* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Cracking-the-Case- Quick-Easy-OMT-in-a-Nutshell-by
Survey
Document related concepts
Transcript
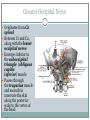
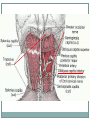
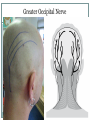
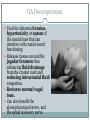
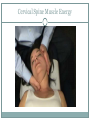
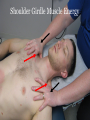
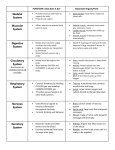
Cracking the Case: Quick, Easy OMT in a Nutshell JESSICA KELNER, DO BRIAN BROWNING, DO FAMILY MEDICINE NEUROMUSCULAR MEDICINE Today’s lecture 3 musculoskeletal cases Differential Diagnosis Documentation and Billing for OMT Pertinent anatomy and special tests 3 OMT treatments for each case Lab after each case Case 1 - HPI 35 year old female c/o intermittent progressively worsening headaches x 1 month. 3-4x a week, worse when she is stressed, better with lying down and closing her eyes Headaches start in the back of her head on the right and radiate around toward the back of her right eye. Pain is “achy” and “sharp” behind her eye, rates them as a 7/10. Associated discomfort on right side of her neck. Tried taking ibuprofen and Excedrin which helps for an hour or two. Case 1 She denies recent head trauma. No association with menstruation ROS: +headache, +right sided neck pain, denies numbness or tingling, denies blurry vision,+ Light sensitivity when she gets the headaches. denies N/V/D/F, denies weakness, denies fatigue All other ROS are negative Medical History Medical History: seasonal allergies, no past history of headaches or motion sickness as a child. Surgical History: none Medications: zyrtec 10mg during allergy season, ibuprofen 600mg every 6 hours as needed for headache Family History: Mom – headaches, HTN Social History: works as a secretary, drinks 2 cups of coffee/day, processed food diet, no exercise, non smoker, lives with husband Physical Exam Temp: 98.8 deg F BP: 128/75 Pulse: 70 Ht: 66inches Wt: 160lbs GEN: Well-nourish, well-hydrated. NAD HEAD: normocephalic, atraumatic ORO-PARYNX: mucus membranes mildly dehydrated, clear, no exudates EYE: PERLA, EOMI LUNGS: CTA B/L, no wheezing or rhonchi CV: RRR, no M/R/G Abd: Soft, NT/ND, no organomegaly NEURO: sensation in b/l upper extremities in-tact to light touch PSYCH: A&O x 3, judgment, memory and insight intact Physical Exam MSK hypertonic paraspinal muscles in thoracic spine and cervical spine B/L hypertonic trapezius B/L hypertonic levator scapula B/L decreased cervical lordosis hypertonic anterior and middle scalenes B/L TTP over right occipital condyle with reproduction of symptoms ROM of head: decreased rotation to the right compared to the left, otherwise full ROM of neck, neck is supple Negative Spurling’s test Osteopathic Exam Patient was found to have tenderness, asymmetry, restriction of ROM, and tissue texture changes in the following areas: HEAD: OA compression on the right, with TTP over occipital condyle CERVICAL SPINE: C2 Flexed RRSR anterior and middle scalenes restriction Right, Right SCM restriction THORACIC SPINE: T2 Flexed SLRL B/L trigger points in upper trapezius Differential Diagnosis Tension headache Migraine headache Dehydration Cerebral aneurysm Meningitis Viral syndrome Trigeminal neuralgia Pseudotumor cerebri Giant Cell Arteritis Diagnosis Allopathic Assessment and Plan Tension headache (G44.209) Muscle spasm of paraspinal muscles (M62.838) Heating pad Stretching exercises for upper back and neck Increase oral fluid intake Diclofenac PRN Osteopathic Assessment and Plan Somatic Dysfunction of Head Region (M99.00) Somatic Dysfunction of Cervical Region (M99.01) Somatic Dysfunction of Thoracic Region (M99.02) OMT to 3 Body Regions (98926) Billing for this Visit 99213 (E/M level 3 establish patient office visit) - 25 modifier on E/M code for other separate procedure (OMT) 98926 (3-4 Body Regions Treated) Billing Tips Evaluation and Management Codes: 99202, 99203, 99204 most often used for new patients 99212, 99213, 99214 most often used for established patients Modifier 25 for “separate and identifiable procedure done the same day” CPT codes 98925 (OMT to 1-2 body regions) 98926 (OMT to 3-4 body regions) 98927 (OMT to 5-6 body regions) 98928 (OMT to 7-8 body regions) 98929 (OMT to 9-10 body regions) Greater Occipital Nerve Originates from C2 spinal Between C1 and C2, along with the lesser occipital nerve Emerges inferior to the suboccipital triangle (obliquus capitis inferior) muscle Passes through the trapezius muscle and ascends to innervate the skin along the posterior scalp to the vertex of the head Greater Occipital Nerve OMT Techniques OA decompression Muscle Energy for Cervical Spine Muscle Energy for the shoulder girdle Upper Thoracic Soft Tissue OA Decompression Used for abnormal tension, hypertonicity or spasm of the cranial base that can interfere with cranial-sacral functioning Releases tissues around the jugular foramen thus enhancing fluid drainage from the cranial vault and reducing intracranial fluid congestion. Restores normal vagal tone. Can also benefit the glossopharyngeal nerve, and the spinal accessory nerve. OA Decompression Physician: seated at the head of patient Patient: supine Place fingers vertically (pointing toward ceiling) so that the patient’s sub-occipital area is balanced on the physicians fingertips. The pads of the fingers should maintain contact with this area. The weight of the patient’s head is the only therapeutic force applied. As tissues relax, maintain pressure, until you can palpate the posterior arch of the atlas (C1). Continue pressure to slowly disengage the atlas from the occiput. Disengagement will be noted by a “floating sensation” of the atlas As the atlas floats, balance it, support it with the tips of your ring finger while moving the occiput gently in a cephalad direction with the tips of your middle fingers. This will further disengage the occiput from the atlas and decompress the condylar region. Cervical Spine Muscle Energy Cervical Spine Muscle Energy Dysfunction (C2 F RRSR) Physician: seated at the head of the table Patient: supine Cradle the patient’s head in your hands and palpate the articular pillars at the level of C2 Extend the patient’s head until motion is felt under your palpating fingers Rotate the patient’s head to the left until motion is felt under your palpating fingers Sidebend your patient to the left at C2 by translating C2 to the right with your left finger (creating left sidebending) Instruct the patient to attempt to bring their head toward their right ear (right sidebending) while providing isometric resistance for 3-5 seconds Instruct the patient to relax while easing your counterforce Reposition to a new restrictive barrier by increasing flexion, left rotation and left sidebending Repeat 3-5x or until no further progress is made Re-check Shoulder Girdle Muscle Energy Shoulder Girdle Muscle Energy Patient: seated or supine Physician position: standing (if patient is seated) or seated (if patient is supine) Used to assist in relaxation of the superior head of trapezius Contact AC joint and ipsilateral neck with hands and have patient shrug shoulder against counterforce. Have the patient relax, take up the slack, and repeat 2 more times or until tissues soften Seated Soft Tissue Upper Thoracic Soft Tissue Can be done in any position (supine, prone, lateral recumbant or seated) Primarily used to address the root of the neck Also to some degree addresses sympathetic innervation (especially if used in conjunction with rib raising)