* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Case conference- chronic diarrhea
Hepatitis B wikipedia , lookup
Leptospirosis wikipedia , lookup
Chagas disease wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Sarcocystis wikipedia , lookup
Cryptosporidiosis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
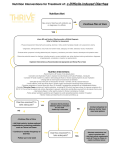
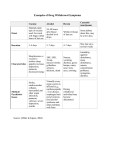
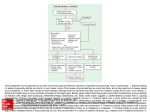
Case conference SHANIKA UDUWANA PGY 1 Case Previously healthy, 9-month-old girl presented with a skin rash to her pediatrician was treated with a 10-day course of cefdinir for presumed impetigo. She developed diarrhea after 1 day of therapy and had up to 20 loose stools per day. The patient was solely on a cow's milk-based formula at the time of presentation, which was then changed to a soy formula. After antibiotics were discontinued the diarrhea persisted, prompting a change to a protein hydrolysate formula. However, the diarrhea continued and the skin rash worsened, resulting in hospitalization a few weeks later. She had no history of fever, vomiting, or hematochezia. No other symptoms were present. Case cont. past medical history was unremarkable. She was born at full term with a birth weight of 3.8 kg. Her growth was normal. no significant medical issues, other than cefdinir she was on no medications. She had no sick contacts or history of travel. The family history revealed that her mother had hypothyroidism, but there was no history of any gastrointestinal illnesses. The social history was noncontributory. Case cont. Examination at the time of hospitalization vital signs were normal. Her weight and height were at the 50th percentile. She was alert, awake, well-developed, mildly dehydrated, and in no acute distress. Skin exam revealed a generalized erythematous rash consistent with staphylococcal scalded skin syndrome. Lung and heart examinations were normal. The abdomen was soft, nontender, nondistended, without hepatosplenomegaly, and with normoactive bowel sounds. Rectal exam was normal and negative for occult blood. Musculoskeletal and neurologic exams were unremarkable. Differentials? Labs? Cbc Bmp Stool for ova and parasites Bacterial culture C difficile toxins A and B Stool cell count Reducing substances were measured at 0.75% to 2% stool pH of 5 glucose breath test were normal Oral feedings were initially held and diarrhea ceased. However, upon reintroduction of enteral feeding with an elemental amino acid-based formula, the diarrhea resumed. Osmotic vs secretory? when oral intake was discontinued, diarrhea ceased, indicating that it was an osmotic and not a secretory type of diarrhea. With the latter, diarrhea continues upon discontinuation of oral intake. Aside from discontinuation of oral intake, another method for differentiating osmotic from secretory diarrhea is by evaluation of the stool ion gap, calculated by the following formula: measured stool osmolarity - 2 (Na[stool] + K[stool]). Using this formula, secretory diarrhea presents with normal stool osmolarity with an ion gap of less than 50 mOsm in contrast to osmotic diarrhea, which causes increased osmolarity and a stool ion gap of greater than 100 mOsm Osmotic diarrhea is caused by the presence of unabsorbed nutrients in the GI tract, frequently secondary to intestinal damage leading to impairment in digestion or absorption. The most common form is lactose intolerance in a setting of infection in which lactose is not being enzymatically cleaved and absorbed in the small intestine. It then reaches the colon in an intact form where the colonic bacteria ferment it causing an osmotic gradient that drives water into the lumen, leading to diarrhea. Secretory diarrhea is characteristically due to epithelial cells secreting electrolytes and water into the lumen of the intestine. Several infectious agents, including Vibrio cholerae, enterotoxigenic Escherichia coli, and Cryptosporidium parvum, can cause secretory diarrhea through the production of a toxin that causes active transport of ions and water into the lumen. In addition to infectious causes, some hormones -- such as vasoactive intestinal peptide, gastrin, serotonin, and acetylcholine -produced by neuroendocrine tumors can cause a secretory diarrhea. What should be the next step in work-up to determine the etiology of the diarrhea? The next step in the evaluation should consider that this was a case of an osmotic diarrhea, indicating malabsorption. Therefore, the evaluation should focus on the nutrient type that is not being efficiently absorbed, ie, protein, carbohydrate, or fat. Positive reducing substances and acidic stool indicate carbohydrate malabsorption; fecal elastase level and 72-hour fecal fat collection for calculation of fat clearance can help evaluate for fat malabsorption; and measurement of the stool alpha-1 antitrypsin level investigates intestinal protein loss. Glucose breath testing was performed to evaluate for the presence of glucose-galactose transporter defect; findings were negative. Further studies that can be performed to determine the specific carbohydrate that is being malabsorbed include esophagogastroduodenoscopy (EGD) with histology and additional duodenal biopsies for determination of disaccharidase levels, and rarely electron microscopy as well as other carbohydrate-specific hydrogen breath tests (lactose, sucrose, fructose, and maltose). The patient underwent EGD; findings, including histology, were normal. Dissacharidase levels were consistent with congenital deficiency of sucrase-isomaltase and maltase. Cow's milk-based formula was restarted without return of symptoms. The reintroduction of a lactose-containing formula that does not contain sucrose or isomaltose was sufficient to resolve the patient's symptoms. Definition: chronic diarrhea Chronic diarrhea is defined as stool volume of more than 10 grams/kg/day in infants and toddlers, or more than 200 grams/day in older children for more than 14 days FUNCTIONAL DIARRHEA Defined as the painless passage of three or more large, unformed stools during waking hours for four or more weeks, with onset in infancy or the preschool years, and without failure to thrive or a specific definable cause. This common, benign disorder has also been termed chronic nonspecific diarrhea of childhood or toddler's diarrhea. Children with functional diarrhea usually pass stools only during waking hours. Early morning stools typically are large and semi-formed, then stools become progressively looser as the day progresses. Virtually all children develop normal bowel patterns by four years of age. Trials of the following dietary changes are recommended: Reduce or eliminate fruit juice or other osmotically active carbohydrates. Apple, prune, and pear juice contain sorbitol and have a particularly high osmotic load. Liberalize the fat content of the diet to 35 to 50 percent of total calories. Other than these two measures, alterations in diet are not helpful and are sometimes counter-productive. Postenteritis syndrome Most enteric infections in otherwise healthy children resolve within 14 days and do not develop into a chronic diarrheal illness. However, in a minority of patients, an acute gastroenteritis can trigger persistent diarrhea by causing mucosal damage to the small intestine, termed a "postenteritis syndrome". The mechanisms underlying this syndrome are not fully understood. Contrary to previous hypotheses, sensitization to food antigens and secondary disaccharidase deficiency, including lactase deficiency (causing lactose intolerance), are uncommon. Therefore, international guidelines discourage the use of hypoallergenic or diluted milk formulas during acute gastroenteritis. Recurrent or sequential enteric infections may be responsible for some of these cases. In some cases, treatment with probiotic bacteria may facilitate recovery from postenteritis syndrome. Bacteria In immuno-compromised patients, common infectious causes of acute diarrhea, such as Campylobacter or Salmonella, can cause persistent diarrhea. Chronic infections with these pathogens are uncommon in immuno-competent hosts. Bacterial cultures should be part of the initial diagnostic evaluation for all patients if the stool contains blood, or for immuno-compromised patients regardless of fecal blood. In children recently treated with antibiotics, Clostridium difficile may cause a colitis characterized by "pseudomembrane" formation. The enzyme immunoassay available in most laboratories detects C. difficile toxins A and B with high specificity but only moderate sensitivity. Polymerase chain reaction (PCR) based diagnostic methods can enhance the detection rate Parasites Intestinal parasites are an uncommon cause of chronic diarrhea in developed countries, except among individuals with an immunodeficiency. Specific antigen assays for Giardia and examination from the stool for parasites is imperative for children with known immunodeficiencies or with a history of travel to endemic areas. These tests are also an appropriate step in the evaluation of immunocompetent children if initial testing fails to determine a cause of the chronic diarrhea. When a specific parasite is identified, treatment with specific medications is generally indicated, although the organism may not always be the cause of the diarrhea. Empiric therapy for enteric pathogens is generally not advisable. IMMUNE DEFICIENCY Chronic diarrhea may present as a complication of a known immune deficiency such as HIV disease. Evaluation should focus on potential infectious causes of the diarrhea, particularly parasites and opportunistic infections such as Cryptosporidium, Isospora, and Cyclospora . These children also are at risk for persistent infectious pathogens that typically cause acute diarrheas, such as rotavirus Chronic diarrhea also may be a presenting symptom of immune deficiency in a child. When a patient is infected with an unusual pathogen, or has multiple or recurrent infections of the gastrointestinal tract or elsewhere, further evaluation for immune deficiency is required. In rare instances, live vaccines may call attention to the potential diagnosis of immunodeficiency by inducing chronic infection. As an example, vaccine-acquired chronic rotavirus diarrhea has been observed in infants with severe combined immunodeficiency ABNORMAL IMMUNE RESPONSE Celiac disease (also known as gluten-sensitive enteropathy or nontropical sprue) Immune-mediated inflammation of the small intestine caused by sensitivity to dietary gluten and related proteins in genetically sensitive individuals. Common, occurring in 0.5 to 1 percent of the general population in most countries. Often presents as chronic diarrhea, with or without malnutrition, during late infancy or early childhood Classic clinical features include symptoms of malabsorption such as diarrhea, steatorrhea, weight loss, or other signs of nutrient or vitamin deficiency, the presence of characteristic histologic changes (including villous atrophy) on small intestinal biopsy, and resolution of the mucosal lesions and symptoms upon withdrawal of gluten-containing foods, usually within a few weeks to months. ABNORMAL IMMUNE RESPONSE Inflammatory bowel disease Ulcerative colitis and Crohn's disease are idiopathic chronic inflammatory diseases of the bowel. These disorders typically present with gradual onset of chronic diarrhea, with or without blood, from mid-childhood through adulthood Considered in a child or adolescent presenting with loose stools or bloody diarrhea, abdominal pain, weight loss or growth failure, perianal disease, anemia, arthritis, or delayed onset of puberty. Extraintestinal manifestations of IBD may involve the skin, joints, liver, eye, bones, and (rarely) respiratory system Laboratory testing often reveals anemia, hypoalbuminemia, and/or an elevated erythrocyte sedimentation rate; however, laboratory studies are normal in a significant number of children with IBD If the clinical presentation and/or initial laboratory testing support the diagnosis of IBD, further evaluation should include both small bowel imaging and colonoscopy, (with biopsies taken from the terminal ileum, if possible). Biopsies from the terminal ileum and each segment of the colon should be sent for histopathologic examination. Upper endoscopy is also routinely performed at the time of the initial colonoscopy, and provides further information as to disease type and extent ABNORMAL IMMUNE RESPONSE Allergic enteropathy An abnormal immune response to food proteins can cause a proctitis/colitis or an enteropathy. Food protein-induced proctitis/proctocolitis is characterized by blood-tinged stools in an otherwise healthy infant, and is caused by proteins from cow's milk, or occasionally soy or other foods, which are ingested through breast milk or standard cow's milk- or soy-based formulas. Treatment is empiric, consisting of complete elimination of cow's milk (or other suspected antigen) from the diet. The sensitivity resolves by one year of age in almost all infants Food protein-induced enteropathy is characterized by malabsorption, failure to thrive, anemia, diarrhea, vomiting, and hypoproteinemia; it is usually induced by cow's milk protein. The diagnosis is suspected based on clinical features and confirmed by endoscopy with biopsies, which show villus blunting. ABNORMAL IMMUNE RESPONSE Eosinophilic gastroenteritis This is an incompletely understood disorder that is sometimes but not always associated with an identifiable dietary antigen. Approximately onehalf of patients have allergic disease, such as asthma, defined food sensitivities, eczema, or rhinitis; some patients have elevated serum IgE levels; rare patients have IgE antibodies directed against specific foods. Microscopic and collagenous colitis Microscopic colitis typically presents with chronic watery nonbloody diarrhea. typically occurs in middle-aged adults, but occasionally presents in children. Endoscopy grossly normal, histopathology > abnormal inflammatory findings, characterized by a collagenous colitis or lymphocytic colitis, sometimes with an eosinophilic infiltrate. This disorder may represent an overlap with the eosinophilic gastroenteropathies. Microscopic colitis in children usually responds well to aminosalicylic acid (5-ASA) medications. Some cases in adults have been successfully treated with budesonide. ABNORMAL IMMUNE RESPONSE Autoimmune enteropathies Autoimmune enteropathies are rare disorders that may present as severe diarrhea during infancy or toddlerhood. The diarrhea may be isolated, or may occur in association with diabetes mellitus as part of the IPEX syndrome (Immune dysregulation, Polyendocrinopathy and Enteropathy, X-linked), which is associated with mutations in the FOXP3 gene. IPEX is characterized by chronic diarrhea, which usually begins in infancy, dermatitis, autoimmune endocrinopathy (diabetes mellitus, thyroiditis). Antienterocyte antibodies may be present. MALDIGESTION OF FAT Cystic fibrosis Cystic fibrosis is the most common cause of pancreatic exocrine insufficiency in children. The disease may present at birth with meconium ileus, or may be suggested later by gastrointestinal symptoms of fat malabsorption, failure to thrive, rectal prolapse (particularly in the setting of diarrhea) or pulmonary symptoms. Other causes of pancreatic insufficiency Other causes of pancreatic exocrine insufficiency include Shwachman-Diamond syndrome (associated with bone marrow failure and skeletal abnormalities), and two rare disorders, Pearson syndrome and Johanson-Blizzard syndrome. CHOLERHEIC DIARRHEA Patients who have undergone resection of the terminal ileum have impaired absorption of bile acids. If sufficient bile acids enter the colon, they may cause a secretory diarrhea. Similarly, patients who have had a cholecystectomy can develop cholerheic diarrhea because the continuous drainage of bile into the small bowel may overcome the terminal ileum’s reabsorptive capacity. BOWEL OBSTRUCTION OR DYSMOTILITY Partial bowel obstruction or dysmotility may present with diarrhea. Hirschsprung's disease may present with dysmotility and diarrhea, and may progress to life-threatening toxic megacolon Intestinal pseudoobstruction This disorder of intestinal motility typically presents with constipation, but patients also may have periods of diarrhea, particularly if bacterial overgrowth supervenes. CONGENITAL SECRETORY AND OSMOTIC DIARRHEAS If a congenital diarrhea is suspected, stool electrolytes, pH, fat, and reducing substances should be measured. A trial of fasting should be performed to determine if the diarrhea is secretory or osmotic. A marked decrease in stool output during fasting and high stool osmolarity (eg, more than 40 mOsm greater than the serum osmolarity) suggests an osmotic diarrhea Mucosal biopsies should be performed in patients with congenital diarrhea. The findings vary with etiology: In congenital chloride diarrhea (CCD) and congenital sodium diarrhea (CSD), the histology is usually normal. In enteric anendocrinosis, the mucosal architecture is normal, but special stains demonstrate absence of enteroendocrine cells. In tufting enteropathy, the histopathology is characterized by villous atrophy, with disorganization of the surface enterocytes with focal crowding, resembling tufts. In microvillus inclusion disease, light microscopy shows a variable degree of hypoplastic villus atrophy without crypt hyperplasia, and PAS-positive granules at the apical pole of enterocytes. Electron microscopy reveals characteristic microvillus inclusions and partial to total atrophy of microvilli on mature enterocytes. In chylomicron retention disease, light microscopy may reveal lipid droplets in duodenal enterocytes. NEUROENDOCRINE TUMORS Gastrinoma In this syndrome, also known as Zollinger-Ellison syndrome, unregulated secretion of gastrin causes hypersecretion of gastric acid, with consequent peptic ulcer disease and chronic diarrhea. Fewer than 5 percent of patients present during adolescence. The disorder may be suspected in a patient presenting with unexplained peptic ulcer disease and/or with a secretory diarrhea and fat malabsorption. Fasting serum gastrin levels are elevated 5 to 10 fold. VIPoma Unregulated hypersecretion of vasoactive intestinal polypeptide (VIP) causes watery diarrhea, hypokalemia, and achlorhydria. VIPomas are very rare in children, but may occur as ganglioneuromas and ganglioneuroblastomas in the sympathetic ganglia and in the adrenal glands (rather than in the pancreas where they are often found in adults). Mastocytosis In children, this disorder usually takes the form of cutaneous mastocytosis, consisting only of the skin lesions of urticaria pigmentosa, and is often self-limited. A few children, particularly those presenting after 2 years of age, have systemic mastocytosis, which may include histamine-induced gastric hypersecretion and chronic diarrhea FACTITIOUS DIARRHEA May be characterized by a true increase in stool volume, which is self-induced (eg, laxative abuse), or the creation of an apparent increase in stool volume by the addition of various substances to the stool (eg, water or urine). Diagnosing factitious diarrhea is often difficult and requires alertness to this possibility, exclusion of other diseases, and may be aided by specific testing Questions 1. Which of the following pairs correctly matches an organism with its most likely source of infection? A. Adenovirus – unpasteurized milk. B. Cryptosporidium parvum – contaminated swimming pool. C. Giardia lamblia – undercooked pork. D. Plesiomonas – raw pig intestines. E. Yersinia – contaminated well water. 2. You are evaluating a 7-year-old girl in your office who has a 6-week history of watery, foul-smelling diarrhea. She also has experienced some bloating and cramping but no weight loss. She just returned from summer camp. You suspect giardiasis. Which of the following tests is the simplest and most reliable in helping you confirm your diagnosis? A. Duodenal biopsy. B. Fecal Giardia antigen test. C. Fecal ova and parasites. D. Stool culture. E. String test. 3. Which of the following diarrheal diseases is most likely to present after 6 months of age? A. Congenital chloride diarrhea. B. Congenital sodium diarrhea. C. Microvillus inclusion disease. D. Tufted enteropathy. E. VIPoma. 4. You are evaluating a 6-month-old boy in the hospital. He has had several episodes of watery diarrhea since the age of 3 months, at which time he was hospitalized for rotavirus infection. He has been receiving an oral electrolyte solution primarily because his mother has been reluctant to start him again on his regular milk-based formula. His weight at 3 months was 5.6 kg; his current weight is 6.2 kg. Except for mild dehydration, findings on his examination are normal. His electrolyte concentrations are normal, with the exception of a serum HCO3 of 12 mEq/L (12 mmol/L). Which of the following is the best next step in management? A. Complete bowel rest and initiation of parenteral nutrition. B. Continuation of his milk-based formula with additional zinc supplementation. C. Initiation of a full-strength lactose-free, sucrose-free formula. D. Initiation of an immunologic evaluation. E. Stool for Giardia fecal antigen and culture. Chronic Diarrhea,DOI: 10.1542/pir.26-1- 5,Pediatrics in Review 2005;26;5,James P. Keating uptodate