* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Pediatric Cardiac Emergencies
Survey
Document related concepts
Cardiovascular disease wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Rheumatic fever wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
Congenital heart defect wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Atrial septal defect wikipedia , lookup
Coronary artery disease wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
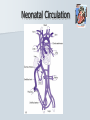
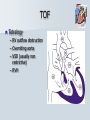
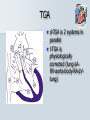
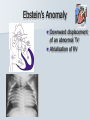
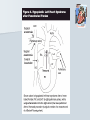
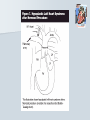
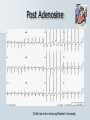
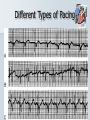
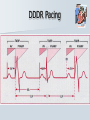
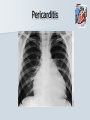
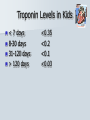
Pediatric Cardiac Emergencies Graham Thompson Francois Belanger Feb 26th 2004 Objectives Review transitional changes in pediatric cardiology CHD – presentations in ED, blue vs pink, ED Tx Post-op issues presenting to the ED Pacers SVT in the PED Acquired Cardiac Disease – Pericarditis – KD – ARF MIs in the pediatric world Cardiac Arrest PALS Guidelines (attached) Neonatal Circulation Changes at Birth Decreased PVR from expansion of lung and high PaO2 Increased SVR from stopping placental circulation Functional closure of PFO from high LA pressures Reversal of flow and then closure of PDA Closure of ductus venosus Slow change from R dominant to L dominant circulation (Malformations often cause changes to this pattern (can be life saving i.e. PDA in CoA!!) Normal Vitals for Children Case #1 4 do boy with central cyanosis Term baby of 17 yo girl, minimal prenatal care ROM 6 hrs, uncomplicated delivery Left hospital w/in 24 hrs Bottle feeding well until today, now only 1 oz/feed WOB increased over the day Case (cont) Brought into resusc room Hr 165 RR 75 BP 65/28 LA SpO2 79% R/A, cyanosed 100% supplied – SpO2 – 84% IV started, NS bolus 70 cc A/E good, clear, mildmoderate WOB S1 S2 (? Single) IV/VI systolic murmur Pulses good, liver 2cm BCM Font flat, soft, neuro intact Bld wk, ECG and CXR pending Congenital Heart Disease 0.5-0.8% of live births (not including PDA or bicuspid aorta) Increased in syndromes – T21 – endocardial cushion defects, ASD, VSD – XO – CoA, bicuspid AV Increased with maternal prenatal drugs – Lithium – Ebstein anomaly – VPA – CoA, HLHS, VSD, AS 40-50% dx in 1st wk, 50-60% by 1st month Frequency of major CHD (% of total) VSD ASD (sec) PDA CoA TOF PS AS d-TGA HLHS 25–30 6–8 6–8 5–7 5–7 5–7 4–7 3–5 1–3 HRHS Truncus TAPVR Tricuspid atresia Single ventricle DORV Others 1–3 1–2 1–2 1–2 1–2 1–2 5–10 * Excluding PDA in preterm neonates, bicuspid AV, physiologic PPS, and MVP Presentations Most complex CHD are picked up on routine prenatal ultrasound (up to 75%) Complex CHD is often picked up prior to D/C from the nursery with cyanosis or abnormal heart sounds BUT…….Timing and symptoms relate to physiologic changes of newborn and the lesion (obstruction vs shunt) so they may show up in the ED!!! Any newborn looking comfortably cyanotic is probably cardiac!! – mixing lesion 0-2 wks Duct dependant lesions Takes 2-14 days for duct closure May present to the ED more often, because of early D/C (duct hasn’t closed yet!) Most common are Left outflow tract obstructions (CoA, interrupted arch, AS, HLHS), TGA, TOF In the words of Dr. Patton – “Beware of the “septic”-like 2 wk old infant with poor pulses: is it possibly CoA or critical AS?” In st 1 year CHD that presents in failure (tachypnea, sweating with feeds, feeds >30 min, FTT, pallor) Most commonly related to L-to-R shunt (ie VSD) At birth, R pressures are high, shunt is minimal so defect may not present itself Drop in R side pressures and increased L pressures occurs over 6-8 wks causing shunt and symptoms Murmurs are not heard in nursery because lack of shunt Late TOF presentations that are relatively protected from failure by RVOT obstruction. May present with tet spells. Childhood Restrictive L-to-R shunts – ASD, Small VSD Mild CoA, mild AS – may present with fatigue or leg pain/wkness or HTN The very rare TOF Presentation of CHD Approach to CHD Dx Cyanotic – Increased Pulmonary flow – Decreased pulmonary flow (RV outflow obstruction) Acyanotic – Increased volume load (ASD, VDS, PDA) – Increased pressure load (LV outflow obstruction) Approach to CHD Hx in CHD Cyanotic episodes – Central vs peripheral Feeding pattern – – – – diaphoresis Stopping frequently Prolonged (>30 min) FTT Gestational age Maternal Hx of medications, infections Prenatal U/S Genetic D/O Previous child with CHD Exercise intolerance Syncope R/O sepsis stuff!!! Px in CHD VS – Tachypnea – Arrhythmias – 4 limb BPs (SBP in legs N > by 10, if not look for LVOT obstruction) – 4 limb SpO2 – T0C – hypermetabolic Colour Diaphoresis Wt gain Heart sounds and murmurs (don’t forget to listen to the back – CoA) Distal pulses, R/F delay Precordium Abdomen – HSM Clubbing Cyanotic Heart Disease Central vs Peripheral Central – 50 g/l of non-oxygenated Hgb – Level of hypoxia varies according to hct, so polycythemic kids can look cyanotic at higher SpO2s Peripheral – Perfusion issues Hyperoxic test Technically – Do gas – Give 100% O2 – After 10 min, redo gas – Mixing cardiac lesion won’t be able to get PaO2 > 100-150 Practically – SpO2 won’t get into 90% in mixing cardiac lesion Cyanotic Heart Disease The 5 T’s – Tetralogy Of Fallot (TOF) – Truncus Arteriosus – Tricuspid Lesions (atresia, Ebstein’s) – Transposition of the Great Arteries (TGA) – Total Anomalous Pulmonary Venous Return (TAPVR) + PA/severe PS TOF Tetralogy – RV outflow obstruction – Overriding aorta – VSD (usually non restrictive) – RVH TOF clinical 5 - 10% of CHD Most common cyanotic CHD after infancy Cyanotic or acyanotic depending on degree of RVOT obstruction – Blue if ++ obstruction = R-L shunt (present earlier) – Pink if minimal obstruction = L-R shunt RVH (felt under xyphoid) Loud, probably single S2 III-V/VI SEM at LSB TOF - Dx Boot shaped heart Decreased pulm. Vasc. 20% R sided arch RVH “Tet” Spells Most frequent in 1st 2 yrs (peak at 2-4 mo) After startle, crying or upon waking Hyperpnea, restless, increasing cyanosis, syncope Sudden decrease in pulmonary flow, increased R-L shunt Prolonged spells can lead to LOC, acidosis, szs Tx – – – – – – – Calm child Knee to chest or Squat position O2 Morphine 0.1-0.2mg/kg SC HCO3 if prolonged ketamine Phenylephrine to increase systemic pressures TGA d-TGA is 2 systems in parallel l-TGA is physiologically corrected (lung-LARV-aorta-body-RA-LVlung) TAPVR A – supracardiac B – cardiac C – cardiac D - infracardiac Truncus Tricuspid atresia No RA outflow Requires ASD (natural or balloon) to have R-L shunt. Requires PDA or VSD to allow L-R shunt RV usually really small, so Fontan works well Usually Dx at birth, but may be later Ebstein’s Anomaly Downward displacement of an abnormal TV Atrialization of RV Evaluation of Cyanotic Infant ABC IV access Physical exam Labs, hyperoxic test CXR Consider meds Call cardio PGE1 Relaxation of ductal smooth muscle Infusion of 0.05-0.2 ug/kg/min – 80 cc NS in 500ug vial run at BW = 0.1ug/kg/min (or 36cc in 225ug vial) Side effects – – – – Jitteriness Fever Hypotension Apnea Relative contraindication – TAPVR – may worsen systemic perfusion CXR in CHD Egg on a string – TGA Snowman – TAPVR Boot – TOF Super huge heart – Ebstein’s Backward E – CoA – notched ribs by collaterals Acyanotic Heart Disease RVOT obstruction presents with shock CoA VSD ASD Surgical Procedures Post-op issues in the ED Shunts – Can obstruct, especially passive flow (glenn) Think of this child presents with URTI or gastro causing dehydration BT shunts are active flow, and when obstructing have increased cyanosis and changed shunt murmur Glenn shunts are passive flow and present with SVC syndrome and decreased murmur – Can flood lungs If R-L shunt is too high, then may present similar to failure – tachypnea, crackles, wet chest Post-op issues in the ED MI – especially in atrial or arterial switches for TGA Arrhythmias – AV block for TGA, VSDs, ASDs – WPW in Ebstein’s anomaly – Atrial flutter Post-op issues in the ED Post pericardotomy syndrome – Sustained febrile period 1 wk – 2 months (mean 3-4 wks) after sx – Thought to be related to autoimmune response – Pericarditis symptoms, CXR and ECG – Tamponade may occur – Usually self limiting in 2-3 wks – Tx Bed rest NSAIDs Steroids Pericardiocentesis if needed. CHD presentations to ED 5 yr retrospective study at UCLA ED Only 8 new CHD presentations – – – – – – – Age ranged from 1 wk to 5 months ASD – 3 VSD – 1 AS – 1 ALCAPA – 1 CoA – 1 TAPVR – 1 – Savitsky E J.Emerg Med 2003, 24(3):239 CHD in the ED Really great references on CHD – Woods WA et al Emerg Med Reports 2003 24(6) – CHD in the ED – Woolridge DP et al Ped Emerg Med Reports 2002 7(7) – CHD in the PED Pt 1 – Woolridge DP et al Ped Emerg Med Reports 2002 7(8) – CHD in the PED pt 2 Case 3 mo boy to ED with grey spells Has happened 3 times in past 2 days Hasn’t taken more than 1 oz for past 3 feeds Intermittent WOB, no URTI sympt. Had been seen last month for decreased feeding, difficulty breathing, stuffy nose and pallor– dx – bronchiolitis Case (cont) Looked dusky at triage Taken directly to resusc. room O2 and monitors, IV started immediately Pinked up with O2, SpO2 = 99% ECG SVT Post Adenosine Child had echo showing Ebstein’s Anomaly Non-pharmacologic Tx for SVT Interrupts about 25% of SVT Cooperative children – Blow against straw – Crouch down Uncooperative or Small Children and Infants – – – – Push legs into chest Carotid sinus massage Ocular pressure Diving reflex Carotid massage for SVT Randomized X-over trial of carotid massage vs valsalva maneuver 148 episodes No difference in efficacy Total of 25% responded to one of the therapies Lim SH et al Ann Emerg Med 1998 31(1):30 Carotid massage is not recommended in young patients (but no reason given!) Paed Drugs 2000 2(3):171 SVT and the Diving Reflex increased parasympathetic tone to the heart causing bradycardia in association with systemic vasoconstriction – – – – ice cube application to the lip and bottom nose immersion of the head into a basin of ice and water for 4-6 s application of a cold, wet facial cloth to the face application of an ice bag to the face “The diving reflex is much more effective than the ‘usual’ vagal maneuvers such carotid sinus massage, gag reflex or rectal stimulation” avoid inducing apnea and aspiration; and avoid prolonged application of ‘cold’ to the face. Moak JP Prog Ped Card 2000 11(1):25 The Diving Reflex and SVT The use of the diving reflex to terminate a case of paroxysmal supraventricular tachycardia (PST) is described in a 2-week-old infant who presented in severe congestive heart failure with supraventricular tachycardia at a rate of 300. The infant's face was placed in a basin of ice water at 5 degrees C. for 5 seconds with manual occlusion of the infant's nostrils to prevent aspiration. The PST converted to a sinus rhythm of 120 within 3 seconds of facial immersion. Hamilton J Am Heart J 1979 97(3):371 Ice for SVT Has been reported to abort up to 90% of SVT in infants Supposedly initiates the “diving reflex” 1st report 1980 – – – – Filled plastic bag with equal volume of water and crushed ice Covered entire face “to preauricular area” Conversion occurred within 15 seconds (n=10) “We can only speculate on the emotional trauma of the ice bag technique” Do you have to cover the whole face? Do you have to cause apnea? – still controversial, no good data Probably shouldn’t cover mouth and nose Complications? Craig JE et al J Pediatr 1998 133:727 Medications for SVT Adenosine – – – – Transient Av node blockade 0.1 mg/kg to max of 6 mg Repeat at 0.2 mg/kg to max of 12 mg Don’t get your knickers in a knot when the monitor shows a flat line – Needs proximal IV with rapid NaCl bolus ‘cause ½ life is a mere 15 seconds Verapamil – CONTRAINDICATED in children < 1yo because of several studies demonstrated increased risk of hypotension, malignant arrhythmias and electomechanical dissociation – 0.1 mg/kg max dose 5mg over 15 minutes Atkins, DL Clin Ped Emerg Med 20012(2):107 North American Society of Pacing and Electrophysiology Generic Pacemaker Code I Chamber(s ) Paced II Chamber(s) Sensed O, None O, None A, Atrium III Response to Sensing IV Programmability, Rate Modulation V Antiarrhythmi a Function O, None O, None O, None A, Atrium T, Triggered P, Simple programmable P, Pacing (antitachyarrhyt hmia) V, Ventricle V, Ventricle I, Inhibited M, Multiprogrammable S, shock D, Dual (A + V) D, Dual (A + V) D, Dual (T + I) C, Communicating R, Rate Modulating D, Dual (P + S) Different Types of Pacing DDDR Pacing Pacemaker Complications Most common include – infection at site – Electromagnetic interference Cell phones – unlikely Antitheft devices – unlikely MRI, cautery etc. Case 14 yo girl gradual onset of chest pain x 2d Now acutely SOB, increased pain Worse when lying down Recent viral URTI symptoms Previously well Pericarditis Pericarditis Normal pericardial fluid volume = 10-15cc Inflammatory response causes increased fluid accumulation (can be > 1L) Symptoms – precordial pain improved with sitting, cough, dyspnea, vomiting, fever Px – friction rub (variable), muffled heart sounds, tachy, venous distention, pulsus paradoxus Etiology of Pericarditis CONGENITAL ANOMALIES INFECTIOUS – Absence (partial, complete) – Cysts – Mulibrey nanism (muscle, liver, brain, eye) with congenital pericardial thickening and constriction – Viral (coxsackievirus B, EBV, influenza, adenovirus) – Bacterial (Streptococcus, Pneumococcus, Staphylococcus, Meningococcus, Mycoplasma, tularemia) – Immune complex (Meningococcus, Haemophilus influenzae) – Tuberculosis – Fungal (histoplasmosis, actinomycosis) – Parasitic (toxoplasmosis, echinococcosis) CONNECTIVE TISSUE DISEASES – – – – – METABOLIC-ENDOCRINE – Uremia – Hypothyroidism – Chylopericardium HEMATOLOGY-ONCOLOGY – Bleeding diathesis – Malignancy (primary, metastatic) – Radiotherapy-induced OTHER – – – – – – Rheumatoid arthritis Rheumatic fever Systemic lupus erythematosus Systemic sclerosis Sarcoidosis Trauma Iatrogenic (catheter related) Postpericardiotomy Aortic dissection Idiopathic Familial Mediterranean fever Pericarditis - Tx To tap or not to tap? – – – – No good data In typical viral pericarditis, probably don’t have to If any doubt of bacterial causes, just do it Other reasons to tap Significant symptoms Possible malignancy Abnormal diastolic fnctn on echo NSAIDs, steroids. Again, no good evidence. Wise words from Dr. Patton ARF Major Criteria – – – – – Carditis Polyarthritis Chorea Erythema Marginatum Subcutaneous Nodules Minor Criteria – Clinical Fever Arthralgia – Investigations Increased ESR or CRP Prolonged PR interval Plus Evidence of GAS infection (swab, ASOT, antiDNase B) Dx = 2 major criteria, 1 major + 2 minor Case 4 mo boy transferred to pediatrics for significant HSM and fever for 7 days Very fussy, not tolerating feeds Erythematous blanching rash on day 3 now gone WBC - 50’s consistently, no blasts seen hgb 99 -105 plts low 400’s Cultures negative Mild resp distress, likely b/c HSM (CXR N) Case (cont) Repeat SWU negative U/S abdo – significant HSM hem/onc investigations started At 11 days – plt – 1340, rpt at 1360 Echo – 3 giant coronary aneurisms Dx of KD Supporting Evidence for KD Sterile pyuria – 70% Arthritis – 40% GI symptoms (hydrops of GB and diarrhea) – 25% Aseptic meningitis Anterior uveitis Irritability Elevated ESR Thrombocytosis at 1 wk from start of symptoms Incomplete KD At least 10% of children will CAAs never meet diagnostic criteria Review of 127 pts Tx for KD – 36% did not meet criteria, but this grp had higher incidence of CAAs than those who did meet criteria Infants < 1 y have up to 45% incomplete KD Up to 30% of atypical KD < 1yo had CAAs Incomplete KD in Infants Review of KD Dx in children < 6 mo Of 33 cases reported, 28% had atypical disease compared to 7-10% in > 1yo. Genizi et al Clin Pediatr 2003 42:263 % fever 97 rash 82 conjunctivitis 61 Extremities 61 MM 57 nodes 30 KD-Initial Therapy Lang et al Best Pract Res Clin Rheum 2002 16(3):427 IVIG in KD Dosing schemes – 400 mg/kg x 4 days – 1 g/kg x 1 – 2 g/kg x1 Highest reduction of CAAs and quickest relief of fever in 2g/kg dose May be repeated fever not responsive in 24-48 hrs Tx and Timing of Presentation Children Tx with IVIG within 10 days of symptoms have reduced rates of giant CAAs (<2%) compared with those Tx at 15 days (6.1%) Benefit after 10 days has not been adequately studied. Current suggestion include IVIG if still evidence of active inflammation (ie fever) Case Risk factors for MI in Kids MI Etiology in Neonates Congenital heart disease – – – – – Anomalies of the origin of the coronary arteries Anomalies producing left ventricular hypertrophy Pulmonary atresia with intact ventricular septum Transposition of the great arteries Truncus arteriosus Endocardial fibroelastosis Mediocalcinosis of the coronary arteries Poor coronary perfusion Hypoxia Sepsis Disseminated intravascular coagulation Embolism MI Etiology in Children Kawasaki disease Idiopathic or inherited cardiomyopathy Myocarditis (Viral, Rheumatic) Collagen vascular disease Substance abuse – – – – – Homocysteinuria Familial hypercholesterolemia Progeria Pseudoxanthoma elasticum Mucopolysaccharidoses, Fabry's, Alkaptonuria, Hurler's syndrome, Pompe's Disease – Hyperbetalipoproteinemia, familial combined hyperlipidemia, and hypoalphalipoprotenemia – Cocaine – Glue sniffing Chest trauma Iatrogenic Post-cardiac transplant Post bypass hypoperfusion Other complications of congenital heart disease surgery, especially damage to coronary arteries. Genetic/metabolic disorders Other systemic disorders – – – – Nephrotic syndrome Sepsis Occult malignancy Idiopathic or premature coronary artery disease without predisposing genetic disease Symptoms of MIs in Kids – Nausea – Vomiting – Irritability – Pallor – Diaphoresis – Poor feeds – Syncope – Weakness – WOB/SOB – Anxiety – Pain Pediatric MIs on ECG Wide Q waves (>35 milliseconds) – Particularly I, aVL, V5, V6, but any lead other than aVR ST segment changes of >2 mm – Elevation in any lead, especially in the presence of reciprocal changes. – ST depression in V1 -V3 . Ventricular arrhythmias – Calculated QTc of >0.48. Based on autopsy proven MI ? Prospective use? (Towbin JA Am J Card 1992 70:1545) Reich JD et al AJ Emerg Med 1998 16(3):296 Troponin Levels in Kids < 7 days 8-30 days 31-120 days > 120 days <0.35 <0.2 <0.1 <0.03 Tx for MI in Children Very small literature bank, most on KD kids Only case reports of streptokinase or urokinase Theoretical risk of using streptokinase as it is contraindicated in pts with recent GAS infection (and what kid doesn’t meet that criteria?!) tPA has been used – Case study from 2000 in 7yo boy post-KD – Resolution of symptoms, improved LV function and no thrombus seen on cath at 1 month (echo + @ presentation) Krendel et al Ann Emerg Med 2000 35(5): 502 Tx for MI in Children Angioplasty pretty difficult in children <5 IIa/IIIb inhibitors are not approved in children (and may have a higher risk of bleeding?) Cardiac Arrests in Kids 20 yrs of cardiac arrest attended by EMS Of 5505 arrests, 2% were in children (017 y.o.) Overall survival = 5% Engdahl J et al Resuscitation 2003 58:131 Cardiac Arrests in Kids Majority of CA occur in 0-1 yo Mostly related to SIDS and respiratory causes Cardiac Arrests in Kids