* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download File
Survey
Document related concepts
Lesbian sexual practices wikipedia , lookup
Female promiscuity wikipedia , lookup
Body odour and sexual attraction wikipedia , lookup
Human female sexuality wikipedia , lookup
Embryo transfer wikipedia , lookup
Human sexual response cycle wikipedia , lookup
Prenatal development wikipedia , lookup
Mammary gland wikipedia , lookup
Fertilisation wikipedia , lookup
Hormonal breast enhancement wikipedia , lookup
Sexual reproduction wikipedia , lookup
Reproductive health wikipedia , lookup
Sexual attraction wikipedia , lookup
Female ejaculation wikipedia , lookup
Transcript
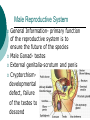
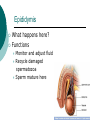
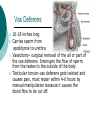
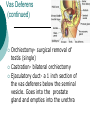
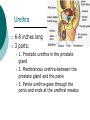
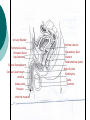
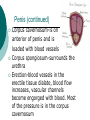
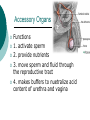
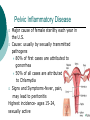
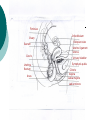
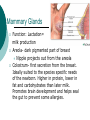
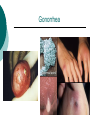
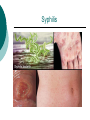
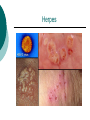
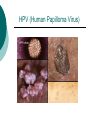
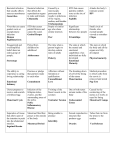
Reproductive System Male Reproductive System General Information- primary function of the reproductive system is to ensure the future of the species Male Gonad- testes External genitalia-scrotum and penis Cryptorchismdevelopmental defect, failure of the testes to descend Testes Testis—singular Each located in a separate compartment Normal sperm production requires a temperature about 2o lower than the rest of the body Function-produce spermatozoan ½ billion spermatozoa are produced a day Spermatozoan Spermatozoa (pl) Parts of spermatozoan: Head, neck, middle piece,tail (flagellum) Epididymis What happens here? Functions Monitor and adjust fluid Recycle damaged spermatozoa Sperm mature here Vas Deferens 16-18 inches long Carries sperm from epididymis to urethra Vasectomy- surgical removal of the all or part of the vas deferens. Interrupts the flow of sperm from the testes to the outside of the body Testicular torsion-vas deferens gets twisted and causes pain, must repair within 4-6 hours by manual manipulation because it causes the blood flow to be cut off. Vas Deferens (continued) Orchiectomy- surgical removal of testis (single) Castration- bilateral orchiectomy Ejaculatory duct- a 1 inch section of the vas deferens below the seminal vesicle. Goes into the prostate gland and empties into the urethra Urethra 6-8 inches long 3 parts: 1. Prostatic urethra in the prostate gland 2. Membranous urethra-between the prostate gland and the penis 3. Penile urethra-goes through the penis and ends at the urethral meatus Urinary Bladder Symphysis pubis Prostate Gland Vas Deferens Corpus Spongiosum Corpus Cavernosum Urethra Glans penis Prepuce Urethral meatus Seminal Vesicle Ejaculatory Duct Rectum Bulbourethral gland Bulb of penis Epididymis Testis Scrotum Penis (continued) Corpus cavernosum-is on anterior of penis and is loaded with blood vessels Corpus spongiosum-surrounds the urethra Erection-blood vessels in the erectile tissue dialate, blood flow increases, vascular channels become engorged with blood. Most of the pressure is in the corpus cavernosum Accessory Organs Functions 1. activate sperm 2. provide nutrients 3. move sperm and fluid through the reproductive tract 4. makes buffers to nuetralize acid content of urethra and vagina Accessory Organs Seminal Vesicles Tubular glands Makes up to 60% of the semen Secretions are high in fructose which is used by the sperm to make them become mobile Accessory Glands Prostate glands- 1 ¼ inch in diameter Makes 30% of semen volume Prostatitis- inflammation of the prostate gland, common in men >50, can cause BPH (benign prostatic hypertrophy). Treatment: medication, TURP (transurethral prostatectomy) which is a partial removal of the prostate. Prostate Cancer- most common cancer in men Higher incidence in African Americans, lower in Asians Treatment: radiation and/or prostatectomy Side effect of surgery: loss of sexual functioning and urinary incontinence Accessory Gland At ejaculation 2-5 ml of semen is released Semen Contains: Spermatozoa (20-100 million) Seminal fluid (liquid part of the semen) Enzymes to help dissolve the mucus in the vagina and to act as an antibiotic (to protect the sperm) Male Sexual Functioning Arousal- erotic thoughts or stimulation of genital area leads to increase in parasympathetic nervous system functioning which leads to erection (tumescence) Intercourse = coitus = copulation Peristaltic contractions push fluid and spermatozoa into prostatic urethra. The seminal vesicles contract, prostate gland contracts which moves seminal fluid into the membranous and penile urethra. Sympathetic stimulation closes the sphincter at the entrance of the urinary bladder which keeps semen out of the bladder and urine out of semen Male Sexual Functioning Ejaculation- powerful contraction of the pelvic floor muscles create a pleasurable sensation with ejaculation Male orgasm Heart rate and blood pressure increase with ejaculation Impotence= male sexual dysfunction the inability to achieve or maintain an erection. Common problem. Causes: low BP in arteries serving the penis, drugs, alcohol, trauma, illness,depression Hormones FSH- follicle stimulating hormone ICSH- interstitial cell stimulating hormone (same as LH in female) Testosterone functions: 1. Promotes maturation of sperm 2. Maintains accessory organs of male repro. system 3. Secondary sex characteristics 4. Stimulate metabolic operations ( protein synthesis and muscle growth 5. Influences brain development especially sexual behavior and sex drive Testosterone production increases at puberty Female Reproductive System Female gonad = ovary Function of ovary Produces ova and sex hormones 2x1 inches, almond shape Produce one ovum per month Fallopian Tubes Alternate names: Uterine tubes Oviducts Fimbriae-the end close to the ovary, with finger like projections Takes 3-4 days for the egg to go through the tube to the uterus Fertilization must occur within 12-24 hrs of ovulation Where does fertilization occur? In the outer 1/3 of fallopian tube Uterus Functions- provides protection and nutritional support for the developing embryo Cervix= neck of the uterus, juts into vagina, opening=external os Uterus (continued) 2 Layers Endometrium- inner lining of uterine wall. Shed each month with menstruation. Provides a rich environment for implantation of fertilized ovum Myometrium- muscular layer of uterus. Bands of overlapping muscle Uterus - Disease/Disorders Uterine fibroids- common tumors of muscle and connective tissue. Usually benign 40% of women >50 uterine fibroids Hysterectomy performed if fibroids are large or pressing on structures Endometrial Cancer-estrogen therapy increases risk of endometrial cancer 2-10 times. The addition of progesterone decreases the risk Vagina Description-muscular tube, 3-3 1/2 inches long, contains rugae (folds of tissue) so it can get longer and wider for intercourse and childbirth Functions Passageway for menstrual fluids Receives penis during coitus Birth canal Vagina Diseases/Disorders Vaginitis- inflammation of vaginal canal. (variety of causes) Cervical Cancer-most common reproductive cancer in women ages 15-34 Primary risk: multiple sex partners, humanpapilloma virus Pap smear- tests for cancerous and precancerous cells Pelvic Inflammatory Disease Major cause of female sterility each year in the U.S. Cause: usually by sexually transmitted pathogens 80% of first cases are attributed to gonorrhea 50% of all cases are attributed to Chlamydia Signs and Symptoms-fever, pain, may lead to peritonitis Highest incidence- ages 15-24, sexually active Fimbriae Ovary Sacrum Infundibulum Fallopian tube Uterine ligament Uterus Cervix Urethra Rectum Anus Urinary bladder Symphysis pubis Clitoris Vagina Labia majora Labia minora Female External Genitalia Vulva Region includes: Labia majora Labia minora Mons pubis Clitoris (erectile tissue-has a prepuce) Vaginal opening Mammary Glands Function: Lactation= milk production Areola- dark pigmented part of breast Nipple projects out from the areola Colostrum- first secretion from the breast. Ideally suited to the species specific needs of the newborn. Higher in protein, lower in fat and carbohydrates than later milk. Promotes brain development and helps seal the gut to prevent some allergies. Mammary Glands Disease/ Disorders Breast Cancer-Most common after age 50- can occur in both men and women Risk factors Family history Never pregnant or pregnant for the first time after age 20 Early menarche (1st menstruation) Late menopause High fat diet No breastfeeding Mammary Gland Disease /Disorder Diagnosis: Mammography uses x-rays to examine the breast for tumors. Also breast self-exam Treatment: surgery plus chemotherapy and/or radiation. Mastectomy- surgical removal of the breast 1. Segmental mastectomy/ lumpectomy- tumor and surrounding tissue removes, but most of breast remains 2. Total mastectomy- entire breast removes, but other tissue left intact 3. Radical mastectomy-breast, pectoralis muscle and auxiliary lymph nodes removed 4. Modified radical mastectomy-most common surgerybreast and lymph nodes removed, pectoralis muscle remains Sexually Transmitted Diseases Chlamydia- leads to PID and infertility. May be as many as 4 million cases yearly, often no symptoms. Bacterial. Treatment: antibiotic Gonorrhea-most common STD in U.S. 80% of women have no symptoms. Can lead to PID. Bacterial Treatment: antibiotics Gonorrhea Sexually Transmitted Disease Syphilis-Bacterial infection Four stages Once the disease is in the fourth and final stage, the effects are not reversible Congenital syphilis-transferred from the infected mother to the fetus. Infects developing bones and cartilage. Causes progressive damage to spleen, liver, bone marrow and kidneys. Diagnosis: blood test Treatment: penicillin or other antibiotic Syphilis Sexually Transmitted diseases Genital Herpes- painful, ulcerate lesion on external genitalia caused by the herpes virus. Can be internal and painless in women leading to the risk of baby contracting congenital herpes infection during birth. Genital herpes infection increases risk of HIV infection Herpes Sexually Transmitted Diseases Hepatitis B (hepatitis= inflammation of the liver) Often no symptoms Can lead to liver cirrhosis or liver cancer No effective treatment Vaccine can prevent it Sexually Transmitted Diseases Human Papilloma Virus (HPV) – causes genital warts Primary cause of cervical cancer. Can cause vulvar, penile and anal cancers Fairly new vaccine can prevent it HPV (Human Papilloma Virus) Sexually Transmitted Diseases AIDS- acquired immunodeficiency syndrome Caused by HIV (human immunodeficiency virus) Hormones and Female Reproduction Ovarian cycle Oogenesis= ovum production Ovarian Cycle Ovarian Follicle- part of ovary where oogenesis occurs After ovulation , the follicle becomes the corpus luteum(yellow body) which degenerates after about 12 days unless pregnancy occurs At puberty there are about 200,000 primordial follicles that can became active follicles. 40 years after puberty, there are few or no follicles that can become active. Ovarian Cycle Before ovulation: Ovarian Cycle begins with menstration. The developing follicle increases estrogen production. When follicle is mature, estrogen level is high which causes a sharp increase in LH which causes follicle wall to burst open so ovulation can occur Ovarian Cycle Pre-ovulation hormones Estrogen-steroid hormones. Estradiol is the most important Estrogen functions: 1. Stimulate bone and muscle growth 2. Maintain female secondary sex characteristics 3. Affect CNS activity (sex-related behaviors and sex drive) 4. Maintain accessory organs 5. Begin repair and growth of endometrium Ovarian Cycle Post Ovulation Corpus luteum produces progesterone and a small amount of estrogen Progesterone is the primary hormone of the post-ovulatory period Progesterone functions: 1. prepare uterus for pregnancy 2. Stimulate metabolic rate leading to increase in basal body temperature If there is no pregnancy, corpus luteum degenerates which causes estrogen and progesterone levels to fall Menstrual Cycle Av. 28 days – range is 21-35 days Menstrual Cycle Phase 1: Menses Beginning of cycle Unneeded endometrial tissues are sloughed off Lasts 1-7 days About 35ml of blood is lost Menarche- 1st menstrual period (avg. age 12-13) Menopause-cessation of menstrual periods (avg. age 51) Menstrual Cycle Phase 1 continued Dysmenorrheal- painful menstruation (cramps) PMS (premenstrual syndrome) Starts 7-10 days before the start of menses May be caused by changes in sex hormone levels directly or indirectly by CNS effects. However, this is largely a cultural phenomenon in the U.S. Symptoms: fluid retention, breast enlargement, headaches, pelvic pain, bloated feeling, irritability, anxiety, depression Treatment: exercise, diet (no caffeine, increase veggies Menstrual Cycle Phase 2: Proliferative Phase After menses Endometrial epithelium is restored Lasts until ovulation (about 14 days) Phase 3: Secretory Phase Begins with ovulation Lasts as long as corpus luteum (about 14 days) Amenorrhea-no mense (without menstrual flow) Pregnancy Conception Zygote Blastocyst Implantation Placenta hCG—human chorionic gonadotropin Amniotic sac and fluid Pregnancy Blastocyst- a ball of cells that reaches the uterus 5-7 days after conception Inner cell mass becomes the baby Outer cell mass becomes the placenta and amniotic sac and fluid Pregnancy Implantation- blastocyst has cilia which secret a digestive enzyme that digests the endometrium so that the blastocyst burrows in. Usually on the upper rear wall of the uterus. Completion of implantation= establishment of pregnancy Pregnancy Placenta- large organ that develops during pregnancy to provide nourishmaent and oxygen to the baby and remove CO2 and other wastes Placenta grows on the endometrium Mother’s blood supply and baby’s are separate Umbilical cord connects placenta to baby Pregnancy hCG- human chorionic gonadotropin- hormone of pregnancy Pregnancy tests detect presence of hCG in urine or blood Pregnancy Amniotic sac- surrounds the baby and is filled with amniotic fluid Has 2 layer membrane-outer layer is the chorion, inner layer is the amnion Amniotic fluid created and absorbed by the amnion Totally replaced 8 times daily Baby drinks amniotic fluid and urinates in it Pregnancy Relaxin- hormone from placenta that softens cartilage in the symphysis pubis, softens the cervix and loosens pelvis in preparation for birth Human placental lactogen and prolactin work together to develop mammary glands in preparation for lactation Birth process begins Aging and the Reproductive System Menopause ovulation and menstruation cease decrease in estrogen and progesterone production Uterus and breast size decrease Vaginal and urethral wall get thinner Decrease in estrogen can lead to osteoporosis Male Climacteric Gradual change in male reproductive system Testosterone levels decrease starting between ages 50-60 Gradual reduction in sexual activity