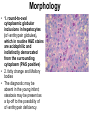
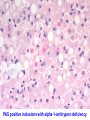
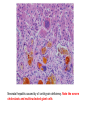
* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Liver Diseases
Survey
Document related concepts
Infection control wikipedia , lookup
Kawasaki disease wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Behçet's disease wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Sjögren syndrome wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Rheumatoid arthritis wikipedia , lookup
Globalization and disease wikipedia , lookup
Schistosomiasis wikipedia , lookup
Germ theory of disease wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
Transcript
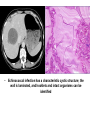
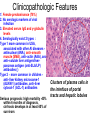
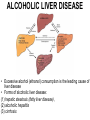
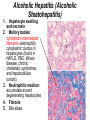
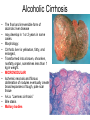
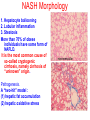
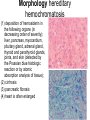
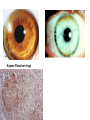
Liver Diseases Non-alcoholic fatty liver disease Hemochromatosis Wilson disease α1-antitrypsin deficiency Neonatal hepatitis Associate Professor Dr. Alexey Podcheko Spring 2015 Intended Learning Outcomes: • Liver Abscesses • Drug-induced Liver Diseases • Alcoholic Liver Diseases • Metabolic Liver Diseases: Non-alcoholic fatty liver disease Hemochromatosis Wilson disease α1-antitrypsin deficiency Neonatal hepatitis Liver abscesses -Causes: Echinococcus Amebic infection -Usually present in immigrants from endemic regions -Pyogenic (secondary bacterial infection) Pathogenesis: 1. via the portal vein 2. arterial supply 3. ascending infection in the biliary tract (ascending cholangitis) 4. direct invasion of the liver from a nearby source 5. penetrating injury Liver abscesses, Clinical • • • • • Associated with fever Right upper quadrant pain and tender hepatomegaly Jaundice Rx: surgical drainage Prognosis: if patients are elderly and have serious coexistent disease, the mortality rate of patients with large liver abscesses ranges from 30% to 90%. • Rupture of Echinococcal cyst has severe clinical consequences, including systemic spread of the organism and resultant shock from massive immune hypersensitivity response. Morphology of Liver abscesses • Size: Variable (millimeters to many centimeters) • Quantity: Multiple (Biliary) or single (trauma) • May produce empyema or a lung abscess • Rupture of subcapsular liver abscesses can lead to peritonitis or localized peritoneal abscesses • Echinococcal infection has a characteristic cystic structure; the wall is laminated, and hooklets and intact organisms can be identified Autoimmune Hepatitis • Definition: chronic and progressive hepatitis of unknown etiology • Pathogenesis: Type IV immunological reactions mediated by IFN-γ produced by CD4+ and CD8+ T cells and by CD8+ Tcell–mediated cytotoxicity. • Pathogenesis: 1. Genetic factors 2. Trigger factor- viral infections, certain drugs such as minocycline, atorvastatin, simvastatin, methyldopa, interferons, nitrofurantoin, and pemoline, and herbal products (such as black cohosh). • 3. Autoimmune hepatitis commonly occurs concurrently with other autoimmune disorders, such as celiac disease, systemic lupus erythematosus, rheumatoid arthritis, thyroiditis, Sjögren syndrome, and ulcerative colitis. Clinicopathologic Features 1. Female predominance (78%) 2. No serologic markers of viral infection 3. Elevated serum IgG and γ-globulin levels 4. Serologically exist 2 types : Type 1 more common in USA, associated with other AI diseases antinuclear (ANA), anti–smooth muscle (SMA), anti–actin (AAA), and anti–soluble liver antigen/liverpancreas antigen (anti-SLA/LP) antibodies () Type 2 - more common in children anti–liver kidney microsome-1 (ALKM-1) antibodies, anti–liver cytosol-1 (ACL-1) antibodies Serious prognosis: high mortality -40% within 6 months of diagnosis, cirrhosis develops in at least 40% of survivors Clusters of plasma cells in the interface of portal tracts and hepatic lobules Drug- and Toxin-Induced Liver Disease • The most common cause of fulminant hepatitis in the United States is drug-induced liver toxicity • Genetic variability is a critical factor • Pathogenesis: 1. Direct toxicity to hepatocytes or biliary epithelial cells 2. Hepatic conversion of a xenobiotic to an active toxin 3. Immune mechanisms (hapten-immunogen) • Drug reactions: • predictable (dose-dependent) or unpredictable (idiosyncratic –no relation with dose of the drug) ALCOHOLIC LIVER DISEASE • Excessive alcohol (ethanol) consumption is the leading cause of liver disease • Forms of alcoholic liver disease: (1) hepatic steatosis (fatty liver disease), (2) alcoholic hepatitis (3) cirrhosis Morphology • Hepatic Steatosis (Fatty Liver): • macrovesicular steatosis • there is little or no fibrosis • fatty change is completely reversible if there is abstention from further intake of alcohol. Alcoholic Hepatitis (Alcoholic Steatohepatitis) 1. Hepatocyte swelling and necrosis 2. Mallory bodies: cytokeratin intermediate filaments -eosinophilic cytoplasmic clumps in hepatocytes (found in NAFLD, PBC, Wilson disease, chronic cholestatic syndromes, and hepatocellular tumors) 3. Neutrophilic reaction: accumulate around degenerating hepatocytes 4. Fibrosis 5. Bile stasis Alcoholic Cirrhosis • The final and irreversible form of alcoholic liver disease • may develop in 1 or 2 years in some cases. • Morphology: • Cirrhotic liver is yellowtan, fatty, and enlarged, • Transformed into a brown, shrunken, nonfatty organ, sometimes less than 1 kg in weight. • MICRONODULAR • Ischemic necrosis and fibrous obliteration of nodules eventually create broad expanses of tough, pale scar tissue • A.k.a. “Laennec cirrhosis” • Bile stasis • Mallory bodies Pathogenesis ALCOHOLIC LIVER DISEASE • 10% to 15% of alcoholics develop cirrhosis • 80 gm of alcohol over one to several days generally produces mild, reversible hepatic steatosis • More prone females, African Americans • Co-morbid conditions: Iron overload, Malnutrition and deficiencies of vitamins Pathogenesis ALCOHOLIC LIVER DISEASE • Alcohol directly affects microtubules and mitochondria • Generation of excess reduced nicotinamide adenine dinucleotide (NADH + H+) causes steatosis • Acetaldehyde induces lipid peroxidation and acetaldehyde-protein adduct formation • Release of bacterial endotoxin from the gut Clinical Features of ALCOHOLIC LIVER DISEASE • Hepatic steatosis: hepatomegaly, elevated bilirubin and alkaline phosphatase, AST:ALT>2 • Alcoholic hepatitis: malaise, anorexia, weight loss, tender hepatomegaly, hyperbilirubinemia, elevated alkaline phosphatase, and a neutrophilic leukocytosis • Alcoholic cirrhosis: micronodular type of cirrhosis!!! similar to other forms of cirrhosis: hypoproteinemia (globulins, albumin, and clotting factors) “Metabolic” Liver Disease • Group of liver diseases is attributable to disorders of metabolism, either acquired or inherited. • Non-alcoholic fatty liver disease • Hemochromatosis • Wilson disease • α1-antitrypsin deficiency • Neonatal hepatitis NONALCOHOLIC FATTY LIVER DISEASE • NAFLD is a group of conditions that have in common the presence of hepatic steatosis (fatty liver), in individuals who do not consume alcohol, or do so in very small quantities (less than 20 g of ethanol/week). • The most common cause of chronic liver disease in the United States • Affects more than 30% of the population • Variants: • 1. hepatic steatosis • 2. steatosis accompanied by minor, non-specific inflammation • 3. non-alcoholic steatohepatitis (NASH) • NASH may progress to cirrhosis in 10% to 20% of cases NASH Morphology 1. Hepatocyte ballooning 2. Lobular inflammation 3. Steatosis More than 70% of obese individuals have some form of NAFLD. It is the most common cause of so-called cryptogenic cirrhosis, namely cirrhosis of “unknown” origin. Pathogenesis. A “two-hit” model : (1) hepatic fat accumulation (2) hepatic oxidative stress macrovesicular NASH Clinical Features • • • • Generally asymptomatic Obesity, insulin resistance, and diabetes Biopsy - fat accumulation in the liver Serum AST and ALT are elevated in about 90% of patients with NASH • The AST/ALT ratio is usually less than 1, in contrast to alcoholic steatohepatitis in which the ratio is generally above 2.0 to 2.5. • Fatigue and right-sided abdominal discomfort HEMOCHROMATOSIS • Excessive accumulation of body iron, most of which is deposited in parenchymal organs such as the liver and pancreas. • Total body iron pool 2 to 6 gm. In hemochromatosis, total iron accumulation may exceed 15 gm/liver • Primary or hereditary hemochromatosis is a homozygous-recessive inherited disorder that is caused by excessive iron absorption. • Secondary H. (hemosiderosis) accumulation of iron in tissues, which may occur as a consequence of parenteral administration of iron HEMOCHROMATOSIS: General features (1) micronodular cirrhosis in all patients; (2) diabetes mellitus in 75% to 80% of patients (3) skin pigmentation in 75% to 80% of patients (4) symptoms usually first appear in the fifth to sixth decades of life (5) Males predominate (5 to 7 : 1) with slightly earlier clinical presentation CAUSES OF HEMOCHROMATOSIS II. HEMOSIDEROSIS Parenteral iron overload Transfusions Long-term hemodialysis Aplastic anemia Sickle cell disease Myelodysplastic syndromes Chronic liver disease Porphyria cutanea tarda Leukemias Iron-dextran injections b-Thalassemia Sideroblastic anemia Increased oral intake of iron African iron overload (Bantu siderosis) Pathogenesis • HFE protein transfers iron from endosomes into cytoplasm of enterocytes. The adult form of hemochromatosis is almost always caused by mutations of HFE • The main regulator of iron absorption is the protein hepcidin . Deficiency in hepcidin causes iron overload. • Iron Toxicity: (1) lipid peroxidation via iron-catalyzed free radical reactions, (2) stimulation of collagen formation by activation of hepatic stellate cells (3) interaction of reactive oxygen species and of iron itself with DNA, leading to lethal cell injury or predisposition to hepatocellular carcinoma. Morphology hereditary hemochromatosis (1) deposition of hemosiderin in the following organs (in decreasing order of severity): liver, pancreas, myocardium, pituitary gland, adrenal gland, thyroid and parathyroid glands, joints, and skin (detected by the Prussian blue histologic reaction or by atomic absorption analysis of tissue); (2) cirrhosis (3) pancreatic fibrosis (4) heart is often enlarged Clinical Features of Hemochromatosis • Hemochromatosis is one of the most common hereditary diseases and inborn errors of metabolism (1:220 in European descents) • Classic triad: cirrhosis with hepatomegaly+skin pigmentation+ diabetes mellitus • Males and rare before age 40 Females – after menopause !!! • • • • • • • • Hepatomegaly Abdominal pain Skin pigmentation (particularly in sun-exposed areas) Diabetes mellitus Cardiac dysfunction (arrhythmias, cardiomyopathy) Atypical arthritis Hypogonadism (e.g., amenorrhea in the female, impotence and loss of libido in the male). WILSON DISEASE • Autosomal recessive disorder caused by mutation of the ATP7B gene, resulting in impaired copper excretion into bile and a failure to incorporate copper into ceruloplasmin • Primary route of copper elimination is excretion through bile • Accumulation of toxic levels of copper in many tissues and organs, principally the liver, brain, and eye Morphology: 1. Fatty change (steatosis) 2. Acute hepatitis 3. Massive liver necrosis 4. Chronic hepatitis Special staining: rhodamine stain for copper, orcein stain for copper-associated protein Clinical Features 1. eye lesions called Kayser-Fleischer rings or cataracts 2. acute or chronic liver disease 3. Neuropsychiatric manifestations(Parkinson) Rx: copper chelation therapy with Dpenicillamine or Trientine Kayser-Fleischer rings α1-ANTITRYPSIN DEFICIENCY • Autosomal recessive disorder due to low levels/activity of α1-antitrypsin • a1-Antitrypsin is synthesized predominantly by hepatocytes • α1-antitrypsin deficiency is the most commonly diagnosed genetic hepatic disorder in infants and children • Pathogenesis: • The accumulated α1AT-Z(mutated form) in the endoplasmic reticulum triggers a series of events, including an autophagocytic response, mitochondrial dysfunction, and possible activation of pro-inflammatory NF-κB, causing hepatocyte damage Morphology • 1. round-to-oval cytoplasmic globular inclusions in hepatocytes (α1-antitrypsin globules), which in routine H&E stains are acidophilic and indistinctly demarcated from the surrounding cytoplasm (PAS positive) • 2. fatty change and Mallory bodies • The diagnostic may be absent in the young infant; steatosis may be present as a tip-off to the possibility of α1-antitrypsin deficiency. PAS positive inclusions with alpha-1-antitrypsin deficiency Neonatal hepatitis caused by α1-antitrypsin deficiency. Note the severe cholestasis and multinucleated giant cells