* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download The Staphylococci
Monoclonal antibody wikipedia , lookup
Common cold wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Ascending cholangitis wikipedia , lookup
Infection control wikipedia , lookup
Urinary tract infection wikipedia , lookup
Staphylococcus aureus wikipedia , lookup
Neonatal infection wikipedia , lookup
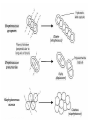
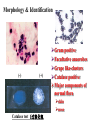
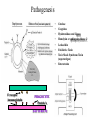
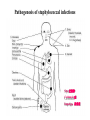
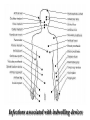
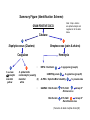
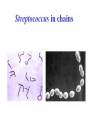
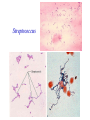
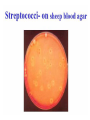
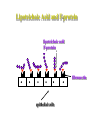
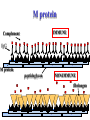
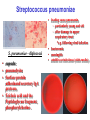
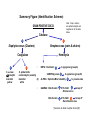
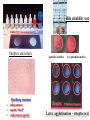
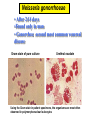
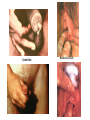
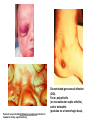
The Staphylococci Morphology & Identification (-) (+) Gram positive Facultative anaerobes Grape like-clusters Catalase positive Major components of normal flora skin nose Catalase test(过氧化氢 Staphylococcus aureus Antigenic Structure Pathogenesis • • • • • • • • Fc receptor immunoglobulin PHAGOCYTE Protein A BACTERIUM Catalase Coagulase Hyaluronidase and Lipase Hemolysin or sphingomyelinase C Leukocidin Exfoliative Toxin Toxic Shock Syndrome Toxin (superantigen) Enterotoxins Pathogenesis of staphylococcal infections Stye:麦粒肿 Carbuncle:痈 Impetigo:脓疱疮 Suppurative • Skin Furuncle; Protein A, Leukocidin, Hemolysin Stye; lipase Impetigo; contagious Epidermal necrolysis Exfoliative Dermatitis (6,7,8); Exfoliative toxin Mastitis Abscess (deep tissue); granulation; coagulase, hyaluronidase (burn, wound) • Systemic Bactermia (from abscess, wound, burn) , Osteomyelitis (tibia) ,Pneumonia • Food poisoning • • • • not a human infection food contaminated from humans – growth – enterotoxin onset and recovery both occur within few hours Vomiting/ nausea/ diarrhea/ abdominal /pain • Toxic shock syndrome • babies – scalded skin syndrome * Exfoliatin • • • • • • fever scarlatiniform rash desquamation vomiting diarrhea myalgias Infections associated with indwelling devices Laboratory • • • 1. 2. 3. • • A. Direct examination; Gram Stain B. Primary media; BAP C. Differential Tests. Mannitol Salts Coagulase DNase D. Phage typing E. Antibiotic Sensitivity (plasmid, B lactamase) : penicillin /methicillin/vancomycin Lysostaphin test Staphylococcus Micrococcus API STAPH Kit Summary Figure (Identification Scheme) Note: Strep. viridans are alpha hemolytic and negative for all the tests below GRAM POSITIVE COCCI Catalase Streptococcus (pairs & chains) + Staphylococcus (Clusters) Coagulase + S. aureus &hemolytic mannitol yellow - Hemolysis • S. epidermidis nonhem olytic (usua lly) mannitol (2) white • BETA: Bacitracin S .pyogenes (group A) + CAMP/Hippurate + S. agalactiae (group B) ALPHA: Optochin/Bile Solubility GAMMA: Bile Es culin + S. pneumoniae + 6.5% NaCl + Group D* Enterococcus Bile Esc ulin NaCl Group D* + 6.5% Non-Enterococcus (*can also be beta or alpha hemolytic) Staphylococcus epidermidis • major component skin flora • opportunistic infections – less common than S.aureus • nosocomial infections – heart valves • Identification – Non-hemolytic (sheep blood agar) – Does not ferment mannitol – Non-pigmented – Coagulase-negative Staphylococcus saprophyticus • urinary tract infections • coagulase-negative – not differentiated from S. epidermidis The Streptococcus Streptococcus Morphology & Identification • • • • facultative anaerobe Gram-positive Chains or pairs Catalase negative (staphylococci are catalase positive) Cell surface structure of S pyogenes and extracellular substances •Lancefield groups *one or more species per group *surface antigens: M, T, R groupable streptococci •A, B and D –most important •C, G, F –Rare Non-groupable •S. pneumoniae –pneumonia •viridans streptococci –e.g. S. mutans *dental caries Lipoteichoic Acid and F-protein lipoteichoic acid F-protein fibronectin epithelial cells M protein • major target – natural immunity • strain variation – antigenicity • re-infection – occurs with different strain M protein IMMUNE Complement IgG r r r M protein NON-IMMUNE peptidoglycan fibrinogen r r r Toxins & Enzymes Hemolysis alpha beta gamma Classofication of Streptococci of Particular Medical Interest Pathogenesis of S pyogenes infections. S. pyogenes (Group A) -suppurative • affect all ages peak incidence at 5-15 years of age • non-invasive – pharyngitis – skin infection, impetigo • invasive bacteremia – toxic shock-like syndrome – "flesh eating" bacteria – pyrogenic toxin • • • Rheumatic fever -etiology Scarlet fever M protein rash – cross-reacts heart myosin – autoimmunity erythrogenic toxin cell wall antigens rheumatic fever – poorly digested in vivo inflammatory disease – persist indefinitely life threatening Post-infectious diagnosis (serology) chronic sequalae • antibodies to streptolysin O fever • important if delayed clinical sequelae Heart occur Joints rheumatic NOT rheumatoid arthritis • superantigen Acute glomerulonephritis • T cell mitogen • activates immune immune complex disease of kidney system Group B streptococcus identification • neonatal meningitis • septicemia • transmission – vaginal flora • hemolysis • hippurate hydrolysis • CAMP reaction – increases hemolysis of S. aureus Group D streptococcus • Growth on bile esculin agar – black precipitate • 6.5% saline • grow – enterococci • no growth – non-enterococci Enterococci • distantly related to other streptococci • genus Enterococcus • gut flora – urinary tract infection • fecal contamination – opportunistic infections • particularly endocarditis • most common E. (S.) faecalis • resistant to many antibiotics – including vancomycin • terminal D-ala replaced by D-lactate Viridans streptococci • • • • • • diverse species oral dental caries hemolytic and negative for other tests non-groupable. includes S. mutans – endocarditis – tooth extraction Streptococcus pneumoniae S. pneumoniae - diplococci • capsule: • pneumolysin: • Surface protein adhesinand secretory IgA protease. • Teichoic acid and the Peptidoglycan fragment, phosphorylchorine . • leading cause pneumonia – particularly young and old – after damage to upper respiratory tract *e.g. following viral infection • bacteremia • meningitis • middle ear infections (otitis media) Summary Figure (Identification Scheme) Note: Strep. viridans are alpha hemolytic and negative for all the tests below GRAM POSITIVE COCCI Catalase Streptococcus (pairs & chains) + Staphylococcus (Clusters) Coagulase + S. aureus &hemolytic mannitol yellow - Hemolysis • S. epidermidis nonhem olytic (usua lly) mannitol (2) white • BETA: Bacitracin S .pyogenes (group A) + CAMP/Hippurate + S. agalactiae (group B) ALPHA: Optochin/Bile Solubility GAMMA: Bile Es culin + S. pneumoniae + 6.5% NaCl + Group D* Enterococcus Bile Esc ulin NaCl Group D* + 6.5% Non-Enterococcus (*can also be beta or alpha hemolytic) Bile solubility test Streptex antiserum optochin sensitive Not optochin sensitive Quellung reaction • • • using antisera capsule "fixed" visible microscopically Latex agglutination - streptococci Prevention and Treatment • Immunity ; 14 capsule types mixed vaccine • Most strains susceptible to penicillin , but resistance is common Neisseria • Gram negative • diplococci (pairs of cocci) • oxidase positive • Culture: 5-10% CO2 • Thayer Martin. – selective – chocolate agar * heated blood N. meningitidis N. gonorrhoeae Virulence Factors Similar, but – Differences in utilization LPS LPS Capsule IgA protease Hemolysin IgA protease PILI Opacity (OPA) proteins Outer Membrane Proteins PILI Opacity (OPA) proteins Outer Membrane Proteins X NO capsule NO hemolysin Neisseria gonorrhoeae • After 2-14 days •Found only in man • Gonorrhea: second most common venereal disease Gram stain of pure culture Urethral exudate Using the Gram stain in patient specimens, the organisms are most often observed in polymorphonuclear leukocytes Neisseria gonorrhoeae Pili = key in anchorage of organisms to mucosal epithelium. Nonpiliated gonococci are avirulent OUTER MEMBRANE PROTEINS Porin proteins (Por) = prevent phagolysosome fusion & allow intracellular survival [ also called protein I] Opacity proteins (Opa) = binding of organisms to epithelium [also called protein II] Reduction-modifiable proteins (Rmp) = protection against bactericidal antibodies [ also called protein III] Urethritis Bartholin’s Duct Disseminated gonococcal infection (DGI). Fever, polyarthritis (or monoarticular septic arthritis), and/or dermatitis (pustules on a hemorrhagic base). Purulent conjunctivitis/Ophthalmia neonatorum Infection in newborns during vaginal delivery Smear • polymorphonuclear cell • Gram negative cocci many in cells • Culture Antibiotic therapy • lactamase-resistant cephalosporin – e.g. ceftriaxone • resistant strains – common – produce lactamases – destroy penicillin N. meningitidis (the "meningococcus") Neisseria meningitidis • resides in man only • usually sporadic cases – mostly young children • outbreaks – adults – crowded conditions * e.g. army barracks Upper respiratory tract infection – adhesion pili Meningococcal meninigitis • 1-4 days • Second most common meningitis – pneumococcus, most common • Fatal if untreated • Responds well to antibiotic therapy – penicillin Bloodstream Brain Prevention Diagnosis • spinal fluid – Gram negative diplococci within polymorphonuclear cells – meningococcal antigens • Culture – Thayer Martin agar • capsule – inhibit phagocytosis • anti-capsular antibodies – stop infection • antigenic variation – serogroups • vaccine – multiple serogroups