* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download PP - Chemistry Courses: About
Survey
Document related concepts
Biochemical cascade wikipedia , lookup
Paracrine signalling wikipedia , lookup
Lipid signaling wikipedia , lookup
Proteolysis wikipedia , lookup
Basal metabolic rate wikipedia , lookup
Biosynthesis wikipedia , lookup
Amino acid synthesis wikipedia , lookup
Citric acid cycle wikipedia , lookup
Phosphorylation wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Blood sugar level wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Biochemistry wikipedia , lookup
Transcript
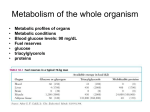
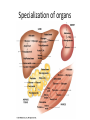
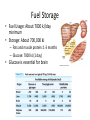
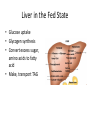
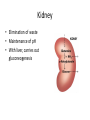
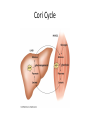
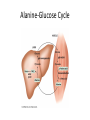
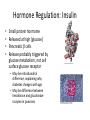
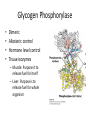
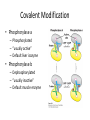
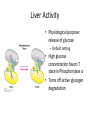
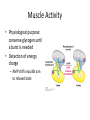
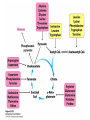
Regulation of Metabolism Pratt and Cornely Chapter 19 Regulation by Compartmentalization • Form of reciprocal regulation • Degradation vs biosynthesis • Requires transporters Specialization of organs Fuel Storage • Fuel Usage: About 7000 kJ/day minimum • Storage: About 700,000 kJ – Fats and muscle protein: 1-3 months – Glucose: 7000 kJ (1 day) • Glucose is essential for brain Liver: Tissue Specific Functions • • • • • Gluconeogenesis Ketogenesis Urea production Lactate recycling Alanine recycling Liver in the Fed State • Glucose uptake • Glycogen synthesis • Convert excess sugar, amino acids to fatty acid • Make, transport TAG Liver in the Fast State • Glycogen breakdown • Maintain blood sugar level • Catabolize glucogenic amino acids to maintain glucose and citric acid cycle • Catabolize fats and ketogenic amino acids for ketone body Muscle • Glucose trapped as glycogen (no blood sugar regulation) • Source of energy in starvation Muscle: Active State • Immediate ATP/creatine • Anaerobic muscle glycogen • Aerobic muscle glycogen • Aerobic liver glycogen • Adipose fatty acids Adipose • Fed state: uptake of fats AND glucose (why?) • Fast state: release of fats by hormone sensitive lipase (HSL) Kidney • Elimination of waste • Maintenance of pH • With liver, carries out gluconeogenesis Cori Cycle Alanine-Glucose Cycle Metabolic Issues • Starvation • Alcoholism • Metabolic Syndrome – Obesity – Diabetes Starvation • Early starvation: convert protein to glucose (cannot convert fat to glucose) • Later starvation – Preserve muscle – Muscle uses fat as fuel; buildup of acetyl CoA shuts down pyruvate acetyl CoA – Low [OAA] means acetyl CoA buildup – Ketone bodies produced – Brain uses KB, glucose is conserved Metabolism of Ethanol • Liver damage – Too much NADH and acetyl CoA – Shuts down citric acid cycle – Fatty acid synthesis upregulated • “fatty liver” – Ketone bodies form • acidosis Obesity • Hereditary, age, and environmental • Set-point • Leptin – Appetite suppressant – Made in adipose • Brown fat Diabetes • Type 1 (Juvenile onset) – Insulin dependent • Type 2 – Insulin resistance • Body feels like a fast – Gluconeogenesis increase – Lower fat storage – Increase in fat utilization • ketogenesis Hyperglycemia • Non-enzymatic glycosylation • Sorbitol production leads to tissue damage • Drugs aimed at undoing metabolic problems • Metformin – Activates AMPK » Suppress gluconeogenesis – Activates glucose and fatty acid uptake in muscle Review of Chemical Regulation • Local vs hormone-level regulation • Signal transduction pathways • Allosteric effectors – Covalent modification • Product inhibition, feedback inhibition, feed forward activation • Energy charge • Reciprocal Regulation • Isozymes • Logic of regulation – Know all purposes of pathway – Know differences in tissue physiology Hormone Regulation: Insulin • • • • Small protein hormome Released at high [glucose] Pancreatic b cells Release probably triggered by glucose metabolism, not cell surface glucose receptor – May be mitochondrial difference, explaining why diabetes changes with age – May be difference between hexokinase and glucokinase isozyme in pancreas Hexokinase • Most tissues except pancreas and liver • First irreversible reaction • Linked to glucose uptake – Locks glucose in cell • Many isozymes – Most inhibited by glucose6-phosphate – Product inhibition Glucokinase • Isozyme in liver and pancreas • Higher Km – Hexokinase always saturated, but glucokinase sensitive to [glucose] • Not inhibited by glucose-6-P – Why? Liver serves to modulate blood sugar Isozyme kinetics • Looks allosteric, but this is monomeric enzyme • May be due to conformational change upon product release— stays in active state at high concentration of glucose Insulin Signal Transduction Glucagon and Epinephrine • Glucagon released with low blood sugar (pancreas a cells) • Epinephrine released by adrenal glands • Oppose insulin – Activates glycogen breakdown – Activates gluconeogenesis – Activates hormone sensitive lipase Hormone Summary • “Insulin signals fuel abundance. It decreases the metabolism of stored fuel while promoting fuel storage.” • “Glucagon stimulates the liver to generate glucose by glycogenolysis and gluconeogenesis, and it stimulates lipolysis in adipose tissue.” Some Major Points of Regulation • Entry of glucose into cell • Glycolysis/gluconeogenesis • Fatty acid synthesis/breakdown • Glycogen synthesis/breakdown Urea: Glucose Entry into Cells • Tissues have unique function • Isozymes of glucose transporter, GLUT – Insulin dependent in muscle – Higher [glucose] required for liver uptake Glycolysis/Gluconeogenesis • Role of citrate in multiple pathways • Regulation by energy charge (ATP, AMP ratio) – [ATP] does not change much • AMP-dependent protein Kinase (AMPK) acts as energy sensor – High [AMP] activates kinase to switch off anabolism and switch on catabolism – Boosts production of F2,6-bP Hormone Regulation of Glycolysis/Gluconeogenesis and AMPK activates phosphoprotein phosphatase Glycogen Metabolism Glycogen Phosphorylase • • • • Dimeric Allosteric control Hormone level control Tissue isozymes – Muscle: Purpose it to release fuel for itself – Liver: Purpose is to release fuel for whole organism Covalent Modification • Phosphorylase a – Phosphorylated – “usually active” – Default liver isozyme • Phosphorylase b – Dephosphorylated – “usually inactive” – Default muscle enzyme Liver Activity • Physiological purpose: release of glucose – Default setting • High glucose concentration favors T state in Phosphorylase a • Turns off active glycogen degradation Muscle Activity • Physiological purpose: conserve glycogen until a burst is needed • Detection of energy charge – AMP shifts equilibrium to relaxed state Glucagon/Epinephrine Regulation through Phosphorylase Kinase • Activation of cascade leads to active degradation of glycogen • Epinephrine affects liver through IP3 pathway Regulating regulators • Influx of calcium in active muscle partially activates kinase • Hormone response fully activates Reciprocal Regulation Glucagon Protein Phosphatase 1 • Opposite of PKA – Deactivates phosphorylase – Activates glycogen synthase • Active in cell unless epinephrine signals PKA – PKA activates its inhibitors Insulin stimulates glycogen synthesis • Insulin blocks the “turn off” switch for glycogen synthase • Allows PP1 to “turn on” glycogen synthase Fatty Acid Regulation • Carnitine Transporter – Matrix malonyl CoA • Error in this picture • Actually produced by acetyl CoA carboxylase isozyme in matrix • Acetyl CoA carboxylase – Local • AMP level • Citrate and Fatty Acids – Hormones AMP level • AMP-activated protein kinase – Fuel sensor – Inactivates acetyl CoA carboxylase under low energy conditions in cell Citrate and Fatty Acids • [Citrate] high in well fed state – Lots of OAA and acetyl CoA • Carboxylase forms active filaments – If [fatty acids] is high, no need to synthesize – Fatty acids break down filaments Hormone-level control • Glucagon and epinephrine – Suppress acetyl CoA carboxylase by keeping it phosphorylated • Insulin—activates storage – Leads to dephosphorylation of carboxylase Review • Principles of Metabolism • Central molecules – Relate to reactions • Enzyme classes • Cofactors • Basic reactions – Redox – Decarboxylation – energetics • Reaction motifs Central Molecules Enzyme classes Problem 6.14. Propose a name for the enzyme, and indicate metabolic purpose of reaciton. Cofactors Problem 12.26-27 • Identify the metabolic pathway. Indicate which redox cofactor is necessary. Problem 33: • Identify the necessary cofactors Reaction Motifs