* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download First-Trimester Emergencies: A Practical Approach To Abdominal
Menstrual cycle wikipedia , lookup
Reproductive health wikipedia , lookup
Women's medicine in antiquity wikipedia , lookup
Maternal health wikipedia , lookup
Prenatal development wikipedia , lookup
HIV and pregnancy wikipedia , lookup
Birth control wikipedia , lookup
Dental emergency wikipedia , lookup
Menstruation wikipedia , lookup
Prenatal nutrition wikipedia , lookup
Fetal origins hypothesis wikipedia , lookup
Prenatal testing wikipedia , lookup
Miscarriage wikipedia , lookup
Maternal physiological changes in pregnancy wikipedia , lookup
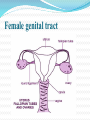
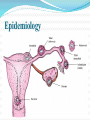
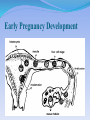
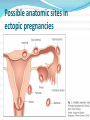
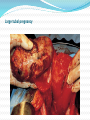
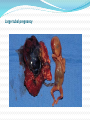
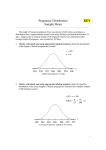
2007.05.31 김의중 Ectopic Pregnancy 목 적 Identify readily available tests: risk-stratify women at risk for ectopic pregnancy List management strategies for treating women with nonviable IUP Describe one reasonable approach to managing the unstable early pregnant woman List U/S findings most suggestive of the D/x of ectopic pregnancy Discuss the clinical utility of the quantitative ß-hCG test and progesterone level 증 례 1주일 전 응급실을 방문한 25세 여자가 심한 복통을 주소로 다시 응급실을 방문을 하였다. 환자의 남편은 병원에 오기 전 복통으로 1차례의 실신을 한 후에 구급차를 불러서 응급실로 왔다고 한다. 환자 clammy & tachycardic 하였고 임신상태처럼 보이지는 않았 다. Systolic BP : 70 mmHg, HR : 130bpm. Her abdomen is diffusely tender. 증 례 Your first thought is the obvious one to any experienced emergency physician—she has a ruptured ectopic pregnancy. Your second thought is, "Who was the idiot who discharged her last week?" As she’s wheeled into the trauma room, you notice that her face looks familiar. Critical Appraisal Of The Literature Kohn et al Retrospective medical record review of 730 women - abdominal pain, vaginal bleeding, or both and a nonzero quantitative ß-hCG. In this cohort, 13% of the women were diagnosed with ectopic pregnancies. Female genital tract Clinical Policies ACEP (American College of Emergency Physicians) - 3 clinical policies in the 1st trimester Abdominal pain, vaginal bleeding, or both. 1. “Clinical Policy for the Initial Approach to Pts Presenting with a C.C. of Vaginal Bleeding. ” - ß-hCG, Rh testing Clinical Policies ACEP (American College of Emergency Physicians) - 3 clinical policies in the 1st trimester Abdominal pain, vaginal bleeding, or both. 2. “Critical Issues for the Initial Evaluation & Mana gement of Pts Presenting with a C.C. of Non-trau matic Abdominal Pain.” Clinical Policies ACEP (American College of Emergency Physicians) - 3 clinical policies in the 1st trimester Abdominal pain, vaginal bleeding, or both. 3. “Critical Issues in the Initial Evaluation & Management of Pts Presenting to the Emergency Department in Early Pregnancy.” - 6 clinical questions ranging from the role of U/S when the ß-hCG < 1000 mIU/mL to the indications for anti-D immunoglobulin Epidemiology Implantation of a fertilized ovum outside the endometrial cavity of the uterus. Occur in up to 2% fallopian tube - 95% of ectopic pregnancies. Ampullary portion ; 80% Isthmus ; 12% Fimbriated end of the tube ; 5% Junction of the fallopian tube and uterus ; 2% interstitial or a cornual ectopic pregnancy. The abdomen, the cervix, and the ovary. Etiology Mucosa Damage - M/C result of tubal infection. S/P tubal surgery Diethylstilbestrol exposure Defects in the fertilized ovum – decreased tubal motility or premature implantation Hormonal factors Pathophysiology 4 possible outcomes from tubal preg. 1. 2. 3. 4. Erode through the muscularis and lamina propria of the tube, resulting in tubal rupture Persist within an intact tube with or without an associated tubal hematoma Abort out of the fimbriated end of the fallopian tube Ectopic pregnancy may spontaneously involute. Intraabdominal hemorrhage may occur in the absence of tubal rupture. Early Pregnancy Development Possible anatomic sites in ectopic pregnancies Large tubal pregnancy Large tubal pregnancy Terminology Threatened Abortion • Abdominal pain or vaginal bleeding without history of passing tissue, closed os, uterus appropriately sized for dates. • 30%-50% of patients classified as having a "threatened abortion" Stovall et al – history and physical examination were used as the primary mode to assess first-trimester vaginal bleeding, almost ½ of the ectopic pregnancies were discharged. Terminology • Inevitable & Incomplete Abortions • “Inevitable abortion" Situation when the cervical os is open but tissue has not yet passed. • “Incomplete abortion " Situation in which tissue has passed but the cervical os remains open, suggesting that products of conception still remain within the endometrial cavity Terminology • “Complete abortion" Situation in which the patient has passed tissue & the closed cervical os. • Clinically useful and is appropriate if definite products of conception are evident. • Frequently mistake blood clots for the products of conception. Terminology • “Missed Abortion” • Prolonged retention of products of conception in the uterus. • Complications Coagulation defects Differential Diagnosis Differential Diagnosis Differential diagnosis of peripubertal and pubertal ovarian masses Gynecologic Ovarian functional masses Ovarian tumors: epithelial, stromal, germ cell tumors Endometriosis/endometrioma Paraovarian/paratubal cysts (embryonic remnants) Ovarian torsion Hydrosalpinx/pyosalpinx Tubo-ovarian abscess Ectopic pregnancy Hematometra (mullerian anomalies, fusion defects) Fibroids (rare) Vaginal/cervical tumor (extremely rare) Gastrointestinal Intestinal duplication Mesenteric cysts Appendiceal abscess Urinary Pelvic kidney Hydronephrosis Wilms' tumor Urachal cyst Other Neuroblastoma ED Evaluation Triage & Initial Management Unstable Patients To a major resuscitation area, start 2 large-bore IV lines, & begin resuscitation with boluses of isotonic saline. Rapid assessment of anemia & confirmation of the pregnancy CBC, type and crossmatch, Rh testing A rapid quantitative pregnancy test The need for blood products Emergent U/S exam & gynecology consultation ED Evaluation Triage & Initial Management Stable Patients Mild pain or bleeding & stable vital signs can typically wait if an exam room is not immediately available Frequent reassessment by the triage nurse ED Evaluation History History Of Present Illness Location, character, onset & severity of the pain. Pain originating from the uterus ; typically midline & crampy Pain originating from the adnexa ; typically unilateral & sharp Review Of Systems Syncope or near-syncope ED Evaluation Past Medical History Outcome of prior pregnancies Past gynecologic surgeries Intrauterine device (IUD) use Prior ectopic pregnancies Infertility treatments History of PID or STD Medications - method of birth control, as well as the use of ovulation induction agents. Protective effects of oral contraceptives Oral contraceptives Decreased risk of endometrial & ovarian cancer Lower risk of benign breast disease & ovarian cysts Decreased risk of major gynecologic problems including PID & ectopic pregnancy, significant menstrual benefits including decreased menstrual flow (and thus anemia) and relief of dysmenorrhea ED Evaluation Physical Examination Vital Signs - assessment of circulation Abdominal Exam. - The location of the tenderness Pelvic Exam Open internal cervical os ; suggestive of the diagnosis of nonviable IUP. ED Evaluation Diagnostic Studies ß-hCG ; one of the most important & accurate lab tests Progesterone; the corpus luteum during the first 8 weeks. > 25ng/mL : strongly associated with the Dx of a viable IUP < 5ng/mL : accurately excludes the Dx of a viable IUP ED Evaluation U/S ; most useful test for evaluating (표 참조) Empty uterus : an empty endometrial cavity Normal sac : anechoic intrauterine fluid collection < 10 mm in mean sac diameter with a regular echogenic border Abnormal gestational sac : anechoic intrauterine fluid collection either > 10 mm in mean sac diameter or with a grossly irregular border Nonspecific fluid : anechoic intrauterine fluid collection < 10 mm in mean sac diameter without an echogenic border Echogenic material : within the endometrial cavity without a defined sac or multiple discrete anechoic collections of varying sizes divided by echogenic septations U/S finding Indeterminate of U/S finding Incidence of ectopic pregnancy Empty uterus 14% Nonspecific fluid 5% Echogenic material 4% Abnormal gestational sac 0% Normal gestational sac 0% ED Evaluation Risk Stratification Combining the Hx, P/Ex, Lab values & U/S findings Rough estimate of the risk of ectopic preg. for a woman with abdominal pain, vaginal bleeding, or both during early preg. Ectopic pregnancy after index PID episode 0, no PID; 1, mild PID; 2, moderately severe PID; 3, severe PID Likelihood Of Ectopic Pregnancy In Women With Abdominal Pain, Vaginal Bleeding, Or Both In Early Pregnancy Higher likelihood of ectopic pregnancy ß-hCG < 1000 mIU/mL Progesterone < 5 ng/mL Empty uterus on ultrasound Adnexal mass on physical examination or U/S Moder ~large amount of free pelvic fluid on U/S Fertility treatments Falling ß-hCG on repeat testing, but < 50% at 48 hours History of PID or other pelvic infection History of tubal ligation History of prior ectopic pregnancy History of intrauterine device (IUD) use Localized, sharp pain with CMT Peritoneal signs Likelihood Of Ectopic Pregnancy In Women With Abdominal Pain, Vaginal Bleeding, Or Both In Early Pregnancy Lower likelihood of ectopic pregnancy ß-hCG > 3000 mIU/mL Progesterone > 25 ng/mL Intrauterine fetus on ultrasound Uterine size appropriate for dates (especially if > 8 week size) Small amount of anechoic pelvic fluid on ultrasound No fertility treatments Rising ß-hCG on repeat testing, > 66% at 48 hours Midline, crampy pain Clinical Pathway Management Of The Hemodynamically Unstable Woman In Early Pregnancy General management Place patient on monitored bed (Class II) High-flow oxygen by facemask (Class III) Prompt vascular access with large-bore peripheral venous catheters (Class II) Bedside qualitative urine pregnancy test if any doubt exists about pregnancy (Class I) Check bedside glucose if mental status is not normal, treat hypoglycemia (Class I) Check bedside hemoglobin if available, identify anemia (Class II) Fluid resuscitate with N/S 1L rapid bolus (Class I) Frequently reassess vital signs (Class II) CBC, blood type and cross and Rh testing (Class II) Clinical Pathway Management Of The Hemodynamically Unstable Woman In Early Pregnancy Ten Pitfalls To Avoid 1. She clearly didn’t have an ectopic preg. because she wasn’t having any pain. : Overreliance on the history & physical exam is one of the great mistakes when evaluating women for suspected ectopic pregnancy. Although it seems intuitive that all patients with an ectopic pregnancy should complain of pain, approximately 10% of patients with a final diagnosis of ectopic pregnancy have no pain at their initial presentation. Ten Pitfalls To Avoid 2. What do you mean she had an ectopic? The radiologist said the ultrasound looked normal! : The description of an empty uterus, no adnexal mass, and no free fluid on ultrasound as being “normal appearing” may be misleading. Both very early pregnancy and ectopic pregnancy can give these findings. Ten Pitfalls To Avoid 3. What do you mean she now has an IUP? Last week she had a complex mass on U/S and her ß-hCG was only 800 mIU/mL. We started her on methotrexate! : Although identification of a complex adnexal mass suggests the presence of an ectopic pregnancy, this finding is not conclusive. It is imperative that the possibility of a viable intrauterine pregnancy be excluded prior to the initiation of methotrexate treatment. Ten Pitfalls To Avoid 4. The ß-hCG is rising appropriately; it couldn’t be an ectopic pregnancy. : Approximately 15% of ectopic pregnancies will have a “normal” rise in their ß-hCG value at the first follow-up blood draw. In fact, in the setting of an empty uterus on U/S , a “normal” ß-hCG rise increases the likelihood of an ectopic pregnancy being present. Ten Pitfalls To Avoid 5. I ruled out an ectopic pregnancy, and she wasn’t bleeding much last week. What do you mean she’s back with profound anemia and hypotension? Her gynecologist should have been able to take care of her. : Many times it is difficult for patients to get in to see doctors in their offices. Assisting patients in arranging follow-up with a specific doctor at a specific location at a given time can help. Ten Pitfalls To Avoid 6. I knew she was bleeding a lot, but what was I supposed to do? I couldn’t take her to the operating room myself! Ten Pitfalls To Avoid 7. I didn’t see any reason to check a quantitative ß-hCG. She said that she had just had a therapeutic abortion a couple days prior to the visit. Ten Pitfalls To Avoid 8. The U/S just showed some retained products of conception, and she wasn’t bleeding too heavily in the ED. I prescribed methergine and ibuprofen and told her to check with her gynecologist in a couple of weeks. Ten Pitfalls To Avoid 9. I know her U/S showed a mass, but her quantitative ß-hCG was low and she really wanted this pregnancy. Ten Pitfalls To Avoid 10. She was undergoing fertility treatment and had severe pain and tenderness. I really thought she had an ectopic pregnancy, but her U/S showed an intrauterine pregnancy, so I sent her home Treatment 3 broad categories of patients 1. Ectopic pregnancies 2. Nonviable IUP 3. Others that are classified simply as "threatened abortions." Treatment Ectopic Pregnancy Surgical Approach Salpingectomy (excision of the affected tube) Tubal preserving surgery Pharmacological Approach Methotrexate - the primary C/Tx agent Inhibits the formation of nucleotides, necessary for DNA and RNA synthesis Treatment Methotrexate Indication 1. Hemodynamically stable 2. Would prefer to avoid surgery 3. Reliable, available for weekly follow-up visits 4. ß-hCG of 3000 mIU/mL or less 5. U/S exam - no fluid outside of the pelvis & mass < 4.0 cm max. diameter ( < 3.5 cm if a fetal heartbeat is present on U/S ). Methotrexate Contraindications 1. 2. Neutropenia, thrombocytopenia Liver dysfunction, kidney disorders (sCr. > 1.5 mg/dL). Methotrexate Treatment Nonviable Intrauterine Pregnancy Emergent D&E of the uterus is mandatory Circulatory compromise Persistent heavy vaginal bleeding Fall in the Hct or signs of infection Surgical Approach D&C - uterine evacuation until the middle of the 20th century D&E - with vacuum evacuation was developed. The D&E is safer and easier to perform than the sharp D&C Treatment Pharmacological Approach Prostaglandin analogs ; Misoprostol - Induce therapeutic abortions. Speeding cervical dilation & initiating uterine contractions, leading to the expulsion of the products of conception. - Contraindications 1. Maternal anemia 2. Crohn’s disease 3. Previous adverse reactions to prostaglandins Treatment Expectant Management - recent studies : some women do well with observation alone Jurkovic et al - 16% of expectantly managed women failed expectant management and required surgical evacuation. 1.2% experienced hemorrhages to require a transfusion Treatment Threatened Abortion F/U with her obstetrician in one week. Although not evidence-based, it is generally recommended that the pt should refrain from douching or intercourse in order to avoid introducing an ascending infection through an open cervical os Special Circumstances Rh-Negative Patients Rh isoimmunization - in ectopic pregnancy or threatened abortion even without fetal loss. Rh status of all symptomatic pregnant patients be checked anti-D Ig be administered to all Rh-negative patients with vaginal bleeding or threatened abortion ACEP committee – the administration of anti-D Ig among women in the 1st trimester with threatened abortion, complete abortion, ectopic pregnancy, or minor trauma. Fertility Treatments Higher risk for heterotopic pregnancy Close consultation with the patient’s gynecologist Cutting Edge & Controversies 1. Who can be safely discharged home from the ED when the initial evaluation is non-diagnostic? 2. Are there better pharmacological agents being developed to treat ectopic pregnancies? 3. What is the best treatment for nonviable IUP? Disposition Discharge From The ED Outpatient gynecologic follow-up: 1. 2. 3. 4. 5. 6. 7. A viable IUP by U/S A nonviable IUP with minimal bleeding & a small volume of intrauterine retained products of conception on U/S An intrauterine gestational sac (NL or abNL) by U/S A progesterone level > 25 ng/mL Crampy, midline, mild pain with an inconclusive U/S evaluation Hemodynamic stability with minimal or no anemia An appropriate rise in ß-hCG when a prior for comparison Disposition Gynecologic Consultation Or Admit 1. 2. 3. 4. 5. A history of fertility treatments Heavy or persistent vaginal bleeding with anemia U/S findings diagnostic or suggestive of ectopic pregnancy. Moderate or large volumes of free fluid in the pelvis on U/S exam. Hemodynamic instability Key Points In Managing 1st Trimester Emergencies 1. Except in rare circumstances, the history and physical 2. 3. 4. 5. exam alone should not be used to exclude ectopic pregnancy. U/S is the best initial test to evaluate the severely symptomatic pregnant pt. The combination of U/S findings and the quantitative ßhCG is useful in stratifying pts with regard to their risk for ectopic preg. Given other indications, the quantitative ß-hCG value is the best predictor of success with methotrexate treatment. In pts with nonviable IUPs, the volume of endometrial contents at U/S is the best predictor of the need for surgical evacuation FIN 감사합니다. Complications of assisted reproductive techniques Ovarian hyperstimulation syndrome: a risk if the ovaries are hyperstimulated (>25 follicles) or the estradiol level is higher than 5000 pg/mL; this risk can be reduced by lowering the gonadotropin dose, using progesterone instead of hCG injections for luteal support, canceling the cycle, and avoiding hCG administration Possible ovarian neoplasm association with use of fertility drugs Multiple gestations: approximately 37% of births resulting from ART, whereas 2% of such births occur in the general population Adverse outcome of pregnancy (22% of clinical pregnancies) ; ectopic pregnancy, spontaneous abortion, induced abortion, or stillbirth Bleeding: rare; includes vaginal blood loss and intraperitoneal bleeding resulting from inadvertent laceration of vessels with the retrieval needle Bowel or ureteral injury with the aspiration needle Infection: although tubo-ovarian abscess formation has been reported following transvaginal oocyte aspiration & transcervical embryo transfer , infection is now rare with the use of prophylactic antibiotics Anesthetic complications: resulting from conscious intravenous sedation; includes drug reaction, apnea, cardiac arrest, and need for intubation Reproductive causes of abnormal uterine bleeding Early miscarriage Threatened abortion Incomplete abortion Missed abortion Ectopic pregnancy Retained products of conception 1. Ectopic pregnancy: a. is defined as the implantation of a fertilized ovum outside the endometrial cavity of the uterus. b. may be more common than is reported because of advances in the diagnosis and treatment of ectopic pregnancy in the past few decades, a substantial decrease in inpatient hospital treatment for ectopic pregnancy, and an increase in multiple outpatient visits for a single ectopic pregnancy. c. usually occurs in the fallopian tube. d. is usually due to mucosal damage, which is usually due to tubal infection. e. all of the above. 2. Heterotopic pregnancy: a. is the simultaneous occurrence of at least one intrauterine and at least one ectopic pregnancy. b. are quite common in naturally occurring pregnancies. c. are relatively rare with ovulation induction and in vitro fertilization as compared to naturally occurring pregnancies. d. can be ruled out by visualization of an intrauterine pregnancy 3. ß-hCG production begins: a. about six days after fertilization. b. about two weeks after fertilization. c. about three weeks after fertilization. d. about five weeks after fertilization 4. Abnormal pregnancies, including ectopic pregnancies, are very likely when the ß-hCG is greater than 1000 mIU/mL and a gestational sac cannot be visualized on ultrasound. a. True b. False 5. Because patients frequently mistake blood clots for the products of conception, the passage of true products of conception should not be made by history alone. a. True b. False 6. Which of the following features of a patient’s past medical history presents the greatest risk for ectopic pregnancy in a patient in early pregnancy? a. Intrauterine device use b. Prior ectopic pregnancies c. Tubal ligation d. Infertility treatments e. A history of pelvic inflammatory disease 7. Which of the following is/are true regarding abdominal pain in the first trimester? a. Pain originating from the uterus is typically midline and crampy. b. Pain originating from the adnexa is typically unilateral and sharp. c. If hemorrhage into the pelvis from an adnexal process has occurred, the pain often becomes bilateral. d. Pain originating from the bladder is midline in location and often associated with dysuria. e. All of the above. 8. Which of the following ultrasound results is associated with the greatest risk for ectopic pregnancy? a. Empty uterus b. Normal sac c. Abnormal gestational sac d. Nonspecific fluid e. Echogenic material