* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Red Book: 2009 Report of the Committee on Infectious Diseases.
Sociality and disease transmission wikipedia , lookup
Germ theory of disease wikipedia , lookup
Acute pancreatitis wikipedia , lookup
Vaccination wikipedia , lookup
Globalization and disease wikipedia , lookup
Hepatitis C wikipedia , lookup
Hepatitis B wikipedia , lookup
Schistosomiasis wikipedia , lookup
Cryptosporidiosis wikipedia , lookup
Infection control wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
Multiple sclerosis signs and symptoms wikipedia , lookup
Urinary tract infection wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Neonatal infection wikipedia , lookup
Marburg virus disease wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Common cold wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
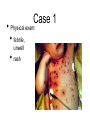
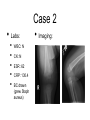
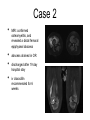
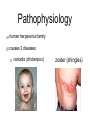
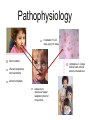
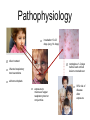
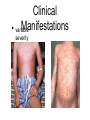
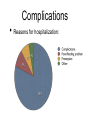
Pediatric Infectious Diseases cont’d... Case 1 • 15 month old Aboriginal male • rash, fever, irritability • 2 sibs with same rash, uncomplicated • PMHx: well • meds: none • NKDA • Imm: 2P, 4P, 6O, 12O Case 1 • Physical exam: • febrile, unwell • rash Case 1 • Management: • • • • • kept in negative pressure room FSWU done - neg U/A and LP covered with vancomycin wound culture grew MRSA stayed 4 days in hospital, discharged on Septra x 2 weeks Case 2 • 12 month old Hutterite male • rash + fever 12 days ago, then sore right knee x 10 days • PMHx: well • meds: none • NKDA • Imm: 2P, 4P, 6P, 12O Case 2 • Physical exam: • afebrile, well • MSK: R distal thigh swollen, warm, not red; decreased ROM of knee (o o 10 flexion, -10 extension); N ROM hip and ankle Case 2 • Labs: • • • • • WBC: N CK: N ESR: 62 CRP: 130.4 BC drawn (grew Staph aureus) • Imaging: Case 2 • Management: • • • covered with cloxacillin admitted to hospital further work-up: • • • • bone scan + U/S: thigh abscess taken to OR for drainage f/u X-ray abN Case 2 • • • • MRI: confirmed osteomyelitis, and revealed a distal femoral epiphyseal abscess abscess drained in OR discharged after 19 day hospital stay iv cloxacillin recommended for 6 weeks What was the underlying illness? What was the underlying illness? Varicella Zoster Virus Pathophysiology human herpesvirus family causes 2 diseases: Pathophysiology human herpesvirus family causes 2 diseases: varicella (chickenpox) zoster (shingles) Pathophysiology Pathophysiology direct contact infected respiratory tract secretions airborne droplets Pathophysiology direct contact infected respiratory tract secretions airborne droplets exposure to mucosa of upper respiratory tract or conjunctiva Pathophysiology incubation 10-23 days (avg, 14 days) direct contact infected respiratory tract secretions airborne droplets exposure to mucosa of upper respiratory tract or conjunctiva Pathophysiology incubation 10-23 days (avg, 14 days) direct contact infected respiratory tract secretions airborne droplets exposure to mucosa of upper respiratory tract or conjunctiva Pathophysiology incubation 10-23 days (avg, 14 days) direct contact contagious 1-2 days before rash until all lesions crusted over infected respiratory tract secretions airborne droplets exposure to mucosa of upper respiratory tract or conjunctiva Pathophysiology incubation 10-23 days (avg, 14 days) direct contact contagious 1-2 days before rash until all lesions crusted over infected respiratory tract secretions airborne droplets exposure to mucosa of upper respiratory tract or conjunctiva 90% risk of disease after exposure • • Clinical Manifestations mild-moderate in children, more severe in adults short or absent prodrome Clinical Manifestations • mild-moderate in children, more severe in adults • short or absent prodrome • • • • macules g papules g vesicles g pustules g scabs evolves as series of “crops” over 3-4 days concentrated on trunk and head 250-500 lesions Clinical Manifestations • variable severity Clinical issues in pregnancy Clinical issues in pregnancy • VZV in first 20 weeks: • • fetal death, or congenital varicella syndrome: • T1 and T2 • • • • 1-2% risk if mum gets varicella limb hypoplasia cutaneous scarring eye abnormalities CNS damage Clinical issues in pregnancy • VZV in second 20 weeks: • T2 and T3 children can develop inapparent varicella and subsequent zoster earlier in life without extrauterine varicella Clinical issues in pregnancy • VZV peripartum: • T3 • varicella infection can be fatal in the neonate if mother develops varicella 5 days before or 2 days after delivery if mum develops varicella >5 days before and if infant >28 wks GA, severity of disease modified by transplacental maternal IgG antibody Prevention once exposed • Postexposure immunization: • • varicella vaccine, to people without evidence of immunity 12 months or older, within 72 hours of exposure (possibly up to 120 hours) contraindicated in: • • pregnant women immunocompromised patients, including those on high dose daily systemic steroids Prevention once exposed • Passive immunization: • • VZIG/VariZIG, given IM, within 96 hours of exposure decision to give depends on: • • • • likelihood exposed person has no immunity likelihood exposure will lead to infection likelihood infection will lead to complications at risk populations: • • • immunocompromised pregnant women certain neonates (mum develops rash -5 days to +2 days of delivery) Diagnostic Tests Diagnostic Tests • PCR or DFA • • virus culture less • sensitive • sites: • • • • vesicle base saliva or buccal mucosa CSF (PCR) rarely from respiratory secretions • serology: Ig M unreliable significant increase in IgG from acute and convalescent serum for retrospective diagnosis Treatment Treatment • no treatment in otherwise healthy children • consider oral acyclovir in patients at risk of moderate to severe varicella: • • • • • > 12 years chronic cutaneous or pulmonary disorders on long-term salicylate therapy on steroids (short, intermittent, or aerosolized courses) pregnant, esp 2nd and 3rd trimesters Treatment • intravenous acyclovir in immunocompromised patients: • • • on chronic corticosteroids immunodeficient, eg. HIV immune-suppressed, eg. leukemia on chemo Complications • bacterial Complications superinfection of skin lesions • MSK infections (arthritis, osteomyelitis, necrotizing fasciitis) • CNS involvement (acute cerebellar ataxia, encephalitis, stroke) • • • • • • pneumonia glomerulonephritis hepatitis thrombocytopenia sepsis etc. Complications • “The burden of varicella complications before the introduction of routine varicella vaccination in Germany.” • JG Liese, V Grote, E Rosenfeld, R Fischer, BH Belohradsky, R vKries, ESPED Varicella Study Group • Pediatr Infect Dis J 2008;27: 119-124 Complications • prospective review of varicella-related hospital admissions in Germany (which has no universal vaccination) Complications Complications Complications • Reasons for hospitalization: Complications • Types of complications: Complications Complications Complications • permanent sequelae in 15 (1.7%) • • • • • • severe scarring (10) ataxia (1) mitral valve insufficiency from endocarditis (1) visual restriction from retinal necrosis (1) liver transplantation due to liver failure NYD (1) hemiparesis from cerebral infarct (1) Complications • possible permanent sequelae in 78 (8.7%) • • • • • severe scarring (19) ataxia/coordination disorder (17) epilepsy (4) cerebral nerve paralysis (3) other (35) Complications • death in 10 (1.1%) • • • congenital varicella (2) 4 immunocompromised patients (3 with ALL, 1 with IgG deficiency) 4 immunocompetent patients (cardiocirculatory failure from myocarditis, severe bacterial superinfection and sepsis x 2, multiorgan system failure - pneumonia, meningoencephalitis, hemorrhagic complications) Summary • VZV: • still out there • importance of immunization history • multiple complications, often in previously children • preventable! healthy References • • • • American Academy of Pediatrics. Varicella-Zoster Infections. In: Pickering LK, Baker CJ, Kimberlin DW, Long SS, eds. Red Book: 2009 Report of the Committee on Infectious Diseases. 28th ed. Elk Grove Village, IL: American Academy of Pediatrics;2009. (electronic access) Gershon AA. Varicella-Zoster Virus Infections. Pediatr Rev 2008;29: 5-11. Heininger U, Seward JF. Varicella. Lancet 2006;368: 1365-76. Liese JG, Grote V, Rosenfeld E, Fischer R, Belohradsky BH, vKries R, ESPED Varicella Study Group. The burden of varicella complications before the introduction of routine varicella vaccination in Germany. Pediatr Infect Dis J 2008;27: 119-124.