* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Vaccine
Monoclonal antibody wikipedia , lookup
Globalization and disease wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Thiomersal controversy wikipedia , lookup
Poliomyelitis eradication wikipedia , lookup
Complement system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Social immunity wikipedia , lookup
Molecular mimicry wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Poliomyelitis wikipedia , lookup
Immune system wikipedia , lookup
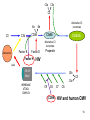
Vaccination policy wikipedia , lookup
Adaptive immune system wikipedia , lookup
Hepatitis B wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Herd immunity wikipedia , lookup
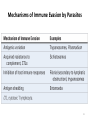
Psychoneuroimmunology wikipedia , lookup
Innate immune system wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
DNA vaccination wikipedia , lookup
Whooping cough wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
HIV vaccine wikipedia , lookup
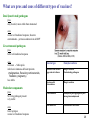
Polio vaccine wikipedia , lookup
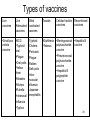
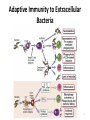
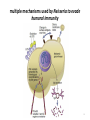
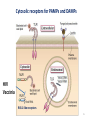
IMMUNE RESPONSES TO MICROBES AND VACCINES DEVELOPMENT Infectious diseases are among the leading causes of death worldwide 2 Innate Immunity to Extracellular Bacteria • Complement activation • Activation of phagocytes and inflammation 3 Adaptive Immunity to Extracellular Bacteria 4 Bacteria Can Evade Host Defense Mechanisms at Several Different Stages 5 multiple mechanisms used by Neisseria to evade humoral immunity 6 IMMUNITY TO INTRACELLULAR BACTERIA 7 8 Mechanisms of Immune Evasion by intercellular Bacteria 9 Innate and adaptive immune responses against viruses 10 Many Viruses Are Neutralized by Antibodies • influenza virus binds to sialic acid residues in cell membrane glycoproteins and glycolipids • rhinovirus binds to inter cellular adhesion molecules (ICAMs) • Epstein-Barr virus (EBV) binds to type 2 complement receptors on B cells. So antibodies may block viral penetration Fc-receptore –mediated phagocytosis complement-activating antibody lysis or C3b-receptore mediated phagocytosis 11 Cell-Mediated Immunity Is Important for Viral Control and Clearance • Antibodies can not eliminate established infection!!! • NOW, cell-mediated immune mechanisms are most important in host defense. • CD8+ TC cells and CD4 TH1 cells • cytokines, including IL-2, IFN-γ, and tumor necrosis factor- α (TNF-α) 12 Viruses Employ Several Different Strategies to Evade Host Defense Mechanisms • Hepatitis C virus (HCV) • human immunodeficiency Virus (HIV) • Herpes simple virus (HSV) • Polio virus 13 14 Cytosolic receptors for PAMPs and DAMPs HIV Vaccinia RIG-1-like receptors 15 C3a C3b C3 Ba C3 C3b Alternative C5 convertase Bb C3bB C3bBb C3bBb3b Alternative C3 convertase Factor B Bacterium Factor D Factor H Properdin HIV Lysis C5-C9 MAC C5b C5a MEMBRANE ATTACK COMPLEX C9 C8 (CD59) C7 C5 C6 HIV and human CMV 16 • An anti-inflammatory cytokine. • An inhibitor of and . • Negative feedback regulator. • Inhibits production of . and ultimately • Inhibits the expression of on MQs and DCs. and Epstein-Barr virus (EBV) produce IL-10 like cytokine 17 Innate and Adaptive Immunity to Fungi • The principal mediators of innate immunity against fungi are neutrophils and macrophages. – TLRs and lectin-like receptors (dectins) • Dendritic cells activated via this lectin receptor produce TH17-inducing cytokines, such as IL-6 and IL-23. – The Th17 cells stimulate inflammation, and the recruited neutrophils and monocytes destroy the fungi • Cell-mediated immunity is the major mechanism of adaptive immunity against fungal infections. – CD4+ and CD8+ T cells cooperate to eliminate the yeast 18 Mechanisms of Immune Evasion by fungal • Virulent strains of Cryptococcus neoformans inhibit the production of cytokines such as TNF and IL-12 by macrophages and stimulate production of IL-10, thus inhibiting macrophage activation. 19 Immune Responses to Disease-Causing Parasites 20 Mechanisms of Immune Evasion by Parasites 21 STRATEGIES FOR VACCINE DEVELOPMENT 22 What are different types of immunization? Passive Immunization -- direct transfer of protective antibodies -- no immunological memory Active Immunization -- activation of immune response -- immunological memory 23 Active Vaccination: What are some important considerations in the design of vaccines? Characteristics of pathogen & disease Intra- vs extra-cellular short or long incubation acute or chronic disease Antigenic stability route of infection Characteristics of vaccine efficacy appropriate response booster safety stability, cost 24 Why are boosters needed? 25 How effective are vaccines? Vaccine “efficacy” incidence among those administered and Is 100% efficacy necessary? -- “herd immunity” incidence among those not administered -- e.g., 60% efficacy -- depends upon population, age, etc Example efficacies Diphtheria: 87%-96% Tetanus: >90% Oral polio: 90%-100% Mumps/Measles/Rubella: 90%-95% HIV vaccine trials 150 vaccines developed 6 have made it to efficacy testing 2009: 1st with efficacy (31%) [2007 had negative efficacy] Diphtheria Hib (<5 yrs old) Measles Mumps Pertussis Polio (paralytic) Rubella Smallpox Tetanus Cases per Year before in (average) 2003 175,885 1 20,000 (est.) 259 503,282 56 152,209 231 147,271 11,647 16,316 0 47,745 7 48,164 0 1,314 20 Decrease in Cases per Year 99.9% 98.8% 99.9% 99.9% 92.1% 100.0% 99.9% 100.0% 98.5% Sources CDC. Impact of vaccines universally recommended for children — United States, 1900-1998. MMWR 8(12):243-8 CDC. Notice to Readers: Final 2003 Reports of Notifiable Diseases. MMWR 2004;53(30):687 Malaria vaccine trial 2011: 45 – 56% 26 How are vaccines made? Dead (inactivated) pathogens IPV – Inactivated polio vaccine – ‘Salk’ vaccine [old pertussis of DPT -- Bordetella pertussis] Live attenuated pathogens MMR – measles, mumps, rubella viruses OVP -- oral polio vaccine – ‘Sabin’ vaccine Subunit / Peptide components Cell cultured virus HBsAG -- Hepititis B surface antigen Flu – purified HA & NA antigens Conjugates (polysaccharides coupled to protein carrier) HiB – Haemophilus influenzae type B PCV – pneumococcal conjugate vaccine Toxoids DTaP -- diphtheria, tetanus toxoids [ + “acellular pertussis” molecular component] Remember Adjuvants? -- increase immune response e.g., aluminum hydroxide 27 What are pros and cons of different types of vaccines? Dead (inactivated) pathogens pros may be safer; more stable than attenuated cons weaker cell mediated response; boosters contaminants – pertussis endotoxin in old DPT Live attenuated pathogens pros better cell-mediated response cons reversion -- Sabin polio infection in immuno-deficient patients (malignancies, Receiving corticosteroids, Radiation, pregnancy) less stable Vaccine type Example reactions Vaccines from Chicken eggs and cell cultures Allergic reactions Contaminating pathogens Vaccines with Preservatives Allergic reactions Live attenuated Susceptibility during preganncy and among immunodepressed Dead whole cell Contamination with toxins Molecular components pros No living pathogen present very stable cons fewer epitopes weaker cell mediated response 28 Types of vaccines Live vaccines Live Killed Attenuated Inactivated vaccines vaccines Toxoids Cellular fraction vaccines Recombinant vaccines •Small pox variola vaccine •BCG •Typhoid oral •Plague •Oral polio •Yellow fever •Measles •Mumps •Rubella •Intranasal Influenza •Typhus •Diphtheria •Tetanus •Meningococcal polysaccharide vaccine •Pneumococcal polysaccharide vaccine •Hepatitis B polypeptide vaccine •Hepatitis B vaccine •Typhoid •Cholera •Pertussis •Plague •Rabies •Salk polio •Intramuscular influenza •Japanise encephalitis 29 New Vaccination Strategies DNA vaccines DNA for an AG injected -- expressed in cells Pros Both arms respond DNA is very stable No pathogen involved Cons Still experimental Limited epitopes 30 The mechanism of action of DNA vaccines 31 New Vaccination Strategies Recombinant vectors e.g., HIV genes in an Adenovirus vector Pors •Easily manufactured and often relatively stable •Cannot “revert” to recreate pathogen Cons • Poorly immunogenic • Post-translational modifications • Poor CTL response 32 برنامه واکسیناسیون جدید در ایران (اجرا از آبان )93 برنامه واكسن بدو تولد ب ث ژ ،هپاتيت ب ،فلج اطفال خوراكي ۴ ،۲و ۶ماهگي پنج گانه (سه گانه +هپاتيت ب +هموفيلوس انفلوانزای ، )Bفلج اطفال خوراكي ،فلج اطفال تزریقی ۱۲ماهگي MMR ۱۸ماهگي يادآور اول سه گانه ،يادآور فلج اطفال خوراكي MMR ، ۶سالگي 33 يادآور دوم سه گانه ،يادآور فلج اطفال خوراكي