* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Impact of Traumatic Brain Injury Among Recently Returned
Alzheimer's disease wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Child psychopathology wikipedia , lookup
Diagnosis of Asperger syndrome wikipedia , lookup
Major depressive disorder wikipedia , lookup
Psychological trauma wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Post-traumatic amnesia wikipedia , lookup
Asperger syndrome wikipedia , lookup
Retrograde amnesia wikipedia , lookup
Symptoms of victimization wikipedia , lookup
Combat stress reaction wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Alcohol withdrawal syndrome wikipedia , lookup
Treatment of bipolar disorder wikipedia , lookup
Externalizing disorders wikipedia , lookup
Conversion disorder wikipedia , lookup
Memory disorder wikipedia , lookup
Depression in childhood and adolescence wikipedia , lookup
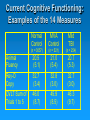
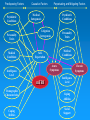
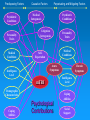
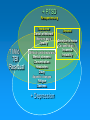
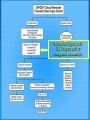
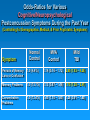
Roles of Neuropsychology and Psychology following Positive TBI Clinical Reminders: The Evaluation and Treatment Process Rodney D. Vanderploeg, Ph.D. Tampa VAMC VA Psychology Leadership Conference/APA May 18, 2007 Objectives Provide an overview of the TBI Clinical Reminder screening process Describe a model follow-up evaluation and treatment process Describe when and how neuropsychological evaluations should be completed Describe other roles of psychology following positive TBI Clinical Reminders Although I love Harry Potter There is No Magic! And, things like this are Pseudo-Magic “Automatic Clock Drawing Test” Featured in the Journal of the American Geriatrics Society, NIH, and the American Bar Association ElderLAW ENEWS. New! 5 minute evaluation If you want to know if someone had a Traumatic Brain Injury (TBI) ASK THEM: Did you experience a physical trauma or injury that resulted in your being: • Knocked out / Rendered unconscious, • Dazed and confused for several minutes, and/or • With memory gaps for some or all of the immediate period after the event If the answer is “yes”, then they had a TBI That is what the “TBI Screening Reminder” Does TBI Screening Reminder April 2007 So, what really are the issues? 1. 2. 3. 4. 5. 6. 7. Who has ongoing symptoms and problems? What are these symptoms and problems due to (TBI, PTSD, Depression, Anxiety, Somatoform Disorder, malingering, combinations of conditions)? What is the appropriate treatment for any identified problems/conditions? Who is responsible for providing the assessment and treatment? Who is responsible for coordinating this process? When should this be done locally, and when should it be done by regional specialists? What are the roles of psychology in points 3-6? “TBI Screening Reminder” Functions Identify possible OIF/OEF Participants Confirm deployment to OIF/OEF Theatres of Deployment Screen for TBI if deployed in OIF/OEF Theatres Identify those with an OIF/OEF-related history of TBI Criteria for Severity of TBI Mild Moderate Severe LOC < 30 min with normal CT &/or MRI LOC < 6 hours with abnormal CT &/or MRI LOC > 6 hours with abnormal CT &/or MRI GCS 13-15 GCS 9-12 GCS < 9 PTA < 24hr PTA < 7days PTA > 7days Don’t confuse combat-trauma psychological confusion with post-TBI PTA (i.e., inability to lay down new memories and therefore having post-TBI “memory gaps”) Screening Questions: 4 Sections Section 1: Trauma Events Section 2: Immediate Disturbance of Consciousness Symptoms after Events Section 3: New or Worsening Symptoms after the event Section 4: Current Symptoms Screen Interpretations A “no” response to any of the sections terminates screening and is a “negative screen” A “yes” response to ALL FOUR sections is a “positive screen” Section 1: Trauma Events Section 2: Immediate Symptoms Section 3: New/Worsening Symptoms Section 4: Current Symptoms Positive TBI Screen: Follow-up Positive replies in all four sections constitute a positive screen Positive screens automatically generate a consult to a TBI specialist or clinic This specialist/clinic has 1 week to initiate contact with patient for more detailed follow-up evaluation Initial treatment trial is based on positive problems on this follow-up evaluation What to Know: Relevant Background (1) Mild TBI Symptoms There is no symptom that is unique to or diagnostic of mild TBI Many postconcussion symptoms occur in normal healthy individuals All symptoms/problems overlap with one or more other conditions (PTSD, Depression, Anxiety, Chronic Pain, Somatoform Disorder, chronic health conditions) What to Know: Relevant Background (2) In prospective cases (non-clinical, nonlegal) virtually all symptoms of mild TBI resolve within 1 - 3 months Cognitive Emotional Physical Yet, a subgroup (about 10-15%) continue to experience a postconcussive syndrome Psychological factors play a large role in symptom presence in this subgroup What to Know: Relevant Background (3) In this subgroup (of about 10-15%) There is no relationship between symptom complaints and objective findings on: • Neuropsychological Testing • Physical Examination • Neurological Examination Again, this is because psychological factors play a large role in symptom complaints Predisposing Factors Psychiatric Conditions Personality Traits Medical Conditions Causative Factors Medical Iatrogenesis Personality Traits Medical Conditions SelfExpectation Acute Symptoms mTBI Coping Abilities Psychiatric Conditions Litigation Iatrogenesis Intelligence Level Demographic Characteristics Perpetuating and Mitigating Factors Chronic Symptoms Intelligence Level Coping Abilities Social Support Predisposing Factors Psychiatric Conditions Personality Traits Medical Conditions Causative Factors Perpetuating and Mitigating Factors Medical Iatrogenesis Psychiatric Conditions Litigation Iatrogenesis Medical Conditions SelfExpectation Acute Symptoms Intelligence Level mTBI Demographic Characteristics Coping Abilities Personality Traits Chronic Symptoms Intelligence Level Coping Abilities Psychological Contributions Social Support Issue One 1. Who has ongoing symptoms and problems? Anyone who responds positively to all four of the TBI Clinical Reminder sections Section 1:Trauma Event(s) Section 2:Immediate Disturbance of Consciousness after Event(s) Section 3:New or Worsening Symptoms after the event(s) Section 4:Current Symptoms Issue Two: Symptom Etiologies 2. What are these symptoms and problems due to (TBI, PTSD, Depression, Anxiety, Somatoform Disorder, malingering, combinations of conditions)? Initial post-TBI Clinical Reminder Assessment (at Tampa and elsewhere) Telephone Administration of: History Questions (e.g., confirmation of exposure, details of TBI severity, history of symptom course), Review of bodily systems and associated complaints, etc. Neurobehavioral Symptom Inventory (22 items rating postconcussive symptoms) PTSD Checklist (PCL) Pain symptoms Issue Two: Symptom Etiologies Interpretation of Initial Assessment Findings What are the most likely etiologies for the symptoms? What etiology(s) is/are primary? (Does PTSD, chronic pain, sleep disturbance likely explain the cognitive symptoms?) Would successful treatment of the primary etiology likely resolve most or all of the symptoms? Referring and Triaging: Refer accordingly for further evaluation and/or treatment Issue Two: Symptom Etiologies When to Refer Refer if the evaluation/referral will: Tell you something you don’t already know Make a difference in the patient’s treatment or management Turning Down a Consult for Neuropsychological Assessment Referral received and chart reviewed. Veteran currently has severe symptoms of PTSD and chronic headaches. Given this, his cognitive complaints of memory and concentration problems are expected. If testing were performed in this situation, any cognitive impairments would likely be attributed to the severity and extent of the mental health problems. Testing would not clarify diagnostic issues nor guide treatment - because mental health and pain management treatment should to be the main focus at this time. Once his mental health and pain symptoms are better managed, and rated as no worse than mild to moderate, if cognitive symptoms remain, a re-referral at that time may be clinically useful. Issue Two: Symptom Etiologies Follow-up Additional Specialized Assessments (and then treatment) TBI: PNS or PSCT (PM&R, (Neuro)Psychology, Speech, Psychiatry) PTSD: PTSD Program Chronic Pain: Pain Program or PM&R Somatoform Disorder(s): ????? Depression, Anxiety, Stress: MHC Seizures, Neurologic Conditions: Neurology Issue Three: Appropriate Treatment(s) Treat the primary condition(s), the one(s) that explains most or all of the symptoms Don’t invest time and effort in conditions that account for only small amounts of symptom variance Just because a condition was/is present (e.g., history of mild TBI), doesn’t mean it should be the focus of further assessment or treatment if other conditions are primary + PTSD Re-experiencing Avoidance Social withdrawal Memory gaps Apathy ? Mild TBI Residual Difficulty with decisions Mental slowness Concentration Headaches Dizzy Appetite changes Fatigue Sadness + Depression Arousal Sensitive to noise Concentration Insomnia Irritability Issue Four: Who is Responsible? TBI Clinical Reminder: Primary and Specialty Clinics (including Urgent Care, MHC, PTSD, Dental, etc.) Initial Follow-up Assessment: Polytrauma Program staff (Level II: PNS or Level III: PSCT), SCI Program staff, or Local Designated Specialist(s) - Physician (e.g., Neurologist, PM&R physician) Issue Four: Who is Responsible? (cont.) Subsequent Evaluations/Treatments: TBI: PNS or PSCT (PM&R, (Neuro)Psychology, Speech, Psychiatry) PTSD: PTSD Program Chronic Pain: Pain Program or PM&R Somatoform Disorder(s): ????? Depression, Anxiety, Stress: MHC Seizures, Neurologic Conditions: Neurology Primary & Specialty Clinics Polytrauma Program staff, SCI Program staff, or Designated Specialist(s) Programs / Clinics for Identified Conditions Issue Five: Coordination of Care Responsibilities If a Level I, II, or III Polytrauma Program, then the polytrauma team If not, the system is not clear who is responsible for making sure evaluations are completed, treatments are initiate, and symptoms/problems are resolving But, if treatment is not successful within a reasonable time (e.g., 90 days), patients should to be referred to a PNS or PRC Issue Six: Local versus Regional Care If the facility has a designated TBI specialist who is assigned to respond to the TBI Clinical Reminders, then initial assessment and treatment should be local If not, assessment should be done by the nearest PNS or PSCT staff If that assessment indicates that local resources can provide the treatment, fine; if not, and the problems are deemed to be TBI-related, then the nearest PNS Issue Seven: Role(s) of Psychology / Neuropsychology Members of the PNS or PSCT staff Assessment and treatment if indicated Neuropsychological Evaluations (15% of cases) Psychological Assessments (15-75+% of cases) TBI Rehab Interventions • Mild TBI Education & Support • Compensatory Training / Cognitive Remediation Stress Management, Education, Support Specialty Treatment • PTSD, Depression, Anxiety, Chronic Pain Important Mild TBI Facts Causes of Persistent Postconcussion Symptoms “Expectation as Etiology” and/or “The Good Old Days” Symptom Mis-Attribution Willey Mittenberg, Ph.D. “Diagnostic Threat” Julie Suhr, Ph.D. Expectation as Etiology Controls asked to imagine symptoms of a mild TBI “expected” symptom presence and severity very similar to mild TBI patients’ actual symptoms Mild TBI patients “under-estimated” the frequency and severity of pre-MTBI symptoms and problems Athletes “expected” lower levels of postconcussion problems than non-athletes Athletes with a concussion “over-estimated” pre-concussion levels of symptoms Mild TBI “Diagnostic Threat” Non-clinical evaluations of college students with a remote history of mild TBI (many months earlier) Neuropsychological Test Performance If told they are participating in a study of the effects of mild TBI, their performance is worse than, If told they are simply participating in a study of cognitive functioning in college students The “context” of the evaluation matters! Mild TBI Treatment Change expectation and attribution of symptoms Provide education Education regarding mild TBI Education regarding symptoms and their course Provide Support/Treatment Stress management Psychological and cognitive coping strategies and resources Cognitive-Behavioral therapy If There is Time which there will not be What to Expect: Literature Review Findings Mild TBI Findings Neuropsychological Test Performance Postconcussion Symptoms Causes of Postconcussion Symptoms Treatment of Mild TBI Neuropsychological Test Performance Mild TBI: Neuropsychological Meta-analytic Studies (1) (Schretlen & Shapiro, 2003) A second recent meta-analytic study found that overall neuropsychological effect size (d) for MTBI in prospective studies was 0.24 Categorized into 4 time-since-injury intervals the effect sizes were: < 7 days 7-29 days 0.41 0.29 30-89 days 0.08 > 89 days 0.04 Mild TBI: Neuropsychological Meta-analytic Studies (2) (Belanger, Curtiss, Demery, Lebowitz, & Vanderploeg, in press) A third recent meta-analytic study found the following, categorized into two time-sinceinjury intervals and three types of studies: Time Post-Inj. Litigation Based Clinic Based Unselected Samples < 90 days 0.52 No studies 0.63 > 90 days 0.78 0.74 0.04 Vietnam Experience Study (VES) Neuropsychological and Postconcussive Symptom Findings Subjects Vietnam Experience Study Data/Center for Disease Control Vietnam Experience Study 1988a, 1988b JAMA 4,462 randomly selected male US Army vets (community dwelling, not clinic-referred or selfreferred) Entered military between 1/65 - 12/71 Minimum of 4 months active duty Served only one tour of duty Subjects cont’d Racial makeup of the 4,462 participants: 81.9% Caucasian 11.8% African-American 4.5% Hispanic 1.9% Other Mean age = 38.36 years (SD = 2.53) Mean level of education = 13.29 years (SD = 2.3) Mean IQ = 105 (SD = 20.32) (based on GTT) Subjects cont’d Participants underwent a 3 day evaluation including: extensive medical, psychological, and neuropsychological examination included were questions regarding MVA, head injury, loss of consciousness, and subsequent hospitalization Evaluations took place approximately 16 years post-military discharge Measures Diagnostic Interview Schedule (DIS-III-A) Extensive surveys of physical functioning and symptoms Battery of neuropsychological tests Groups and Sample Sizes Groups Number No MVA, No Head Injury 3057 MVA, No Head Injury 521 Head Injury with LOC 254 Neuropsychological Measures Multivariate analysis of variance (MANOVA) was conducted with 14 neuropsychological measures, which cover the domains of: » Complex Attention » Non-Verbal Abilities » Psychomotor Speed (visuospatial) » Verbal Memory » Visual Memory & Coordination » Verbal Abilities » Executive Abilities Statistical Analyses: Neuropsychological Measures (Matching groups on premorbid IQ) MANOVA was not significant F(30,7620) = 1.28, p = 0.14, eta squared = 0.005 On average, the MTBI group performed 0.03 of a standard deviation more poorly than either control group Current Cognitive Functioning: Examples of the 14 Measures Normal Control MVA Control Mild TBI (n = 3057) (n = 521) (n = 254) Animal Fluency 20.5 (5.1) 21.0 (5.4) 20.7 (5.3) Rey-O Copy 32.7 (3.4) 32.8 (3.0) 32.7 (3.0) CVLT Sum of Trials 1 to 5 46.0 (8.7) 45.9 (8.5) 46.3 (9.7) Postconcussion Symptoms Postconcussion Symptoms Physical Headache, dizziness, fatigue, noise/light intolerance, insomnia Cognitive Memory complaints, poor concentration Emotional Depression, anxiety, irritability, mood lability PCS Diagnostic Criteria DSM-IV Three or more of: 1. Fatigue 2. Disordered Sleep 3. Headache 4. Dizziness 5. Irritability 6. Anxiety, depression, or affective lability ICD-10 Three or more of: 1. Headache, dizziness, malaise, fatigue, or noise intolerance 2. Irritability, depression, anxiety, or emotional lability 3. Subjective concentration, memory, or intellectual difficulties 4. Insomnia or affective lability Odds-Ratios for Occurrence of the Postconcussion Symptom Complex over Past Year (Controlling for Demographics, Medical, & Prior Psychiatric Symptoms) Diagnosis Normal Control MVA Control Mild TBI DSM-IV Postconcussion Syndrome 1.0 (20.6%) 1.04 (0.82 - 1.31) 2.00 (1.49 - 2.69) (25.2%) (40.9%) ICD-10 Postconcussion Syndrome 1.0 (19.1%) 1.13 (0.90 - 1.44) 1.80 (1.33 - 2.43) (24.9%) (37.4%) Odds-Ratios for Various Physical/Neurological Postconcussion Symptoms During the Past Year (Controlling for Demographics, Medical, & Prior Psychiatric Symptoms) Symptom Normal Control MVA Control Mild TBI Balance Problems 1.0 (3.4%) 1.58 (1.02 – 2.45) 2.43 (1.48 – 3.97) Sensitivity to Light 1.0 (3.6%) 1.14 (0.72 – 1.80) 1.92 (1.15 – 3.20) Headache Problems 1.0 (13.0%) 1.15 (0.89 – 1.50) 1.94 (1.42 – 2.68) Trouble Sleeping 1.0 (24.9%) 1.22 (1.01 – 1.51) 1.85 (1.39 – 2.45) Double Vision 1.0 (5.7%) Fatigue Easily 1.0 (20.9%) 1.00 (0.80 – 1.26) 1.42 (1.05 – 1.91) 1.10 (0.75 – 1.61) 1.81 (1.17 – 2.79) Odds-Ratios for Various Cognitive/Neuropsychological Postconcussion Symptoms During the Past Year (Controlling for Demographics, Medical, & Prior Psychiatric Symptoms) Symptom Normal Control MVA Control Mild TBI Periods of Memory Loss or Confusion 1.0 (4.4%) 1.14 (0.76 – 1.72) 2.80 (1.83 – 4.28) Memory Problems 1.0 (13.7%) 1.13 (0.87 – 1.46) 1.75 (1.28 – 2.41) Concentration Problems 1.0 (13.4%) 1.40 (1.10 – 1.80) 1.28 (0.91 – 1.80) Odds-Ratios for Various Emotional/Psychological Postconcussion Symptoms During the Past Year (Controlling for Demographics, Medical, & Prior Psychiatric Symptoms) Symptom Normal Control MVA Control Mild TBI Irritability or Short Temper 1.0 (26.5%) 1.10 (0.89 – 1.35) 1.36 (1.02 – 1.81) Aggressive and Angry Behavior 1.0 (10.2%) 1.34 (1.02 – 1.77) 1.32 (0.91 – 1.91) Sadness and Depression 1.0 (11.2%) 1.28 (0.97 – 1.69) 0.92 (0.62 – 1.37) Anxious 1.0 (13.8%) 1.29 (0.99 – 1.65) 1.10 (0.77 – 1.56) Causes of Persistent Postconcussion Symptoms “Expectation as Etiology” and/or “The Good Old Days” Symptom Mis-Attribution Willey Mittenberg, Ph.D. “Diagnostic Threat” Julie Suhr, Ph.D. Expectation as Etiology Controls asked to imagine symptoms of a mild TBI “expect” symptom presence and severity very similar to mild TBI patients’ actual symptoms Mild TBI patients “under-estimate” the frequency and severity of pre-MTBI symptoms and problems Athletes “expect” lower levels of postconcussion problems than non-athletes Athletes with a concussion “over-estimate” pre-concussion levels of symptoms Mild TBI “Diagnostic Threat” Non-clinical evaluations of college students with a remote history of mild TBI (many months earlier) Neuropsychological Test Performance If told they are participating in a study of the effects of mild TBI, their performance is worse than, If told they are simply participating in a study of cognitive functioning in college students The “context” of the evaluation matters! Other Factors Influencing the Development and Persistence of Persistent Postconcussion Symptoms Predictors of Persistent PCS: Vietnam Experience Study Data Examine the influence of the following predictors on the presence of a persistent Postconcussion Symptom Complex (PPCS) following mild head injury Predictors: demographic variables early life psychiatric difficulties social support variables loss of consciousness Results Overall model was significant MTBI R2 = 33.0 2 (26, N = 532) = 137.85, p < .001 Unique Variance per predictor MTBI demographic variables early life psychiatric symptoms (9.2%) (6.3%) • Internalizing (e.g., depression/anxiety) (4.9%) • Externalizing (ASP, alcohol, drugs) MTBI social support LOC / MVA 2-way Interactions 3-way Interactions (0.9%) (4.9%) (1.4%) (5.4%) (0.1%) Contribution of Demographic Variables in MTBI MTBI Overall Demogr. Variance 9.2% unique variance Variable Age at evaluation Level of education Race Intelligence MTBI 0.9% 0.2% 0.3% 3.3% MTBI: Intelligence by LOC (1.8%) Frequency of PPCS by Level of Premorbid Intelligence and LOC Frequency of PPCSC 70 60 LOC 50 No LOC 40 30 20 10 GTT < 96 GTT 96 - 114 GTT > 114 MTBI: Intelligence by Social Support (1.2%) Frequency of PPCS by Level of Premorbid Intelligence and Level of Social Support Frequency of PPCSC 80 70 GTT < 96 60 GTT 96 - 114 GTT > 114 50 40 30 20 10 0 Poor Social Support Average Social Support Good Social Support MTBI: Internalizing by Social Support (1.0%) Frequency of PPCS by History of Premorbid Internalizing problems and Level of Social Support Frequency of PPCSC 80 70 60 50 Internalizing Problems 40 No Internalizing Problems 30 20 10 Poor Social Support Average Social Support Good Social Support PCS Conclusions LOC is only a small factor in predicting the presence of PPCS (1.4% unique variance) in MHI Multiple factors and their interactions accounted for approximately 33% of the variance in PPCS status in the sample with MHI PCS Conclusions Within a MTBI sample: Lower pre-injury intellectual ability, Less poor social support, and More early life emotional problems (e.g., depression, anxiety) were associated with higher frequencies of Persistent PCS Loss of consciousness (MTBI) interacts with cognitive reserve in influencing the development or persistence of PCS Treatment of Mild TBI Mild TBI Treatment Change expectation and attribution of symptoms Provide education Education regarding mild TBI Education regarding symptoms and their course Provide Support/Treatment Stress management Psychological and cognitive coping strategies and resources Cognitive-Behavioral therapy References Belanger, H. G., Curtiss, G., Demery, J. A., Lebowitz, B. K., & Vanderploeg, R. D. (2005). Factors moderating neuropsychological outcomes following mild traumatic brain injury: A Meta-analysis. Journal of the International Neuropsychological Society, 11, 215-227. Belanger, H.G., & Vanderploeg, R.D. (2005). The Neuropsychological Impact of Sports-Related Concussion: A Meta-Analysis. Journal of the International Neuropsychological Society, 11, 345-357. Luis, C. A., Vanderploeg, R. D., Curtiss, G. (2003). Predictors for a postconcussion symptom complex in community dwelling male veterans. Journal of the International Neuropsychology Society, 9, 1001-1015. Miller, L.J. & Mittenberg, W. (1998). Brief cognitive behavioral interventions in mild traumatic brain injury. Applied Neuropsychology, 5, 172-183. Mittenberg, W., Tremont, G., Zeilinski, R., Fichera, S., & Rayls, K. (1996). Cognitive behavioral prevention of postconcussion syndrome. Archives of Clinical Neuropsychology, 11, 139-145. Mittenberg, W., Zielinski, R.E., & Fichera, S. (1993). Recovery from mild head injury: A treatment manual for patients. Psychotherapy in Private Practice, 12, 37-52. References Schretlen, D. J., & Shapiro, A. M. (2003). A quantitative review of the effects of traumatic brain injury on cognitive functioning. International Review of Psychiatry, 15, 341-349. Suhr, J.A. & Gunstad, J. (2005). Further exploration of the effect of “diagnosis threat” on cognitive performance in individuals with mild head injury. Journal of the International Neuropsychological Society, 11, 23-29. Vanderploeg, R. D., Curtiss, G., & Belanger, H. G. (2005). Adverse longterm neuropsychological outcomes following mild traumatic brain injury. Journal of the International Neuropsychological Society, 11, 228-236. Vanderploeg, R.D., Belanger, H.G., & Curtiss, G. (2006). Mild Traumatic Brain Injury: Medical and Neuropsychological Causality Modeling. (pp. 279-307). In Young, G., Kane, A. & Nicholson, K. (Eds.), Psychological Knowledge in Court: PTSD, Pain and TBI. New York: Springer-Verlag. Vanderploeg, R.D. (2004). Veterans Health Initiative: Traumatic Brain Injury. (Editor). VA Employee Education System. Web-based physician, psychologist, & other health care professionals CME/CEU training program. http://www1.va.gov/vhi/docs/TBIfinal_www.pdf [1-31-04] Vanderploeg, R. D., Curtiss, G., Luis, C. A., & Salazar, A. M. (in press). Long-term morbidity and quality of life following mild head injury. Journal of Clinical and Experimental Neuropsychology.