* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download L. monocytogenes is gram-positive and rod
Survey
Document related concepts
Quorum sensing wikipedia , lookup
Gastroenteritis wikipedia , lookup
Urinary tract infection wikipedia , lookup
Neonatal infection wikipedia , lookup
Phospholipid-derived fatty acids wikipedia , lookup
Sarcocystis wikipedia , lookup
Infection control wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Marine microorganism wikipedia , lookup
Human microbiota wikipedia , lookup
Triclocarban wikipedia , lookup
Bacterial cell structure wikipedia , lookup
Anaerobic infection wikipedia , lookup
Bacterial taxonomy wikipedia , lookup
Transcript
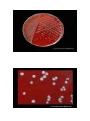
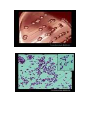
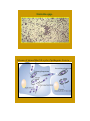
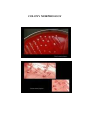
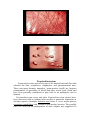
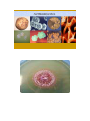
Corynebacterium diphtheriae Corynebacteria are Gram-positive, catalase positive, non-sporeforming, non-motile, rod-shaped bacteria that are straight or slightly curved. Metachromatic granules are usually present representing stored phosphate regions. Their size falls 6 2-micrometers in length and 0.5 micrometers in diameter. The bacteria group together in a characteristic way, which has been described as the form of a "V", "palisades", or "Chinese letters". They are aerobic or facultatively anaerobic, chemoorganotrophs, with a 51–65% genomic G:C content. They are pleomorphic through their life cycle. Diseases The most notable human infection is diphtheria, caused by Corynebacterium diphtheriae. It is an acute and contagious infection characterized by pseudomembranes of dead epithelial cells, white blood cells, red blood cells, and fibrin that form around the tonsils and back of the throat. It is an uncommon illness that tends to occur in unvaccinated individuals, especially school-aged children. Four subspecies are recognized: C. diphtheriae mitis, C. diphtheriae intermedius, C. diphtheriae gravis, and C. diphtheriae belfanti. The four subspecies differ slightly in their colonial morphology and biochemical properties such as the ability to metabolize certain nutrients, but all may be toxigenic (and therefore cause diphtheria) or nontoxigenic. Unusually, the diphtheria toxin gene is actually encoded by a bacteriophage which is found in toxigenic strains, not on the bacterial chromosome itself. Diagnosis For primary isolation, a variety of media may be used: Loeffler agar, Mueller-Miller tellurite agar, or Tinsdale tellurite agar. Sterile cottontipped applicators are used to swab the pharyngeal tonsils or their beds. Calcium alginate swabs may be inserted through both nares to collect nasopharyngeal samples for culture. Following initial isolation, C diphtheriae may be identified as mitis, intermedius, or gravis biotype on the basis of carbohydrate fermentation patterns and hemolysis on sheep blood agar plates . The toxigenicity of C diphtheriae strains is determined by a variety of in vitro and in vivo tests. The most common in vitro assay for toxigenicity is the Elek immunodiffusion test. C. diphtheriae can grow on media with sheep blood with or without beta-hemolysis. Tinsdale agar (TIN) is used for the primary isolation and identification of Corynebacterium diphtheriae. The medium differentiates between C. diphtheriae and diphtheroids found in the upper respiratory tract. This differentiation was based on the ability of C. diphtheriae to produce black (or brown) colonies, surrounded by a brown/black halo. The dark halo is due to the production of H2S from cystine, interacting with the tellurite salt. COLONY MORPHOLOGY Listeria monocytogenes L. monocytogenes is a non-fastidious bacterium growing well on commonly used cultivation media. On blood agar it forms small colonies about 1-2 mm in diameter after 24 hours of cultivation. Colonies are βhemolytic but many strains of L.monocytogenes produce only narrow zones of hemolysis that frequently do not extend much beyond the edge of the colonies. In appearance, they may resemble colonies of Enterococci or some Corynebacteria. L. monocytogenes is gram-positive and rod-shaped. Listeria are known to be the bacteria responsible for listeriosis, They are able to grow in temperatures ranging from 4°C (39°F), the temperature of a refrigerator, to 37°C (99°F), the body's internal temperature. Furthermore, listerosis's deadliness can be partially attributed to the infection's ability to spread to the nervous system and cause meningitis. Finally, Listeria has a particularly high occurrence rate in newborns because of its ability to infect the fetus by penetrating the endothelial layer of the placenta. Vegetables can become contaminated from the soil, and animals can also be carriers. Listeria has been found in uncooked meats, uncooked vegetables, unpasteurized milk, foods made from unpasteurized milk, and processed foods. Listeria is killed by pasteurization and cooking. Listeriosis is a serious infection caused by eating foods contaminated with the bacterium Listeria Monocytogenes. Monocytogenes. This disease affects primarily pregnant women, newborn, and adults with weakened immune systems. This bacterium is too small to be seen without a microscope. Listeria spp. Schema of intracellular life cycle of pathogenic Listeria COLONY MORPHOLOGY Propionibacterium Propionibacterium species are part of the normal bacterial flora that colonize the skin, conjunctiva, oropharynx, and gastrointestinal tract. These non-spore-forming, anaerobic, gram-positive bacilli are frequent contaminants of specimens of blood and other sterile body fluids and have been generally considered to play little or no pathogenic role in humans. Propionibacterium acnes and other Propionibacterium species have, been recovered with or without other aerobic or anaerobic organisms as etiologic agents of multiple infection sites Some P. acnes strains possess synergistic capabilities with facultative and aerobic bacteria. The possible role of P. acnes in the pathogenesis of acne vulgaris was suggested. In addition to its ability to elaborate enzymes such as lipase, protease, and hyaluronidase, and on its ability to activate the complement system and enhance chemotactic activity of neutrophils. Actinomyces Actinomyces (from Greek "actis" ray, beam and "mykes" mucus, fungus) is a genus of the actinobacteria class of bacteria. They are all Gram-positive. Actinomyces are facultatively anaerobic (except A. meyeri, a strict anaerobe). All species grow best under anaerobic conditions. Actinomyces species do not form endospores, and, while individual bacteria are rod-shaped, Actinomyces colonies form funguslike branched networks of hyphae. The aspect of these colonies initially led to the incorrect assumption that the organism was a fungus and to the name "Actinomyces" or ray fungus. Many Actinomyces species are opportunistic pathogens of humans and other mammals, particularly in the oral cavity. In rare cases, these bacteria can cause actinomycosis, a disease characterized by the formation of abscesses in the mouth, lungs, or the gastrointestinal tract. Actinomycosis is most frequently caused by Actinomyces israelii. A. israelii may also cause endocarditis, though the resulting symptoms may be similar to those resulting from infections by other bacterial species. Actinomycetes are Gram-positive organisms. This means they have a thicker layer of peptidoglycan in their cell wall than Gramnegative bacteria. Actinomycetes contain a cell wall. Flagella grows in and on the substrate. Another internal structure is thallus (a tissue like mass that grows in cultures). One more internal structure is mycelium (tangled mass of hyphae that is found in nature). Actinomycetes can be identified by their branching growth pattern that results in large threadlike structures. These filaments may break apart to form rods or spheroidal shapes, called bacillus. Some actinomycetes can form spores. Actinomycetes reproduce by spores. One form of reproduction is Hyphal growth is followed by fragmentation and release of spores. Another form of reproduction is Conidia is when spores produce asexually on aerial fillaments. Actinomycetes produce Streptomycin which is an antibiotic that prodeces... Spectinomycin, Neomycin, Tetracyclines, Chamydias, Rickettsias etc., Nystatin, Erythromycin, Legionella, and Chloramphenicol.