* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download RSV Epidemiology
Survey
Document related concepts
Whooping cough wikipedia , lookup
Onchocerciasis wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Gastroenteritis wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Bioterrorism wikipedia , lookup
Meningococcal disease wikipedia , lookup
Chagas disease wikipedia , lookup
Hepatitis B wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Schistosomiasis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Leptospirosis wikipedia , lookup
Transcript
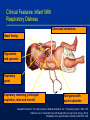
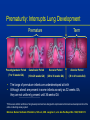
Respiratory Infections and the Infant Rees Oliver MD Assistant Professor Department of Pediatrics Division of Neonatology University of Alabama at Birmingham Disclosure statement: I do speak as a consultant on behalf of MedImmune for the product Synagis. Causes of Acute Respiratory Infections in Children <5 Years of Age Adenovirus 7% C. pneum. 0% M. pneum. 9% RSV 62% H. infl. 6% Parainfluenza 2% Infl. B 2% Infl. A 3% S. pneum. 8% Data from the Belgian sentinel network’s epidemiology surveillance (2000–2001 season) 3 With permission from Simoes EAF and Carbonell-Estrany X. Pediatr Infect Dis J. 2003;22:S13-S20. Leading Viral Causes of Infant Mortality Estimated mortality for underlying pneumonia and influenza deaths, based on data from Centers for Disease Control and Prevention Mortality Rate per 100,000 Person-Years 4 3.1 RSV Influenza 3 2 1 0 0.3 <1 0.1 <0.01 0.2 1–4 0.2 5–49 Age Bracket (years) 12 Thompson WW et al. JAMA. 2003;289:179-186. Clinical Features: Infant With Respiratory Distress Chest wall retractions Nasal flaring Hypoxemia and cyanosis Expiratory grunt Expiratory wheezing, prolonged expiration, rales and rhonchi 16 Tachypnea with apneic episodes Adapted from Netter F. The Ciba Collection of Medical Illustrations. Vol. 7, Respiratory System. CIBA, 1979. Collins PL et al. In: Fields BN, Knipe DM, Howley PM, et al, eds. Fields Virology. 5th ed. Philadelphia, Pa: Lippincott-Raven Publishers; 2007:1601-1646. Signs and Symptoms of Respiratory Distress in Infants Mild symptoms: moderate tachypnea, rhinorrhea, low-grade fever, and, frequently, otitis media. Recovery occurs after an illness of 7 to 12 days Severe symptoms: coughing and wheezing followed by dyspnea; severe tachypnea is common; in cases of extreme hypoxemia, respiratory failure occurs In high-risk infants, respiratory failure severe enough to require airway intubation can occur early in the course of illness 17 Collins PL et al. In: Fields BN, Knipe DM, Howley PM, et al, eds. Fields Virology. 5th ed. Philadelphia, Pa: Lippincott-Raven Publishers; 2007:1601-1646. Transmission of Viruses • Viruses can be transmitted by droplets, large particles, and fomites • Can survive for as long periods of time on nonporous surfaces • Medical personnel transmit these viruses readily • Nosocomial infection remains an enormous problem Blydt-Hansen T, et al. Pediatr Infect Dis J. 1999;18(2):164; Hall CB, et al. J Pediatr. 1980;141:98-102; Hall CB. Clinical Infectious Diseases; 2000;31:590-6; Cohen B, et al. Pediatric Infectious Disease Journal. 2003;22:494-9 Epidemiology of Viral Processes • Several of these viruses produce outbreaks each year particularly RSV • In the case of these outbreaks they can vary in length from region to region, and from season to season and can last for months throughout much of the U.S. • Year-round epidemics have been reported Mavunda K, et al. Am J Crit Care Pulm Med. 2000;ATS Abstr # G55:348; Ledbetter JC, et al. Ped ResAPS/SPR/APA. 2002;Abstr #2787; Doraisingham S, Ling ,AE. Ann Acad Med Singapore. 1986;15:9-14 Viral Epidemiology • During any given season a large portion of the population develops an upper or lower respiratory tract infection (LRTI), Bronchiolitis • More than half of all children will be infected by their first birthday especially with RSV • By two years of age essentially all children have been experienced Bronchiolitis Glezen WP, et al. Am J Dis Child. 1986;140:543-6 Re-infection • If you look at studies looking at these viruses there are reports that between 6% and 83% of children followed longitudinally have been re-infected each year • Antibody response is sometimes not sufficient to prevent subsequent re-infection • Infected lymphocytes and macrophages may suppress secondary immune responses Feigin RD, Cherry JD, (Eds.). Textbook of Pediatric Infectious Diseases, 4th Ed. 1998. 185.2095; Hall CB, et al. Journal of Infectious Diseases. 163,no.4(1991):693-8; Openshaw, P.J.M. Respiratory Research 3, Suppl 1. (2002):S15 Recent Trends in Hospitalizations • Up to 126,300 annual hospitalizations among U.S. infants for bronchiolitis or pneumonia may be attributed to RSV alone. • Bronchiolitis hospitalizations 1980-1996 – 1.65 million hospitalizations – 7 million inpatient days – 57% were in children <6 mo – 81% were in children <1 yo – 239% increase in bronchiolitis hospitalizations in children less than six months of age Shay DK, et al. J Infect Dis. 2001;183:16-22; Institute of Medicine. In: New Vaccine Development: Establishing Priorities. Vol I. Wash DC Nat Aca Press 1986: 397-409; Shay DK, et al. JAMA. 1999;282:1440-9 Top Causes of Infant Hospitalization Based on National Hospital Discharge Survey, 1997-1999 RSV Bronchiolitis 220,379 Bronchiolitis (cause unspecified) 181,662 Pneumonia (cause unspecified) 121,558 87,826 Jaundice Dehydration 73,250 0 50,000 100,000 Leader S, Kohlhase K. Pediatr Infect Dis J. 2002;21:629-32 150,000 200,000 250,000 • Several prospective studies have shown that even RSV bronchiolitis is associated with recurrent wheezing during subsequent years • Recurrent wheezing tends to diminish by early adolescence (age 13) • Conclusion: RSV bronchiolitis appears to be linked to recurrent childhood wheezing through early adolescence Sigurs N, et al. Am J Crit Care Med. 2000;161:1501-7 Taussig LM, et al. Am J Epidemiol. 1989;129:1219-31 Stein RT, et al. The Lancet. 1999;354:541-5 Children at Highest Risk for Severe Respiratory Distress as an Infant Premature birth Chronic Lung Disease Congenital Heart disease Neuromuscular disease Immune deficiency • Altered airway anatomy • Absence of maternal antibody • Bronchial hyper-responsiveness • Reduced lung capacity • Pulmonary vascular hyper-responsiveness • Pulmonary hypertension • Increased pulmonary blood flow • Decreased respiratory muscle strength and endurance • Decreased host defenses • Impaired capacity to eliminate virus Adapted from a presentation by L Weisman, MD: 1st International Congress RSV, 2002 Problems in Premature Infants •Respiratory: Airway alteration, respiratory distress/failure, apnea, air leaks, CLD/BPD •Cardiovascular: Patent ductus arteriosus •CNS: Intraventricular hemorrhage, periventricular leukomalacia, seizures •Renal: Electrolyte imbalance, acid-base disturbances, renal failure •Ophthalmologic: Retinopathy of prematurity, strabismus, myopia •Gastrointestinal-nutritional: Feeding intolerance, necrotizing enterocolitis, inguinal hernias, failure to thrive •Immunologic: Poor defense to infection Prematurity: Increased Disease Severity • Several studies have confirmed the high-risk status of premature infants • Among premature infants hospitalized with RSV and other viral pathogens: – 28-34% were admitted to the ICU – 7-22% required mechanical ventilation Boyce TG, et al. J Pediatr. 2000;137:865-70; Law BJ, et al. Paediatr Child Health. 1998;3:402-4; Imaizumi S, Agarwal S, Pereira GR, et al. APS/SPR/APA – 2001 convention 4-28-2001. Abstract Premature Infants are at High-Risk Altered lung development • Altered airway anatomy • Reduced lung function through early childhood Immature immune system • Impaired humoral and cellular immunity Prematurity: Interrupts Lung Development Premature Term Pseudoglandular Period Canalicular Period Saccular Period Alveolar Period (7 to 16 weeks GA) (16 to 26 weeks GA) (26 to 36 weeks GA) (36 to 41 weeks GA) • • The lungs of premature infants are underdeveloped at birth Although alveoli are present in some infants as early as 32 weeks GA, they are not uniformly present until 36 weeks GA *Pictures are artistic renditions of lung development and are designed to emphasize terminal acinus development & not the entire conducting airway system Behrman: Nelson Textbook of Pediatrics, 16th ed., 2000. Langston C, et al. Am Rev Respir Dis. 1984;129:607-13 Serum Antibody (IgG) Levels at Birth: Premature & Term infants 1100 Serum IgG (mg/100ml) 1200 1000 800 520 600 320 400 200 200 0 <28 wks GA 28-31 wks GA 32-35 wks GA Term Adapted from data and formulas as published by Yeung CY, Hobbs JR. Lancet. 1968;7553:1167-70 Summary: Risk of Severe Disease in Premature Infants • Hospitalization rates demonstrate that premature infants up to 36 wks GA are potentially high risk for severe respiratory distress • Premature infants, even those without a history of ventilation or oxygen use, are high risk due to – Altered airway anatomy-significant obstruction seen throughout early childhood – Immature immunity-impaired cellular and humoral immunity Congenital Heart Disease • Increased morbidity and mortality. Statistics among children hospitalized: – 25-33% admission to PICU – 11-24% mechanical ventilation – 3.4% fatality rate • CHD patients with associated pulmonary hypertension are at highest risk for complications. Navas L, et al. J Pediatr. 1992;121:348-54; Altman CA, et al. Pediatr Cardiol. 2000;21:433-8; Moler FW, et al. Crit Care Med. 1992;20:1406-13; MacDonald NE, et al. N Engl J Med. 1982;307:397-400; Khongphatthanayothin A, et al. Crit Care Med. 1999;27:1974-81 Risk Factors in CHD Patients • Compromised cardiorespiratory status at baseline • Altered pulmonary mechanics may contribute to disease severity • Pulmonary hypertension may exacerbate the adverse effects of respiratory disease • Inability to properly compensate for intercurrent disease Chronic Lung Disease: Increased Risk of Severe Respiratory Distress • Studies have confirmed the high-risk status of children with Chronic Lung Disease (CLD) • Among CLD children hospitalized viral processes: – 32% were admitted to the ICU – 17% required mechanical ventilation – 3.5% died within two weeks Navas L, et al. J Pediatr. 1992;121:348-54 Therapeutic Options for Bronchiolitis • Prevention – Limit exposure – Avoid daycare – Excellent hand washing – Passive immunoprophylaxis: Synagis® (palivizumab) • Supportive care • Overcoming airway obstruction and inflammation Prophylaxis: Reserved for the Highest Risk Children • RSV immunoprophylaxis is the only available safe and effective method for preventing severe RSV disease • Prophylaxis is reserved for high risk infants and children – Premature infants <36 wks GA are at a significantly elevated risk of severe RSV disease – Children with chronic lung disease, congenital heart disease, immunodeficiencies, and other high-risk conditions The IMpact-RSV Study Group. Pediatrics. 1998;102(3):531-7; Boyce TG, et.al. J. Pediatr. 2000;137:865-70; Imaizumi S, et al. Abstract # 2311:APS/SPR/APA-2001;Law BJ, et al. CAAC 1998 (abstract #MN-9); Meissner HC, et al. Pediatr Infect Dis J. 1999;18:223 IMpact-RSV Clinical Trial: Study Design Multicenter, randomized, placebo-controlled trial Infants 35 weeks gestational age (GA) or with bronchopulmonary dysplasia (BPD) were randomized (N=1502) to receive 5 injections of Synagis® (palivizumab) (15 mg/kg) or equivalent volume of placebo every 30 days 65 The IMpact-RSV Study Group. Pediatrics. 1998;102:531-537. Please see full prescribing information for Synagis® (palivizumab). IMPACT-RSV TRIAL RSV Hospitalization Rates by Subgroup Placebo: 1996-1997 IMpact-RSV trial (n=500) Synagis® (palivizumab): 1996-1997 IMpact-RSV trial (n=1,002) 12 10 11.0 10.6 9.8 8 6 4 5.8 4.8 2 2.0 0 All patients 55% All < 32 weeks GA 47% Reduction The IMpact-RSV Study Group. Pediatrics. 1998;102(3):531-7 All 32-35 weeks GA 80% Summary • There is significant viral pathogens, some producing annual epidemics and others that are common to our communities • Bronchiolitis is a major threat to the health of all infants and can lead to hospitalization and death • The threat of these viruses is greatest in high-risk groups, such as infants born prematurely and children with CLD or CHD • Treatment options are limited