* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download PYOGENIC COCCI
Survey
Document related concepts
Transmission (medicine) wikipedia , lookup
Germ theory of disease wikipedia , lookup
Gastroenteritis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Urinary tract infection wikipedia , lookup
Schistosomiasis wikipedia , lookup
Human microbiota wikipedia , lookup
Anaerobic infection wikipedia , lookup
Triclocarban wikipedia , lookup
Infection control wikipedia , lookup
Neonatal infection wikipedia , lookup
Neisseria meningitidis wikipedia , lookup
Transcript
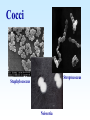
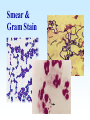
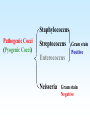
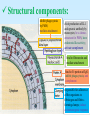
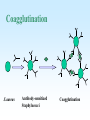
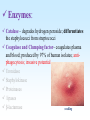
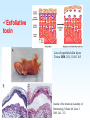
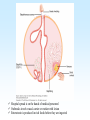
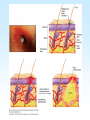
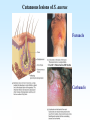
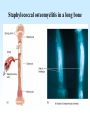
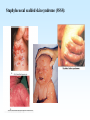
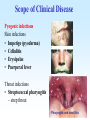
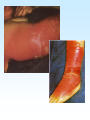
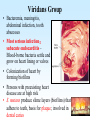
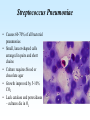
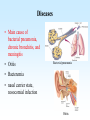
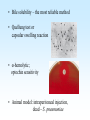
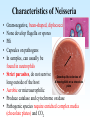
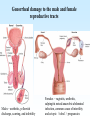
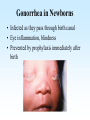
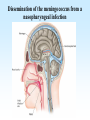
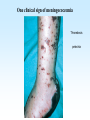
PYOGENIC COCCI Staphylococcus, Streptococcus, Neisseria Junqi Zhang (张俊琪), PhD MOH&MOE Key Lab of Medical Molecular Virology Shanghai Medical College, Fudan University (复旦大学上海医学院分子病毒学教育部/卫生部重点实验室) Cocci Streptococcus Staphylococcus Neisseria Smear & Gram Stain Staphylococcus Pathogenic Cocci (Pyogenic Cocci) Streptococcus Enterococcus Neisseria Gram stain Positive Gram stain Negative Staphylococcus >40 species Staph=grape-like clusters coccus=round Scanning Electron Microscope General Characteristics of the Staphylococci Include a major human pathogen and skin commensals Spherical cells arranged in irregular clusters Gram-positive Coagulase: an important indicator of pathogenic staphylococci Lack spores and flagella May have capsules Gram staining Classification I: isolate character on blood agar plate S.aureus S.epidermidis S. saprophyticus Classification II: coagulase coagulase positive staphylococcus S. aureus coagulase negative staphylococcus, CNS S. epidermidis S. saprophyticus Coagulase: an important indicator of pathogenic staphylococcus S. aureus Morphology, culture, and biological characteristics Pathogenesis: virulent factors, diseases Diagnostic laboratory tests Principles of controlling staphylococcal infections Culture Characteristics - S. aureus Facultative anaerobe Grows in large, round, opaque, golden yellow colonies; βhemolysis on blood agar plate Optimum temperature of 37oC Tolerate high salt: 10%-15% NaCl, high temperatures: 60oC 1h; 80oC 30min Withstands extremes in pH Drug resistance: MRSA Virulence factors of S. aureus Structural components Enzymes Toxins Structural components: inhibit phagocytosis by PMN; mediate attachment elicit production of IL-1 and opsonic antibody by monocytes; be a chemoattractant for PMN; have endotoxin-like activity; activate complement bind to fibronectin and mediate attachment bind to Fc portion of IgG; inhibit phagocytosis; anti complement responsible for adherence of the organisms to fibrinogen and fibrin – forming clumps; induce an immunogenic response Staphylococcus Protein A (SPA) PHAGOCYTE Fc receptor SPA IgG BACTERIUM antibody opsonization Binds to Fc portion of IgG(IgG1,2,4); Inhibits phagocytosis; Anti complement Coagglutination S.aureus Antibody-sensitized Staphylococci Coagglutination Enzymes: Catalase – degrades hydrogen peroxide; differentiates the staphylococci from streptococci Coagulase and Clumping factor– coagulates plasma and blood; produced by 97% of human isolates; antiphagocytosis; invasive potential Uronidase Staphylokinase Proteinases lipases β-lactamase swelling Coagulase and Clumping factor responsible for adherence of the organisms to fibrinogen and fibrin – forming clumps; induce an immunogenic response(vaccine efforts) Clumping factor + Clumping factor - ★ Toxins: (5) Hemolysins (α, β, γ, δ)– lyse red blood cells Leukocidin (PVL) – lyses neutrophils and macrophages Exfoliative toxin – separates the epidermis from the dermis Enterotoxin– 9 serotypes, induce gastrointestinal distress, heat stable protein Toxic shock syndrome toxin (TSST) – induces fever, vomiting, shock, systemic organ damage superantigens Enterotoxin, Exfoliative toxin, TSST-1 genes are on a pathogenicity island Exfoliative toxin Loss of superficial skin layers Toxins 2010, 2(5), 1148-1165 Journal of the American Academy of Dermatology Volume 48, Issue 2 2003 244 - 252 Superantigen Exotoxins Bind directly to MHC II Cytokines are released from large proportion of T cells Virulence factors of S. aureus Biological activities Enzymes Coagulase Hyaluronidase Staphylokinase DNase Lipases Penicillinase Catalase Toxins Hemolysins (α, β, γ, δ) Leukocidin Enterotoxin Exfoliative toxin Toxic shock syndrome toxin (TSST) coagulates plasma and blood; alter ingestion and destruction by phagocytic cells; an important indicator of invasive pathogenic staphylococcus digests connective tissue digests blood clots digests DNA digest oils; enhances colonization on skin inactivates penicillin degrades hydrogen peroxide lyse red blood cells lyses neutrophils and macrophages induces gastrointestinal distress separates the epidermis from the dermis induces fever, vomiting, shock, systemic organ damage Structural components Capsule/polysaccharide Peptidoglycan Teichoid acid SPA Clumping factor (bound coagulase) inhibits phagocytosis by PMN; mediate attachment elicits production of IL-1 and opsonic antibody by monocytes; be a chemo-attractant for PMN; has endotoxin-like activity; activates complement binds to fibronectin and mediates attachment binds to Fc portion of IgG; inhibits phagocytosis; anti complement responsible for adherence of the organisms to fibrinogen and fibrin forming clumps; induces an immunogenic response Staphylococcal Disease • Pyogenic infections: Range from localized to systemic • Toxigenic disease: -Food intoxication -Staphylococcal scalded skin syndrome (SSSS) -Toxic shock syndrome (TSS) Hospital spread is on the hands of medical personnel Outbreaks involve nasal carrier or worker with lesion Enterotoxin is produced in rich foods before they are ingested Pyogenic infections: Range from localized to systemic Localized cutaneous infections – invade skin through wounds, follicles, or glands – Folliculitis (毛囊炎)– superficial inflammation of hair follicle; usually resolved with no complications but can progress – Furuncle (疖)– boil; inflammation of hair follicle or sebaceous gland progresses into abscess or pustule – Carbuncle (痈)– larger and deeper lesion created by aggregation and interconnection of a cluster of furuncles – Impetigo (脓胞)– bubble-like swellings that can break and peel away; most common in newborns Cutaneous lesions of S. aureus Furuncle Carbuncle Systemic infections Bacteremia – primary origin is bacteria from another infected site or medical devices; endocarditis possible Osteomyelitis – infection is established in the metaphysis; abscess forms Staphylococcal osteomyelitis in a long bone Toxigenic disease: Food intoxication: ingestion of heat stable enterotoxins; gastrointestinal distress Staphylococcal scalded skin syndrome (SSSS): toxin induces bright red flush, blisters, then desquamation of the epidermis; infants, adults with hypoimmunity Toxic shock syndrome (TSS) :toxemia leading to shock and organ failure; fever, hypotension, diarrhea, erythroderma (rash) Staphylococcal scalded skin syndrome (SSSS): Following controversial test marketing in Rochester, New York and Fort Wayne, Indiana, in August 1978, Procter and Gamble introduced superabsorbent Rely tampons to the United States market in response to women's demands for tampons that could contain an entire menstrual flow without leaking or replacement. 1. Rely used carboxymethylcellulose (CMC) and compressed beads of polyester for absorption. 2. This tampon design could absorb nearly 20 times its own weight in fluid. 3. Further, the tampon would "blossom" into a cup shape in the vagina to hold menstrual fluids without leakage. Coagulase Negative Staphylococcus • CNS - Normal flora • 35 spp. ~ 15 potential human pathogens – Staphylococcus saprophyticus • Common cause of UTI in young women • Treated as outpatients – Staphylococcus epidermidis • UTI, uncommon • Bacterial endocarditis • Biofilms – implanted medical devices related infections Generally hospital acquired – Distiguished by novobiocin in the lab BACTERIAL BIOFILMS Identification of Staphylococcus in Samples The identification of organisms is based on cellular, cultural, and biochemical characteristics • Specimens: pus, tissue exudates, sputum, urine, spinal fluid, blood, etc. • Smears: Gram staining-positive, cocci in clusters; can't distinguish saprophytic from pathogenic organisms • Cultivation -On nutrient agar they tend to be white (or cream colored), circular, entire, convex colonies. -On Sheep Blood Agar Staphylococcus aureus may exhibit hemolysis of the agar in the area around the colonies. Colonies of S. aureus (medium sized, smooth and glossy, raised, opaque, inaurate liposolubility pigment) Colonies of S. aureus with zone of hemolysis on a blood agar plate White colonies of S. epidermidis on a blood agar plate • Chemical and Biochemical Tests Tests to be performed: 1. Catalase test 2. Coagulase test 3. Growth and fermentation on Mannitol Salt Agar 4. Susceptibility to the antibiotic “Novobiocin” Staphylococcus genus S. aureus S. epidermidis S. saprophyticus Catalase Catalase + 2 H2O2 2 H2O + O2 (g) Characteristics S. aureus S. epidermidis S. saprophyticus pigment of colony Golden yellow White White coagulase SPA + + + + + + + - - novobiocin Sensitive Sensitive Resistant pathogenesis suppuration, abscess, septicemia endocarditis, bacteremia, UTI UTI mannitol glucose heat-stable nuclease α-toxin 1. Catalase Test • The Catalase test determines if the organism produces the enzyme “Catalase”, which breaks down hydrogen peroxide (H2O2) to water and oxygen (O2). Catalase 2 H2 O2 2 H2O + O2 (g) _ + A drop of 3% hydrogen peroxide solution is placed on a slide, and a small amount of the bacterial growth is placed in the solution. Bubbling indicates a positive test for the presence of the catalase enzyme. 2. Coagulase Test + Staphylococcus aureus _ Coagulase + Coagulase – Citrated rabbit (or human) plasma diluted 1:5 is mixed with an equal volume of broth culture or growth from colonies on agar and incubated at 37oC. If clots form in 1-4 hours, the test is positive. Agglutination of the “Test” latex with no agglutination of the “Control” latex is considered a positive (+) test for the presence of this enzyme. All reactions occurring after 20 seconds should be ignored. 3. Mannitol Salt Agar • • • • Two different characteristics of the organism are determined with this agar. The first is the organism’s ability to tolerate a high salt environment. Evidence of growth on the slant indicates the organism can grow in a high salt environment. Organisms that can ferment the sugar Mannitol produce an acid end-product that changes the red pH indicator (Phenol red) in the media to yellow. red at neutral pH (~ 7.0) yellow under acidic conditions Any yellow in the media is considered a positive test for Mannitol fermentation. It is possible to have growth, but no Mannitol fermentation. 4. Novobiocin Susceptibility • • A zone of growth inhibition 16 mm or less in diameter indicates resistance (R) to Novobiocin. If the zone is greater than 16 mm the organism is susceptible (S) to Novobiocin. • Molecular typing Polymerase chain reaction (PCR) Pulsed-field gel electrophoresis (PFGE) Multilocus sequence typing ELISA - toxins Epidemiology Present in most environments frequented by humans Readily isolated from fomites High carriage rate: healthy adults – 20~50%; medical staff – ~70% Carriage is mostly in anterior nares, skin, nasopharynx, intestine Predisposition to infection include: poor hygiene and nutrition, tissue injury, preexisting primary infection, diabetes, immunodeficiency Clinical Concerns 95% have penicillinase and are resistant to penicillin and ampicillin Nosocomial infections Increase in community acquired methicillin resistance -MRSA (methicillin-resistant S. aureus) -Carry multiple resistance -Some strains have resistance to all major drug groups except vancomycin Treatment of Staphylococcal Infections Timely cleanliness, hygiene, and aseptic management of lesions Abscesses have to be surgically perforated Prescription of appropriate antibiotics: Perform antimicrobial susceptibility tests to help in the choice of drugs Systemic infections require intensive lengthy therapy Prevention of Staphylococcal Infections • Prevent nosocomial infections Proper hygiene, segregation of carrier from highly susceptible individuals Precautions and frequent surveillances: areas at highest risk; high risk patients Protection of health care workers Good aseptic techniques when handling surgical instruments • Hygiene and cleansing Streptococci Morphology, culture, and biological characteristics Pathogenesis: virulent factors, diseases Diagnostic laboratory tests Principles of controlling staphylococcal infections Classification of Streptococci I. II. III. IV. V. Colony morphology and hemolytic reaction on blood agar Lancefield classification system Biochemical reactions & resistance to physical and chemical factors Ecologic features Molecular genetics I. Classification based on colony morphology hemolysis reaction on blood agar In 1903 J.H. Brown grouped streptococcus by their ability to lyse RBCs -hemolysis: complete disruption of erythrocytes with clearing of the blood around the bacterial growth pathogens A, B, C, G and some D strains -hemolysis: incomplete lysis of erythrocytes with reduction of hemoglobin and the formation of green pigment S. pneumoniae and others collectively called viridans conditional pathogens -hemolysis: no effect on RBCs, nonhemolytic streptococcus Hemolysis patterns on blood agar II. Lancefield classification system Capsule Proteins (M protein) Carbohydrates Cell wall (C carbohydrate) Peptidoglycan Cell membrane Cytoplasma II. Lancefield classification system In 1927 Rebecca Lancefield originated the “Lancefield groups” of Streptococci that we still use now: Based on surface antigens: C-carbohydrate 17 groups (A-H, K-U) each group has one or more species Group A, B and D - most important; Group A: ~90% human pathogenic Streptococci Group C, G, F - rare Lancefield later determined that Streptococcus viridans & pneumococci did NOT possess antigens that reacted with her antisera. Summarize of classification system hemolysis reaction Streptococci 1 2 A M protein B Streptococci C-carbohydrate C … V groups 3 … 100 types Human Streptococcal Pathogens S. pyogenes S. agalactiae Enterococcus faecalis Viridans streptococci S. pneumoniae -hemolytic S. pyogenes The most important member of Group A Most serious streptococcal pathogen Strict parasite Inhabits throat, nasopharynx, occasionally skin Virulence Factors of -Hemolytic S. pyogenes – Structural components hinders complement and neutrophil response major, contributes to resistance to phagocytosis protect against lysozyme; classifications provokes no immune response adherence **group A streptococcus, Streptococcus pyogenes Capsule-anti phagocyte Adherence factors M protein-adherence, anti phagocyte (Surface molecules) LTA-adherence Virulence Factors Streptokinase Invasive enzymes Hyaluronidase Streptodornase Toxins *Streptolysins (SLO,SLS) Erythrogenic toxin (pyrogenic exotoxin) Superantigens Virulence Factors of b-Hemolytic S. Pyogenes Extracellular enzymes Help bacteria be easier to spread • Streptokinase – digests fibrin clots • Hyaluronidase – breaks down connective tissue • Streptodornase – depolymerizes DNA, decrease viscosity of purulent exudates Virulence Factors of -Hemolytic S. pyogenes Extracellular toxins: Streptolysins – hemolysins; streptolysin O (SLO) and streptolysin S (SLS) – both cause cell and tissue injury Erythrogenic toxin (pyrogenic exotoxin) – induces fever and typical red rash, superantigen Superantigens – strong monocyte and lymphocyte stimulants; cause the release of tissue necrotic factor Epidemiology and Pathogenesis Source of infection: patients and carriers Transmission – contact, droplets, food, vomits Portal of entry generally skin or pharynx Children predominant group affected for cutaneous and throat infections Systemic infections and progressive sequelae possible if untreated Scope of Clinical Disease Pyogenic infections Skin infections • Impetigo (pyoderma) • Cellulitis • Erysipelas • Puerperal fever Throat infections • Streptococcal pharyngitis – strep throat Pharyngitis and tonsillitis 61 Scope of Clinical Disease Systemic infections • Scarlet fever(猩红热) – strain of S. pyogenes carrying a prophage that codes for erythrogenic toxin; can lead to sequelae • Septicemia • Pneumonia • Streptococcal toxic shock syndrome (链球菌毒素休克综合征) Long-Term Complications of Streptococcus Group A Infections • Rheumatic fever – follows overt or subclinical pharyngitis in children; carditis with extensive valve damage possible, arthritis, chorea, fever • Acute glomerulonephritis – nephritis, increased blood pressure, occasionally heart failure; can become chronic leading to kidney failure -Hemolytic Streptococci: Viridans Group • Large complex group – Streptococcus mutans, S. oralis, S. salivarus, S. sanguis, S. milleri, S. mitis • Most numerous and widespread residents of the gums and teeth, oral cavity, and also found in nasopharynx, genital tract, skin • Not very invasive; dental or surgical procedures facilitate entrance Viridans Group • Bacteremia, meningitis, abdominal infection, tooth abscesses • Most serious infection: subacute endocarditis – Blood-borne bacteria settle and grow on heart lining or valves • Colonization of heart by forming biofilms • Persons with preexisting heart disease are at high risk • S. mutans produce slime layers (biofilms) that adhere to teeth, basis for plaque; involved in dental caries 66 Group B: Streptococcus Agalactiae 无乳链球菌 Regularly resides in human vagina, pharynx, and large intestine Can be transferred to infant during delivery and cause severe infection Most prevalent cause of neonatal pneumonia, sepsis, and meningitis Pregnant women should be screened and treated Wound and skin infections and endocarditis in debilitated people Group D Streps and Enterococci • Group D: - Streptococcus bovis, S. equinus • Enterococci: - Enterococcus faecalis, E. faecium, E. durans, etc. – Normal colonists of human large intestine – Cause opportunistic urinary, wound, and skin infections Identification • Specimens: a throat swab, pus, blood, etc. • Smears: Gram staining-positive, often show single cocci or pairs rather than chains • Cultivation – hemolysis • Rapid diagnostic tests based on monoclonal antibodies that react with C-carbohydrates ASO test – Serologic test • When the body is infected with streptococci, it produces antibodies against the various antigens that the streptococci produce. • Anti-streptolysin O (ASO) is the antibody produced against an antigen produced by group A streptococci. • A rise in the titer of ASO can be estimated by this test. >400 unit Treatment and Prevention • Groups A and B are treated with penicillin G. • Long-term penicillin prophylaxis for people with a history of rheumatic fever or recurrent strep throat • Enterococcal treatment usually requires combined therapy Streptococcus Pneumoniae • Causes 60-70% of all bacterial pneumonias • Small, lancet-shaped cells arranged in pairs and short chains • Culture requires blood or chocolate agar • Growth improved by 5-10% CO2 • Lack catalase and peroxidases – cultures die in O2 Virulence factors • Capsule: 90 different capsular types major virulence factor, anti-phagocytosis, Smooth(S)/Rough(R) • Pneumolysin O: hemolysis • LTA: attachment • Neuraminidase: digest N-Acetylneuraminic Acid colonization, proliferation, spreading Diseases • Main cause of bacterial pneumonia, chronic bronchitis, and meningitis • Otitis Bacterial pneumonia • Bacteremia • nasal carrier state, nosocomial infection Otitis Cultivation and Diagnosis • Gram stain of specimen – presumptive identification Gram + Capsule + Diplococcus • Bile solubility – the most reliable method • Quellung test or capsular swelling reaction • α-hemolytic; optochin sensitivity • Animal model: intraperitoneal injection, dead – S. pneumoniae Treatment and Prevention • Traditionally treated with penicillin G or V Increased drug resistance; Vancomycin • Two vaccines available for high risk individuals: – Capsular antigen vaccine for older adults and other high risk individuals – effective 5 years – Conjugate vaccine for children 2 to 23 months The Neisseria • Gram-negative cocci • Residents of mucous membranes of warmblooded animals • 2 primary human pathogens: – Neisseria gonorrhoeae (Gonococci) – Neisseria meningitidis (Meningococci) Characteristics of Neisseria Pili • • • • • • • • • Gram-negative, bean-shaped, diplococci None develop flagella or spores Pili Capsules on pathogens In samples, can usually be found in neutrophils Strict parasites, do not survive Dewdrop-like colonies of N.meningitidis on a chocolate long outside of the host plate Aerobic or microaerophilic Produce catalase and cytochrome oxidase Pathogenic species require enriched complex media (chocolate plates) and CO2 Neisseria gonorrhoeae:The Gonococcus Virulence factors: 1. Pili (Fimbriae), other surface molecules (Rmp, Por, Opa) for attachment; slows phagocytosis 2. Lipooligosaccharide (LOS): endotoxic effects; molecular mimicry of human glycosphingolipid, evade immune recognition 3. IgA1 protease: cleaves secretory IgA, attachment Causes gonorrhea, in top 5 STDs Gonorrheal damage to the male and female reproductive tracts Males – urethritis, yellowish discharge, scarring, and infertility Females – vaginitis, urethritis, salpingitis mixed anaerobic abdominal infection, common cause of intertility and ectopic (tubal )pregnancies Gonorrhea in Newborns • Infected as they pass through birth canal • Eye inflammation, blindness • Prevented by prophylaxis immediately after birth Neisseria Meningitidis: The Meningococcus • >13 serogroups; serotypes A, B, C, X, Y and W-135 cause most cases • Virulence factors: – – – – Capsule Adhesive pili (fimbriae) IgA protease Lipooligosaccharide (LOS): endotoxic effects Epidemiology and Pathogenesis • Prevalent cause of meningitis; sporadic or epidemic • Human reservoir – nasopharynx; 5-30% of adult population may harbor meningococci; 70% carrier rate during epidemics • High risk individuals are those living in close quarters, children 6 months-3 years • Disease begins when bacteria enter bloodstream, cross the blood-brain barrier, permeate the meninges, and grow in the cerebrospinal fluid • Very rapid onset; neurological symptoms; endotoxin causes hemorrhage and shock; can be fatal Dissemination of the meningococcus from a nasopharyngeal infection One clinical sign of meningococcemia Thrombosis petechia Immunity, Vaccination and treatment • humoral immunity: IgG, IgM, IgA • Vaccines: against capsular polysaccharides types: A, C ; A, C,Y, W-135 • Treatment: penicillin G, cephalosporin Key points • The virulence factors of staphylococcus and streptococcus • Diseases caused by staphylococcus and streptococcus • Differences between pathogenic and nonpathogenic staphylococcus • Classification of streptococci Questions 1. Chapter 13: 2,3,4,5,6,7,10,11 2. Chapter 14: 1,2,3,4,5,6,7,9,10 3. Chapter 20: 1,4,6,7,9 4. How to distinguish pathogenic staphylococcus species from non-pathogenic ones ? 5. Describe the main virulence factors of staph, strep and Neisseriae genus. 6. Please definition SPA. 7. “Strep” vs. “staph”, how do they differ?