* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download File - Developing Anaesthesia
Survey
Document related concepts
Transcript
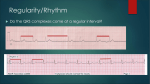
PALPITATIONS “The Night Alarm: The Advance”. Oil on canvas, Charles West Cope, 1871, Royal Academy of Arts, London PALPITATIONS Introduction Patients usually complain of palpitations when they become aware of their own heartbeat. This symptom is a very common presentation to the ED. The commonest cause is ectopic atrial and/ or ventricular beats. More serious causes may be due to non-sustained or sustained tachyarrhythmias. Bradyarrhythmias are not usually perceived as palpitations, and if symptomatic, syncope, near syncope or dizziness will be the more likely presenting symptom. ED assessment will be primarily aimed at distinguishing a benign cause from a more serious cause. Management and disposition of the patient who presents with palpitations will depend on: ● The cause of the symptoms ● The severity of the symptoms ● The index of suspicion for a more serious underlying pathology, as well as the risk profile of the patient. Pathophysiology In general terms the causes to consider include: 1. Benign ectopic beats, (atrial or ventricular): Causes may include: ● Anxiety (very common) ● Emotional states ● Excessive caffeine, (tea as well as coffee) More serious causes of ectopics or tachyarrhythmias may include: 2. Hypoxia/ hypercarbia 3. Drug induced: ● Illicit, (eg amphetamines, cocaine) ● ● Medicinal, for example: ♥ Digoxin in particular, (ectopics or tachyarrhythmias may indicate toxicity) ♥ Any sympathomimetic agent. Toxins/ poisons, for example: ♥ Smoking, (nicotine) ♥ Aconite ♥ Chloral hydrate 4. Ischaemic heart disease or an acute coronary syndrome: 5. Electrolyte disturbance: 6. ● Hyperkalemia/ hypokalemia ● Magnesium, Calcium disturbances less commonly. Thyrotoxicosis Clinical Assessment Some causes of palpitations are obviously “malignant”, (VT for example) Others causes may seemingly not be, such as atrial or ventricular ectopics, hemodynamically stable SVT, however these must also be interpreted in the light of the underlying cause as well as the cardiovascular risk profile a patient has. Important points of history: 1. 2. Establish what the patient means by “palpitations”: ● It is important to establish precisely just what a patient means by “palpitations”, as it is not a clearly defined term, and so may mean different things to different (lay) people. Strictly it is an abnormal sensation or awareness of one’s heartbeat. 1 ● Not uncommonly patients may label their symptoms as “palpitations”, but on careful questioning it may not be arrhythmias that they are describing. Establish the exact nature of the patient’s presenting “palpitations”: Ask about: 3. ● Extra-beats, (suggests ectopic beats) ● Fast and regular, suggests SVT, or atrial flutter, or more seriously VT ● Fast and very irregular (sometimes described as “starting and stopping”), suggests AF Time course: ● 4. 5. eg: Sustained, recurrent, frequent or occasional. Associated symptoms, in particular: ● Chest pain, (ACS, PE, pericarditis) ● Shortness of breath ● Syncopal or pre-syncopal features Risk profile: In particular for: ● Cardiovascular: ● 6. ACS, documented CAD on angiography, poor left ventricular function, are all important considerations Family history: A family history of sudden cardiac death at a young age A family history of an electrophysiological cardiac disorder with familial associations such as WPW, Brugada’s syndrome, ARVC, prolonged QT syndromes. Drugs, including: ● Medications ● Illicit Drug use ● Smoking ● Excessive caffeine (tea as well as coffee). Important points of examination: 1. Assess all vital signs, (not merely the pulse rate), and including pulse oximetry. 2. Cardiac auscultation, for murmurs in particular indicating a possible valvular lesion. Further points of examination will be directed by the index of suspicion for any given specific pathology Investigations 1. ECG: ● Look to document any arrhythmia, which may be the cause of the palpitations ● Look for evidence of possible myocardia ischemia ● Look for evidence of hypokalemia or hyperkalemia ● Look for evidence of an underlying electrophysiological pathology, such as: ♥ WPW ♥ Brugada’s syndrome ♥ Prolonged QT interval ♥ Epsilon waves, (ARVC) After an ECG and full clinical assessment of the patient, no further investigations may be necessary. The degree of subsequent investigation will depend on the nature of the associated symptoms, the patient’s risk profile, and the overall clinical suspicion for a serious underlying pathology. The following may need to be considered: Blood tests: 1. FBE: ● 2. Anaemia U&Es/ glucose: 3. ● In particular look for hypokalemia or hyperkalemia ● Magnesium/ Calcium, (according to index of suspicion for an abnormality in these, uncommon causes). Troponin I: ● 4. TFTs: ● 5. If an ACS is suspected Hyperthyroidism may tachyarrhythmias. initially present with ectopics and/ or Serum digoxin: ● If digoxin toxicity is suspected. CXR: This is not routinely necessary in all cases. It should be considered when more serious underlying pathology is suspected. ● In particular if there is serious associated symptoms such as shortness of breath, chest pain or syncope. ● Look for cardiomegaly, suggestive of a cardiomyopathy Management Management and disposition of the patient who presents with palpitations will of course depend on the cause of the symptoms, the severity of the symptoms, and/ or the index of suspicion for a more serious underlying pathology. In general management terms: 1. Treatment of the underlying cause when known: ● 2. Tachyarrhythmias: ● 3. Eg: Digoxin toxity, thyrotoxicosis, hypokalemia Treat as appropriate, (see separate guidelines for individual arrhythmias). Benign ectopic activity: A benign aetiology is likely if: ● Occasional atrial ectopic or unifocal ventricular ectopics. (Ventricular R on T, multifocal, or salvo ectopic activity is more concerning however and will require further observation/ investigation, see also PVC guidelines). ● There is no obvious underlying pathology, (such as drug toxicity) ● The patient is not clinically compromised Patients with benign ectopic activity can usually be reassured and discharged home for review by their GP. 4. 5. Ectopic activity in high risk patients: ● Here the significance of ectopic activity is more concerning ● Each individual case needs to be assessed on its merits but the threshold for admission and a further period of observation and / or investigation should be low. Palpitations not documented: Not uncommonly a patient will present a complaint of palpitations, which have resolved and so are not able to be documented on 12 lead ECG or on continuous ECG monitoring. If no obvious cause can be determined on clinical assessment and initial investigation in the ED, then a decision on the best disposition plan needs to be formulated. Again each case must be assessed on its merits, but in general terms: Probable benign cause: ● If a benign cause is suspected, the patient can be reassured and discharged. ● If symptoms are frequent, an outpatient holter monitor may be considered, to document the nature of the patient’s symptoms, or indeed to establish if an arrhythmia is the cause of the patient’s symptoms at all Possible malignant cause: ● A more malignant cause should be suspected when: ♥ Patients have cardiomyopathy) ♥ There is a family history of sudden cardiac death and/ or known electrophysiological disorders. ♥ Significant associated symptoms, such as syncope, near syncope or chest pain significant cardiac disease, (ischemic, Even in seemingly well patients, it is best to admit patients in high risk categories for a period of ongoing monitoring. There is no place for example, for elective out patient holter monitoring in cases where the (presumed) arrhythmia is significant enough to cause a patient to collapse. The arrhythmia may be a lifethreatening one such as VT, (see also syncope guidelines). References 1. Talley N.J, O’Conner S. Clinical Examination, 3rd ed 1996, p.29. Dr J. Hayes January 2010