemia POTASSIUM SPARING DIURETICS: • CLASSIFICATION & PROTOTYPES o SPIRINOLACTONE – antagonist of aldosterone in the collecting tubules • Has a slow onset & offset of action (24-72 hrs) o TRIAMTERENE & AMILORIDE – inhibitors of Na flux in this portion of the tubule ADVERSE EFFECTS: • Decrease K & H ion excretion and may cause hyperchloremic metabolic acidosis • Interfere with steroid biosynthesis CLINICAL USE: • Hyperaldosteronism – important indication • Potassium wasting caused by chronic therapy with loop diuretic or thiazide if not controlled by dietary K supplements • Most common use is in the form of products that combine a thiazide with a K sparing agent TOXICITY: • Hyperkalemia – most important toxic effect • Metabolic acidosis in cirrhotic patients • Gynecomastia & antiandrogenic effects OSMOTIC DIURETICS • CLASSIFICATION & PROTOTYPE: – MANNITOL – prototype osmotic diuretic given intravenously MECHANISM OF ACTION: • Holds water in the lumen by virtue of its osmotic effect • Major location for this action is the proximal convoluted tubule, where the bulk of isosmotic reabsorption takes place • Reabsorption of H2O is also reduced in the descending limb of the loop of henle & the collecting tubule EFFECTS: • Volume or urine is increased • Most filtered solutes will be excreted in larger amounts unless they are actively reabsorbed CLINICAL USES: • Maintain high urine flow (when renal blood flow is reduced & in conditions of solute overload from severe hemolysis or rhabdomyolysis) • Useful in reducing intraocular pressure in acute glaucoma & increase intracranial pressure in neurologic conditions TOXICITY: • Hyponatremia & pulmonary edema due to removal of water from the intracellular compartment • Headache, nausea, vomiting • dehydration Asymptomatic Mild to LV Dysfubction moderate CHF Moderate to severe CHF ACE inhibitor Digoxin Digoxin Beta blocker Diuretics Diuretics ACE inhibitor ACE inhibitor Beta blocker Beta blocker Spironolactone