* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
Survey
Document related concepts
Transcript
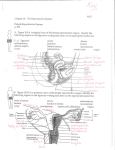
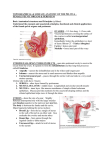
Stump the Professor Women’s Health Symposium August 2, 2009 Jenny Lovegreen Elizabeth VonderHaar Leah Smith History of Present Illness • CO is 14 year old G0 referred from an outside facility with an 18 month history of cyclic abdominal pain. The patient has never had any vaginal bleeding and for the last two cycles, her pain was severe enough that she had to hospitalized for pain control with IV medication. Past Medical History • • • • MEDICATIONS: tetracycline ALLERGIES: NKDA SURGICAL HISTORY: appendectomy OB/GYN HISTORY: – Began breast development and pubic hair development at age 11 – Has never had any vaginal bleeding – Denies sexual activity – G0 – Is not on contraception Past Medical History • FAMILY HISTORY: – Non-contributory • SOCIAL: – Student – Denies EtOH, Tobacco, Illicit drug use PHYSICAL EXAM • GENERAL: 5’ 7” 55.5 KG white female in NAD • VITALS: P 92 BP 100/54 R 18 • ABDOMEN: Flat, Soft, non-tender • Differential Diagnosis • Further Work up Pelvic Exam • Normal external female genitalia • Tanner stage 3 pubic hair • No signs of clitoral enlargement Pelvic Exam • Speculum Exam: long vaginal canal with no cervix visualized at the apex • 1-finger digital exam performed and the apex of the vagina appeared to cover a structure that felt like a long thin cervix • No adenexal masses or tenderness • Small anteverted uterus IMAGING • MRI: – Vaginal canal with what appears to be a thin septum covering the external cervical os – No free fluid outside of the Uterine Cervix – Normal Appearing Left and Right Ovaries – Uterus • Minimal indentation/Possibly suggestive of arcuate uterus • Narrowing in the lower segment and cervical canal • Endometrium noted IMAGING • MRI (CONT) – Small amount of free fluid noted in the pouch of Douglas – Urinary Tract: • Both Kidneys present • Right Renal collecting system completely unremarkable • Left Renal collecting system with what may be some duplication, although duplicated ureter could not be confirmed in its entirety IMAGING • TRANSABDOMINAL ULTRASOUND: – 6.8 X 3 X 6 cm uterus. – Central endometrial echo thickened (1.5 cm) at the fundus, which thins going to the uterine corpus and is thin going through what appears to be a cervical canal LABS • H/H: 10.5/30.9 • O positive/Negative ABSC Operative Findings • • • • Normal appearing uterine size and shape Normal appearing left tube and ovary Normal appearing right tube Small right ovary with a streak-like appearance • Bilateral Ureters • Posterior cul-de-sac containing multiple cystic structures, likely endometriosis WHAT REALLY HAPPENED . . . • CO started on continuous oral contraceptives with significant relief of her dysmenorrhea • MRI repeated, diagnosis of most likely cervical agenesis with a small vaginal septum • CO, stepmother and sister included in discussion of treatment options: – Continuous OCPs • Future GIFT procedure • Future attempt at recanalization – Attempt at recanalization – Hysterectomy with retention of her ovaries OPERATIVE FINDINGS • Laparoscopic examination revealed no identifiable cervical canal at the distal Uterine segment • Digital vaginal exam revealed no blood • Boggy-feeling inferior portion of the uterus (specimens removed via the morcilator) PATHOLOGY • Uterus – Cervix not identified grossly or microscopically – Endometrium: benign inactive endometrium with stromal pseudodecidual changes consistent with hormone effect – Myometrium: extensive adenomyosis • Posterior cul-de-sac biopsy: – Changes consistent with endometriosis; no atypia and no malignancy identified Cervical Agenesis • Rare condition: 1 in 80,000 – 100,000 births • Associated with both partial and complete vaginal aplasia and renal anomalies • Type Ib mullerian anomaly Cervical Agenesis • Mullerian ducts develop into the fallopian tubes, uterus, cervix, and upper vagina. • Fused mullerian ducts form the corpus and cervix of the uterus • Vagina has dual origin – upper portion from uterine canal and lower from urogenital sinus • Atresia of both sides of mullerian ducts leads to cervical agenesis – Usually associated with lack of upper vagina due to common mullerian source • Uterus develops normally Diagnosis: Cervical Agenesis Presentation • • • • Presentation of obstructive anomaly Primary amenorrhea Cyclic abdominal or pelvic pain Distended uterus if functional endometrium is present • Endometriosis due to retrograde flow Diagnosis and Management • CT scan, ultrasound, and MRI are all helpful in evaluating anatomy • If uterus is obstructed – hysterectomy is recommended – Creation of epitheliazed endocervical tract and vagina is an alternative • Associated with significant morbidity Diagnosis and Management • Conservative management using OCPs to suppress retrograde menses can be possible until pt is ready to evaluate reproduction options References • Creighton, SM, et al, “Laparoscopic management of cervial agenesis,” Fertility and Sterility. Vol. 85 No. 5 May 2006 • Sadler, TW, “Urogenital System,” Langman’s Medical Embryology. 9th ed • William’s Gynecology. “Cervical Defects.” Access Medicine, 2009.