* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Clonidine
Survey
Document related concepts
Transcript
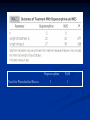
Future Trends in the Treatment of the Neonatal Abstinence Syndrome Walter K. Kraft, MD Associate Professor Director, Clinical Research Unit Thomas Jefferson University Philadelphia, PA Disclosure (past 3 years) Consulting Merck Synageva Speakers Panel None Research Grants Merck, Schering Bristol Myers Squibb Data Safety Monitoring Board Wyeth, RePros Therapeutics Outline Limitations of Current Therapies Potential New Drugs Clonidine Buprenorphine Ongoing Research Future Needs Opioid Neonatal Abstinence Syndrome Newborns of mothers with chronic use Methadone, buprenorphine, morphine, heroin 5% of 56,000 women in US who reported heroin use in previous month were pregnant SAMHSA. 2006 National Survey on Drug Use and Health: National Findings., NSDUH Series H-32, DHHS Publication No. SMA 07-4293). Rockville, MD. 2007 In Australia 40 cases per 10,000 live births US extrapolation—16,000/yr O'Donnell M. Pediatrics. 2009; 123(4):e614-21 Signs and symptoms Neurologic GI Autonomic Why do we treat NAS with medications? Weight gain Ensure development Prevent seizures Patient comfort Pharmacologic Treatment Opiates are preferred therapy Improve weight gain and reduce need for supportive care, but at cost of longer hospital stays Osborn, DA; Opiate treatment for opiate withdrawal in newborn infants. The Cochrane Library 2007 Benzodiazapines helpful only in seizures Phenobarbital useful as adjunct therapy Osborn, DA; Sedatives for opiate withdrawal in newborn infants. The Cochrane Library 2007 Common Drug Treatments Morphine Phenobarbital Tincture of opium Methadone Chloral hyrdate Paregoric What is the problem? At least 50% of infants require pharmacologic treatment We just don’t know which ones Hospital stays are too long Home treatment difficult No generally recognized standard of care Other drug-induced withdrawal symptoms Goals of treatment for NAS shortened hospital stay shortened time of exposure to opiates lowered hospital costs improved parenting maternal-infant bonding lessened maternal guilt Greif J. Subst Abuse Treat. 1993; 10(4):339-34 Clonidine Alpha 2 adrenergic agonist Decreases catecholamine release in the CNS Common uses Hypertension Acute opioid withdrawal Low dose opioids Low dose methadone Rapid detoxification Clonidine Cochrane Review: Adult opioid withdrawal More effective than placebo More side effects compared to tapering methadone Gowing L, Farrell M, Ali R, White JM. Alpha2-adrenergic agonists for the management of opioid withdrawal. Cochrane Database Syst Rev. 2009 Apr 15;(2):CD002024 Side effects Hypotension Rebound hypertension Dry mouth Sedation Clonidine in NAS Year n Hoder, 1984 Case Series 7 Leikin, 2009 Case Series 14 Esmaeili, Case 2010 Series 29 Agthe, 2009 40 RCT Clonidine dose (mcg/kg) 0.5–1.0 po Q 6 13 day LOS hr 0.5–1.0 po Q 6 7 day LOT hr In utero exposures = 3 Iatrogenic NAS = 11 0.5–3.0 hr IV 14 day LOT 32 day LOS Chloryl hydrate rescue 1.0 po Q 4 hr 11 day LOT vs. 15 for (+ morphine) placebo Agthe Morphine dose requirements Square = clonidine Circle = placebo Length of Treatment Agthe: Secondary Endpoints Treatment failures: 5 vs. 0 with clonidine Seizures: 3 vs. 0 with clonidine Deaths: 0 vs. 3 with clonidine (all post discharge) Myocarditis SIDS Homicide (methadone overdose) DSMB ruled these not clonidine related SVT noted 3 days following cessation of clonidine Heart rate and blood pressure changes noted, but none outside of normal ranges Clonidine Optimal use Adjunct to opioid Fixed dose 1.5 mcg/kg q 4 starting week 2? Xie HG. J Clin Pharmacol. 2010 May 19. [Epub ahead of print] Formulation Liquid oral vs. transdermal Buprenorphine Cochrane Review: Management of withdrawal in adults More effective than clonidine Probably quicker in resolution of withdrawal symptoms Longer duration of treatment but higher rates of completion Gowing L, Ali R, White JM. Buprenorphine for the management of opioid withdrawal. Cochrane Database Syst Rev. 2009 Jul 8;(3):CD002025. Safety margin Increasing use in adults Pregnant females Buprenorphine is a partial mu receptor agonist Potential Advantage in NAS Safety Ceiling effect on respiratory depression Fatalities in adults primarily seen with concomitant benzodiazapine abuse Less abuse potential Long half life Improved control of abstinence? Ability to wean out of the hospital? Challenges to use in Neonates No pediatric indication One study in preterm critically ill infants using IV formulation Case reports of maternal use of buprenorphine No good PK data Sublingual administration Metabolic ontogeny Unknown potency of norbuprenorphine Clinical Trial Study Goal Primary Demonstrate sublingual buprenorphine for NAS is safe, tolerable, and feasible Secondary 1) Investigate comparative efficacy for endpoints of length of treatment and length of stay 2) Explore buprenorphine pharmacokinetics Buprenorphine Protocol 4.4 gm/kg q8 buprenorphine sublingual (Buprenex in 30% alcohol/sucrose) Dose up-titration by 20% ~one PK sample/day Weaning by 10%/dose after stable 48 hours Cessation at or near initial dose Provision for rescue dose followed by up-titration At maximum 39 gm/kg/day, rescue with phenobarbital Observation for 48 hr after cessation of therapy Buprenorphine Need for Phenobarbital Rescue 3 NOS 1 Dose adjustment Observation Lower than expected bup concentration Rapid up-titration Relatively frequent need for phenobarbital rescue Adjusted dose 1) Increase initial daily dose from 13.2 mcg/kg to 15.9 mcg/kg 2) Increase the up-titration from 20% increase to 25% increase 3) Increase maximum daily dose from 39 mcg/kg to 60 mcg/kg Update 24 patients randomized to new dose schema 40 35 30 23 Buprenorphine (12) Morphine (25) 4 Length of treatment Length of Stay 2 Phenobarbital Adjunct Length of Treatment: All treated patients in trial (N=50) 70 60 50 40 30 20 10 0 Morphine Buprenophine Safety: Serious Events Status epilepticus, treated with lorazepam and phenobarbital Full-term female, scores of 4-6 after 3 days of treatment Neurological work up negative Level = 0.35 ng/mL Normal development at 12 months of age Elevated liver enzymes associated with cytomegalovirus infection Poor feeding, aminoaciduria Abnormalities persisted weeks after dechallenge BuprenorphineSummary Appears as safe as, and more efficacious than morphine Efficacy needs to be tested in blinded clinical trial Use may facilitate expansion into outpatient treatment Polysubstance abuse Thomas Jefferson University Hospital 2000-06 47 50 40 Duration 30 of Therapy 20 (days) 38 31 Nonbenzodiazepine exposed Poly-substance exposed Benzodiazepine exposed 10 0 Seligman NS,. Am J Obstet Gynecol. 2008; 199(4):396.e1-396.e7 Polysubstance abuse Common Worse outcomes Up to 50% of babies at risk for NAS have exposure to benzodiazepines Cause or marker of treatment resistance? Even less clarity of optimal treatment Effects of concomitant psychiatric medications 10.3% of drug-using pregnant women had other psychiatric disorders compared to 1.4% of controls Kennare R. Aust N Z J Obstet Gynaecol 2005;45:220–225. 56% of participants in MOTHER study had prescription for psychiatric medication during pregnancy Mostly anxiolytics and SSRIs Benzodiazepines were exclusion criteria Martin PR. Am J Addict. 2009 ; 18(2): 148–156 Neonatal responses to in utero exposure Antidepressant Mild CNS and respiratory systems 3-5 day duration, self limited Koren G. CMAJ. 2005; 172(11):1457-1459 Ferreira E. Pediatrics. 2007; 119(1):52 Antipsychotics Adults have mild withdrawal symptoms of agitation and insomnia Anecdotal reports of hypertonicity and early onset NAS Paucity of published reports of neonatal withdrawal Einarson A. Use and safety of antipsychotic drugs during pregnancy. J Psychiatr Pract. 2009 May;15(3):183-92. Pharmacogenetics P glycoprotein ABB1 haplotypes have been associated with decreased methadone requirements Coller JK. Cln Pharmacol Ther. 2006,80:682-90 Mu opioid receptor Polymorphism A118G has reduced response to ligands and has been associated with differential pain response, but not methadone dosage A118G may represent propensity for heroin abuse Drakenberg K,. Proc Natl Acad Sci U S A. 2006; 103(20):7883-7888 Somogyi AA, Clin Pharmacol Ther. 2007;81(3):429 Weaker candidates dopamine receptor type 1, preproenkephalin and preprodynorphin Skorpen F, Palliat Med. 2008; 22(4):310-327 Will a genetic test tell us who we can send home early? Not any time soon! Association of genes with addiction in adults not established Relevance of adult polymorphisms to neonates unclear Responses are polygenic and not monogenic Example of sickle cell anemia PK/PD modeling Powerful mathematical techniques to evaluate data Drug levels with sparse sampling NAS scores Age, weight, development Assess sources of variability Understand the biology of development Predict best dose PK/PD model of buprenorphine in neonates 0.5 ID = 12 0.0 0.1 Conc (ng/mL) 0.2 0.3 0.4 Observ ed Predicted Indiv idual 0 100 200 Time (hr) 300 PK/PD models in NAS Clonidine Xie HG. J Clin Pharmacol. 2010 May 19. [Epub ahead of print] Buprenorphine Morphine IV models available NO ORAL DATA! Long term developmental effects of NAS treatment Very difficult data to obtain NAS treatment vs. NAS Post discharge effects likely dwarf treatment Even if there were developmental effects, how would these risks compare to non-treatment of NAS? Actively Recruiting Clinical Trials Maternal acupuncture P. Janssen, Univ. British Columbia LOT primary outcome RCT Fetal neurobehavior and autonomic tone L. Jansson, Johns Hopkins Two observational cohorts Summary of Future Trends Increased research in clonidine and buprenorphine Pharmacogenetics Polysubstance abuse treatment Dose optimization Clear need for more research Black Walnut, Blenerhasset Island, WV