* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download GBCA CPD notes presentation version 2016 DM
Survey
Document related concepts
Transcript
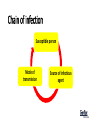
• Wendy Davis • Dip Carbon Management, Swinburne University, Melbourne • MBA (executive), Harvard Business School, Boston • M Ad Ed (adult workplace education), UTS, Sydney • B App Sci (medical microbiologist), RMIT, Melbourne Facilities – protecting your assets and minimising hospital/facility acquired infection Learning outcomes – Health Facilities At the end of this session you will be able to… Systematically identify areas of High infection control requirements High and medium horizontal impact risk & understand why this is critical Learning outcomes – Health Facilities At the end of this session you will be able to… Design interiors to Withstand the daily inundation of collisions Minimise the opportunity for hospital/facility acquired infections & understand why this is critical and how they are related Learning outcomes – Health Facilities At the end of this session you will be able to… Apply a cost benefit approach to design materials Discuss the impact financial and other of hospital acquired infection Justify reduced operational costs vs capex & understand why this is critical Importance of high infection control requirements. Hospital - acquired = nosocomial INFECTIONS • Pertaining to or originating in a hospital The most common complication affecting patients in hospital • Unnecessary pain and suffering for patients and families • Prolong hospital stays • Costly to the health system www.health.gov.au/internet/main/publishing.nsf/Content/Glossary#n Accessed Dec 2015 Challenges • Normal bacteria - ‘hospital’ strains of bacteria that are resistant to antibiotics “ensure consistent cleaning and disinfection of surfaces in close proximity to the patient and those likely to be touched by the patient, staff and visitors” www.nhmrc.gov.au/_files_nhmrc/publications/attachments/cd33_infection_control_healthcare_140616.pdf. Accessed Dec 2015 You might have heard of these… • MRSA, Golden Staph, MRSE (MR = methicillin resistant) • VRE • Clostridium difficile • MRO (M = multi) • SARS, • Ebola • Aspergillus • Gastro. causing viruses – Norovirus • Evolving influenza virus Hospital acquired infections 200,000 reported in Australia in 2010 (very under reported) People die Chain of infection Susceptible person Mode of transmission Source of infectious agent Risk of infection accessed 2 Mar 2016 (http://www.nhmrc.gov.au/book/australian-guidelines-prevention-and-control-infection-healthcare-2010/b4-1-1-classifying-proce Highlight in yellow, areas of high infection risk – see handout Minimise the opportunity for hospital acquired infections • Best protection against infection is intact skin • Similarly best way to protect against bacteria/viruses in the environment is to minimise the opportunity for reservoirs • Minimise cracks/damage/joins/pooling of water Design interiors to Minimise high and medium horizontal impact risk Withstand collisions, scrapes, and scratches Design interiors to • Withstand collisions, scrapes and scratches. High impact high traffic areas CORNER • Plan 2.3 Corner protection - remember we want to maintain the integrity of the “barrier”(just like skin). • So doors to operating theatre particularly those within the isolated theatre space • High visibility, and high use..patients in wheel chairs/wheeling drips etc.. • This will be pretty easy to see when you walk around the existing facility – just look for the bumps and scratches. Find the high profile - high infection risk – high visibility to public. Obviously it would be easier to just do all…but cost effectiveness is important. Nord Parisien Private Hospital - Sarcelles (95) flu-like human metapneumovirus (hMPV) • Families blame hospital for four deaths at Herberton, North Queensland • January 30, 2016 1:00amPeter MichaelThe Courier-Mail • FAMILIES believe the botched handling of a sick patient is to blame for a deadly virus outbreak that “swept like wildfire” through an aged-care facility in far north Queensland. • Four patients died and eight more were infected as the flu-like illness took a lethal stranglehold at the public hospital in Herberton, 90 minutes southwest of Cairns. • Doctors, nurses, patients and family of victims spoken to by The Courier-Mail expect a top-level probe will reveal how “Patient Zero”, the index case, was not put into an isolation ward nearly three weeks ago. • In a fatal mistake, it is understood a sick patient was transferred from another hospital and placed into a general ward with “very elderly, frail, and vulnerable patients in poorly ventilated rooms”, sources said. Friday, Mar 4th 2016 Gastric flu outbreak spreads in Britain Britain is in the grip of a gastric flu outbreak which has spread from hospitals in Scotland to the south coast, health chiefs said today. Levels of the virus, which has already affected 12 hospitals in Scotland, are higher than those recorded in the past, said the Public Health Laboratory Service. The number of people struck down with the viral infection on hospital wards was today expected to rise amid reports of the bug in Manchester, Hertfordshire, Sussex, Dorset and Cornwall. There was also a similar case in Birmingham earlier this month. So far, Glasgow's Victoria Infirmary has been worst hit with 283 patients and staff hit by the illness. It has forced emergency admissions to the hospital to be diverted to the city's Southern General Hospital until further notice. How long do bacteria/viruses/fungi live outside of humans? MRSA can survive for days to weeks on hard surfaces C.difficile has survived for 5 months Norovirus can survive for weeks or months Aspergillus http://www.nhs.uk/chq/Pages/how-longdo-bacteria-and-viruses-live-outside-the-body.aspx Health care examples • Airborne fungal spores eg. Aspergillus sp– indoor and outdoor sources in high-risk patients. • Bird droppings, soil, contaminated fire proofing material, damp timber and plaster (particularly particle board) • Building and maintenance activities disturb these reservoirs and can send millions of spores throughout the health care facility Example • Construction related Nosocomial infections for Hospitalized patients: Decreasing the Risk of Aspergillus, Legionella and Other Infections cites 25 outbreaks of nosocomial Aspergillus sp infections over 20 year period, 106 deaths. • These deaths were either suspected or confirmed as being caused by construction activity Canada Communicable Disease Report July 2001 http://publications.gc.ca/pub?id=9.559516&sl=0 National Health and Medical Research Council – accessed on line Feb 2015 2010 How is this playing out in health - USA • Oct 2008 Medicare decline payments for 8 conditions that could be avoided if “the hospital followed preventative procedure or common sense precautions”. • 3 of these are Hospital Acquired Infections Infection prevention • This responsibility applies to everybody working and visiting a healthcare facility, including administrators, staff, patients and carers. • Successful approaches for preventing and reducing harms arising from HAIs involve applying • a risk-management framework to manage ‘human’ and ‘system’ factors associated with the transmission of infectious agents. 2009 figures 2009 • 2 million bed days per year in Australia lost to Hospital Acquired Infection So what? Direct effects during hospital stay Increase length of stay Diagnosis and treatment cost increase After discharge from hospital Health – care services used more intensively Pharmaceuticals required to treat infection Indirect effects Patient/carers miss out on normal productive activities Reputation of hospital damaged Risk of litigation Apply a cost benefit model to the selection of design materials • Cost of poor aesthetics - priceless?/missed opp/’bad press’ • Cost of wall repair? /Disruption of normal usage?/ how many hospital administrators does it take to repair a wall…involvement of engineer, tradesperson, nursing unit manager, operations manager, ward staff, environmental services staff, patients, visitors, clinicians… • How frequently do they paint? Should they paint? What’s the cost? • Cost to the community of increased chance of hospital acquired infection Impact of overall infection rates of 1% on bed availability (days) (2004-2005) Graves, Nicholas and Halton, Kate A. and Paterson, Davis and Whitby, Michael (2009) The economic rationale for infection control in Australian hospitals. Healthcare Infection, 14 (3). pp. 81-88. What if we could decrease by 1%? • 1% increase means loss of > 150,000 bed days nationally (2004-2005) • 1% decrease means increase of 150,000 bed days nationally AT LEAST • Total Loss of approx. 2 million bed days nationally (2009) • What is it in 2016? LH PHOTO LESS THEN 12 MONTHS OLD Chipping and caps see circle LHS poor RHS correct QUIZ • Multiple choice. 7 Questions.