* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
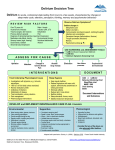
Download Trigger for Managing Delirium
Survey
Document related concepts
Transcript
CHAMP: Bedside Teaching MANAGING AGITATED DELIRIUM Andrea Bial MD Teaching Trigger: A hospitalized senior with delirium is agitated, although not a threat to self or others. The team wants to give haldol now; the nurse wants an order for soft wrist restraints “just in case” because the patient will be going to radiology later for a CT scan. I. Clinical Question: What are the appropriate indicators and choices for medication use in delirium? Teaching Points: 1. Pharmacologic Management a. No RCT of treating delirium in hospitalized seniors. b. Most recommendations are extrapolated from delirium in other patient populations (cancer, AIDS, etc) or from agitation in dementia patients. c. See Table 1 below. TABLE 1: MEDICATIONS FOR THE TREATMENT OF DELIRIUM DRUG CATEGORY Risperidone Atypical Antipsychotic Min sedating; less EPS Olanzapine Atypical Antipsychotic Min sedating; less EPS Quetiapine Atypical Antipsychotic Min sedating; less EPS; better in PD? DISADVANTAGES ↓ sz thrshld; more EPS; ↑QT; ↑ risk of Torsades Take time to work; no evidence in acute use Same as Risperidone Same as Risperidone DOSE 0.25-0.5mg po, IM, IV; can repeat in 30 mins x1, then q4h 21h (10-30h) 0.25-0.5mg po bid 2.5-5mg po qd 25mg po bid 20-30h 30h (21-54h) 6h 12h Probably a better choice in acute setting when patient is very agitated Use the atypicals when medication needed but not urgently Same as Risperidone Same, except use this if pt has or is suspected to have PD Do not use for delirium except in the case of w/d or if antipsychotics cannot be used ADVANTAGES T1/2 AVG (RANGE) COMMENTS II. Haldol Typical Antipsychotic Min sedating; can be given IM or IV (not FDA-apprvd) Lorazepam Benzodiazepine Useful in w/d; no 1st-pass liver effect; no renal adjustment necessary Very sedating; possible disinhibition effect; can cause delirium 0.5-1mg po, IM, IV q6-8h Clinical Question: What is the nonpharmacological management of delirium? Teaching Points: 1. Background a. As stated previously, you will often need to be treating the patient while also evaluating the cause of his/her delirium. b. Focus on reassurance, orientation, noise reduction, and mobilization of the patient. c. AVOID restraints (see below); use family members or request bedside sitters. 2. Non-pharmacologic management/7 key areas: a. Cognition: ensure orientation with correct date on orientation boards and keeping drapes open during the day. b. Sleep: minimize sleep deprivation by avoiding 2am blood draws; no overnight VS or BS if can be avoided; orders meds for “when awake” (e.g., nebs). c. Mobility: OOB to chair asap; order PT/OT asap; avoid foley catheters and restraints. See below. d. Vision: assess whether or not patient uses (or needs) glasses, and if so, attempt to get them; if N/A, post sign stating “Low vision.” e. Hearing: assess whether or not the patient is hard of hearing and has aids; if not, post sign stating “HOH; please speak loudly in front of patient.” f. Dehydration: ensure fluid intake (po is best) even if it means teammember sits with patient at mealtime to observe. Avoid the accumulation of cans of nutrition supplements at the bedside. g. Observation: ask family members to sit with patient or get sitter; move patient closer to nurse’s station. III. Clinical Question: What is the role of restraint use in the delirious older patient? Teaching Points: 1. Avoid physical restraints whenever possible, including “unofficial” restraints such as using a bed-sheet to tie a patient down. 2. Restraints increase the risk of falls, injury, and delirium. 3. If needed for emergent situation (patient is a threat to self or others), use for the shortest duration possible with frequent re-evaluations for need and possibility of discontinuing.