* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Skin and Soft-Tissue Infections - Hatzalah of Miami-Dade
Survey
Document related concepts
Traveler's diarrhea wikipedia , lookup
Globalization and disease wikipedia , lookup
Onchocerciasis wikipedia , lookup
Urinary tract infection wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Schistosomiasis wikipedia , lookup
Antibiotics wikipedia , lookup
Sarcocystis wikipedia , lookup
Neonatal infection wikipedia , lookup
Infection control wikipedia , lookup
Staphylococcus aureus wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Transcript
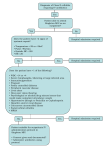
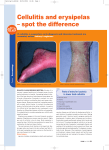
Skin and Soft-Tissue Infections Superficial lesions vs Deadly disease Outpatient Management and Indications for Hospitalization Nayef El-Daher, MD, PhD Richard Magnussen, MD J Crit Illness, 1998; 13(3):151-160 3/98 medslides.com 1 Skin and soft-tissue Infections • Localized infections – cellulitis – erysipelas • Potentially lethal infections – necrotizing fascitis – myonecrosis – pyomyositis 3/98 medslides.com 2 Cellulitis and Erysipelas pathogenesis • Cellulitis – group A streptococci typically follows an innocuous or unrecognized injury; inflammation is diffuse, spreading along tissue planes – staphylococcus aureus usually associated with wound or penetrating trauma; localized abscess become surrounded by cellulitis 3/98 medslides.com 3 Cellulitis and Erysipelas pathogenesis • Erysipelas – caused most often by group A streptococci – rarely cased by ß-hemolytic streptococci of the B, C, or G serologic group 3/98 medslides.com 4 Cellulitis and Erysipelas diagnosis • General features – varying degrees of skin or soft-tissue erythema, warmth, edema, and pain – associated fever and leukocytosis – history of trauma, abrasion, or skin ulceration (not reported by every patient) 3/98 medslides.com 5 Cellulitis and Erysipelas diagnosis • physical exam – cellulitis has an ill-defined border that merge smoothly with adjacent skin; usually pinkish to redish – erysipelas has an elevated and sharply demarcated border with a fiery-red appearance 3/98 medslides.com 6 Cellulitis and Erysipelas diagnosis • laboratory exam – needle aspiration of the leading edge of the cellulitis should be obtained (1) – elevated antistrptolysin O titer supports diagnosis of streptococcal infection – blood cultures for patients with symptoms of toxicity or temp > 1020F 3/98 1. Arch Intern Med 1990; 150:1907-1912 medslides.com 7 Cellulitis and Erysipelas management • Local care – immobilization – elevation to reduce swelling • 2 weeks of antibiotic therapy – penicillin and dicloxacillin for most pts – many new, potent and expensive antibiotics offer no advantage 3/98 medslides.com 8 Outpatient Therapy Infection Cellulitis mild-mod severe Erysipelas mild-mod severe 3/98 Most patients Pencillin allergic patients Dicloxacillin (500 mg po q6h) Nafcillin 1-2g iv q4h Vancomycin 1g iv q12h Cephalexin 500mg po q6h Clindamycin 450mg po q6h Cefazolin 1g iv q8h Penicillin V (500 mg po q6h) Cephalexin 500mg po q6h Erythromycin 500mg po q6h Clindamycin 450mg po q6h Cefazolin 1g iv q8h Clindamycin 900mg iv q8h Pen G 1-2 million U q6h medslides.com 9 Admission Criteria for Cellulitis • Animal bite on patient’s face or hand • Area of skin involvement >50% of limb or torso, or >10% of body surface • Coexisting morbidity (diabetes, heart failure, renal failure, generalized edema) • Edge of cellulitis advancing at rate exceeding 5cm, or 2 in, per hour • History of saphenous venectomy, pelvic surgery, pelvic irradiation, or neoplastic pelvic lymph nodes (with lower extremity cellulitis) 3/98 medslides.com 10 Admission Criteria for Cellulitis • • • • • • • • 3/98 Immunosuppression Intolerance of oral or IM antibiotic therapy Lack of response after 72 hours of oral therapy Noncompliance with medication and follow-up visits Purpuric or petechial rash, numbness at skin surface, or impaired tendon or nerve function shock or disseminated intravascular coagulation Signs and symptoms suggestive of bacteremia Total WBC < 1000 / uL medslides.com 11 Necrotizing Fasciitis pathogenesis • a polymicrobial infection, commonly caused by a mixture of anaerobic and aerobic bacteria – clostridium species, enterobacteriaceae ( E. coli, Enterobacter, Klebsiella, and Proteus species), and “flesh-eating” streptococci • usually starts at the site of nonpenetrating trauma (a bruise) 3/98 medslides.com 12 Necrotizing Fasciitis diagnostic clues • Underlying diabetes mellitus, peripheral vascular disease, alcoholism, intravenous drug use or immunosupression • Most often involve the lower extremities • Infected area is swollen, erythematous, painful, warm, and very tender • Rapidly advancing border (5 cm, or 2 in, per hour) of discoloration (red to blue-gray) 3/98 medslides.com 13 Necrotizing Fasciitis diagnostic clues • Bulllae formation and cutaneous gangren • Frank pus in discolored area (revealed by needle aspiration or surgical exploration) • Numerous bacteria evident on the Gram stain • Tendon or nerve impairment (superficial nerve destruction and small vessel thrombosis) • Systemic toxicity and/or hypotension 3/98 medslides.com 14 Necrotizing Fasciitis management • Immediate surgical debridement is critical and life saving • empiric antibiotics to cover anaerobes, gram negative bacilli, streptococci, and Staph aureus – pen+metronidazole+clindamycin+ceftriaxone – vancomycin+chloramphenicol – monotherapy with imipenem • antibiotics for a minimum of 3 wks 3/98 medslides.com 15 Myonecrosis (Gas Gangrene) • • • • a pure Clostridium perfringens infection gas in a gangrenous muscle group incubation period of hours to days local edema and pain accompanied by fever and tachycardia • discharge is serosanguinous, dirty, and foul • pen G (3-4 million U q4h) or chloramphenicol • surgical removal of infected muscle 3/98 medslides.com 16 Pyomyositis (tropical myositis) • 50% with co-morbidity (diabetes, alcoholic liver disease, concurrent corticosteroid therapy, immunosuppression) • endemic in the tropics • area is indurated with a “woody” consistency; erythema and tenderness is minimal initially • fever and marked muscle tenderness may develop in 1-3 weeks 3/98 medslides.com 17 Pyomyositis (tropical myositis) • Rhabdomyolysis - along with myoglobinuria and acute renal failure - may develop • Staph aureus is the most common organism • MRI or CT may show muscle enlargement • surgical drainage is essential • empiric antibiotics directed against Staph – nafcillin 2 g iv q4h – vancomycin 1 g iv q12h or cefazolin 1g iv q8h 3/98 medslides.com 18