* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download CARDIAC ARRYTHYMIAS
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Heart failure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Myocardial infarction wikipedia , lookup
Jatene procedure wikipedia , lookup
Electrocardiography wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
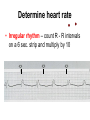
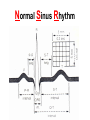
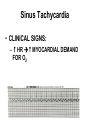
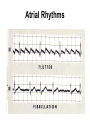
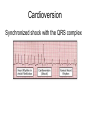
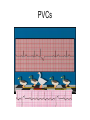
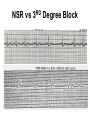
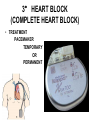
CARDIAC Rhythms Arrhythmias Dysrhythmias Oh, my! NUR240 Lecture 3 JB 9/10 Arrhythmia ARRHYTHMIA – VARIATION IN NORMAL RHYTHM DYSRHYTHMIA – ABNORMAL, DISTURBED RHYTHM RESULTS FROM IMPULSE FORMATION DISTURBANCE OR CONDUCTION DISTURBANCE AXIOM ALL RHYTHM INTERPERTATION MUST BE CORRELATED WITH SIGNS & SYMPTOMS AND PATIENT CONDITION… “TREAT THE PATIENT, NOT THE MONITOR” Dysrhythmia Impulse formation (site of impulse origin) SA Node Ectopic AV Node Premature Beat Ventricle Dysrhythmia Altered conduction • Bradycardia / Tachycardia • Flutter / Fibrillation • Heart blocks Basic Rhythm Strip Interpretation 1. Determine the rate. Does the atrial rate equal the ventricular rate. 2. Is the rhythm regular/irregular? 3. Find the P wave. Is there a P wave for every QRS? 4. Determine the PRI (Normal 0.12-0.20 sec) 5. Find the QRS (Normal <0.12seconds) 6. Any ectopic beats? 7. Find the T wave. http:www.rnceus.com EKG strip identification and evaluation Determine heart rate REGULAR RHYTHM – count boxes between 2 “R” waves and divide into 300 5 300 / 5 = 60 1 small box = .04 second 1 large box = .20 second 15 large boxes = 3 seconds 30 large boxes = 6 seconds 300 large boxes = 1 minute 1 mm = 0.1 millivolt (mV) Determine heart rate • Irregular rhythm – count R - R intervals on a 6 sec. strip and multiply by 10 Normal Sinus Rhythm • NORMAL SINUS RHYTHM IS PRODUCED BY THE SA NODE – P – WAVE FOLLOWS QRS COMPLEX IN A PREDICTABLE RELATIONSHIP – ALL “P” WAVES LOOK ALIKE, ALL QRS COMPLEXES ARE NARROW – R – R INTERVAL IS REGULAR – RATE: 60 – 100 bpm Normal Sinus Rhythm Normal Sinus Rhythm Sinus / Atrial dysrhythmia • ORIGINATE FROM SA NODE OR ATRIA (ABOVE VENTRICLES) • CONDUCTION WITH VENTRICLE IS UNDISTURBED • USUALLY BENIGN & SYMPTOMATIC • RHYTHM MAY BE IRREGULAR Sinus / Atrial dysrhythmias – SINUS TACHYCARDIA – SINUS BRADYCARDIA – ATRIAL FIBRILLATION – ATRIAL FLUTTER – Premature atrial contractions – Paroxysmal atrial tachycardia – Supraventricular Tachycardia Sinus Tachycardia • VENTRICULAR RATE 100 bpm ETIOLOGY: – MAY REFLECT PHYSIOLOGIC DEMAND FOR O2 – SYMPATHOMIMETIC DRUGS – FEVER – PAIN Sinus Tachycardia • CLINICAL SIGNS: – HR MYOCARDIAL DEMAND FOR O2 Treatment – MAY RESOLVE WITH TREATMENT OF UNDERLYING CAUSE – DRUGS WITH RATE SLOWING EFFECT: DIGOXIN, β-BLOCKERS – CAROTID MASSAGE – VAGAL MANEUVER Sinus Bradycardia • VENTRICULAR RATE = 60 ETIOLOGY: RESPONSE TO MYOCARDIAL ISCHEMIA VAGAL STIMULATION ELECTROLYTE IMBALANCE DRUGS I.C.P. HIGHLY TRAINED ATHLETE CLINICAL SIGNS • C.O. IF BODY CAN’T COMPENSATE OR IMPROVED C.O. DUE TO DIASTOLIC FILLING TIME MAY LEAD TO ARRHYTHMIA • TREATMENT – DEPENDS ON CAUSE: – ATROPINE – AVOID VALSALVA – HOLD RATE SLOWING DRUGS I.E.: DIGOXIN, blockers Atrial Flutter • ATRIAL RATE = 250 – 400 IMPULSES/ MINUTE – ETIOLOGY: • OCCURS /W HEART DISEASE • CAD • VALVE DISORDERS – CLINICAL SIGNS • • • • “SAW TOOTH” P-WAVES, CALLED F-WAVES ATRIAL RATE = 250 – 400/ MIN AV NODE BLOCKS SOME IMPULSES INCOMPLETE EMPTYING OF ATRIA CAUSE RISK FOR THROMBUS GIVE ANTICOAGULANTS Atrial Flutter • TREATMENT – TREAT UNDERLYING CAUSE – IRRITABILITY, RAPID VENTRICULAR RESPONSE – DIGOXIN SLOWS RATE BY ENHANCING AV BLOCK – QUINIDINE SUPRESSES ATRIAL ECTOPIC BEATS – AMIODARONE – CALCIUM CHANNEL & β-BLOCKERS – CONSIDER CARDIOVERSION Atrial Fibrillation • CHAOTIC ELECTRICAL ACTIVITY IN ATRIA • ATRIA QUIVER (>500 beats/minute) INSTEAD OF CONTRACTING AS A UNIT • ETIOLOGY: ADVANCED AGE VALVE DISORDERS CARDIOMYOPATHY Atrial Fibrillation “F” FIBRILLATORY WAVES ø P-WAVES, ø P-R INTERVAL QRS normal VENTRICULAR RATE IS IRREGULAR RAPID VENTRICULAR RESPONSE PULSE DEFICIT Atrial Fibrillation TREATMENT 1. Amiodarone-may cause liver, lung damage and worsening of arrhythmias. Pt to report SOB, wheezing, jaundice, palpitations, lightheadedness 2. Pronestyl, Ca channel blockers, beta blockers, digoxin 3. Synchronized cardioversion if unstable 4. Radio frequency catheter ablation 5. Anticoagulation therapy Atrial Rhythms Synchronized Electrical Cardioversion Oh O2 Saturation Monitoring Say Suction Equipment It IV Line Isn’t Intubation equipment So Sedation and possibly analgesics Cardioversion Synchronized shock with the QRS complex JUNCTIONAL DYSRHYTHMIAS • IMPULSE BEGINS IN AV NODE • VENTRICULAR RATE IS EXTREMELY SLOW • MONITOR FOR SYMPTOMS OF REDUCED CARDIAC OUTPUT AND HEMODYNAMIC INSTABILITY Paroxysmal Supraventricular Tachycardia • ABRUPT ONSET OF HR • ETIOLOGY: SNS STIMULATION CARDIOMYOPATHY • CLINICAL SIGNS: ABRUPT ONSET/ CESSATION S/S ARE RELATED TO C.O. RATE = 150 – 250 bpm PSVT • TREAT UNDERLYING CAUSE – DRUGS: ADENOSINE, β-BLOCKERS, DIGOXIN, MS, QUINIDINE – CAROTID / VAGAL MANEUVERS – SYNCHRONIZED CARDIOVERSION IF UNSTABLE Ventricular Arrhythmias • ORIGINATES IN VENTRICLES • PATIENT MAY BE SYMPTOMATIC, REQUIRES IMMEDIATE ATTENTION – PVC, couplet, bigeminy, trigeminy – V-TACH (ventricular tachycardia) – V-Fib (Ventricular fibrillation) PREMATURE VENTRICULAR CONTRACTION (PVC) – EARLY IRREGULAR VENTRICULAR BEATS – QRS IS WIDE /BIZZARE – CAN BE CHRONIC ASYMPTOMATIC ABNORMALITY OR WARNING OF SERIOUS DYSRHYTHMIA PREMATURE VENTRICULAR CONTRACTION (PVC) • ETIOLOGY: HYPOXIA DIGOXIN TOXICITY MECHANICAL STIMULATION ELECTROLYTE (K) IMBALANCE MI PVCs PREMATURE VENTRICULAR CONTRACTION (PVC) • CLINICAL SIGNS: – DEPEND ON FREQUENCY – PVC SHORT DIASTOLIC FILLING TIME C.O. – FREQUENT PVC – SENSATION OF PALPATIONS, SKIPPED BEATS – BIGEMINY – PVC EVERY OTHER BEAT – TRIGEMINY – PVC EVERY 3RD BEAT PREMATURE VENTRICULAR CONTRACTION (PVC) • TREATMENT: – TREAT IMPAIRED HEMODYNAMICS – ANTIARRHYTHMICS – OXYGEN – MONITOR FOR PVC LANDING ON T-WAVE – OBSERVE FOR UNIFOCAL (VS) MULTIFOCAL Ventricular Arrhythmias • VENTRICULAR TACHYCARDIA – 3 OR MORE PVC’s – QRS IS WIDE/ BIZARRE EXTREMELY SERIOUS MAY LEAD TO LETHAL RHYTHMS • ETIOLOGY: SAME CAUSES AS PVC, ALSO CARDIOMYOPATHY, MYOCARDIAL IRRITABILITY Ventricular Tachycardia Treatment – VT /W PULSE - CARDIOVERT – MONITOR MORE CLOSELY – PREPARE FOR CARDIOVERSION (O2, LIDOCAINE, TREAT CAUSE) – VT W/O PULSE - DEFIBRILLATE VENTRICULAR FIBRILLATION TOTAL UNORGANIZED MULTIFOCAL RHYTHM, VENTRICLES QUIVER, NO CARDIAC OUTPUT V-fib • ETIOLOGY: SAME AS VT, PVC SURGICAL MANIPULATION OF HEART FAILED CARDIOVERSION • CLINICAL SIGNS: SAME AS CARDIAC ARREST EKG SHOWS DISORGANIZED RHYTHM V-fib • TREATMENT IMMEDIATE DEFIBRILLATION X3 CPR SURVIVAL IS < 10% FOR EVERY MINUTE THE PATIENT REMAINS IN V-fib SCREAM for Vfib and Pulseless VTach 1.Shock360J* monophasic, 1st and subsequent shocks.(Shock every 2 minutes if indicated) 2.CPR After shock, immediately begin chest compressions followed by respirations (30:2 ratio) for 2 minutes. 3.Rhythm check after 2 minutes of CPR (and after every 2 minutes of CPR thereafter) and shock again if indicated. Check pulse only if an organized or non-shockable rhythm is present. SCREAM CARDIAC ARREST • VENTRICULAR ASYSTOLE 80 – 90% DUE TO V-fib TOTAL ABSENCE OF ELECTRICAL AND MECHANICAL ACTIVITY • ETIOLOGY TRAUMA OVERDOSE MI • CLINICAL SIGNS – ASYSTOLE or V-fib – NO DEFINABLE WAVE FORMS – ABSENCE OF VITAL SIGNS Ventricular Asystole Acronym Comments T Transcutaneous Pacemaker Only effective with early implementaion E Epinephrine 1 mg IV q3-5 min A Atropine 1 mg IV q3-5 min PEA- Pulseless Electrical Activity • • • • • • Asystole Algorithm PEA Problem search Epinephrine – 1mg IV/IO q3-5min Atropine- with a slow HR, I mg IV/IO q3-5min Consider termination of efforts if asystole persists despite appropriate interventions. CARDIAC ARREST Review ACLS Guidelines 2005 TREATMENT: IMMEDIATE CPR A. AIRWAY/ ADVANCED AIRWAY CONTROL B. BREATHING/ POSITIVE PRESSURE VENTILATION C. CIRCULATION/ CPR, START IV D. DEFIBRILLATE (V-fib, V-tach ONLY) E. DRUGS-Antidysrhythmic tx CARDIAC ARREST • • • • • • EPINEPHRINE 1:10,000 IV PUSH REPEAT Q 5 MIN. AMIODORONE: ATROPINE: VASOPRESSIN: CONSIDER ANTIARRHYTHMICS USE ACLS ALGORITHMS CARDIAC ARREST • TREATMENT: POST CARDIAC ARREST MONITOR CARDIAC STATUS RESPIRATORY STATUS TREAT UNDERLYING CAUSE EMOTIONAL SUPPORT SAFE ENVIRONMENT DEFBRILLATION (vs) CARDIOVERSION • DEFIBRILLATION ASYNCHRONOUS ELECTRICAL DISCHARGE THAT CAUSES DEPOLARIZATION OF ALL MYOCARDIAL CELLS AT ONCE. THIS ALLOWS (HOPEFULLY) THE SA NODE TO RESTORE ITS PACEMAKER FUNCTION AND DICTATE A REGULAR SINUS RHYTHM. USED FOR PULSELESS V-tach AND V-fib VOLTAGE: 200 – 360 joules (“stacked shock”) or AED CARDIOVERSION (aka) SYNCHRONIZED CONVERSION ELECTRICAL IMPULSE IS DISCHARGED DURING QRS (VENTRICULAR DEPOLARIZATION) USUALLY TIMED /W CARDIAC MONITOR TO PREVENT SHOCK ON T-WAVE USED FOR RAPID A-fib, V-tach /W PULSE AND PERSISTENT PAT / PSVT VOLTAGE: 50 – 100 joules EQUIPMENT REVIEW • DEFIBRILLATOR SELECT ENERGY LEVEL, THEN CHARGE • PADDLES USE 25 POUNDS OF PRESSURE WHEN APPLIED TO CHEST, Placed 2nd RICS and 5th LAAS • CONDUCTING AGENT GEL OR PAD WHICH ESTABLISHES SKIN CONTACT, REDUCES SKIN BURNS • JOULES MEASUREMENT OF ELECTRICAL ENERGY • DISCHARGES NO ONE SHOULD COME IN CONTACT WITH PATIENT OR BED DURING DISCHARGE HEART BLOCK • DEPRESSED CONDUCTION OF IMPULSE FROM ATRIA TO VENTRICLES • AV NODE BECOMES DEFECTIVE AND IMPULSES (P-WAVES) ARE BLOCKED FROM BEING TRANSMITTED TO VENTRICLES FIRST DEGREE SECOND DEGREE TYPE I TYPE II THIRD DEGREE 1° HEART BLOCK • PR INTERVAL > 0.20 SECONDS • CAUSES: MAY BE NORMAL VARIANT INFERIOR WALL MI DRUGS: DIGOXIN VERAPAMIL • TREATMENT: MONITOR OBSERVE FOR SYMPTOMS FIRST DEGREE HEART BLOCK 2° HEART BLOCK • ONE OR MORE P-WAVES ARE NOT CONDUCTED THROUGH THE VENTRICLE • HEART RATE - VENTRICULAR RATE SLOW TO NORMAL ATRIAL RATE MAY BE 2 – 4 X’s FASTER THAN VENTRICULAR 2° HEART BLOCK CAUSES: ORGANIC HEART DISEASE MI, Dig toxicity, B and Ca Channel Blockers DIGOXIN TOXICITY SYMPTOMS • Tx: Monitor HR Atropine Temporary pacemaker Avoid meds that decrease conductivity 2 TYPES OF 2° HEART BLOCK MOBITZ TYPE I- Wenkeback MOBITZ TYPE II Second Degree Heart Block Mobitz I • PRI becomes progressively longer until drops QRS Second Degree Heart Block Mobitz Type II • PRI constant and regular, but in a 2:1 , 3:1 pattern 3° HEART BLOCK (COMPLETE HEART BLOCK) • ATRIAL IMPULSES & VENTRICULAR RESPONSE ARE IN TOTAL DISASSOCIATION • P-WAVES ARE SEEN & ARE IRREGULAR • QRS COMPLEX ARE SEEN & ARE IRREGULAR (ESCAPE RHYTHM) • NO CORRELATION BETWEEN P-WAVES & QRS (RATE IS SLOW) – independent rhythms 3° HEART BLOCK (COMPLETE HEART BLOCK) • CAUSES ORGANIC HEART DISEASE MI DRUGS ELECTROLYTE IMBALANCE EXCESS VAGAL TONE • SIGNS & SYMPTOMS EXTREME DIZZINESS HYPOTENSION SYNCOPE S/S OF C.O. ALTERED MENTAL STATUS NSR vs 3RD Degree Block 3° HEART BLOCK (COMPLETE HEART BLOCK) • TREATMENT PACEMAKER TEMPORARY OR PERMANENT PACEMAKER • Indications: Speed up a slow HR or Slow down a rapid HR • ELECTRICAL DEVICE THAT DELIVERS CONTROLLED ELECTRICAL STIMULUS THROUGH ELECTRODES PLACED IN CONTACT WITH HEART MUSCLE • 2 PIECES PULSE GENERATOR IMPLANTED IN CHEST WALL UNDER R CLAVICLE PACEMAKER ELECTRODES IMPLANTED IN MYOCARDIAL TISSUE Paced Rhythm • Pacemaker spike PACEMAKER • TEMPORARY PACEMAKER – USED IN EMERGENCY SITUATION – FIXED (COMPETITIVE) PACEMAKER SENDS STIMULUS TO VENTRICLE AT A FIXED RATE, REGARDLESS OF VENTRICULAR ACTIVITY Types of Pacemakers Use a 5 letter code system, first 3 used more often: 1. Chamber being paced: A, V, D 2. Chamber being sensed: A, V, D, O 3. Type of response by the PM to the sensing: I, T, D, O PATIENT TEACHING • • • • • • • • Carry PM ID card MEDI ALERT BRACELET Avoid swimming, golf and weight lifting AVOID MRI Check PM q3-6 mos. PACEMAKER SURVEILANCE Monitor pulse rates Don’t hold cell phones over generators AUTOMATIC IMPLANTABLE CARDIOVERSION DEFIBRILLATOR (AICD) • PROVIDES INTERNAL SHOCKS WHEN SERIOUS ARRHYTHMIA IS DETECTED (V-tach OR V-fib) • Has a pulse generator and a sensor that monitors the heart • If pt has dysrhythmia it delivers a shock which the pt will feel • USEFUL WHEN ARRHYTHMIA IS UNRESPONSIVE TO MEDS OR SURGICAL ABLATION OR IRRITABLE MYOCARDIAL TISSUE References • http://www.rnceus.com/ekg/ekgsecond2.ht ml • ACLS Guidelines 2005 • www.EMS-ED.net • http://www.doctorshangout.com/forum/topi cs/acls-algorithms-1