* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Fitting challenge for ocular surface that has undergone
Survey
Document related concepts
Transcript
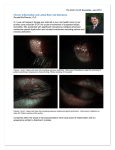
Contact lens fitting challenge post reconstructive surgery with corneal limbal stem cell autograft and amnionic membrane transplant Eva Duchnowski, O.D., Heidi Wagner, O.D., M.P.H., F.A.A.O Nova Southeastern University College of Optometry Abstract: After undergoing ocular surface reconstruction for nonhealing ulcer, a MiniScleral Design (msdtm) contact lens is used on this irregular cornea to maximize patient’s visual acuity and aid in ocular surface healing. I. Case History - A 26-year-old black female was referred from a tertiary health care center for specialty contact lens fitting, OS. - Chief complaint: Constant tearing, sensitivity to light, and reduced vision, OS. - Ocular History: Patient was involved in a car accident which resulted in a blow out fracture and muscle entrapment OS secondary to deployed airbag and fire extinguisher explosion. Patient underwent orbital floor repair with metal plates followed by limbal stem cell transplant (LSCT) form OD to OS and amnionic membrane transplant (AMT) OS for nonhealing ulcer. - Medications: No known allergies to medications; patient is using 1 gtt Vigamox® (Alcon Laboratories, Fort Worth, TX) i.d. OS. II. Pertinent findings - Entering Distance Visual Acuity: without correction OD 20/20 and with unknown soft contact lens power OS 20/60 pinhole to 20/40, OU 20/25 - Unremarkable confrontation fields and extra-ocular muscle testing - Pupils OD equal round and reactive with negative afferent pupillary defect (APD); OS difficult to evaluate due to corneal haze but negative APD by reverse - Refraction OD +0.75 DS best corrected visual acuity (BCVA) 20/20 and OS +3.00 DS BCVA 20/30 - Observations: Excessive tearing OS and left upper lid ptosis with enophthalmos - Biomicroscopy examination OS revealed moderate corneal haze; the corneal epithelium was clear to lissamine green. Sodium fluorescein demonstrated negative pooling inferior temporal. Corneal neovascularization and mild diffuse injection were also noted. 1 III. Differential Diagnosis - Reduced visual acuity secondary to uncorrected refractive error, irregular cornea, and/or corneal compromise - Non-specific ocular surface inflammation - Structural or architectural disruption to the lacrimal drainage apparatus IV. Diagnosis and Discussion - Reduced visual acuity secondary to: o Uncorrected hyperopic refractive error o Irregular astigmatism - Epiphora secondary to: o Non- specific ocular surface inflammation o Structural or architectural disruption to the lacrimal drainage apparatus - Amnionic membrane transplant is a useful adjunct to LSCT in an attempt to promote healing.1 - Amnionic Membrane is used in ocular surgery, primarily in ocular surface reconstruction because of its relatively immunologically inert nature and unique matrix component.2 - Amnionic Membrane facilitates epithelialization , reduces tissue inflammation , neovascularization in corneal stroma, and scarring.3 - Little is known about the long term-results of LSCT for ocular surface reconstruction, however, good eyelid closure and good tear film layer are thought to be important components for successful limbal stem cell transplantation.4 - It has been documented that spontaneous lacrimal punctual occlusion is a very rare complication after stem cell transplantation.5 V. Treatment and Management - Gas-permeable scleral lens vs hydrophilic bandage lens o Mini-Scleral Design contact lens (Blanchard Labs, Inc.) was used to provide tear film reservoir for the reconstructed ocular surface. - Co-management with the referring physician VI. Conclusion - Patients who have undergone reconstructive ocular surface procedures such as limbal stem cell autograft and amnionic membrane transplant present a fitting challenge to contact lens practitioners. Further study is merited. 2 REFERENCES 1. Cauchi P, Ang GS, Azuara-Blanco A, Burr JM. A Systematic Literature Review of Surgical Interventions for Limbal Stem Cell Deficiency in Human. American Journal of Ophthalmology. 2008; 146(2): 251-259. 2. Skorin L. Amnionic membrane as ophthalmic medical, surgical tool. Primary Care Optometry News. September 2007. 3. Schwan B. Human Amniotic Membrane Transplantation For The Treatment of Ocular Surface Disease. Jacksonville Medicine 2002: 53(6) Available at http://www.dcmsonline.org/jax-medicine/2002journals/augsept2002/amniotic.htm Accessed August 11, 2008. 4. Santos M, Gomes J, Hoflinf-Lima AL, Rizzo L, Romano A, Belfort R. Survival Analysis of Conjunctival Limbal Grafts and Amniotic Membrane Transplantation in Eyes With Total Limbal Stem Cell Deficiency. American Journal of Ophthalmology 2005: 223.e1223.e9. 5. Kamoi, Mizuka, Ogawa, Yoko, Dogru, Murat, Uchino, Miki, Kawashima, Motoko, Goto, Eiki, Mori, Takehiko, Okamoto, Shinichiro, Shimazaki, Jun and Tsubota. Spontaneous Lacrimal Punctal Occlusion Associated with Ocular Chronic Graft-versus-Host Disease. Current Eye Research 2007; 32(10): 837 — 842. 3