* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Emergencies in adults with congenital heart disease: a guide for the
Survey
Document related concepts
Cardiac contractility modulation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Artificial heart valve wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Infective endocarditis wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Aortic stenosis wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
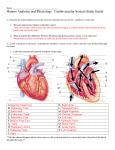
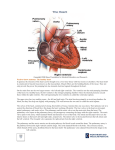
Adults with congenital heart disease: a survival guide R. Dobson Clinical Research Fellow Congenital Heart Disease • CHD is by far the commonest congenital abnormality and >85% of these patients survive to adult life • From 2010 approximately 1 in 150 young adults will have CHD; 1 in 300 will have lesions of moderate or severe complexity • Some conditions may not be diagnosed until adulthood (e.g. ASD, aortic coarctation) • Your local cardiologist might not know much more than you do! General considerations ABCDE & stabilise patient Seek information Get help & plan definitive management ABCDE • As per ALS but… • Beware atrial flutter – may look like sinus rhythm • BP measurements may be unreliable if previous surgical shunts – look for lateral scars • Cyanosed patients can often tell you what their usual SpO2 is Seek information • • • • Good history Previous clinic letters – check Portal Old ECGs Google image search or wikipedia for unfamiliar terms • For each patient try and describe how the blood goes round Get help • Think what help is available locally • Phone GJNH switchboard 0141 951 5000 – Mon-Fri 9-5pm Scottish Adult Congenital Cardiac Service – OOH ask for CCU at GJNH • Will be able to access clinic letters, old ECGs and echoes instantly and send them through • Can speak to SpR on call for further advice Emergencies in ACHD 1. 2. 3. 4. 5. Supraventricular tachyarrhythmia Blackout / collapse Acute aortic syndromes Endocarditis Massive haemoptysis 1. Supraventricular tachyarrhythmia Case history • • • • • • • 35yo male “Fontan repair” for “tricuspid atresia” Sudden onset palpitations 6h ago Light headed on exertion Feels OK at rest Undistressed, looks well On warfarin for years ABCDE • Talking • RR 20 SpO2 97% lungs clear • BP 100/60 L arm, HR 100bpm regular, warm peripheries. No murmurs • Apyrexial, BM 5.6, E4 V5 M6 • Abdomen soft non-tender • Bloods OK – INR therapeutic ECG Previous ECG Seek information – what is a Fontan? What do you do now? 1. 2. 3. 4. Do nothing? Urgent DC cardioversion? Start flecainide? Start amiodarone? What do you do now? 1. 2. 3. 4. Do nothing? Urgent DC cardioversion? Start flecainide? Start amiodarone? What happened • • • • Admitted to CCU Fasted Started amiodarone Plan for DCCV if amiodarone unsuccessful Then… • 5 hours into his amiodarone the patient became very unwell. Repeat ECG showed ventricular rate of over 200bpm • Shut down, drowsy with BP 60/24 • Cardiac arrest call – single DC shock into asystole • Prolonged CPR. Intubated and ventilated. After 30 minutes worsening acidosis with no clear reversible cause and no sign of recovery – resuscitation ceased What went wrong • Fontan is a passive circulation and utterly dependent on central venous pressure 1. Patient fasted – dehydration, reduced systemic venous return – Cardiac output falls... 2. Amiodarone given – negatively inotropic – Cardiac output falls... 3. Slows to 1:1 conduction of flutter – Cardiac output falls... 4. Positive pressure ventilation increases intrathoracic pressure. CVP is already low no longer sufficient to drive blood to lungs – CPR unsuccessful How to do it • Get advice • Keep patient fasted but give IV fluids (crystalloid) to maintain CVP • Contact anaesthetist, explained potential seriousness of situation • Cautious GA to avoid excessive vasodilation, minimum of PEEP • DCCV performed successfully with single shock Key points • Understand the circulation • Patients can look deceptively well initially • SVT poorly tolerated in single ventricle hearts (ditto for severe ventricular impairment and obstructive valve lesions) • Avoid ‘anti’ arrhythmics – unpredictable effect • Electricity is clean and quick 2. Blackout / collapse Tetralogy of Fallot • Complete repair (most adult patients) involves closure of VSD and enlargement of RVOT (infundibular resection or transannular patch). • Severe / free pulmonary regurgitation and progressive RV dilatation is almost universal • Can be tolerated well for years Case History • 27 year-old female with repaired tetralogy of Fallot • Fit and well, no medications • Told has a leaky heart valve which will need to be replaced soon • GP referral with 2 episodes T-LOC past 24 hours at rest. Sudden onset, no warning. No witnesses. ABCDE • Talking, undistressed • RR 20 SpO2 97% lungs clear • BP 50/30 R arm. HR 80bpm regular, warm peripheries. S1 + ESM + S2 + EDM • Apyrexial, BM 5.6, E4 V5 M6 • Abdomen soft non-tender Hypotension in CHD • Why is the BP so low? • How can you tell? Blalock-Thomas-Taussig shunt • Subclavian to ipsilateral branch pulmonary artery • Increases pulmonary blood flow • Look for a lateral thoracotomy scar! 12 lead ECG Seek information • Detailed history • Previous ECGs and clinic letters • She had a right BT shunt prior to corrective surgery • Echo / MRI – severe pulmonary regurgitation with a severely dilated right ventricle and referred for PVR • Holter 2/12 ago showed NSVT Get help • Local cardiologist • ACHD service Management • Monitored bed • Basic bloods, echo • Treat the haemodynamic lesion – may need valve replacement • May need EP studies (VStim) to risk stratify • If symptoms infrequent could consider ILR (Reveal) Issues • 20 year survival in ToF reported at 80-99% • Sudden death occurs in 2.5% per decade of F/U • A number of risk factors identified (QRS >180ms, age at time of surgery, high grade ectopy on Holter, impaired LV) • No clear consensus on risk stratification and device therapy • No role for prophylactic antiarrhythmics 3. Acute aortic syndromes Case history • 30 year-old male • BP checked a couple of times in the past year – told it was “high” but no further action • Sudden onset severe interscapular back pain • Looks distressed and unwell ABCDE • Talking in sentences • RR 24 SpO2 98% 2LPM nasal cannula, lungs clear • BP 200/110 R arm, HR 110bpm reg cool peripheries. S1 + ESM + S2 + EDM • Apyrexial E4 V5 M6 equal tone and reflexes all 4 limbs • Abdomen soft and non tender • What else do you want to check on examination? • What is the most likely diagnosis? Initial management • Wide bore IV access • CT angiogram aorta • Echo if available – check for aortic valve involvement +/- effusion but should not delay transfer Get help • Phone a cardiac surgeon! • If type A dissection urgent cardiac surgery is the only treatment (mortality is 1-2% per hour) Coarctation of the aorta • Severe hypertension refractory to treatment • Premature MI, stroke, dissection • Associated with bicuspid aortic valve and ascending aortic aneurysm • Stenting or surgery • Always check femorals 4. Endocarditis Case history • 30 year-old male • Underwent heart surgery 4 weeks ago • Surgeons placed a tissue valve and did something to the blood vessel connected to the heart as well • This week intermittent night sweats, shivering. Poor appetite, lethargic. Light headed on exertion Annals of Thoracic Surgery ABCDE • Airway patent • SaO2 97% air, RR 18, lungs clear • BP 110/70, HR 100bpm, S1 plus ESM plus pS2, warm peripheries • E4V5M6, BM satisfactory, no focal neurological deficit. • Abdomen soft and non-tender. No rashes. Temp 37.8oC Initial management • Lots of blood cultures • Imaging • Serial 12 lead ECGs if suspect aortic valve involvement – why? • Antibiotics as per microbiology Seek information • Get clinic letters, op note • Had a bicuspid aortic valve with severe stenosis and moderate regurgitation in association with dilated aortic root 55mm • Underwent tAVR and root replacement (Bentall) Annals of Thoracic Surgery Get help • • • • Admit CCU Local cardiology review asap Microbiology opinion Phone tertiary centre – let surgeons know Which one of these is not in the modified Duke criteria? 1. 2. 3. 4. Paravalve abscess Glomerulonephritis Fever >37.5°C Pulmonary embolus Which one of these is not in the modified Duke criteria? 1. 2. 3. 4. Paravalve abscess Glomerulonephritis Fever >37.5°C Pulmonary embolus Clinical course • Transferred to tertiary centre D2 of admission • Operated on next day after CT • 7 hour procedure with massive blood loss and two periods of circulatory arrest • Global hypoxic brain injury • Three months in hospital Other considerations • Right sided valve endocarditis also very common e.g. ToF patient with preexisting pulmonary regurgitation and poor dental hygiene – tends to be more insidious and better tolerated • Always think endocarditis if CHD patient nonspecifically unwell and / bloods not completely normal e.g. anaemia (usually Fe deficiency), mild leucocytosis 4. Haemoptysis in cyanotic patients Case history • 40 year old female with large VSD and Eisenmenger syndrome • Coughed up about two cupfuls of fresh blood • Recent chest infection and just finished course of antibiotics ABCDE • Airway patent...for now • SaO2 80% air, RR 18, lungs sound relatively clear • HR 88 regular, BP 130/86. Warm peripheries. Clubbed++ Loud second heart sound, no murmurs • E4V5M6, BM OK, No neurological deficit • Abdomen soft and non-tender Initial management • • • • • • Always consider HDU Anaesthetist Wide bore IV access FBC – beware a normal Hb X-match Keep fasted Seek information • What is Eisenmenger syndrome? Eisenmenger physiology • A large uncorrected shunt (e.g. VSD, PDA) with bidirectional flow and pulmonary hypertension • Systemic BP = pulmonary artery BP! • Prone to bleeding from dilated, friable bronchial arteries, PE, pulmonary AVMs, bronchiectasis • A leading cause of death in these patients www.yorksandhumberhearts.nhs.uk Mayo clinic Medscape Get help & further management • Respiratory review locally • Control BP but avoid vasodilating antihypertensives (increase R to L shunt) • Carefully titrated opiates / benzodiazepines if distressed • CTPA • Interventional radiology Eisenmenger physiology • A large uncorrected shunt (e.g. VSD, PDA) with bidirectional flow and pulmonary hypertension • Systemic BP = pulmonary artery BP! • Prone to bleeding from dilated, friable bronchial arteries, PE, pulmonary AVMs, bronchiectasis • A leading cause of death in these patients ABCDE & stabilise patient Seek information Get help & plan definitive management Questions