* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download pnh-2
Survey
Document related concepts
Transcript
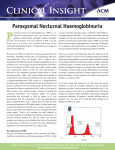
Paroxysmal Nocturnal Hemoglobinuria J. Christian Barrett, MD PATHOPHYSIOLOGY OF PNH Paroxysmal Nocturnal Hemoglobinura • A disease of the hematopoietic stem cell – Non-malignant clonal disease • Defective post-translational processing of glycosylphosphotidylinositol biosythesis – Involves >26 different gene products – Mutations in any of them could potentially lead to PNH phenotype. PIG-A Gene • Acquired somatic mutation of the PIG-A gene – Located on X-chromosome – Involved in the first step of the GPI anchor biosynthesis • The addition of n-acetylglucosamine to the phosphatidylinositol on the cytoplasmic side of the endoplasmic reticulum membrane Glycosylphosphatidylinositol Anchor Glycosylphosphatidyinositol Anchor http://www.sigmaaldrich.com/technical-documents/articles/biology/glycobiology/gpianchored-glycoproteins.html Transport to the Cellular Surface http://www.fbs.osaka-u.ac.jp/organelle-network/eng/research/22/ PNH arises through a block in the biosynthesis of the GPI anchor. PIG-T mutations also described in a patient with a double hit on the PIG-T gene located on chromosome 20—involves the last step of attaching the surface protein to the formed GPI-anchor Lucio Luzzatto Blood 2013;122:1099-1100 ©2013 by American Society of Hematology CD55 and CD 59 • CD 55 – Decay Activating Factor (DAF) • CD 59 – MAC Inhibitory Protein (MAC-IP) – Membrane Inhibitor of Reactive Lysis (MIRL) Noris, M. et al. (2012) STEC-HUS, atypical HUS and TTP are all diseases of complement activation Nat. Rev. Nephrol. doi:10.1038/nrneph.2012.195 Normal State: Protection Against Complement Deposition Lucio Luzzatto, Antonio Maria Risitano, Rosario Notaro Haematologica April 2010 95: 523-526; Doi:10.3324/haematol.2009.017848 Complement-Medicated Hemolysis Lucio Luzzatto, Antonio Maria Risitano, Rosario Notaro Haematologica April 2010 95: 523-526; Doi:10.3324/haematol.2009.017848 Hemolysis-Induced Nitric Oxide Depletion Smooth muscle contraction Vascular constriction systemic HTN pulmonary HTN GI dysmotility Erectile dysfunction Platelet activation Thrombosis formation American Society of Hematology Hematology 2005;2005:544-552 ©2005 by American Society of Hematology PNH and Thrombosis Risk • Most common cause of PNH-related mortality • ~44% of clinical PNH patients have a thrombus • Venous thrombosis most common – Often in unusual sites • Arterial events possible and also increased • Etiology is multifactorial PNH and Thrombosis Risk • Nitric oxide depletion by free HGB – Vasoconstriction – Platelet activation • Complement deposition on platelets – Platelets microparticle release • Increased C5a due to complement activation – Leads to inflammatory cell release of IL-6, IL-8 and TNF-alpha • Decreased GPI-anchored tissue factor pathway inhibitor receptor – Leads to increased coagulation cascade activation • Decreased GPI-anchored plasminogen activator receptor – Leads to impaired fibrinolysis More than Just Complement Disease • • • • Prion Protein (PrP) FcgIII receptor (CD16) -- APCs Tissue factor pathway inhibitor receptor Urokinase-type plasminogen activator receptor Clonal Evolution and Expansion Hypothesis of Clonal Selection and Expansion Bone Marrow Failure States • Association with Aplastic Anemia and MDS – Long appreciated – ? Mechanism – ? Causal relationship PNH Clone in Patients with Bone Marrow Failure British Journal of Haematology Volume 147, Issue 1, pages 102-112, 28 JUL 2009 DOI: 10.1111/j.1365-2141.2009.07822.x http://onlinelibrary.wiley.com/doi/10.1111/j.1365-2141.2009.07822.x/full#f1 Fate of PNH Clone in Patients with Bone Marrow Failure 17% 59% 24% British Journal of Haematology Volume 147, Issue 1, pages 102-112, 28 JUL 2009 DOI: 10.1111/j.1365-2141.2009.07822.x http://onlinelibrary.wiley.com/doi/10.1111/j.1365-2141.2009.07822.x/full#f3 IST did not appear to influence this fate among the 35 AA patients treated compared with the untreated patients DIAGNOSIS OF PNH Clinical Presentation • Intravascular hemolysis – Fatigu,. lethargy, and asthemia – Dyspnea with exertion – Chest pain – Jaundice – Hemoglobinuria Clinical Presentation • Vascular thrombosis – Leg pain and/or edema – Chest pain and/or Dyspnea – Liver failure – Abdominal pain – Headaches Laboratory Investigation • Routine labs – CBC – Hemolysis labs • • • • • Reticulocyte count LDH and fractionated bilirubin Haptoglobin Urine hemosiderin Direct Antigen Test (DAT) – Iron studies • Flow cytometry looking at CD55 and CD59 – RBC and Granulocytes Flow Cytometry Results • Percentage of PNH cells is highly variable High-sensitivity flow cytometric analysis of erythrocytes. Charles Parker et al. Blood 2005;106:3699-3709 ©2005 by American Society of Hematology Flow Cytometry Type II cells Type III cells Type I cells Type I cells Endo et al. Blood 1996;87:2546-2557 Phenotypic Mosaicism: Hypothetical histograms of RBC stained with anti-CD59 Charles Parker et al. Blood 2005;106:3699-3709 ©2005 by American Society of Hematology Flow Cytometry: PMNs vs. RBCs PMNs are more reliably informative Classification of PNH • Classic – Hemolysis • Florid (markedly abnormal LDH often with episodic macroscopic hemoglobinuria) – Marrow • Cellular marrow due to erythroid hyperplasia and normal or near-normal morphology†† – Flow • Large population (>50%) of GPI-AP deficient PMNs – Effectiveness of Eculizumab • Yes Based on recommendations of the International PNH Interest Group(Blood2005;106:3699-3709) Classification of PNH • PNH in the setting of another bone marrow failure syndrome§ – Hemolysis: • Mild (often with minimal abnormalities of biochemical markers of hemolysis) – Marrow • Evidence of a concomitant bone marrow failure syndrome§ – Flow • Although variable, the percentage of GPI-AP deficient PMNs is usually relatively small (<50%) – Effectiveness of Eculizumab • Typically no, but some patients have relatively large clones and clinically significant hemolysis and may benefit from treatment § Aplastic anemia or low risk myelodysplastic syndrome Based on recommendations of the International PNH Interest Group(Blood2005;106:3699-3709) Classification of PNH • Subclinical – Hemolysis • No clinical or biochemical evidence of intravascular hemolysis – Marrow • Evidence of a concomitant bone marrow failure syndrome – Flow • Small (<1%) population of GPI-AP deficient PMNs detected by high-resolution flow cytometry – Effectiveness of Eculizumab • No § Aplastic anemia or low risk myelodysplastic syndrome Based on recommendations of the International PNH Interest Group(Blood2005;106:3699-3709) MANAGEMENT OF PNH Management of Classic PNH • Anticoagulation therapy – NOT ALWAYS effective – Duration is controversial • Complement blockade • Hematopoietic stem cell transplantation Management of Classic PNH • Complement blockade – Eculizumab • Humanized monoclonal antibody • Binds C5 – Administration • IV every 7 days x 5 doses every 14 days Eculizumab Toxicities • Headache – Due to sudden increase in nitric oxide – ~50% with the first dose • Improves with repeated dosing • Life-threatening Neissserial infections – ~0.5%/year (5% after 10 years) – Should vaccinate • Ciprofloxacin prophylaxis x 2 weeks if must urgently start therapy concomitantly with vaccination Complement regulation and eculizumab. Robert A. Brodsky Blood 2014;124:2804-2811 ©2014 by American Society of Hematology What is the Clinical Effect of Eculizumab Therapy? • • • • • • On symptoms of fatigue and QOL? On renal function? On thrombosis? On hemolysis? On marrow failure? On transfusion needs? Overall survival of eculizumab treatment compared with an age- and sex-matched normal population. Richard J. Kelly et al. Blood 2011;117:6786-6792 ©2011 by American Society of Hematology Overall Survival of Patients before and after Eculizumab. Richard J. Kelly et al. Blood 2011;117:6786-6792 ©2011 by American Society of Hematology Blood transfusion requirements in the 12 months before eculizumab therapy and the most recent 12 months on eculizumab treatment in 64 patients. Richard J. Kelly et al. Blood 2011;117:6786-6792 ©2011 by American Society of Hematology PNH Treated with Eculizumab Now often DAT C3+ Lucio Luzzatto, Antonio Maria Risitano, Rosario Notaro Haematologica April 2010 95: 523-526; Doi:10.3324/haematol.2009.017848 What is the Clinical Effect of Eculizumab Therapy? • Effect of Complement Receptor 1 (CR1) polymorphisms? • Effect of C5 mutation c.2654G→A ? Hematopoietic Stem Cell Transplantation • Failure to respond to Eculizumab Bone Marrow Failure States • Treat as you otherwise would – Aplastic anemia • Allogeneic transplantation • Immunosuppressive therapy – Myelodysplasia • Hypomethylating agent • Allogeneic transplantation Prognosis after IST compared between patients with PNH+ and with PNH-. Chiharu Sugimori et al. Blood 2006;107:1308-1314 ©2006 by American Society of Hematology Charles J. Parker Hematology 2011;2011:21-29 ©2011 by American Society of Hematology