* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
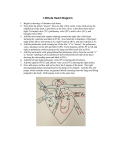
Download "Birth defect of Heart, its presentation and treatment"
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Electrocardiography wikipedia , lookup
Artificial heart valve wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Cardiac surgery wikipedia , lookup
Aortic stenosis wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
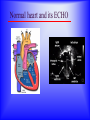
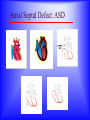
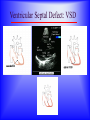
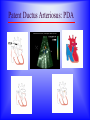
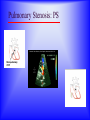
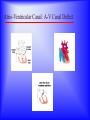
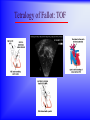
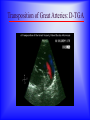
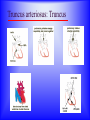
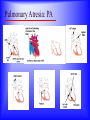
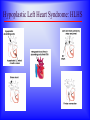
Sanjay Gandhi Postgraduate Institute of Medical Sciences Lucknow Department of Cardiovascular & Thoracic Surgery and Telemedicine network at SGPGIMS Welcomes participants in this presentation "Birth defect of Heart, its Presentation and Treatment" Nirmal Gupta Head Department of Cardiovascular and Thoracic Surgery SGPGIMS, Lucknow. U.P. Magnitude: Birth defects of Heart in India Every year 2 lakh children are born with congenital heart defects At least 60,000 of these need treatment in the 1st year of life Only 5000 get treatment because of lack of awareness amongst public in general and GP’s: delayed diagnosis Poor socio-economic status of families: delayed treatment Current facilities Requires highly trained and dedicated team of diagnostic facilities, Surgeons and Nurses Poor availability of facilities even in best hospitals Not a financially viable option for private setups Lack of trained manpower in the country (only 5 dedicated units other than SGPGIMS) SYMPTOMS "Birth defects of Heart, its Presentation and Treatment" Neonatal History Cyanosis Failure to thrive Exercise intolerance Shortness of breath Syncope Palpitation Chest pain NEONATAL HISTORY Cyanosis, shortness of breath. Did the child need to stay in the hospital after maternal discharge? Neonatal history Cyanosis Failure to thrive Exercise intolerance Shortness of breath Syncope Palpitation Chest pain CYANOSIS > 5g/dl of deoxygenated Hb False positive........... polycythemia False negative...........anemia Pathophysiology leading to cyanosis: Obstruction of systemic venous blood flow to the lungs Shunting of deoxygenated blood to left heart Desaturation of systemic arterial blood Neonatal history Cyanosis Failure to thrive Exercise intolerance Shortness of breath Syncope Palpitation Chest pain FAILURE TO THRIVE Poor cardiac output and increased myocardial energy consumption coupled with poor feeding due to S.O.B. Neonatal history Cyanosis Failure to thrive Shortness of breath Exercise intolerance Syncope Palpitation Chest pain EXERCISE INTOLERANCE Baby................ poor ability to suck and feed Child.................sedentary Pathophysiology leading to exercise intolerance: Poor cardiac output. Increased energy consumption by an overworked heart. Neonatal history Cyanosis Failure to thrive Exercise intolerance Shortness of breath Syncope Palpitation Chest pain SHORTNESS OF BREATH Some children may be short of breath without appearing in distress "Happily tachypnoec" Pathophysiology of S.O.B.: Increase pulmonary blood flow Interstitial edema Decreased oxygen diffusion Hypoxemia Neonatal history Cyanosis Failure to thrive Shortness of breath Exercise intolerance Syncope Palpitation Chest pain SYNCOPE Pathophysiology: Inability to increase cardiac output suddenly due to restricted left ventricular outflow, e.g. severe aortic stenosis, IHSS. Abnormal vasomotor tone resulting in vasodilatation when vasoconstriction is needed to maintain adequate blood pressure. Neonatal history Cyanosis Failure to thrive Exercise intolerance Shortness of breath Syncope Palpitation Chest pain PALPITATION Pathophysiology: Irregular rhythm Tachycardia Awareness of normal rate and rhythm. Neonatal history Cyanosis Failure to thrive Exercise intolerance Shortness of breath Syncope Palpitation Chest pain CHEST PAIN Rarely cardiac in origin. Look for extra cardiac causes: Skin, Musculoskeletal, Costochondral joints, Pleural membranes, Pericardium, Referred pain SIGNS "Birth defects of Heart, its Presentation and Treatment" SIGNS Inspection Palpation Auscultation INSPECTION Does the child appear ill? Decreased tissue oxygenation due to poor cardiac output or severe cyanosis Respiratory distress due to pulmonary edema or hypoxemia. Cyanosis Edema Distended neck veins due to increased right heart pressure leading to systemic venous congestion Clubbing of digits Chronic peripheral tissue hypoxemia SIGNS Inspection Palpation Auscultation PALPATION Peripheral perfusion, normal 1-2 seconds. Reflection of cardiac output. FA=BA, Normal = full Diastolic runoff = bounding Poor stroke volume = thready PALPATION ( Contd.) Precordium Increased cardiac output, ventricular hypertrophy = hyperactive Highly turbulent blood flow = thrill Indicators of ventricular hypertrophy or atrophy = RV, LV impulses Aortic stenosis, turbulent blood flow in ascending aorta = Suprasternal notch: thrill? Hepatomegaly, check below right and left costal margins. SIGNS Inspection Palpation Auscultation AUSCULTATION LUNGS Pulmonary edema = rales, crackles HEART First heart sound (S1): Closure of atrio-ventricular valves. Second heart sound (S2): A2: closure of aortic valve P2: closure of pulmonary valve Single S2 = absent pulmonary or aortic component or delayed closure of A2 superimposing P2 inaudible P2 in TGA Does the splitting of S2 vary with respiration? Added sounds: Gallop rhythm: S3, S4 AUSCULTATION (Contd.) Murmurs Grade: 1-6, one being the softest and six being the loudest. By definition grade four murmur is associated with a palpable thrill. Systolic murmur: Holosystolic: Shunting of blood between two structures , the pressure in one structure is higher than the other throughout systole Harsh: VSD Soft: Atrio-ventricular valve regurgitation Ejection: Increase in blood flow turbulence as systole progresses due to an increasing amount of blood flow through a restricted orifice Aortic stenosis Pulmonary stenosis Small VSD AUSCULTATION (Contd.) Mid-systolic: Increase volume of blood flowing through normal valves ASD Anemia Diastolic murmur: Early: Regurgitant blood flow from aorta or pulmonary artery into the ventricles Aortic insufficiency Pulmonary insufficiency Late: Austin Flint murmur Aortic regurgitation blood flow causes vibration of left ventricular free wall Systolic and diastolic murmur: Pressure difference between two structures during systole and diastole. PDA & Shunts and collaterals Congenital Heart Diseases and their Treatment "Birth defects of Heart, its presentation and treatment" Normal heart and its ECHO Atrial Septal Defect: ASD Coarctation of aorta Ventricular Septal Defect: VSD Patent Ductus Arteriosus: PDA Pulmonary Stenosis: PS Aortic Stenosis: AS Atrio-Ventricular Canal: A-V Canal Defect Tetralogy of Fallot: TOF Transposition of Great Arteries: TGA Transposition of Great Arteries: D-TGA Truncus arteriosus: Truncus Tricuspid Atresia: TA Pulmonary Atresia: PA Total Anomalous Pulmonary Venous Drainage: TAPVD Hypoplastic Left Heart Syndrome: HLHS Ebstein’s Malformation: Ebstein’s General guidelines: At birth Blueness at birth or immediately after Murmur of the heart Rapid breathing Low blood pressure General guidelines: At 2 – 6 months Difficulty in feeding- baby is unable to suck properly, sweats or starts rapid breathing while feeding Blue nails and toes and fainting spells Inadequate weight gain Recurrent chest infections General guidelines: In first 3 years of life Fainting spells Abnormal heart beats Child avoids rigorous activities Unable to play with his mates General guidelines for couples Drugs to avoid during pregnancy Strict “NO” to Isoretinoin, Thalidomide, Estrogens, Oral contraceptives, ACE inhibitors, Chloramphenicol, Chlorpropamide, Erythromycin, Tetracycline and Haloperidol. Anti-cancer drugs and Phenytoin are harmful but benefits outweigh the side effects. Epinephrine, Ephedrine, B-blockers and Promethazine do not pose any significant risk, though the research is inadequate In the end… “There are a million times more patients in India with congenital heart diseases than polio, but the government’s budget for the treatment of congenital heart diseases is miniscule in comparison” ….so the gap is of more than billions magnitude Thanks for your attention friends Can I have your questions, please.