* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chapter 42
Survey
Document related concepts
Transcript
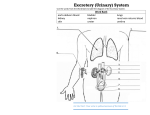
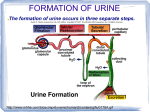
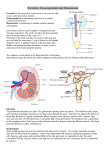
Chapter 42 The Internal Environment: A Summary AP Biology Spring 2011 Gains and Losses in Water and Solutes Interstitial fluid: fills tissue space between cells Circulatory system: moves blood to and from tissues Interstitial fluid and blood are extracellular fluid that functions as an internal environment for body cells Composition and volume must be maintained within range body can tolerate (homeostasis) Terms Urinary system: collection of interacting organs that counter shifts in the composition and volume of extracellular fluid Paired kidneys: filter blood, from urine, help maintain body’s water-solute balance Urine: fluid excreted from the body, contains nitrogenous wastes and excess amounts of other solutes and water Challenges in Water In most marine invertebrates, interstitial fluid is like seawater in its concentrations of solutes, so little water is gained or lost by osmosis In vertebrates, body fluids about 1/3 as salty as seawater Challenges in Water Freshwater fish and amphibians constantly gain water and lose solutes Neither can drink water Water move in by osmosis, leaves as dilute urine Solute loss balanced by intake of more solutes with meals and active pumping of sodium into cells of gills and skin at membrane transport proteins Marine bony fish contain les salt and lose water by osmosis Gulp in seawater, gill cells pump out excess solutes, dissolved wastes are excreted in tiny volume of concentrated urine Challenges on Land Gain and loss of water: Water enters gut through food or drink Do not lose water by way of osmosis Lost it in controlled ways, mainly urinary excretion Urinary excretion: excess water and solutes exit body as urine Some water evaporates from respiratory surfaces, leaves from sweating, small amounts leave through feces Challenges on Land Gain and loss of solutes: Absorption of nutrients from gut, secretions from cells, and release of carbon dioxide wastes adds solutes; air intake from lungs adds oxygen Loose solutes mainly in sweat, respiration, and urinary excretion All exhale carbon dioxide Urea: ammonia, toxic by product of protein metabolism is converted to urea, which is then excreted in urine Components of Urinary System 2 kidneys 2 ureters Urinary bladder Urethra Components of Urinary System 2 kidneys: bean-shaped organs about the size of a fist, located between peritoneal lining and abdominal cavity wall, where they flank the backbone Components of Urinary System Dense connective tissue encapsulates each kidney Beneath capsule is outer tissue zone, kidney cortex Cortex is continuous with kidney medulla, inner zone with pyramid shaped lobes of tissue, appears striated because of long tubes that extend down to a chamber, the renal pelvis Components of Urinary System Renal artery: transports blood to kidney Then flows through arterioles, capillaries, and venules in cortex and medulla Venules connect with renal vein, leads out of kidney Components of Urinary System Urine forms in kidneys Then enters one of two ureters that connect with muscular sac, the urinary bladder Urinary bladder: has stretch receptors that are stimulated when urine fills the sac Reflex response causes smooth muscle to contract and forces urine into urethra Urethra: muscular tube that opens on to the body surface After age 2-3, urination can be voluntarily controlled by neural signals that act on a sphincter of skeletal muscle at the start of the urethra The Nephron Nephron: small functional units that are only one cell thick all along their length Each kidney contains more than a million The Nephron Nephron starts in kidney cortex Nephron’s wall balloons outward like a cup Nephron continues in cortex as a twisting tube Straightens as descends to kidney medulla, then ascends into the cortex There, another convoluted region connects with a collecting duct As many as 8 nephrons can empty into the same duct Duct extends through the kidney medulla and opens into renal pelvis The Nephron The cup shaped entrance = Bowman’s capsule At Bowman’s capsule, thin nephron wall doubles back on itself and encloses walls of highly porous blood vessels clustered inside Glomerular capillaries Bowman’s capsule and glomerular capillaries interact as blood filtering unit Unit= renal corpuscle The Nephron Bowman’s capsule collects fluid that is forced out, under pressure, from glomerular cappilaries Fluid enters proximal convoluted tubule Proximal means region closest to start of nephron Loop of Henle: plunges into medulla, makes hairpin turn, and ascends out of it Distal tubule: convoluted part most distant from entrance of nephron Nephron A. Glomerular B. C. D. E. F. capillaries Bowman’s Capsule Proximal tubule Distal tubule Collecting duct Loop of Henle Renal artery branches into The Nephron afferent arterioles, one for each nephron Delivers blood to glomerular capillaries Capillaires rejoin and form an efferent arteriole, which carries away blood that did not get filtered into Bowman’s capsule Arteriole branches to form peritubular capillaries that thread all around nephron Rejoin as venules, which join renal vein leading out of kidney The Nephron Urine forms continually by 3 processes that exchange water and solutes between all of the nephrons, glomerular capillaries, and peritubular capillaries Glomerular filtration Tubular reabsorption Tubular secretion Each minute nephrons in both kidneys filter close to 125 milliliters of fluid from the blood flowing past = 180 L/day Urine Formation: Glomerular Filtration Blood pressure generated by heart drives glomerular filtration, first step of urine formation In glomerular capillaries inside Bowman’s capsule of each nephron, pressure forces out 20% of volume of plasma Cell wall of glomerular capillaries, the inner cell wall of Bowman’s capsule, and basement membrane between them are like a sieve They nonselectivly let everything (water, ions, glucose, etc.) besides blood components become the filtrate Urine Formation: Glomerular Filtration Urine Formation: Glomerular Filtration Volume of blood kidneys must handle at any time is adjusted at afferent arterioles that deliver blood to nephron Will vasodilate in response to signals from sympathetic neurons (blood pressure increases) Will vasoconstrict when blood pressure decreases If too much fluid enters body- reflex pathway overrides sympathetic signals, vasdilates Urine Formation: Tubular Reabsorption Nephron (proximal tubule), gives back most of filtrate, in amounts required to maintain volume and composition of internal environment Tubular reabsorption: variety of substances leak or get pumped out of nephron, diffuse through interstitial fluid, and enter peritubuler capillary Returns close to 99% of filtrates water, 100% of glucose and A.A, all but 0.5% of Na+, and 50% of urea to blood Urine Formation: Tubular Reabsorption Cotransporters span plasma membrane of cells making up nephrons tubular walls As filtrate flows through proximal tubule, ions and some nutrients are actively and passively transported outward, into interstitial fluid Water follows by osmosis Cells making up peritubular capillaries transport them into blood, water follows by osmosis Passive transporters: Na+ and glucose Sodium potassium pump Electrochemical gradient: Na+, Cl Osmosis Urine Formation: Tubular Reabsorption Occurs at Proximal Tubule Urine Formation: Tubular Secretion Urea, H+, K+, other wastes, end up in blood Tubular Secretion: transporters in walls of peritubular capillaries move ions into interstitial fluid Transporters in tubular wall of nephrons move them from interstitial fluid into filtrate, can be excreted in urine Secretion of H+ is maintaining body’s acid-base balance Urine Formation: Concentrating the Urine Kidney’s cortex, filtrate is isotonic with interstitial fluid No net movement of water from one to another Kidney’s medulla, interstitial fluid is hypertonic Draws water out of filtrate by osmosis, along loop of Henle’s descending limb Filtrate becomes most concentrated and attracts most water by hairpin turn Urine Formation: Concentrating the Urine Loop of Henle’s wall after turn is impermeable to water Transporters in ascending limb actively pump Na+ and Cl-, which makes interstitial fluid in medulla even saltier, which draws out even more water before hairpin turn Countercurrent mechanism: transporters are altering composition of filtrate that is flowing in opposite direction inside loop of Henle Thirst Mechanism When you do not drink enough water Solute concentration in blood is high, which slows saliva secretions into mouth Drier mouth stimulates nerve endings that signal thirst center Region of hypothalamus Thirst center also receives signals from osmoreceptors that detect rise of blood level of sodium inside brain Thirst center notifies other centres in cerebral cortex, which compel you to search for and drink fluid Hormonal controls act to conserve water already inside body Effect of ADH ADH: antidiuretic hormone When signaled by osmoreceptors, hypothalamus stimulates the pituitary gland to secrete ADH Promotes water conservation ADH makes walls of distal tubules and collecting ducts more permeable to water, thus urine becomes more concentrated As volume of extracellular fluid rises and solute concentration declines, ADH secretion slows Effect of ADH Loss of blood pressure or nausea and vomiting can also trigger ADH secretions Aquaporines selectively allow water to diffuse rapidly across plasma membrane ADH alters reabsorption in target cells by affecting these passive transporters Effect of Aldosterone Aldosterone: hormone stimulates production of sodium- potassium pumps and their insertion into the plasma membrane of cells in collecting ducts walls Cells in arterioles release the enzyme rennin in response to a decline in the volume of extracellular fluid Renin starts chain of reactions that results in secretion of aldosterone by adrenal glands located above each kidney Effect of Aldosterone Aldosterone stimulates production and placement of sodium- potassium pumps into the plasma membrane of cells in collecting duct wall Urine becomes more concentrated Atrial natruitec peptide (ANP) makes urine more dilute by inhibiting the secretion of aldosterone and also by indirectly inhibiting rennin secretion Abnormalities in Hormonal Control Diabetes insipidus occurs when pituitary gland secreted too little ADH, when receptors do not respond to ADH, or when the aquaporin proteins are missing or modified and do not work Symptoms: large volumes of highly dilute urine and insatiable thirst Abnormalities in Hormonal Control Oversecretion of ADH causes kidneys to retain too much water, allowing solute concentrations in interstitial fluid to decline Solutes move out of body cells into interstitial fluid while water in the interstitial fluid move out and into body cells In brain cells this process can be deadly Hyperaldosteronism occurs when adrenal gland tumors cause over secretion of aldosterone, leading to fluid retention and high blood pressure Acid-Base Balance Maintained by controlling hydrogen ions through buffer systems, respiration, and excretion by kidneys Buffers can neutralize hydrogen ions by bicarbonate-carbon dioxide buffer system; the lungs can eliminate carbon dioxide Acid-Base Balance Only urinary system can eliminate excess hydrogen ions The HCO3- that forms in nephron cells is moved to capillaries where it neutralizes excess acid The H+ that forms in cells is secreted into tubular fluid where it combines with bicarbonate ions to form carbon dioxide (which is returned to blood and excreted by the lungs) and water (which is excreted in urine) Hydrogen ions are permanently removed from extracellular fluid Life-threatening metabolic acidosis develops when kidneys cannot excrete enough of the H+ released during metabolism Renal Failure Most kidney problems are outcomes of diabetes mellitus and high blood pressure While some people are genetically predisposed to kidney problems, toxins (lead, arsenic, pesticides) may accumulate in kidney tissues, causing them to fail High protein diets increase the risk of for kidney stones and cause kidneys to work hard to dispose of nitrogen-rich breakdown products Renal failure occurs when rate of filtration through glomerular capillaries drops by half Kidney Dialysis A kidney dialysis machine is used to restore proper solute balances after renal failure Hemodialysis connects machine to vein or artery and pumps blood through semipermeable tubes soaked in solutes; as patients blood flows through the tube, the wastes diffuse out and solute concentrations are restored as the cleansed, balanced blood flows back to patient Peritoneal dialysis pumps a fluid of a specific composition into a patient’s abdominal cavity, allowing the peritoneum (lining of the abdominal cavity) to function as the membrane for dialysis Kidney Dialysis Kidney Transplants About 12,000 people are recipients of kidney transplants annually in US Shortage of suitable donors; 40,000 remain on waiting list Most are available after donors death or from relatives or friends; kidney’s from living donors have a higher success rate in transplants than a kidney from a dead person Potential alternative to donors is use of genetically modified pigs as organ factories Core Temperature Change The core temperature of an animal body rises when heat from surrounding or metabolism builds up Core Temperature Change 4 processes drive exchange of heat Thermal radiation: gain of heat from some source, or loss of heat from the body to the surroundings, depending on temperatures of environment Conduction: transfer of heat from one object to another when they are in direct contact, as when a human sits on cold or hot concrete Convection: transfer of heat by way of a moving fluid such as air or water Evaporation: process whereby heated substance changes from a liquid to a gaseous state with a loss of heat to the surroundings Core Temperature Change Endotherm, Ectotherm, Heterotherm Ectotherms: (lizards) have low metabolic rates; therefore they must gain their heat from their environment in behavioral temperature regulation Endotherm, Ectotherm, Heterotherm Endotherm: (birds, mammals) generate heat from metabolic activity and exercise controls over heat conservation and dissipation by means of adaptations such as feathers, fur, or fat, which reduce heat loss Endotherm, Ectotherm, Heterotherm Heterotherm: (hummingbird) generate body heat during their active periods but resemble ecototherms during inactive times Endotherm, Ectotherm, Heterotherm Warmer climates favor ectotherms since they conserve energy as they maintain the core temperature Cold climates favor endotherms Temperature Regulation in Mammals: Responses to Heat Stress When mammals become too hot the hypothalamus send signals to widen diameter of blood vessels to allow greater volumes of blood to reach the skin and dissipate the heat Evaporative heat loss by sweating is cooling mechanism Sweating to dissipate heat can only be effective when the external temperatures are high enough to cause evaporation Nearly all mammals (except marine species) sweat; many pant or lick fur to assist evaporative cooling Temperature Regulation in Mammals: Responses to Heat Stress Hyperthermia is rise in core temperature, with devastating effects Fever is defensive response against pathogens that occurs with a rise in core temperature above normal set point Temperature Regulation in Mammals: Responses to Cold Stress Mammals respond to cold by redistributing blood flow, fluffing hair and fur, and shivering In some responses hairs or feathers become more erect to create a layer of still air that reduces convection and radiative heat losses Shivering responses are common response to cold but are not effective for very long and come at high metabolic cost Nonshivering responses include release of thyroid hormones that bind to brown adipose tissue increasing metabolism Hypothermia is condition in which the core temperature drops below normal; may lead to brain damage and death




























































![Urinary System_student handout[1].](http://s1.studyres.com/store/data/008293858_1-b77b303d5bfb3ec35a6e80f57f440bef-150x150.png)