* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Unit 3-6 Urinary System Notes File
Survey
Document related concepts
Transcript
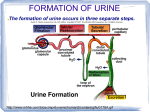
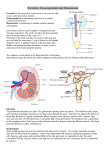
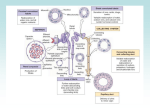
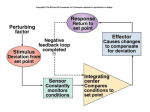
I. Osmoregulation = Solute (salts) / Solvent (H2O) Balancing • • • • Physiological systems of animals operate in a fluid environment (cells are in liquid) Relative concentrations of water and solutes must be maintained within fairly narrow limits Osmoregulation regulates solute concentrations and balances the gain and loss of water Controls movement of solutes and/or solvents between internal fluids and the external environment Examples: • Freshwater animals – Too much water dilutes solutes – Have adaptations that reduce water uptake and conserve solutes (excrete less Na +) • Desert and marine (i.e. saltwater) animals face desiccating environments that can quickly deplete body water Homeostasis of body fluids • Maintain the salt (solute) concentration • Maintain water concentration • Maintain the osmotic concentration Also: • Maintain H+ concentration (blood pH) • Excrete waste products (e.g. nitrogenous wastes) II. Excretion of Wastes An animal’s nitrogenous wastes reflect its phylogeny and habitat • The type and quantity of an animal’s waste products may greatly affect its water balance • Among the most important wastes are nitrogenous breakdown products of proteins and nucleic acids ammonia (NH3) • Some animals convert toxic ammonia (NH3) to less toxic compounds prior to excretion Requires large volumes of urine Small volumes of urine but energy expended to produce Ammonia • Animals that excrete nitrogenous wastes as ammonia need lots of water • They release ammonia across the whole body surface or through gills Urea • The liver of mammals and most adult amphibians converts ammonia to less toxic urea • The circulatory system carries urea to the kidneys, where it is excreted • Conversion of ammonia to urea is energetically expensive; excretion of urea requires less water than ammonia Uric Acid • Insects, land snails, and many reptiles, including birds, mainly excrete uric acid • Uric acid is largely insoluble in water and can be secreted as a paste with little water loss not urine • Uric acid is more energetically expensive to produce than urea Transport Epithelia • specialized epithelial cells that regulate solute movement • essential components of osmotic regulation and metabolic waste disposal • arranged in complex tubular networks Example: ialt glands of marine birds remove excess sodium chloride from the blood Protonephridia: The Flame-cell system of planaria • network of dead-end tubules connected to external openings • smallest branches capped by a cellular unit called a flame bulb • These tubules excrete a dilute fluid and function in osmoregulation Metanephridia Each segment of earthworm has pair of open-ended metanephridia: collect coelomic fluid and produce dilute urine for excretion Malpighian Tubules • Arthropods • Insects produce a relatively dry waste matter, an important adaptation to terrestrial life Excretory Processes Most excretory systems produce urine by refining a filtrate derived from body fluids Key functions of most excretory systems: – Filtration: pressure-filtering of body fluids – Reabsorption: reclaiming valuable solutes – Secretion: adding toxins and other solutes from the body fluids to the filtrate – Excretion: removing the filtrate from the system Kidney Functions 1. Filters 200 liters of blood daily toxins, metabolic wastes, and excess ions leave the body in urine 2. Regulate volume and chemical makeup of the blood 3. Maintain the proper balance between water and salts, and acids and bases Other Renal Functions 4. Gluconeogenesis during prolonged fasting 5. Production of renin to help regulate blood pressure and erythropoietin to stimulate RBC production 6. Activation of vitamin D The Nephron Nephrons are the structural and functional units that form urine Two main parts 1. Glomerulus: a tuft of capillaries 2. Renal tubules: • Glomerular (Bowman’s) capsule –cup-shaped end that completely surrounds the glomerulus - Renal corpuscle – the glomerulus and its Bowman’s capsule • Proximal Convoluted Tubules • Loop of Henle • Distal Convoluted Tubues • Collecting Duct (technically not part of nephron) Capillary Beds of the Nephron Every nephron has two capillary beds 1. Glomerulus - Each glomerulus is: • Fed by an afferent arteriole • Drained by an efferent arteriole 2. Peritubular capillaries or vasa recta • Arise from efferent arterioles • low-pressure & porous • Cling to adjacent renal tubules • Empty into the renal venous system Peritubular capillaries Vasa recta Filtration: Blood pressure forces fluids and solutes out of the glomerulus into the renal tubules Tubular Reabsorption process whereby most tubule contents are returned to the blood Transported substances move through three membranes Luminal and basolateral membranes of tubule cells Endothelium of peritubular capillaries Only Ca2+, Mg2+, K+, and some Na+ are reabsorbed via paracellular (inbetween cells) pathways Sodium Reabsorption: Primary Active Transport Na+ enters the tubule cells at the luminal membrane, because of conc. gradient derived from Na+-K+ ATPase pump - sodium actively transported out of the tubules From there it moves to peritubular capillaries due to: • Low hydrostatic pressure (not much water in capillary) • High osmotic pressure of the blood (relatively low amounts of salts in blood) + Na reabsorption provides the energy and the means for reabsorbing most other solutes Reabsorption by PCT Cells - Site of most reabsorption • 65% of Na+ and water, All nutrients, Ions, Small proteins Loop of Henle • Descending limb: H2O • Ascending limb: Na+, K+, Cl DCT and collecting duct - Reabsorption is hormonally regulated • Ca2+ (regulated by PTH) • Water (regulated by ADH) • Na+ (regulated by aldosterone and ANP) Tubular Secretion Reabsorption in reverse –substances move from peritubular capillaries or tubule cells into filtrate Tubular secretion is important for: Disposing of substances not already in the filtrate Eliminating undesirable substances (urea and uric acid) Ridding the body of excess potassium ions Controlling blood pH The loop of henle and collecting duct form a complex countercurrent system Countercurrent trades osmolarity ie- [NaCl] (NaCl and H2O) In the descending loop H2O leaves Increasing Osm (conc) In the ascending loop NaCl leaves Decreasing Osm (conc) With a small amount of active transport (energy), a lot of H2O & NaCl can be reabsorbed passively (without energy consumption) In the collecting duct H2O leaves Increasing Osm (conc) Nonreabsorbed Substances A transport maximum (Tm): Reflects the number of carriers in the renal tubules available Exists for nearly every substance that is actively reabsorbed When the carriers are saturated, excess of that substance is excreted Substances are not reabsorbed if they: Lack carriers Are not lipid soluble Are too large to pass through membrane pores Urea, creatinine, and uric acid are the most important nonreabsorbed substances DCT and collecting duct - Reabsorption is hormonally regulated • Ca2+ (regulated by PTH) • Water (regulated by ADH) • Na+ (regulated by aldosterone and ANP) -ADH Juxtaglomerular Apparatus (JGA) ↑ Blood NaCl or ↓BP ↑ renin ↑ ADH +ADH Antidiuretic hormone (ADH) inhibits diuresis (urine ouput) This equalizes the osmolality of the filtrate and the interstitial fluid In the presence of ADH, 99% of the water in filtrate is reabsorbed Diabetes Insipidus – inability to produce ADH Diuretics Chemicals that enhance the urinary output include: Any substance not reabsorbed Substances that exceed the ability of the renal tubules to reabsorb it Substances that inhibit Na+ reabsorption Osmotic diuretics include: High glucose levels – carries water out with the glucose – Diabetes Mellitus Alcohol – inhibits the release of ADH Caffeine and most diuretic drugs – inhibit sodium ion reabsorption Lasix and Diuril – inhibit Na+-associated symporters Urine Urine is 95% water and 5% solutes Nitrogenous wastes: urea, uric acid, and creatinine Other normal solutes include: Sodium, potassium, phosphate, and sulfate ions Calcium, magnesium, and bicarbonate ions Color and transparency • Clear, pale to deep yellow (due to urochrome) - Concentrated urine has a deeper yellow color • Drugs, vitamin supplements, and diet can change the color of urine • Cloudy urine may indicate infection of the urinary tract Odor • Fresh urine is slightly aromatic • Standing urine develops an ammonia odor • Some drugs and vegetables (asparagus) alter the usual odor pH • Slightly acidic (pH 6) with a range of 4.5 to 8.0 - Diet can alter pH Specific gravity (density, water = 1) • Ranges from 1.001 to 1.035 (means more solutes in it) • Is dependent on solute concentration Renal Clearance The volume of plasma that is cleared of a particular substance in a given time Renal clearance tests are used to: Determine the Glomerular Filtration Rate (GFR) Detect glomerular damage Follow the progress of diagnosed renal disease For any substance freely filtered and neither reabsorbed nor secreted by the kidneys (e.g., inulin), RC = GFR = 125 ml/min (~2%) If RC < 125 ml/min (2%), the substance is reabsorbed If RC = 0, the substance is completely reabsorbed If RC > 125 ml/min (2%), the substance is secreted (most drug metabolites)