* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Geriatric Drug-Drug Interactions
Discovery and development of integrase inhibitors wikipedia , lookup
Discovery and development of cyclooxygenase 2 inhibitors wikipedia , lookup
Compounding wikipedia , lookup
Discovery and development of direct thrombin inhibitors wikipedia , lookup
Drug design wikipedia , lookup
Discovery and development of ACE inhibitors wikipedia , lookup
Discovery and development of proton pump inhibitors wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Drug discovery wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Theralizumab wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Prescription drug prices in the United States wikipedia , lookup
Prescription costs wikipedia , lookup
Pharmacognosy wikipedia , lookup
Neuropharmacology wikipedia , lookup
Psychopharmacology wikipedia , lookup
Pharmacokinetics wikipedia , lookup
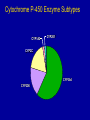
Drug-Drug Interactions Robert Kelly, MD Assistant Professor of Psychiatry Weill Cornell Medical College White Plains, New York Lecture available at www.robertkelly.us Financial Conflicts of Interest As faculty of Weill Cornell Medical College we are committed to providing transparency for any and all external relationships prior to giving an academic presentation. I do not have an interest in any commercial products or services—Robert Kelly, MD Case I 68-year-old female BIB police after calling 911 Believes objects stolen from home Sudden debut of sx in early morning hours Says she saw numerous animals and people in home Much anxiety BP 145/90, HR 100, T 97.6 H/o mild memory impairment, worsening over time Current medications simvastatin 20 mg QHS amlodipine 5 mg QAM ibuprofen 400 mg TID chlorpromazine 50 mg, prn for sleep Case II Syncope in 70yo woman with Dementia Admitted due to behavioral disturbance Medications upon admission: metoprolol 50 BID for HTN Tylenol 650 mg prn for pain Tx with Haldol 1 mg BID for psychosis Three days later added Cymbalta 30 mg BID Three days after that passed out while walking in the lounge area Common Mistakes Treat Young and Old Adults Alike Benzos for Anxiety Anticholinergic Medications Medication for Behavioral Disturbances Results Falls Cognitive Impairment Vicious cycle Confusion Delirium Importance of Drug-Drug Interactions Increased Number of Medications Greater likelihood of interactions Aging Effects Pharmacokinetics Pharmacodynamics ADRs per 10,000 Population Adverse Drug Reactions (ADRs) as a Function of Increasing Age 60 50 40 30 20 10 0 1 (infancy) 20-29 Ghose K. Drugs Aging. 1991;1:2-5. 40-49 Age (y) 60-69 80+ Incidence of Bleeding During Anticoagulant Therapy 75 years 100 65-74 years 80 < 65 years 60 Major Bleeding (%) 40 20 0 Years 0 1 2 3 4 N = 660 231 189 114 64 Beyth RJ, Schorr RI. Drugs Aging. 1999;14:231-239. Adverse Drug Reactions in the Nursing Home • Psychoactive medications (antipsychotics, antidepressants, and sedatives/hypnotics) and anticoagulants were the medications most often associated with preventable ADRs Gurwitz JH, et al. Am J Med. 2000;109:87-94. Patients (%) Relationship Between Prescribing Rate and Prevalence of Potential Drug Interactions % of Patients With Interacting Combinations 100 90 80 70 60 50 40 30 20 10 0 0 1 2 3 4 5 6 7 8 9 No. of Drugs Prescribed per Patient Nolan L, O’Malley K. Age Ageing. 1989;18:52-56. 10 11 12 Clinical Dilemma • Number of possible drug interactions too large to memorize • Difficult to determine which interactions are important Aging Primary Intrinsic, pre-programmed limit Linked to Maximum cell divisions Cell damage accumulation Interspecies variability Physiology Secondary Accumulated effects of Environmental insult Disease Trauma Intraspecies variability Pathology Physiology Pharmacokinetics Absorption Distribution Elimination Metabolism Excretion Pharmacodynamics Tissue response to drug Distribution Compartments Water Decreases Hydrophilic meds Fat Increases Lipophilic meds Plasma Protein Decreased (albumin), or increased Barriers Blood-brain Intestinal Elimination Excretion Bodily fluids Urine (Kidneys) Sweat Others Vapors (Lungs) Feces (Intestines) Tissues (Skin) Metabolism Liver Intestinal Cellular Liver Aging Effects Few Generalizations Possible Reduction in Enzyme Activity Reduction in Blood Flow, 45% from 25-65 Reduction in Size, One-third Metabolism Phase I (P450 enzyme system Actions include oxidation, reduction, hydrolysis Often active metabolites Generally reduced with age Phase II Actions include acetylation, conjugation Usually inactive metabolites Water-soluble, eliminated by kidneys Relatively spared with age Kidneys Anatomy Loss of renal mass Loss of glomeruli Basement membrane thickenin Intimal thickening of arteries Physiology Reduced GFR (approx. 50%) Reduced renal plasma flow Brain Cognitive Changes Processing Speed Memory Susceptible to delirium Atrophy Variable Substantia Nigra Balance CNS Proprioception Central processing Semicircular canals Vision Lack of exercise Medications for HTN Sedating medications Interactions Elimination Increases Decreases Synergism Toxic Effects Anticholinergic Medications Commonly Prescribed in the Elderly Commonly prescribed in the elderly at levels that can impair cognition: • • • • • Codeine Digoxin Dipyridamole Isosorbide Nifedipine • • • • Prednisolone Ranitidine Theophylline Warfarin Tune L, et al. Am J Psychiatry. 1992;149:1393-1394. SSRIs Hyponatremia Exacerbated with HCTZ and others Bleeding Inhibits platelet aggregation Possible Synergism Warfarin Aspirin Ginko Biloba Lithium Narrow therapeutic window Reduced in elderly Signs of toxicity Tremor Ataxia GI upset Severe polyurea Cognitive Impairment Delirium Blood levels affected by: NSAIDS Dehydration Salt intake Non-adherence Valproic Acid Liver enzyme inhibitor Signs of Toxicity Usually mild Sedation Anticholinergic effects Elevated LFTs Platelet production inhibition Elevated serum ammonia levels Carbamazapine Enzyme Inducer Need to increase dose after 6 weeks Signs of Toxicity Sedation Confusion Ataxia Sialorrhea MAOIs Reversible Not available in US Selective Selegiline patch, low dose Nonselective Risk of hypertensive crisis Medications--Demerol Food restrictions Cytochrome P-450 Enzyme Subtypes CYP1A2 CYP2E1 CYP2C CYP3A4 CYP2D6 CYP isoform Representative substrates 1A2 Caffeine, theophylline, tacrine 2B6 Propofol, bupropion 2C9 Phenytoin, S-warfarin, tolbutamide, NSAIDs 2C19 2D6 Omeprazole (partial contributor to many) 2E1 Some CNS and cardiac drugs 3A Fluranes, chlorzoxane (many) CYP3A • High abundance • Present in G.I Tract • No polymorphism, but high individual variability CYP3A Substrates Complete Partial Benzodiazepines (short t1/2) Zolpidem Buspirone Amitriptyline Trazodone Imipramine Nefazodone Sertraline Cyclosporine Citalopram Statins Diazepam Calcium antagonists Clozapine Quinidine Protease Inhibitors Sildenafil CY3A Inhibitors High Risk Moderate Risk Ketoconazole Fluconazole Itraconazole Fluvoxamine Nefazodone Fluoxetine Ritonavir (acute) Grapefruit juice Erythromycin Other HIV PIs Clarithromycin Delavirdine Calcium Antagonists Cimetidine CYP3A Inducers • • • • • • Rifampin Barbiturates Carbamazepine Ritonavir (chronic) Nevirapine Hypericum perforatum (St. John’s Wort) St. John’s Wort • Induces P-glycoprotein – Digoxin by 30% • Induces CYP3A4 – Indinavir – Cyclosporine – Statins Ruschitzka F, et al. Lancet. 2000;355(9203):548-549. Piscitelli SC, et al. Lancet. 2000;355(9203):547-548. Cytochrome P-450: Enzymes and Selected Substrates 1A2 2C 2D6 3A4 Theophylline Phenytoin Codeine Antihistamines Warfarin Warfarin Venlafaxine Calcium channel blockers Antipsychotics Amitriptyline Trazodone Carbamazepine Benzodiazepines Clomipramine Risperidone Cisapride Fluvoxamine Omeprazole Haloperidol Corticosteroids Tramadol Cyclosporine -Blockers Fentanyl Protease inhibitors Statins Triazolobenzodiazepines Michalets EL. Pharmacotherapy. 1998;18:84 -112. Cupp MJ, Tracy TS. Am Fam Physician. 1998;57:107-116. Inhibition of Human Cytochrome P-450 Isoenzymes by Newer Antidepressants Cytochrome P-450 Isoenzyme Antidepressant Fluoxetine Norfluoxetine Sertraline Desmethylsertraline Paroxetine Fluvoxamine Citalopram R-Desmethylcitalopram Escitalopram S-Desmethylcitalopram Nefazodone Triazoledione Hydroxynefazodone Venlafaxine O-Desmethylvenlafaxine Mirtazapine 0 + ++ +++ — 1A2 + + + + + +++ + 0 0 0 0 0 0 0 0 0 2C9 ++ ++ + + + ++ 0 0 0 0 0 0 0 0 0 — = minimal or zero inhibition. = mild inhibition. = moderate inhibition. = strong inhibition. = no data available. Greenblatt DJ, et al. J Clin Psychiatry. 1998;59(suppl 15):19-27. von Moltke LL, et al. Drug Metab Disposition. 2001;29:1102-1108. 2C19 + to ++ + to ++ + to ++ + to ++ + +++ 0 0 0 0 0 0 0 0 0 — 2D6 +++ +++ + + +++ + 0 + 0 0 0 0 0 0 0 + 2E1 — — — — — — 0 0 0 0 — — — — — — 3A + ++ + + + ++ 0 0 0 0 +++ + +++ 0 0 0 Pharmacokinetic Issues in BP Elders • Reduced renal clearance of some drugs, e.g lithium; • Decreased volume of distribution for hydrophilic drugs, e.g. lithium; • Changes in plasma binding proteins, e.g. lower albumin conc.; proportion of non bound valproate is increased; • Changes in effective drug concentration/dose may have clinical meaning for benefit/toxicity: lithium- lower doses and longer time to steady state Pharmacodynamics in Aged • Older BP patients may be slow to improveduration of adequate treatment trial not clear; • Optimal doses/concentrations not defined; • Some patients respond to low concentrations, e.g. of lithium. • Patients with dementia, and mild cognitive impairments, may have slower/attenuated benefit and greater neurocognitive side effects. Elderly Are More Difficult to Treat Safely • Pharmacokinetic changes result in higher and more variable drug concentrations • The elderly often take multiple medications • Greater sensitivity exists to a given drug concentration • Homeostatic reserve may be impaired Coping With Drug Interactions • Anticipation and prevention – Highly potent inducer/inhibitor – Narrow therapeutic index of victim – Victims dependent on one metabolic enzyme/transport protein Coping With Drug Interactions • Recognize interaction potential of “nondrugs” (herbals) • Keep knowledge base current • Consider interactions whenever the clinical picture unexpectedly changes