* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Applications of Cone Beam Computed Tomography in
Survey
Document related concepts
Transcript
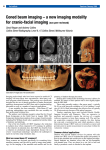
CURRENT THERAPY J Oral Maxillofac Surg 66:791-796, 2008 Applications of Cone Beam Computed Tomography in the Practice of Oral and Maxillofacial Surgery Faisal A. Quereshy, MD, DDS,* Truitt A. Savell, DDS, MD,† and J. Martin Palomo, DDS, MSD‡ Providing imaging in 3 dimensions, computed tomography (CT) has had a profound effect on surgical and medical practice since its introduction in 1973.1 Practitioners at that time certainly marveled at the new technology, but likely were at a loss as to how to apply it or what exactly the images meant. It was only after years of research, as well as the development of a whole new aspect of radiology, that we have been able to apply this technology for the benefit of our patients. In oral and maxillofacial surgery, we are accustomed to using CT in patients with trauma and pathological conditions in the hospital setting; however, in dental practice, practitioners depend almost entirely on 2-dimensional plain films. The applications and advantages of CT in dentistry remain largely unrealized. Cone beam CT (CBCT) was first developed for use in angiography. In 1998, Mozzo et al2 reported the first CBCT unit developed specifically for dental use, the NewTom 9000 (Quantitative Radiology, Verona, Italy). Other similar devices introduced at around that time included the Ortho-CT, which was renamed the 3DX (J. Morita Mfg Corp, Kyoto, Japan) multi-image micro-CT in 2000.3,4 In 2003, Hashimoto et al4 reported that the 3DX CBCT produced better image quality with a much lower radiation dose than the newest multidetector row helical CT unit (1.19 mSv vs 458 mSv per examination). CBCT machines have 2 major differences compared with so-called “medical” CT scanners. First, CBCT uses a low-energy fixed anode tube, similar to that used in dental panoramic x-ray machines. Second, CBCT machines rotate around the patient only once, capturing the data using a cone-shaped x-ray beam. These changes allow for a less expensive, smaller machine that exposes the patient to approximately 20% of the radiation of a helical CT, equivalent to the exposure from a full-mouth periapical series.5-8 All of the CBCT scanners currently on the market use the same technology, with only slight differences. The major difference is in the detector used, either an amorphous silicon flat-panel detector or a combination of an image intensifier and a charge-coupled device (CCD) camera. Both these technologies have been proven to be accurate and reliable and to provide sufficient resolution for the needs of dental medicine (Fig 1). Within every field, the introduction of new technology raises several fundamental questions, including identifying the practical applications of the new technology and determining whether it is truly superior to existing modalities. These questions are not easily answered, but require research and comparison. This article explores the possible applications of this new CBCT technology and the ongoing research in these areas, with the goal of applying CBCT data in an evidence-based manner. Received from the School of Dental Medicine, Case Western Reserve University, University Hospitals Case Medical Center, Cleveland, OH. *Program Director, Department of Oral and Maxillofacial Surgery. †Former Resident, Department of Oral and Maxillofacial Surgery. ‡Associate Professor of Orthodontics and Director, Craniofacial Imaging Center. Address correspondence and reprint requests to Dr Quereshy: Department of Oral and Maxillofacial Surgery, School of Dental Medicine, Case Western Reserve University, 2123 Abingdon Road, Cleveland, OH 44106; e-mail: [email protected] Implant Dentistry The advantages of CBCT in visualizing the alveolus in 3 dimensions and making precise measurements before surgery are obvious in the field of implant dentistry (Fig 2). With conventional panoramic radiography, it is not unusual to anticipate adequate bony support preoperatively, only to be disappointed in the reflection of tissue. Obviously, having this information preoperatively greatly reduces the likelihood of the need to change the treatment approach intraoperatively. This gives the surgeon the ability to anticipate implant placement and even to place implants in a virtual model in © 2008 American Association of Oral and Maxillofacial Surgeons 0278-2391/08/6604-0026$34.00/0 doi:10.1016/j.joms.2007.11.018 791 792 CONE BEAM COMPUTED TOMOGRAPHY FIGURE 1. Some currently available CBCT scan devices. A, NewTom 3G (courtesy of Aperio Services, Sarasota, FL). B, i-Cat (courtesy of Imaging Sciences, Hatfield, PA). C, ILUMA (courtesy of IMTEC Corp, Ardmore, OK). D, ProMax 3D (courtesy of Planmeca Oy, Helsinski, Finland). E, CB MercuRay (courtesy of Hitachi Medical System America Inc, Twinsburg, OH). F, Dental CBCT (courtesy of TeraRecon Inc, San Mateo, CA). G, 3D Accuitomo (courtesy of J Morita USA, Irvine, CA). H, Sirona Galileos (courtesy of Sirona Dental Systems North America, Charlotte, NC). Quereshy, Savell, and Palomo. Cone Beam Computed Tomography. J Oral Maxillofac Surg 2008. terms of bone height, bone width, nerve position, and even objective measures of bone quality.9 With regard to a traditional panoramic radiography, the average machine produces approximately 25% magnification, which must be accounted for when planning implant placement. Preliminary studies on CBCT, specifically the NewTom 9000, have concluded that the CBCT image underestimates the actual distances; however, these differences were significant FIGURE 2. Images produced from a single exposure for the purpose of dental implant planning. The images selected here are panoramic and cross-sectional views with the mandibular nerve marked, as well as a surface and radiographic (maximum intensity projection) view with the stent in place. Quereshy, Savell, and Palomo. Cone Beam Computed Tomography. J Oral Maxillofac Surg 2008. only for the skull base. Imaging within the dentomaxillofacial regions was found to be quite reliable, demonstrating no significant differences.10 The fact that measurements from the CBCT are routinely accurate throughout the maxilla and mandible makes this an excellent modality for planning implant placement.11 Conventional multislice CT has been used for implant planning and in fabrication of a stent used intraoperatively for precise implant placement in pre- 793 QUERESHY, SAVELL, AND PALOMO FIGURE 3. CBCT images of a patient with a mandibular cyst. A, Mesial view of right half of the mandible in a surface mode. B, Anterior view of the mandible in the surface mode (measurements in mm). C, Lingual view of the mandible in surface mode (measurements in mm). D, Radiographic cross-sectional view of the maxilla and mandible. E, Panoramic view. Quereshy, Savell, and Palomo. Cone Beam Computed Tomography. J Oral Maxillofac Surg 2008. determined locations. The stent can be fabricated on top of a CT image without the need for patient contact, allowing for precise placement of implants, prefabrication of the prosthesis and abutments, and delivery of the prosthesis on the same day as surgery.12 CBCT images have similar capabilities with the benefit of less radiation exposure to the patient. Oral and Maxillofacial Pathology Conventional CT is used routinely in the diagnosis of maxillofacial pathology. Given the higher resolution, lower radiation dose, and lower cost of CBCT in imaging the maxillofacial region, it stands to reason that CBCT can easily replace conventional CT in this regard. Threedimensional imaging of cysts and tumors of the maxillofacial region can give the surgeon the vital information necessary for planning surgery; with volumetric analysis, this can help anticipate the need for and volume of a potential graft for reconstruction (Fig 3). CBCT data also can be useful in creating a stereolithic model of the area of interest. Temporomandibular Joint Disorders The diagnosis and treatment planning of temporomandibular joint (TMJ) disorders often are quite challenging. Although magnetic resonance imaging remains the gold standard for imaging the intra-articular components of the TMJ, evaluation of the bony components is often left to conventional panoramic radiographs. Panoramic radiographs can provide a general impression of the joint in 2 dimensions but have low sensitivity in evaluating changes in the condyle, poor reliability, and low accuracy in evaluating the temporal components of the joint.13 The imaging offered by current CBCT machines has been shown to provide a complete radiographic evaluation of the bony components of the TMJ (Fig 4). The resulting images are of high diagnostic quality. Given the significantly reduced radiation dose and cost compared with conventional CT, CBCT may soon become the investigational tool of choice for evaluating bony changes of the TMJ.14 Craniofacial Surgery Treatment planning for patients with cleft lip and palate entails many unique considerations. Due to the young age of the patients and concerns about radiation exposure, conventional CT is not always used. Timing of alveolar cleft repair is often determined based on panoramic and occlusal radiographs. Other considerations include palatal expansion as well as segmental alignment. CBCT should allow better evaluation of dental age, arch segment positioning, and cleft size compared 794 CONE BEAM COMPUTED TOMOGRAPHY FIGURE 4. Different possible views of the TMJ complex using CBCT. A, Surface mode. B, Radiographic mode. C, Close up of the radiographic view. D, Crosssectional view in the radiographic mode. Quereshy, Savell, and Palomo. Cone Beam Computed Tomography. J Oral Maxillofac Surg 2008. with traditional radiography (Fig 5). Volumetric analysis promises to offer better prediction in terms of the morphology of the defect, as well as the volume of graft material necessary for repair. Questions abound regard- FIGURE 5. CBCT images of a patient with a cleft palate. A, Anterior view of the maxilla in the surface mode. B, Anterior view of the maxilla in the radiographic mode. C, Occlusal view of the maxilla in the surface mode. D, Occlusal view of the maxilla in the radiographic mode. Quereshy, Savell, and Palomo. Cone Beam Computed Tomography. J Oral Maxillofac Surg 2008. ing the stability of the arch after grafting, the quality of the bone graft over time, and the effect on overall facial growth; CBCT provides a means to investigate these issues in depth. QUERESHY, SAVELL, AND PALOMO 795 FIGURE 6. Preoperative and postoperative CBCT images of a patient who underwent bilateral split saggital osteotomy. A, Preoperative soft tissue profile view in surface mode. B, Preoperative radiographic view of the patient’s right half. C, Preoperative radiographic view of the patient’s left half. D, Postoperative soft tissue profile view in surface mode. E, Postoperative radiographic view of the patient’s right half. F, Postoperative radiographic view of the patient’s left half. Quereshy, Savell, and Palomo. Cone Beam Computed Tomography. J Oral Maxillofac Surg 2008. FIGURE 7. CBCT images of a patient with an impacted supranumerary tooth. A, Anterior view of the maxilla in the radiographic mode. B, View of the right half of the maxilla in the radiographic mode. C, Surface view of the anterior right segment of the maxilla. D, Anterior view of the maxilla in the surface mode. E, Occlusal view of the maxilla in the radiographic mode. Quereshy, Savell, and Palomo. Cone Beam Computed Tomography. J Oral Maxillofac Surg 2008. 796 Orthognathic Surgery Clinicians have long evaluated the usefulness of 3-dimensional imaging in orthodontics and orthognathic surgery, with a major concern being the correlation between soft tissue and hard tissue changes.15 For decades, lateral cephalography has been the standard modality for diagnosing skeletal and dental deformities, as well as for use in surgical prediction and treatment planning. These applications are made possible by the early growth studies of the mid-1970s that set the stage for current cephalometric analysis and prediction.16,17 In like fashion, it stands to reason that before a 3-dimensional model can be reliably adopted for orthodontic and orthognathic analysis and surgical prediction, extensive research is needed to characterize the landmarks and relationships that this technology allows us to measure. As useful as cephalometric analysis can be, its imaging accuracy is inadequate in such deformities as hemifacial microsomia, severe facial asymmetries, and occlusal cant. Three-dimensional imaging of the hard and soft tissue makes all of the data available (Fig 6); the only question is how best to apply and manipulate that data for more accurate surgery and treatment planning. Impacted Teeth The identification, treatment planning, and evaluation of potential complications of impacted teeth are greatly improved by adding the third dimension through CBCT. The site evaluation becomes not only less invasive and less time-consuming, but also more complete. The relationship of impacted third molars to the mandibular canal, adjacent teeth, sinus walls, and cortical borders is important diagnostic information that can directly impact the outcome of surgery.18 Using CBCT to locate and evaluate impacted cuspids and supernumerary teeth seem to make the surgical procedure more efficient and less invasive (Fig 7).19 Because the anatomic structures adjacent to the region of interest can be seen in 3 dimensions, this additional information may reduce the morbidity and potential complications during surgery, contributing to a better outcome. In summary, with the continued decreasing cost of CBCT technology, it is only a matter of time until CBCT finds its way into the average oral and maxillofacial surgery practice. The increased diagnostic capa- CONE BEAM COMPUTED TOMOGRAPHY bility combined with the lower radiation dose also will help bring this technology into the mainstream. The applications described herein are merely the beginning. We are now capable of obtaining significantly more data to characterize a patient’s condition. The next step is to establish how best to use these additional data in the most effective manner. References 1. Hounsfield GN: Computerized transverse axial scanning (tomography): Description of the system. Br J Radiol 46:1016, 1973 2. Mozzo P, Procacci C, Tacconi A, et al: A new volumetric CT machine for dental imaging based on the cone-beam technique: Preliminary results. Eur Radiol 8:1558, 1998 3. Arai Y, Tammisalo E, Iwai K, et al: Development of a compact computed tomographic apparatus for dental use. Dentomaxillofac Radiol 28:245, 1999 4. Hashimoto K, Yoshinori A, Kazui I, et al: A comparison of a new, limited cone beam computed tomography machine for dental use with a multi– detector row helical CT machine. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 95:371, 2003 5. Mah J, Hatcher D: Three-dimensional craniofacial imaging. Am J Orthod Dentofac Orthop 126:308, 2004 6. Kunihiko S, Kazuo Y, Kan U, et al: Development of dentomaxillofacial cone beam X-ray CT system model CB MercuRay. Medix 37:40, 2002 7. Palomo JM, Kau CH, Bahl Palomo L, et al: Three-dimensional cone beam computerized tomography in dentistry. Dent Today 25:130, 2006 8. Sukovic P: Cone beam computed tomography in craniofacial imaging. Orthod Craniofac Res 6(Suppl 1):31, 2003 9. Norton MR, Gamble C: Bone classification: An objective scale of bone density using the computerized tomography scan. Clin Oral Implants 12:79, 2001 10. Lascala CA, Panella J, Marques MM: Analysis of the accuracy of linear measurements obtained by cone beam computed tomography (CBCT-NewTom). Dentomaxillofac Radiol 33:291, 2004 11. Hatcher DC, Dial C, Mayorga C: Cone beam CT for presurgical assessment of implant sites. J Calif Dent Assoc 31:825, 2003 12. Marchack CB, Moy PK: The use of a custom template for immediate loading with the definitive prosthesis: A clinical report. J Calif Dent Assoc 31:925, 2003 13. Dahlstrom L, Lindvall AM: Assessment of temporomandibular joint disease by panoramic radiography: Reliability and validity in relation to tomography. Dentomaxillofac Radiol 25:197, 1996 14. Tsiklakis K, Syriopoulos K, Stamatakis HC: Radiographic examination of the temporomandibular joint using cone beam computed tomography. Dentomaxillofac Radiol 33:196, 2004 15. Hajeer MY, Millett DT, Ayoub AF, et al: Applications of 3D imaging in orthodontics: Part I. J Orthodont 31:62, 2004 16. Popovich F, Thompson GW: Craniofacial templates for orthodontic case analysis. Am J Orthod 71:406, 1977 17. Broadbent BH Sr, Broadbent BH Jr, Golden WH: Bolton Standards of Dentofacial Developmental Growth. St Louis, MO, Mosby-Year Book, 1975 18. Danforth RA, Peck J, Hall P: Cone beam volume tomography: An imaging option for diagnosis of complex mandibular third molar anatomical relationships. J Calif Dent Assoc 31:847, 2003 19. Walker L, Enciso R, Mah, J: Three-dimensional localization of maxillary canines with cone-beam computed tomography. Am J Orthod Dentofac Orthop 128:418, 2005