* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download obstetrics-and-gynecology-practical-exam-topics-with
Survey
Document related concepts
Dental emergency wikipedia , lookup
Infection control wikipedia , lookup
HIV and pregnancy wikipedia , lookup
Birth control wikipedia , lookup
Maternal health wikipedia , lookup
Menstrual cycle wikipedia , lookup
Women's medicine in antiquity wikipedia , lookup
Prenatal nutrition wikipedia , lookup
Menstruation wikipedia , lookup
Maternal physiological changes in pregnancy wikipedia , lookup
Prenatal development wikipedia , lookup
Prenatal testing wikipedia , lookup
Breech birth wikipedia , lookup
Transcript
“OVIDIUS “ UNIVERSITY OF CONSTANTA
FACULTY OF GENERAL MEDICINE
VIth YEAR – ENGLISH
http://drddp.wordpress.com/
OBSTETRICS AND GYNECOLOGY
Practical exam topics
1. Bony pelvis, side walls
A. large pelvis
limited by anterior inner wing of iliac bone which form the iliac fossa
BITROANTERIAN diameter: 32 cm
BICREST diameter: 28 cm
BISPINOS diameter: 24 cm
Antero-posterior diameter: 19 to 20 cm
B. small pelvis (obstetrical pelvis) presents:
I.
Superior Inlet
Transverse diameter -> 13.5 cm
Oblique diameter -> 12 – 12.5 cm
promonto-suprapubic diameter -> 11 cm
Antero-posterior diameter (CONJUGATA VERA) -> 10.5 – 11 cm
II. Middle Inlet
Sagittal diameter -> 11.5 cm
III. Inferior Inlet
Lower margin of coccyx -> 9.5 cm and can get till 11-12.5 cm
bi-ischial diametre 10cm
Pelvimetry
diagonal conjugate 12.5 – 13cm
bi-ischial diametre 10cm
incisura ischiadica 5-6 cm
angle of sub-pubic arch 90 degrees
2. Perineum
The perineum or perineum is the region of the body between the anus and genitals. In
human anatomy, the perineum is a region of the body including the perineal body and
surrounding structures. According to some definitions, in females it is located between the
vagina and anus and in males between the scrotum and anus.
Both men and women can experience the perineum as an erogenous zone that it is sensitive
to touch, both of caresses and pressure. That's because the area's musculature is rich in
nerves and blood vessels. Tissue under the skin also border area around the prostate gland , a
point which is sensitive to sexual stimulation, and therefore also called man - G point.
At a birth may tissue of the perineum at the woman stretched too much and crack.
1
To avoid such uncontrolled cracks, or to speed up a slow and the child dangerous childbirth,
it happens that the midwife put an incision in the perineum, which is called an episiotomy.
If such a cut, or spontaneous fracture , heal poorly, it can affect a woman's sexual prowess.
When severe cases it can also lead to fecal incontinence.
Terminology
It is generally defined as the surface region in both males and females between the pubic
symphysis and the coccyx. The perineum is the region of the body inferior to the pelvic
diaphragm and between the legs. It is a diamond-shaped area on the inferior surface of the
trunk that includes the anus and, in females, the vagina. Its definition varies: it can refer to
only the superficial structures in this region, or it can be used to include both superficial and
deep structures. The perineum corresponds to the outlet of the pelvis.
It is an erogenous zone for both males and females. Perineal tears and episiotomy often
occur in childbirth with first-time deliveries, but the risk of these injuries can be reduced by
preparing the perineum, often through massage.
The anogenital distance is a measure of the distance between the anus and the base of the
penis or vagina. Studies show that the human perineum is twice as long in males as in
females. Measuring the anogenital distance in neonatal humans has been suggested as a
noninvasive method to determine male feminisation and thereby predict neonatal and adult
reproductive disorders.
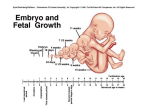
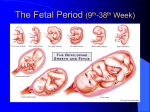
3. Fetal head
The fetal head is composed of:
face, 2 frontal bones, 2 parietal bones, 2 temporal bones, occipital bone, the wings of
the sphenoid
Sutures:
Frontal, sagittal, coronal, lambdoid
Fontanels:
the greater (anterior, bregmatic)
the lesser( posterior, lambdoid )
the casserian( temporal )
The diamters of the newborn skull
The occipitofrontal diameter = 11,5 – 12 cm
The biparietal diameter = 9,5 cm
The bitemporal diameter = 8 – 8,5 cm.
The mobility of fetal head in relation with the vertebral column.
Engagement diameters of the fetal head
suboccipito-bregmatic diameter- engagement diameter in flexed head presentation =
9,5 cm
suboccipito – frontal diameter– sinciput presentation = 11 cm.
submento – bregmatic diameter – facial presentation = 9,5 cm.
sincipito-mentonier diameter– brow presentation = 13,5 cm.
The head circumferences
the great circumference – corresponds to the occipito-frontal diameter = 34,5 cm.
the small circumference – corresponds suboccipito- bergmatic diameter= 32 – 33
cm.
modulation process of the head.
2
4. Clinical diagnosis of the pregnancy
There are three degrees of certainty in diagnosis approach: Det finns tre grader av säkerhet i diagnos
tillvägagångssätt:
- presumptive signs (Amenohrea, breast tenderness, nausea, vomiting, increase skin
pigmentation,
skin striae),
- probable signs (enlargement of the uterus, maternal sensation of uterine contractions or
fetal movement, hegar sign, positive urine or serum B-HCG)
- positive signs (hearing fetal heart tones, sonographic visualization of a fetus, perception of
fetal movements by an external examiner, and x-ray showing a fetal skeleton)
a. Amenorrhea
It is significant for brutal stop menstruation in a woman of reproductive age with
regular cycles in advance, >10 days after the expected date of menstruation
Amenorrhea of pregnancy is maintained by estrogen and progesterone secreted by
the placenta
b. Digestive manifestations
Nausea and Vomiting: manifests usually in the morning
Other: changes in taste, changes in appetite, heartburn, constipation
c. Urinary disturbances
Polyuria due to increase in uterus size and pressure on the bladder
d. General Manifestations / neuropsychiatric
Fatigue, increased temperature
e. Perception of fetal movements
Pregnant women perceive fetal movements at 16 to 20
f. skin changes
skin hyperpigmentation: is explained by stimulation of MSH (melanocyte stimulating hormone)
Stretched skin
g. Breast modification
Dilated superficial veins
Fullness, increased pigmentation of nipple region/areola, prominent Montgomery
h. Cervix/ vagina
Deep-bluish in colour (venous dilatation)
Endocervix softens
i. Uterus
From firm, flattened to soft and globular; Hegar Sign
Uterine a. pulsation may be felt at lateral fornix
Uterine size by palpation: 6,8,10,12w – at 12w becomes abdominal and just palpable
suprapubically
Differential diagnosis: uterine tumour, estrogen secreting ovarian tumour
j. Braxton-Hick's contractions
This involves painless uterine contractions occurring throughout pregnancy.
3
It usually begins about the 12th week of pregnancy and becomes progressively
stronger.
k. Abdominal changes
This corresponds to changes that occur in the uterus, as the uterus grows the
abdomen gets larger.
Abdominal enlargement alone is not a sign of pregnancy.
Enlargement may be due to uterine or ovarian tumors, or edema.
l. Positive signs of pregnancy
Positive signs of pregnancy are those signs that are definitely confirmed as a
pregnancy.
They include fetal heart sounds, ultrasound scanning of the fetus, palpation of the
entire fetus, palpation of fetal movements, x-ray, and actual delivery of an infant.
m. Cervical Changes
Goodell's sign. The Goodell's sign is when there is marked softening of the cervix.
This is present at 6 weeks of pregnancy.
Formation of a mucous plug. This is due to hyperplasia of the cervical glands as a
result of increased hormones.
5. Laboratory diagnosis of the pregnancy
Tests Utilized To Determine Pregnancy
Tests are based on the presence of human chorionic gonadotropin (HCG) in the urine or
blood.
Urine. This test can be performed accurately 42 days after the last menstrual period
or 2 weeks after the first missed period. The first urine specimen of the morning is
the best one to use.
Blood. Radioimmunoassays (RIA) can detect HCG in the blood 2 days after
implantation or 5 days before the first menstrual period is missed.
NOTE: HCG levels peak between 50 to 90 days after the last menstrual period.
Home pregnancy test kits are easily available and inexpensive. This test allows
prenatal care to be started early.
Urine tests:
Test of HCG (chorionic gonadotrophin hormones)
Alpha and beta (glycoprotein) subunit
Cross reaction for alpha : LH,FSH, TSH (sharing of alpha subunit)
Morning specimen urine; repeat 1-2 weeks if necessary
2 methods ; indirect and direct antibody test
Serum HCG produced by synciotrophoblast; peaks at 10weeks; luteotropic &
maintains corpus luteum until placental steroidogenesis level is satisfactory
False positive:
cross reaction to above hormones. Current test using specific beta-subunit
Contamination by higher than normal urine protein
Ovarian tumour
False negative:
Technical error
Test done too early
Abnormalities of pregnancy eg miscarriage
Sensitive serum assay : radioreceptor assay or radioimmunoassay
Advantage of sensitivity, allowing diagnosis of pregnancy well before the
first missed period
More expensive,reserved for special indications eg. Ectopic
pregnancy,surveillance for molar pregnancy
4
Hormonal Withdrawal Test:
Large dose of estrogen/progesterone for 2-3 days. Usually withdrawal bleed after 35days if not pregnant
Possible harm; NOT DONE
Later Signs
After 12 weeks – uterus palpable above symphysis pubis
Fetal heart sounds, fetal parts and fetal movement
6. Ultrasound examination in obstetrics
First-trimester ultrasound can be done transvaginally or transabdominally and should:
Document location of the gestational sac. An intrauterine sac is visible
transvaginally as early as 5 weeks' gestation.
Document fetal number.
Confirm fetal viability. Fetal cardiac activity can be detected transvaginally when
the embryo is 5 mm or greater in length (approximately 6 weeks' gestation).
Evaluate gestational age. Measurement of the fetal crown-rump length between 6 to
13 weeks' gestation can estimate fetal age within 5 days
Evaluate the uterus and adnexal structures.
Second-trimester ultrasound is usually performed transabdominally. It is routinely
performed between 18 and 20 weeks' gestation for evaluation of fetal anatomy, gestational
age, placental location, and amniotic fluid volume. Measurement of cervical length should
be done by transvaginal ultrasound.
The fetal anatomic survey should include, but not to be limited to:
Intracranial anatomy with visualization of the lateral ventricles, choroids
plexus, thalamus, cerebellum, and cisterna magna.
Thorax, diaphragm, heart
Visualization of the stomach.
Visualization of the kidneys and bladder.
Umbilical cord insertion on an intact abdominal wall and determination of
the number of vessels of the umbilical cord (normal: two small arteries and
one large vein).
Upper and lower extremities.
Fetal biometry includes:
The biparietal diameter is the most accurate measurement of gestational age
between 12 and 18 weeks' gestation. The head circumference is measured at
the same level as the biparietal diameter.
Fetal weight may be estimated by composite measurement of the biparietal
diameter, head circumference, femur length, and abdominal circumference.
Placental location should be documented
Amniotic fluid volume
Maternal anatomy. Evaluate the uterus and adnexal structures.
Third-trimester ultrasound is approached transabdominally. The indications for thirdtrimester ultrasound are multiple and include estimation of fetal weight and follow-up of
fetal growth, evaluation of the amniotic fluid volume, follow-up of a fetal anomaly,
determination of fetal presentation, and evaluation of fetal well-being.
Fetal weight is estimated as previously described
If the estimated fetal weight is below the 10th percentile for the gestational
age, the fetus is small for gestational age (SGA) and intrauterine growth
restriction (IUGR) is suspected
If the estimated fetal weight is above the 90th percentile for the gestational
age, the fetus is large for gestational age (LGA) and macrosomia is
suspected.
Amniotic fluid volume
What Should Be Seen In A First Trimester Pregnancy?
5
The site of pregnancy
The gestational sac, amniotic cavity including numbers
The fetus and viability
Any other pelvic masses
Earliest sign could be thickened ET > 12mm
4-5 weeks – gestational sac (1-2 mm)
7. Lie, presentations and positions
Fetal Lie
The relation of the long axis of the fetus to that of the mother
Longitudinal lie - found in 99% of labours at term
Transverse lie - multiparity, placenta praevia, hydramnios, uterine anomalies
Oblique lie: unstable (become logitudinal or transversal)
By abdominal palpation, vaginal examination, and auscultation, or by technical means
(USG, X-ray)
Fetal Presentation
The presenting part is the portion of the body of the fetus that is foremost in the birth canal
The presenting part can be felt through the cervix on vaginal examination
Longitudinal lie
-> cephalic presentation
-> breech presentation
Transverse lie
-> shoulder presentation
Cephalic Presentation
Head is flexed sharply
-> vertex / occiput presentation
Head is extended sharply
-> face presentation
Partially flexed
-> bregma presenting (sinciput presentation)
Partially extended
-> brow presentation
Breech Presentation
Frank breech
Complete breech
Footling breech
Position
The relation of an arbitrary chosen point of the fetal presenting part to the Rt or Lt side of
the maternal birth canal
The chosen point
Vertex presentation -> occiput
Face presentation -> mentum
Breech presentation -> sacrum
Each presentation has two positions Rt or Lt
Each position has 3 varieties : anterior, transverse, posterior
8. Labor and delivery
Childbirth, labor, delivery, is the culmination of a period of pregnancy with the expulsion of
one or more newborn infants from a woman's uterus.
The process of normal childbirth is categorized in three stages of labour:
The shortening and dilation of the cervix,
Descent and birth of the infant,
Birth of the placenta.
When a patient first presents to the labor floor a quick initial assessment is made, using the
history of present pregnancy, obstetric history and the standard of medical and social
history.
Routinely patients are queried regarding contractions, vaginal bleeding, leakage of fluid and
fetal movement.
6
Beyond the standard physical examination the obstetric examination includes maternal
abdominal examination for contraction and the fetus (Leopold maneuvers), cervical
examination, fetal heart tones, and sterile speculum examination if rupture of membranes is
suspected.
9. Mechanism of labor in occipital presentation
1.
2.
3.
4.
5.
6.
Engagement
The biparietal diameter of the fetal head, the greatest transverse diameter of the head
in occiput presentations, passes through the pelvic inlet. LOT -> 40%
ROT -> 20%
OP -> 20% ROP > LOP
ROA / LOA -> 20%
Descent
In nullipara engagement takes place before the onset of labour & further descent may
not occur till the 2nd stage
In multipara descent begins with engagement
It is gradually progressive till the fetus is delivered
It is affected by the uterine contractions & thinning of the lower segment
Flexion
The descending head meets resistance of pelvic floor, Cx & walls of the pelvis ->
flexion
Internal Rotation
Turning of the head from the OT position -> anteriorly towards the symphysis pubis
ie. Occiput moves from transverse to anterior 45º
Less commonly OT -> posteriorly towards the sacrum 135º
Extension
When the flexed head reaches the vulva it undergoes extension Æ the base of the
occiput will be in direct contact with the inferior margin of the symphysis pubis
Crowning Æ the largest diameter of the fetal head is encircled by the vulvar ring
The head is born by further extension as the occiput, bregma, forehead, nose, mouth
& chin pass successively over the perineum
External Rotation (Restitution)
After delivery of the head it returns to the position it occupied at engagement, the
natural position relative to the shoulders (oblique position)
Then the fetal body will rotate to bring one shoulder anterior behind the symphysis
pubis (biacromial diameter into the APD of the pelvic outlet)
Restitution is followed by complete external rotation to transverse position (occiput
lies to next to left maternal thigh)
The anterior shoulder slips under the pubis
By lateral flexion of the fetal body the post shoulder will be delivered & the rest of
the body will follow
Occiput Posterior Position
Mechanism of labour is identical to OT & anterior varieties
The occiput rotate to the symphysis pubis through 135º instead of 90º or 45º
If rotation does not occur -> direct occiput posterior or partial rotation -> transverse
arrest
10.Mechanism of labor in face presentation
Difficult birth, prolonged
Engagement
the orientation of the presentation with the sincipito-mentonier ( 13,5 cm ) diameter
into an oblique diameter of the maternal pelvis
complete deflectation – the skull solidarise with the frontal back
7
the presentation reach the surface of the pelvic inlet but the progression is halted
because the solidarized fetal head and back brings at the level of the superior
straightthe presternosincipital diameter (13,5 cm) with which the engagement is
impossible
The descent
cannot occur unless the flexion of the fetal head occurs, which is possible only if the
menton rotates anteriorly in MP
Expulsion
Occurs by progressive flexion of the head sustained by the menton witch is fixed
under symphisis
The head expulsion is produced with the face up, showing successively at the
vulva:mouth, nose, forehead and the rest of the skull
If rotation occurs in MS, the skull stops and the vaginal birth cannot occur by
theinclavation of the fetal face
Obstetrical conduct
Close supervision of labor
When progression of the presentation is not optimal → cesarean delivery
When doing the engaging and turnover in MP birth can move towards vaginal
delivery
Newborns have a characteristic appearance - caput succedaneum make a purplish
swellingof the lips, nose, cheeks. The head remains in deflected attitude a few days
after birth
11.Mechanism of labor in bregmatic presentation
The engagement is in an oblique diameter, producing real plastic phenomena →
cylindricalaspect of the head
Descent and internal rotation are laborious → FP, respectively OS.
Expulsion :
is achieved in 92% in OS
nasofrontal sulcus take fixed under the symphysis and serves as a pivot for the
headwhich becomes flexed in order to deliver → will appear at the opening vulva
thelarge fontanel, frontal boses, parietal boses, the occiput
follows a second time of deflecting , suboccipital region appearing at the rear
cornersof the vulva → the face will deliver
the head sometimes does not rotate → delivery is performed in oblique or
transversediameter
The evolution of birth is prolonged
Obstetrical approach
labor test
12.Mechanism of labor in breech presentation
A breech birth is the birth of a baby from a breech presentation, in which the baby exits
the pelvis with the buttocks or feet first as opposed to the normal head-first presentation. In
breech presentation, fetal heart sounds are heard just above the umblicus.
The bottom-down position presents some hazards to the baby during the process of birth,
and the mode of delivery (vaginal versus Caesarean) is controversial in the fields of
obstetrics and midwifery.
Though vaginal birth is possible for the breech baby, certain fetal and maternal factors
influence the safety of vaginal breech birth. The majority of breech babies born in the
United States are delivered by Caesarean section as most obstetricians do not have the
required skill set anymore and most hospital policies do not permit vaginal breech birth.
8
Factors predisposing to term breech presentation include:
Multiple (or multifetal) pregnancy (twins, triplets, or more)
Abnormal volume of amniotic fluid: both polyhydramnios and oligohydramnios
Fetal anomalies: hydrocephaly, anencephaly, and other congenital abnormalities
Uterine abnormalities.
Prior Caesarean sections
Contracted pelvis
Placenta praevia
Congenital malformation of the uterus such as septate or bicornuate uterus
Multiparae with lax abdominal wall
There are either three or four main categories of breech births, depending upon the source:
Frank breech – the baby's bottom comes first, and his or her legs are flexed at the hip and
extended at the knees (with feet near the ears); 65–70% of breech babies are in the frank
breech position
Complete breech – the baby's hips and knees are flexed so that the baby is sitting
crosslegged, with feet beside the bottom
Footling breech – one or both feet come first, with the bottom at a higher position; this is
rare at term but relatively common with premature fetuses
Kneeling breech – the baby is in a kneeling position, with one or both legs extended at the
hips and flexed at the knees; this is extremely rare, and is excluded from many
classifications
13.Amnioscopy
Examination of a fetus and the amniotic fluid in the lowest part of the amniotic sac using an
amnioscope introduced through the cervical canal after dilatation of the cervix
Amnioscopy sure about is the fetal position and what state it is amniotic fluid.
Amnioscopy also be used to take blood samples from the fetus if there is rupture
Results:
If yellowish that could indicate the presence of bilirubin, resulting in a blood incompatibility
in the event that the pitch is green could warn of the presence meconium, which would
result in hypoxia, ie there is a deprivation of oxygen and therefore the possibility of fetal
distress is occurring
the tone of the amniotic fluid is reddish this would mean that the fetus is dead.
procedure
The patient is placed in the lithotomy position.
“Endoscope inserted through abdomen or in cervix to view fetus and amniotic fluid. Cervix
must be dilated to accept 1 finger because scope diameter is approx. 1 cm – the size of an
average finger” dr. Tomescu
According to the state of the cervix, the largest suitable amnioscope is selected, The suitable
speculum applied, then, the selected tube is guided into the cervical canal.
The obturator is removed and a light source is inserted so that the amnion sac could be
inspected through the intact forewaters.
Indications
To evaluate for possible fetal hypoxia by noting change in color of amniotic fluid caused by
passage of meconium from the rectum of the fetus
To secure a fetal scalp blood sample to determine fetal acid–base and blood gases status in
the diagnosis of fetal hypoxia and distress
Contraindication:
Active labour
Ruptured membrane
9
Cervical infection or STD. Closed cervix
unexplained vaginal bleeding.
14.Amniocentesis
An amniocentesis may be performed beyond 15 weeks to obtain a fetal karyotype, once the chorion
and amnion have fused. Amniocentesis is also offered to any patient of advanced maternal age
(AMA). Amniocentesis involves placing a needle transabdominally through the uterus into the
amniotic sac and withdrawing some of the fluid. The fluid contains sloughed fetal cells that can be
cultured. These cultured cells can then be karyotyped and also utilized in DNA tests.
Early in pregnancy, used for diagnosis of chromosomal and other fetal problems such as:
Down syndrome
Trisomy 13 & Trisomy 18
Later on, it also can be used to detect problems such as:
Infection
Rh incompatibility (to examine bilirubin levels after 24 weeks GS)
Prediction of lung maturity and fetal maturity studies lecithin-sphingomyelin ratio and
phosphatidyl glycerol
Decompression of polyhydramnios
The common risks are rupture of membranes, preterm labor, respiratory distress, postural
deformities, fetal trauma.
15.Clinical and laboratory diagnosis of the membranes rupture
Ruptured membranes are signified at any time during pregnancy by either a sudden gush or
a steady trickle of clear fluid from the vagina.
In a term pregnancy, labor usually follows within 24 hours of membrane rupture.
The risk of intrauterine infection (chorioamnionitis) increases if the patient has ruptured
membranes for longer than 24 hours, with or without labor.
Procedure
Pooling. Upon sterile speculum examination, a pool of amniotic fluid may be present
and visible at the vaginal vault.
Nitrazine test. Testing the fluid with nitrazine paper, which will turn blue in the
presence of the alkaline amniotic fluid
Ferning. Placing a sample on a microscopic slide, air drying, and examining for
ferning.
16.Clinical and laboratory diagnosis of the fetal distress
pathological state of the fetus caused by decreased oxygen and nutrients leading to
disruption of metabolic activity and fetal growth.
It can be installed during pregnancy (Chronic fetal distress) or labor (Acute fetal distress).
Etiological factors:
Diseases associated in decreased maternal blood oxygen;
Vasculo-renal syndrome;
Fetal malformations;
prematurity;
Placenta praevia;
Prolabare cord;
Dystocia
Premature rupture of membranes;
Maneuvers to extract the fetus;
Diagnostic:
Major clinical signs of fetal distress in labor are:
Impaired fetal heart rate;
Green staining in amniotic fluid
10
More findings:
recording fetal heart rate in fetal distress suggests that:
heart rate is higher than 180 beats / min
heart rate is less than 120 beats / min
fetal heart rate is fixed
Late decelerations are present in fetal anoxia or variable decelerations
in cord pathology.
17.Induction of labor
Induction of labor is the attempt to begin labor in a nonlaboring patient, whereas
augmentation of labor is intervening to increase the already present contractions.
Labor is induced with :
Prostaglandins
oxytocic agents
mechanical dilation of thecervix, and/or artificial rupture of membranes.
The indications for induction are based on either maternal, fetal, or fetoplacental reasons.
Common indications:
postterm pregnancy
preeclampsia
premature ROM
nonreassuring fetal testing
intrauterine growth restriction
The success of an induction (defined as achieving vaginal delivery) is often correlated with
favorable cervical status as defined by the Bishop score. A Bishop score of 5 or less may
lead to a failed induction.
The total score is achieved by assessing the following five components on vaginal
examination
cervical dilation
Cervical effacement
Cervical consistency
Cervical position
Fetal station
Each components is given a score of 0-2 or 0-3. The highest possible score is 13.
There are both maternal and obstetric contraindications for the use of prostaglandins.
Maternal reasons include asthma and glaucoma. Obstetric reasons include having had more
than one prior cesarean section and nonreassuring fetal testing.
Labor may also be induced by amniotomy. Amniotomy is performed with an amnio hook
that is used to puncture the amniotic sac around the fetus and release some of the amniotic
fluid. After the amniotomy is performed, a careful examination should be performed to
ensure that prolapse of the umbilical cord has not occurred. When performing amniotomy, it
is important not to elevate the fetal head from the pelvis to release more of the amniotic
fluid because this may lead to prolapse of the umbilical cord beyond the fetal head.
18.Management of labor and delivery
Management
Eating or drinking during labour is an area of ongoing debate. While some have argued that eating
in labour has no harmful effects on outcomes, others continue to have concern regarding the
increased possibility of an aspiration event (choking on recently eaten foods) in the event of an
11
emergency delivery due to the increased relaxation of the esophagus in pregnancy, upward pressure
of the uterus on the stomach, and the possibility of general anesthetic in the event of an emergency
cesarean. A 2013 Cochrane review pointed out that in recent years, obstetrical anaesthesia has
changed considerably, with better general anaesthetic techniques and a greater use of regional
anaesthesia and reported "no benefits or harms of restricting foods and fluids during labour in
women at low risk of needing anaesthesia." The review suggested "fasting does not guarantee an
empty stomach or less acidity" and that "poor nutritional balance may be associated with longer and
more painful labours." The review concluded that "women should be free to eat and drink in labour,
or not, as they wish."
Active management
Active management of labour consists of a number of care principles, including frequent assessment
of cervical dilatation. If the cervix is not dilating, oxytocin is offered. This management results in a
slightly reduced number of caesarean births, but does not change how many women have assisted
vaginal births. 75% of women report that they are very satisfied with either active management or
normal care.
Pain control
Non pharmaceutical
Some women prefer to avoid analgesic medication during childbirth. They can still try to alleviate
labour pain using psychological preparation, education, massage, acupuncture, TENS unit use,
hypnosis, or water therapy in a tub or shower. Some women like to have someone to support them
during labour and birth, such as the father of the baby, a family member, a close friend, a partner, or
a doula. The human body also has a chemical response to pain, by releasing endorphins. Endorphins
are present before, during, and immediately after childbirth. Some homebirth advocates believe that
this hormone can induce feelings of pleasure and euphoria during childbirth, reducing the risk of
maternal depression some weeks later.
Water birth is an option chosen by some women for pain relief during labour and childbirth, and
some studies have shown waterbirth in an uncomplicated pregnancy to reduce the need for
analgesia, without evidence of increased risk to mother or newborn. Hot water tubs are available in
many hospitals and birthing centres.
Meditation and mind medicine techniques are also used for pain control during labour and delivery.
These techniques are used in conjunction with progressive muscle relaxation and many other forms
of relaxation for the mind and body to aid in pain control for women during childbirth.
The injection of small amounts of sterile water into or just below the skin at several points on the
back has been a method tried to reduce labor pain, but no good evidence shows that it actually
helps.
Pharmaceutical
Different measures for pain control have varying degrees of success and side effects to the woman
and her baby. In some countries of Europe, doctors commonly prescribe inhaled nitrous oxide gas
for pain control, especially as 50% nitrous oxide, 50% oxygen, known as Entonox; in the UK,
midwives may use this gas without a doctor's prescription. Pethidine (with or without
promethazine) may be used early in labour, as well as other opioids such as fentanyl, but if given
too close to birth there is a risk of respiratory depression in the infant.
Popular medical pain control in hospitals include the regional anesthetics epidurals (EDA), and
spinal anaesthesia. Epidural analgesia is a generally safe and effective method of relieving pain in
labour, but is associated with longer labour, more operative intervention (particularly instrument
delivery), and increases in cost. Generally, pain and cortisol increased throughout labour in women
without EDA. Pain and stress hormones rise throughout labour for women without epidurals, while
12
pain, fear, and stress hormones decrease upon administration of epidural analgesia, but may rise
again later. Medicine administered via epidural can cross the placenta and enter the bloodstream of
the fetus. Epidural analgesia has no statistically significant impact on the risk of caesarean section,
and does not appear to have an immediate effect on neonatal status as determined by Apgar scores.
19.Episiotomy. Perineum repair
Definition
An is epiostomy an incision of the perineum made to enlarge the vaginal outlet to
facilitate delivery.
It is made at the end of the second stage of labor just before delivery, when
indicated.
It increases the area of the outlet for the fetal head during delivery,
particularly in assisted deliveries with forceps or the vacuum extractor.
Function
An episiotomy is used to prevent major perineal lacerations.
Prophylactic episiotomy has been advocated to prevent pelvic relaxation, although
this has never been proven.
Types
Median or medialy. This incision should be one-half the length of the distended
perineum and is cut vertically in the midline of the perineal body.
Advantages: less blood loss, easier to repair, more comfortable during
healing
Disadvantage: possible occurrence of inadvertent cutting or extension into
the anal sphincter and rectum. It is important to recognize and repair this
complication during repair of the episiotomy so that rectovaginal fistula does
not result.
Mediolateral . This incision of the perineum, at a 45-degree angle to the hymenal
ring, extends laterally to the anus onto the inner thigh, allowing more room than a
median incision.
Advantage: more room with less risk of injury to the rectum and sphincter
Disadvantages: more difficult to repair, more blood loss, more discomfort
during healing
There are four degrees of vaginal or perineal lacerations:
First-degree lacerations involve the , perineal skin, and vaginal mucosa.
Second-degree lacerations involve the skin, mucosa, fascia, and muscles of the
perineal body
Third-degree lacerations involve the anal sphincter.
Fourth-degree lacerations involve the rectal mucosa to expose the lumen of the
rectum.
indications:
large size baby
preterm baby
breech delivery
direct -occipitio posterior
Perianal Repair :
First and second degree repair :
Some first degree tears will not require suturing and second will require one
or two interrupted suture ,non –locking suture technique to oppose each layer
(vaginal epithelium, perineal muscle and skin) is associated with less short
term pain.
Third and fourth repair:
Adequate muscle relaxation with regional or general anesthesia is essential.
As the anal sphincter (levator ani muscle) is normally in a state of tonic
13
contractions. A suture is made in order to bring the muscle ends together,
using an absorbable synthetic suture if possible to do it as subcutaneous
stitch.
20.Complications of the IIIrd stages of labor
AND
21.Complications of the IVth stages of labor
Abnormal placental
Placenta acreta describe any placental implantation there is abnormal adherence of
placenta villous placental penetration time of the superficial portion of the
myometrium.
Placental increta is characterized by invading myometrium curled across its
thickness.
Placenta percreta is characterized by invasion of myometrium and overcome it,
reaching up to serous.
Retained placenta
The placenta remains inside the uterus for longer than 30 minutes after delivery of
the baby, usually due to one or more of the following:
Uterine contractions may be inadequate to expel the placenta
The cervix might have retracted too fast and partially closed, trapping the
placenta in the uterus
The bladder may be full and obstructing placental delivery.
Postpartum hemorrhage (PPH)
is the loss of more than 500 ml of blood following delivery of the baby. Most
bleeding comes from where the placenta was attached to the uterus, and is bright or
dark blood and usually thick. PPH occurs when the uterus fails to contract well,
usually due to:
Partially separated placenta (it remains partly attached to the uterine wall
Completely separated placenta, but retained inside the uterus
Atonic uterus; the muscular wall of the uterus could not contract powerfully
enough to arrest the natural bleeding which occurs when the placenta
separates.
Uterine inversion
The uterus is pulled ‘inside out’ as the baby or the placenta is delivered, and partly
emerges through the vagina.
Etiology
factors predisposing
Strong traction on the umbilical cord
Relaxation of uterine fundus
Traction on the bottom of the uterus by placental weight
Maneuvers by pressing the bottom of uterine
placenta acreta
22.Manual extraction of the placenta
The diagnosis of retained placenta is made when the placenta does not deliver within 30
minutes after the infant.
Procedure:
The retained placenta may be removed by manual extraction.
A hand is placed in the intrauterine cavity and the fingers used to shear the placenta
from the surface of the uterus .
If the placenta cannot be completely extracted manually, a curettage is performed to
ensure no products of conception (POC) are retained.
Causes of retained placenta include:
Weak or insufficient uterine contractions:
14
Uterine anomalies:
Hormonal Causes: During childbirth, the hormone oxytocin is released into the
blood. Oxytocin is responsible for uterine muscle contractions.
Complication
lose a large amount of blood
severe infection
fertility issues.
23.Manual and instrumental curettage of the uterine cavity
Dilation (or dilatation) and curettage (D&C) refers to the dilation (widening/opening) of
the cervix and surgical removal of part of the lining of the uterus and/or contents of the
uterus by scraping and scooping (curettage). It is a therapeutic gynecological procedure as
well as a rarely used method of first trimester abortion.
D&C normally refers to a procedure involving a curette, also called sharp curettage.
However, some sources use the term D&C to refer more generally to any procedure that
involves the processes of dilation and removal of uterine contents, which includes the more
common suction curettage procedures of manual and electric vacuum aspiration.
Procedure
An illustration of a Dilation and Curettage
The first step in a D&C is to dilate the cervix, usually done a few hours before the surgery.
The woman is usually put under general anesthesia before the procedure begins. A curette, a
metal rod with a handle on one end and a sharp loop on the other, is inserted into the uterus
through the dilated cervix. The curette is used to gently scrape the lining of the uterus and
remove the tissue in the uterus. This tissue is examined for completeness (in the case of
abortion or miscarriage treatment) or pathologically for abnormalities (in the case of
treatment for abnormal bleeding).
Clinical uses
D&Cs are commonly performed for the diagnosis of gynecological conditions leading to
'abnormal uterine bleeding'; to resolve abnormal uterine bleeding (too much, too often or too
heavy a menstrual flow); to remove the excess uterine lining in women who have conditions
such as polycystic ovary syndrome (which cause a prolonged buildup of tissue with no
natural period to remove it); to remove tissue in the uterus that may be causing abnormal
vaginal bleeding, including postpartum retained placenta; to remove retained tissue (also
known as retained POC or retained products of conception) in the case of a missed or
incomplete miscarriage; and as a method of abortion that is now uncommon. In contrast,
D&C remains 'standard care' for missed and incomplete miscarriage in many countries
despite the existence of alternatives currently used for abortions.
Because medical and non-invasive methods of abortion now exist, and because D&C
requires heavy sedation or general anesthesia and has higher risks of complication, the
procedure has been declining as a method of abortion. The World Health Organization
recommends D&C as a method of surgical abortion only when manual vacuum aspiration is
unavailable. Most D&Cs are now carried out for miscarriage management and other
indications such as diagnosis.
Hysteroscopy is a valid alternative to D&C for many surgical indications from diagnosis of
uterine pathology to the removal of fibroids and even retained products of conception. It
poses less risk because the doctor has a view inside the uterus during surgery, unlike with
blind D&C.
15
Medical management of miscarriage and medical abortion using drugs such as misoprostol
and mifepristone are safe, non-invasive and cheaper alternatives to D&C.
Complications
Complications may arise from either the introduction or spreading of infection, adverse
reaction to general anesthesia required during the surgery or from instrumentation itself, if
the procedure is performed blindly (without the use of any imaging technique such as
ultrasound or hysteroscopy).
One risk of sharp curettage is uterine perforation. Although normally no treatment is
required for uterine perforation, a laparoscopy may be done to verify that bleeding has
stopped on its own. Infection of the uterus or fallopian tubes is also a possible complication,
especially if the woman has an untreated sexually transmitted infection.
Another risk is intrauterine adhesions, or Asherman's syndrome. One study found that in
women who had one or two sharp curettage procedures for miscarriage, 14-16% developed
some adhesions. Women who underwent three sharp curettage procedures for miscarriage
had a 32% risk of developing adhesions. The risk of Asherman's syndrome was found to be
30.9% in women who had D&C following a missed miscarriage, and 25% in those who had
a D&C 1–4 weeks postpartum. Untreated Asherman's syndrome, especially if severe, also
increases the risk of complications in future pregnancies, such as ectopic pregnancy,
miscarriage, and abnormal placentation (e.g.placenta previa and placenta accreta).
According to recent case reports, use of vacuum aspiration can also lead to intrauterine
adhesions.
24.Transverse lie. Internal version
Definition
At the end of pregnancy or during of labor, champ of pelvic inlet is not fetal head or
fetal breech
Variety
shoulder right in dorso-anterior
shoulder left in dorso-anterior
shoulder right in dorso-posterior
shoulder left in dorso-posterior
Etiology
Mistake of accommodation: the grand cause of transverse position is multipara (relax
of uterine wall)
Other cause can hydramnios, previa tumor, shortness umbilical cord
Uterine malformation
Internal Version
(is an obstetric procedure wherein the fetus is turned within the uterus such that one
or both feet present through the cervix during childbirth. It is used most often in
cases where the fetus in transverse lie or in another abnormal position in the uterus)
the foot is grasped and pulled gently and continuously into the birth canal
Indicaations:
intrauterine to transfere the transverse lie to breech
only in twin delivery in cephalic presentation
multipara with small baby
conditions for internal version:
membrane must be intact
full dilatation of the cervix
16
normal maternal bony pelvis
a live fetus
general anesthesia for uterine relaxation
Causes of transverse:
multipara
polyhydramnios
short cord
25.Fetal extraction ???
26.Caesarian section
Cesarean section is delivery of a viable fetus through an abdominal incision (laparotomy) and
uterine incision (hysterotomy).
Indications
Contraindications to labor
Placenta previa
Vasa previa
Previous classic cesarean section
Previous myomectomy with entrance into the uterine cavity
Previous uterine reconstruction
Malpresentations of the fetus
Active genital herpes infection
Dystocia and failed induction of labor
Cephalopelvic disproportion, failure to descend, or arrest of descent or
dilation
Failure to progress in normal-size infant, usually because of fetal malposition
or posture
Failed forceps or vacuum extractor delivery
Certain fetal malformations that may obstruct labor (i.e.,large
hydrocephalus,sacrococ-cygeal tumor)
Emergent conditions that warrant immediate delivery
Abruptio placentae with antepartum or intrapartum hemorrhage
Umbilical cord prolapsed
Nonreassuring antepartum or intrapartum fetal testing
Intrapartum fetal acidemia, with intrapartum scalp pH of less than 7.20
Uterine rupture
Impending maternal death
Types of cesarean operations
Cesarean operations are classified according to the orientation (transverse or vertical) and
the site of placement (lower segment or upper segment) of the uterine incision.
Low transverse (Kerr). The low transverse uterine incision is the preferred incision
and the one most frequently used today.
Low vertical (Sellheim). The vertical incision begins in the noncontractile lower
segment but usually extends into the contractile upper segment.
Classic incision (Sanger). The classic incision is a longitudinal incision in the
anterior fundus.
Procedure
Anesthesia. Most often, anesthesia is regional (spinal or epidural), but it can be
inhalational (general) as dictated by the individual situation. Surgical techniques
Abdominal incision
The abdominal incision maybe midline, paramedian, or Pfannenstiel.
Uterine incision
17
The pregnant uterus is palpated and inspected for rotation. The type of
uterine incision is selected depending on development of the lower uterine
segment, presentation of the infant, and placental location.
Complications
Common postoperative complications include the following conditions:
Endomyometritis. Postoperative infection is the most common complication
after cesarean section.
Urinary tract infection
Wound infection
Thromboembolic disorders
Cesarean hysterectomy
Uterine rupture in future pregnancies
27.Postpartum period in caesarian section
-
Considerations. The risks of a vaginal birth after cesarean section, when performed in the
proper setting, are less than the risks of a repeat cesarean section.
A previous vaginal delivery is the best prognostic indicator for success.
Women with nonrecurring indications (e.g., breech presentation, fetal distress, or
hemorrhage) have higher success rates than women with recurring indications (e.g.,
previous cephalopelvic disproportion or failure to progress)
Prerequisites
No maternal or fetal contraindications to labor
Previous low transverse cesarean section, with documentation of the uterine scar
Informed consent regarding risks and benefits of repeat cesarean and vaginal birth
Personnel able to perform emergency delivery and appropriate facility
Contraindications. The risk of vaginal birth after cesarean section in multiple gestations
and breech presentations has not been determined.
Previous classic uterine incision
Maternal or fetal contraindications to labor
Trial of labor declined by mother
Previous low vertical scar, unless absence of upper segment extension is well
documented
History of more than two prior cesarean sections
Extra informations:
As more than 30% of deliveries are now by cesarean, wound care and pain management in
these women are a common component of postpartum care. Local wound care and
observation for signs of wound infection or separation are part of routine care. Wound
infections include cellulitis or a wound abscess. Wound separations can be at the level of the
skin or subcutaneous tissue or deeper at the level of the rectus fascia known as a wound
dehiscence. Pain is usually managed with opioids that can contribute to a postoperative ileus
or constipation. Patients on opioids should therefore be prescribed stool softeners and
occasionally laxatives. NSAIDs should be used concomitantly for the cramping pain caused
by uterine involution. Patients have usually received a first- or second generation
cephalosporin during the cesarean section as prophylaxis against infection. Although it is
routine in many institutions to give additional dosages, this has never been shown to further
decrease the risk of infection.
28.Forceps application
These are metal instruments used to provide traction , rotation , or both to the fetal head.
Simpson: used for traction only
Kjelland : used for head rotation and traction
Piper : used for the after – coming head of a vaginal breech baby
18
Barton : used to deliver the head in occiput transverse position with a platypelloid
pelvis
Indication
Prolonged second stage : may be because of dysfunctional labor, this is the most
indication for forceps
Avoid the maternal pushing : like in cardiac , pulmonary or neurologic disorders
Breech presentation: shorten time to deliver the head of a vaginal breech fetus.
Prerequisites
Clinically adequate pelvic dimensions
Experienced operator
Full cervical dilation
Engaged fetal head
Orientation of fetal head is certain
Complication
Maternal : lacerations to the vagina , cervix , perineum and uterus
Fetal- neonatal : soft tissue injury caused bu incorrectly placed forceps blades
29.Normal puerperium
This period of 4 to 6 weeks starts immediately after delivery and ends when the reproductive
tract has returned to its nonpregnant condition.
Involution of the uterus. The uterus regains its usual nonpregnant size within 5 to 6 weeks,
shrinking from 1000 g immediately postpartum to 100 g. Breastfeeding accelerates
involution of the uterus because stimulation of the nipples releases oxytocin from the
neurohypophysis; the resulting contractions of the myometrium facilitate the involution of
the uterus.
Involutional changes of the renal system. The puerperal bladder has an increased capacity
and a relative insensitivity to intravesical fluid pressure.
Anatomic changes, such as the dilation of the calyces, renal pelvis, and ureters, that are
characteristic of pregnancy may persist as long as 8 weeks postpartum.
Cardiovascular changes. The changes that occurred during pregnancy (e.g., increases in
heart rate, cardiac output, and blood volume) generally return to baseline by approximately
6 weeks postpartum
Blood. A marked leukocytosis occurs during and after labor.
Ovulation and menstruation
Nonlactating women. The first menstrual flow usually returns within 6 to 8 weeks
after delivery, with ovulation occurring at 2 to 4 weeks postpartum.
Lactating women. Ovulation is much less frequent in women who breast feed
compared with those who do not. The first menstrual flow may occur as early as the
second month or as late as the 18th month after delivery.
Amenorrhea during lactation is due to a lack of appropriate ovarian stimulation by
pituitary gonadotropins.
30.Pathological puerperium
The most common complications include hemorrhage, genital tract infections, urinary tract
infections, and mastitis.
Postpartum hemorrhage is defined as a blood loss in excess of 500 mL during the first 24
hours after delivery.
Causes
Failure of compression of blood vessels at the implantation site of the
placenta because of:
An atonic uterus due to general anesthesia; overdistension of the
uterus from a large fetus, hydramnios (excess amniotic fluid), or
multiple fetuses; prolonged labor; very rapid labor; high parity; or a
19
labor vigorously stimulated with oxytocin. The most common cause
of postpartum hemorrhage is uterine atony.
Retention of placental tissue, as seen in placenta accreta, a
succenturiate placental lobe, or a fragmented placenta
Trauma to the genital tract because of:
Episiotomy
Lacerations of the cervix, vagina, or perineum
Rupture of the uterus
Coagulation defects,as seen in hypofibrinogenemia or thrombocytopenia
Management should be directed at the underlying cause(s)
Vigorous massage of the uterine fundus for uterine atony
Use of uterine contracting agents for uterine atony
Oxytocin Prostaglandin Methylergonovine
Manual exploration of the uterine cavity for retained placental fragments or
uterine rupture
Inspection of the cervix and vagina for lacerations
Curettage of the uterine cavity
Hypogastric artery ligation; embolization of the uterine vessels; and, rarely,
hysterectomy
Puerperal infection is defined as any infection of the genitourinary tract during the
puerperium accompanied by a temperature of 38 c or higher that occurs for at least 2 of the
first 10 days postpartum, exclusive of the first 24 hours. Prolonged rupture of the
membranes accompanied by multiple vaginal examinations during labor is a major
predisposing cause of puerperal infection.
Pelvic infections
Endometritis (childbed fever), the most common form of puerperal infection,
involves primarily the endometrium and the adjacent myometrium.
Parametritis, infection of the retroperitoneal fibroareolar pelvic connective
tissue
Thrombophlebitis results from an extension of puerperal infection along
pelvic veins.
Urinary tract infections are common during the puerperium because of:
Trauma to the bladder from a normal vaginal delivery
A hypotonic bladder from conduction anesthesia
Catheterization.
Management
Antibiotics should be administered. Broad-spectrum antibiotics, which
include anaerobic coverage, are recommended for those pelvic infections in
which identification of the offending organism is impossible.
31.Cardinal symptoms in gynecology: pain
Pain
1. Spontaneous acute pain
a. without fever:
In case of acute pain in pelvis without pain in a young women who had a normal
menstrual cycle (without abnormalities) the doctor think first about a rupture
because of an ectopic pregnancy it can also be acute torsion or an ovarian cyste.
b. with fever:
Pelvic pain with fever we think first about salpingite (appendicite can also be
evocated).
2. Intermenstruel syndrome: (in the middle of the cycle)
Pelvic pain irradiate to the vulva and vagina ; sometimes to the lower back and all
the abdomen can be associated with nausea and vomiting ;with leukorrhea and
vaginal bleeding.
20
Occure usualy in the ovulation periode between 12and 16 days it can last from few
hours till 48 hours.
3. Dyspareunia
Pain wich occure in sexual act in womens it can be superficiel or deep with the
penetration it can be primary (the first act)or secondary(in all the sexual acts)
It can be caused about:
Vaginal infections :mycoses; herpes;tricomonas vaginalis…
malformations ;hormonal deficiencies
endometriosis
vaginal dryness (decresing of oestrogene in premenaupose)
And it can be psychiatrique desease the treatment is related with the pathologie.
4. Vaginismus
The vaginismus is a involontary contracture wich is spasmodic of the musculature of
the vulva and the perineum it occurs during the penetration in the vagina and stop it
or make it very painfull.we call it primary if occurs in the first sexual act or
secondary if its appear after a period of time of normal sexual acts.
No gynocological exam is possibl .
Sometimes the etiologie is organic:
local erosions
vulvovaginitis
menopause
herpes or eczema of the vulva
hemorroidaire anal fissure or no.
But In the most of the cases its psychological desease.
32.Cardinal symptoms in gynecology: bleeding
Bleeding
an abnormal condition in which blood is passed from the vagina other than during the
menses or abnormality in menses. It may be caused by abnormalities of the uterus or cervix,
an abnormal pregnancy, endocrine abnormalities, abnormalities of one or both ovaries or
one or both fallopian tubes, or an abnormality of the vagina.
Abnormal Uterine Bleeding
Defined as alteration of normal flow
Dysfunctional uterine bleeding (DUB) is most common cause of abnormal uterine bleeding
prior to menopause
Heavy, prolonged or inter-menstrual
Terms used in abnormality menses
Menorrhagia: excess menstrual bleeding
Hypomenorrhea: decreased menstrual bleeding
Polymenorrhea: increased frequency of menstruation
Metrorrhagia: uterine bleeding in between menstruation
Etiology
Organic: coagulopathies, liver/renal disease, drugs (steroids, chemo & Coumadin),
obesity and endocrine abnormalities (thyroid, diabetes & adrenal)
Uterine: leiomyomas, polyps, endometrial hyperplasia, PID, IUD, pregnancy,
cancers & endocrine active tumors
Non organic: persistent ovulatory failure, the most common cause is the continuous
acyclic estrogen production leading to anovulation and endometrial proliferation
DUB is the most common cause of bleeding in adolescent & young adults
Dysfunctional Uterine Bleeding
Pathology is excluded
Most patient anovulatory
May be related to hypothalamic-pituitary axis resulting in continued estrogenic stimulation
of the endometrium
21
The endometrium outgrows its blood supply partially breaks down bleeding occurs
in irregular manner
Organic causes (thyroid, adrenal must be excluded)
Diagnosis - based on:
history
absence of ovulatory temperature changes
low serum progesterone
result of endometrial sampling in the older woman
Post Menopausal Bleeding
always abnormal and is Cancer until proven otherwise
requires a Definitive Diagnosis and if chronic, re-evaluate Every Year
Diagnosis
History: Previous customary cycles, episode of irregular bleeding, heavy bleeding
Exam: Pelvic for possible sites of internal bleeding (vaginal / rectal), uterine or
adnexal enlargement
Endometrial biopsy may be required
Possible D&C and hysteroscopy may be helpful.
33.Cardinal symptoms in gynecology: amenorrhea
Defined as failure of menarche by age 16 regardless of development or the absence of
menstruation for 3-6 months after menarche
Two different types: primary & secondary
Primary Amenorrhea
Failure of development by 14 years of age
Failure of menses by 16 years of age regardless of development
Secondary to chromosomal (Turners 45XO) genital agenesis/congenital
abnormalities (absent vagina or imperforated hymen), failure of pituitaryovarian axis
Secondary Amenorrhea
Failure to menstruate for 3-6 months or 3 cycles after menarche
Ovarian failure most common i.e.: menopause, but can be premature
Outflow tract obstruction
Etiology: Causes divided into ovulatory and anovulatory
Ovulatory: results from anatomic genital abnormalities with normal hormonal function
Reproductive Outflow Disorders:
Mullerian agenesis - absence of either vagina or uterus
Imperforated hymen
Vaginal and uterine aplasia
Cervical stenosis
Intra-uterine adhesions (Asherman’s syndrome naturally or surgical
etiology)
Anovulatory: in which both ovulation and menses are absent (is most common)
Ovarian Disorders:
Chronic anovulation/ Autoimmune disorders/Gonadal dysgenesis/Premature
ovarian failure
Pituitary Disorders:
Hyperprolactinemia/ Various tumors/ Pituitary insufficiency
Hypothalamic Disorders:
Functional- Exercise, stress anorexia/ obesity/ Neoplastic lesions
Diagnosis
Exam: Neuro for possible intracranial lesions, Pelvic (limited external in
adolescent)Secondary sex characteristics
pregnancy testing (hCG) / measurement of hormone levels {Prolactin,TFT (T3/T4/TSH) ,LH/FSH,
Estrogen/progesterone}
22
progesterone challenge: - If bleeding occurs, the cause is chronic anovulatory or oligo-ovulatory
-If no withdrawal bleeding, the cause is either a low estrogen state
of anatomic
Treatment
Aims to correct any underlying disorder and minimize excess androgenic effects
Depends on the basic cause
Goal to induce menstrual flow 3-4 /year
Surgical - for any lesion/tumors/defects
80-90% of CNS or pituitary tumors will need resection
Absent genital: cosmetic surgery, but will never be functional
Pharmacological - wide range usually long term
Hypothalamic disorder - behavior or lifestyle changes
Treat any hypothyroid and hyperprolactinimia with surgery &/or Parlodel.
34.Cardinal symptoms in gynecology: vaginal discharge
Vaginal discharge is a fluid produced by glands in the vaginal wall and cervix that drains from the
opening of the vagina. The amount and appearance of normal vaginal discharge varies throughout
the menstrual cycle. An increase in the amount of vaginal discharge, an abnormal odor, colour,
consistency of the fluid, or pain that accompanies vaginal discharge can all be signs of infection or
other disorders.
The normal pH in vaginal secretions is usually <4.5
Examples
Thrush (Yeast Infection): the most common non-sexual acquired infection, usually caused
by candida species, gives a thick, white, lumpy discharge,that looks like cheese. often
associated with marked vulval itching.
Bacterial Vaginosis: usually caused by Gardnerella vaginalis,produces a watery,fishysmelling discharge.pH >5
Trichomoniasis: causes a vaginal discharge that is yellow-green, foamy, and bad smelling
Diagnosis
Speculum examination
Vaginal culture for bacterial or candidiasis
Gram stain to determine the relative concentration of lactobacilli
The affirm test -> to detect the bacteria ‘trichomonal vaginitis’
Testing of vaginal fluid for pH, odor
Treatment
Antibiotics: Metronidazole, usually for 7 days.
35.Cervical and endometrial neoplasm – screening, HPV-CIN, Pap smear
Pap Smear
is a screening test used for the detection and diagnosis of various infections, abnormal
hormonal activities, and pre-cancerous and cancerous processes in the endocervical canal.
Characteristics:
It is an excellent test, but not perfect in preventing cervical carcinoma
detect treatable premalignant lesions
not a good test for glandular lesions, which are the most common form of uterine
cancer
In taking a Pap smear, a speculum is used to open the vaginal canal and allow the collection of
cells with a plastic spatula and small brush from the outer opening of the cervix of the uterus
and the endocervix. The cells are examined under a microscope to look for abnormalities. The
test aims to detect potentially pre-cancerous changes (called cervical intraepithelial neoplasia
(CIN) or cervical dysplasia), which are usually caused by sexually transmitted human
papillomaviruses. The test may also detect infections and abnormalities in the endocervix and
endometrium.
23
Conditions for conducting
Avoid sexual intercourse 24 hours before
sampling takes place outside the period, outside local infection and preferably in the
mid-cycle
speculum is inserted without lubricant or disinfectant
Material:
Spatula, small brush, glass slides
fixative - alcohol-ether in equal or spray
Abnormal Results: include:
Squamous cell abnormalities (SIL)
Atypical squamous cells of undetermined significance
Low-grade squamous intraepithelial lesion
Atypical squamous cells
High-grade squamous intraepithelial lesion
Squamous cell carcinoma
Glandular epithelial cell abnormalities
Atypical Glandular Cells not otherwise specified
Endocervical and endometrial abnormalities can also be detected, as can a number
of infectious processes, including yeast, herpes simplex virus and trichomoniasis.
However it is not very sensitive at detecting these infections, so absence of detection
on a Pap does not mean absence of the infection.
Classification of Pap
Class I- absence of abnormal or atypical cells
Class II-a - atypical cytology but no evidence for malignancy
Class III-a - cytology suggestive but inconclusive for malignancy
Class IV-a - cytology strongly suggestive for malignancy
Class V-a - cytology conclusive for malignancy
36.Vaginal smear
Vaginal Smear (Wet Mount)
Smear taken from the vaginal mucosa for cytological analysis
It is used to find the cause of vaginitis or vulvitis
Indications
May be considered in case of vaginitis symptoms such as: vaginal itching, burning, rash,
odor, or discharge
It may assist in suspicion of vaginal yeast infection, trichomoniosis, and bacterial vaginosis
Method
Is not done during menstrual period, because menstrual blood can affect the results
Vaginal irrigation, tampon use or sex (disrupting the pH) should be avoided for 24 hours
before the test
Antibiotics treatment is not administered at least 8 days before.
The sampling is done with the patient in lithotomy position. A speculum is used to facilitate
use of a swab or spatula to sample fluid inside the vagina. The sampling procedure may
cause some discomfort and minor bleeding, but otherwise there are no associated risks. The
sample is then smeared upon a microscope slide and is observed by wet mount microscopy
by placing the specimen on a glass slide and mixing with a salt solution.
37.Colposcopy
is a medical diagnostic procedure to examine an lighted, magnified view of the cervix and
the tissues of the vagina and vulva.
It is done using a colposcope, which provides an enlarged view of the areas, allowing the
physician to visually distinguish normal from abnormal appearing tissue and take directed
biopsies for further pathological examination.
24
The main goal of colposcopy is to prevent cervical cancer by detecting precancerous lesions
early and treating them.
EXTRA: is a binocular operating microscope with magnification of between 5- and 20 times. It
has been used to examine the cervix in details to identify CIN and pre-clinical invasive cancer.
Indications
Most patients undergo a colposcopic examination to further investigate a cytological
abnormality on their pap smears. Other indications for a patient to have a colposcopy
include:
assessment of diethylstilbestrol (DES) exposure in utero,
immunosuppression such as HIV infection, or an organ transplant patient
an abnormal appearance of the cervix as noted by a primary care provider
as a part of a sexual assault forensic examination done by a Sexual Assault Nurse
Examiner
Procedure
Colposcopy is performed with the patient in dorsal lithotomy position. A speculum is placed
in the vagina after the vulva is examined for any suspicious lesions.
The cervix is first examined for abnormal vessel patterns known to be associated with
premalignant and malignant lesions of the cervix.
To assist in the identification of abnormal vessels, the cervix may be washed with normal
saline and may be viewed through a green filter, which highlights the blood vessels as black
lines.
3 to 5% acitic acid to the area highlight CIN as white compaired with the pink of the
squamous epithelium
Colposcopic direct biopsy will be taken from the most abnormal areas of the epithelium to
confirm the Diagnosis
Lahm-schiller test will be used and biopsy for the suspected areas
Following any biopsies, an endocervical curettage (ECC) is often done.
Complications
Significant complications from a colposcopy are not common, but may include bleeding,
infection at the biopsy site or endometrium, and failure to identify the lesion.
38.Lahm-schiller test
is a medical test in which iodine solution is applied to the cervix in order to diagnose
cervical cancer (squamous cell carcinoma).
Lugol's iodine solution is applied to the cervix under direct vision.
Stratified squamous epithelial cells are rich in glycogen and stained by iodine fixation in
brown, whereas abnormal areas, such as early cervical cancer, do not take up the stain, and
appearing as white areas with net margins - Iodine negative areas.
Lahm-Schiller's test is not specific for cervical cancer, other iodine-negative areas include:
ectopia, erosions, ulcers, dysplasia, areas of inflammation, neoplasms.
The abnormal areas can then be biopsied and examined histologically.
39.Biopsy
Biopsy is the procedure to collect a sampling of tissue for histopatholgical examination and
diagnosis
Vulvar Biopsy
Is done in order to collect tissue from the suspected lesions, i.e: infectious origin,
dystrophic or neoplastic at the vulva.
Biopsy is performed under local anesthesia with lidocaine 1%.
Using forceps biopsy
Selected fragment is cut with a scalpel
Haemostasis is achieved by applying a silver nitrate pencil, termocoagulare or often
by applying suture.
25
Vaginal Biopsy
It is achieved by selecting a biopsy forceps fragment from vaginal lesion and cut it
with knife.
The maneuver often requires local anesthesia with lidocaine 1% and followed with
hemostasis.
Suspicion of cancer (squamous cell carcinoma, adenocarcinoma)
Cervical Biopsy
a sample from the cervix is collected and analyzed by histopathology.
If suspicious lesions invisible to the naked eye indicates taking colposcopic control
after application of acetic acid and Lugol's solution (Lahm-schiller test)
Cervical conization
refers to a biopsy of the cervix in which a cone-shaped sample of tissue is
removed from the mucous membrane.
Conization may be used either for diagnostic purposes, or for therapeutic
purposes to remove pre-cancerous cells.
Conization of the cervix is a common treatment for dysplasia following
abnormal results from a pap smear.
Side effects of the treatment may include cervical stenosis with a resulting
severe endometriosis
Endometrial Biopsy
a small sample is collected from the lining of the uterus
using dilation and curettage D&C, then collect a small sample with a syringe or
suction.
The test is done to find the cause of:
Abnormal menstrual periods (heavy, prolonged, or irregular bleeding)
Bleeding after menopause
Bleeding from taking hormone therapy medications
Thickened uterine lining seen on ultrasound
Abnormal pap test
The test is usually done in women over age 35.
Abnormal results can be:
Endometrial cancer or precancer (hyperplasia)
Uterine fibroids, Uterine polyps, Infection, Hormone imbalance
Complications
Infection / Making a hole in (perforating) the uterus or tearing the cervix
(rarely)
Prolonged bleeding / Slight spotting and mild cramping for a few days.
40.Bioptic curettage
It is a painless and easy routine screening of the endometrium avoiding dilation and traction
of the uterus neck
It can be performed on the cervix and uterus with the help of anesthetic general or local
Uses: miscarriage, menstrual irregularities and biopsies
Endometrial biopsy by aspiration without dilation
This method of endometrial sampling easier and less painful than curettage of the
uterine cavity prior to expansion
Indication
detection of malignancy or endometrial hyperplasia
follow up patients on hormone therapy for endometrial hyperplasia
diagnosis of luteal failure
development of endometrial tissue cultures
Contraindications: Inflammation of the cervix or uterus
Endocervical curettage
Indication
26
for determining the extent of endocervical CIN
diagnosis of endocervical polyps, glandular hyperplasia, a chronic
endocervical
diagnosis of endocervical glandular dysplasia, CIS, or invasive carcinoma
setting behavior therapy in women with cervical dysplasia
Contraindications: in pregnant women
Fractional uterine curettage
Is a useful diagnostic and therapeutic method, frequently used in gynecology.
The main purpose of fractional uterine curettage is obtaining endometrial tissue for
diagnostic and histopathological endocol
Indication
unusual bleeding or abnormal uterine origin whose causes were not detected
by routine examinations
removing debris and placental ovulare for incomplete abortion
before a hysterectomy for a benign condition in order to exclude the
coexistence of malignancy
microscopic examination of the endometrium is useful for retrospective
diagnosis of ovulation.
41.Hysterometry
Hysterometry is a maneuver that measures the length of the uterine cavity and cervical canal
Can be done in certain conditions:
is made only in the first cycle, in the absence of local infection and pregnancy
first practice vaginally cough for determining the uterus position
Hysterometry is used in cm (Meigs), which has a concave curvature of the gradient.
The maneuver involves disinfection of the cervix and vagina with an antiseptic solution
Procedure
Upper lip of the cervix is caught with Pozzi forceps and traction exert a slight
decrease for anteflexed uterus.
The Hysterometry is inserted into the vagina and into the cervical canal with a slight
push motion without force.
Introducing of the Hysterometry should not be either painful or difficult.
Normal uterine cavity total length is 70-75 mm in nulliparous and 75-80 mm in multiparous.
If hysterometry cannot enter the uterine cavity, the following are taken into account:
a poor technique, an abnormality of the cervix, or a spasm at this level.
42.Hysterosalpingography
Hysterosalpingography is an x-ray of the uterus and fallopian tubes that involves the
injection of contrast (dye) through the cervix.
Uses: to see the structure of the uterus and fallopian tubes and to determine if there is any
blockage or other problems, it’s usually as a part of infertility examination
Abnormal results may indicate any of the following:
Developmental disorders of the structures of the uterus or fallopian tubes
Intrauterine adhesion
Obstruction of the fallopian tubes
Presence of foreign bodies
Scarring
Tubal adhesions
Uterine tumors or polyps
Risks
allergic reaction
infection like endometritis and salpingitis
perforation of the uterus
27
Contraindicated
vaginal bleeding
pelvic inflammatory diseases (PID)
43.Ultrasound in gynecology
Ultrasound of the uterus
In longitudinal section the uterus is a pear-shaped mass with greater upper extremity,
echogenic, homogeneous, with regular contours.
In cross section appears as a more oval uterus, myometrium is homogeneous, poorly
echogenic, and measures typically 2-3 cm.
The endometrium is poorly visible in the first week after menstruation, then
appearing as a low echogenic band that thickens progressively up to menstruation.
Uterine cavity, usually virtual, are viewed as a fine linear echoes the union of the
two girls endometrial.
Pathological changes of the uterus can be confirmed by echocardiography.
malformation, endometrial polyp, endometrial cancer
Uterine fibroids less echogenic than the myometrium, are easily detected and
measured, especially subserosal and earlier. Endometrial hyperplasia translates into
an area of endometrial thickening.
Intrauterine collections are viewed as a hypoecogenic areas in the uterine cavity.
Intrauterine pregnancy is confirmed by the presence of ovular sac surrounded by an echo
trophoblastic, and an embryo, after 6 weeks of amenorrhea abdominal and after 5 weeks of
amenorrhea intravaginal probe.
Ultrasound of the ovaries
Ovaries, most commonly latero-uterine, measuring 25-35 mm in length and 12-20
mm thick.
Ovarian pathology that can be appreciated at ultrasound is represented by serous
cysts, mucous, dermoid tumor or cancer.
Fallopian tubes, which normally can’t be clear in ultrasound, they may be
pathological cases such as: tubal pregnancy, hydrosalpinx, hematosalpinx,
pyosalpinx.
Indication of Ultrasound
suspected intrauterine pregnancy;
suspicion of ectopic pregnancy;
differential diagnosis between uterine fibroids and an ovarian pathology;
indication of organic or functional origin of adnexal masses;
specifying the structure of a liquid or solid tumor
examination of obese patients, which is inconclusive vaginal cough;
monitoring of ovulation induction treatment
44.Uterine curettage
Dilation and curettage (D&C) is a brief surgical procedure in which the cervix is dilated and
a special instrument is used to scrape the uterine lining.
Reasons for Dilation and Curettage
Remove tissue in the uterus during or after a miscarriage or abortion or to remove
small pieces of placenta after childbirth. This helps prevent infection or heavy
bleeding.
Diagnose or treat abnormal uterine bleeding. A D&C may help diagnose or treat
growths such as fibroids, polyps or endometriosis, hormonal imbalances, oruterine
cancer. A sample of uterine tissue is viewed under a microscope to check for
abnormal cells.
28
After a D&C, there are possible side effects and risks. Common side effects include:
Cramping
Spotting or light bleeding
perforation
45.Termination of pregnancy - voluntary or therapeutic
Therapeutic abortion is the intentional termination of a pregnancy before the fetus can live
independently
An abortion may be performed whenever there is some compelling reason to end a
pregnancy. Women have abortions because continuing the pregnancy would cause them
hardship, endanger their life or health, or because prenatal testing has shown that the fetus
will be born with severe abnormalities.
Abortions are safest when performed within the first 6 to 10 weeks after the last menstrual
period.
Complications from abortions can include:
uncontrolled bleeding
infection
blood clots accumulating in the uterus
a tear in the cervix or uterus
missed abortion where the pregnancy continues
incomplete abortion where some material from the pregnancy remains in the uterus.
-----------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------
Cervical screening is a way of preventing cervical cancer from developing, and diagnosing the disease at an early precancerous stage. In the USA, cervical screening is usually performed using the Pap test (or 'smear test'),
The Papanicolaou test (also called Pap smear, Pap test, cervical smear, or smear test) is a method of cervical
screening used to detect potentially pre-cancerous and cancerous processes in the endocervical canal (transformation
zone) of the female reproductive system. Unusual findings are often followed up by more sensitive diagnostic
procedures, and, if warranted, interventions that aim to prevent progression to cervical cancer. The test was invented by
and named after the prominent Greek doctor Georgios Papanikolaou.
In taking a Pap smear, a speculum is used to open the vaginal canal and allow the collection of cells from the outer
opening of the cervix of the uterus and the endocervix. The cells are examined under a microscope to look for
abnormalities. The test aims to detect potentially pre-cancerous changes (called cervical intraepithelial neoplasia (CIN)
or cervical dysplasia), which are usually caused by sexually transmitted human papillomaviruses. The test remains an
effective, widely used method for early detection of pre-cancer and cervical cancer. The test may also detect infections
and abnormalities in the endocervix and endometrium.
In general, in countries where Pap smear screening is routine, it is recommended that females who have had sex seek
regular Pap smear testing. Guidelines on frequency vary from every three to five years. If results are abnormal, and
depending on the nature of the abnormality, the test may need to be repeated in six to twelve months.[4] If the
abnormality requires closer scrutiny, the patient may be referred for detailed inspection of the cervix by colposcopy.
The patient may also be referred for HPV DNA testing, which can serve as an adjunct to Pap testing. Additional
biomarkers which may be applied as ancillary test with Pap test are evolving.
Human papillomavirus (HPV) is a DNA virus from the papillomavirus family that is capable of infecting humans.
Like all papillomaviruses, HPVs establish productive infections only in keratinocytes of the skin or mucous membranes.
While the majority of the known types of HPV cause no symptoms in most people, some types can cause benign
papillomas (such as warts [verrucae] or squamous cell papilloma), while others can in a minority of cases lead to
cancers of the cervix, vulva, vagina, penis, oropharynx and anus. HPV has been linked with an increased risk of
cardiovascular disease. In addition, HPV 16 and 18 infections are a cause of a unique type of oropharyngeal (throat)
cancer.
More than 30 to 40 types of HPV are typically transmitted through sexual contact and infect the anogenital region.
Some sexually transmitted HPV types may cause genital warts. Persistent infection with "high-risk" HPV types
different from the ones that cause skin warts may progress to precancerous lesions and invasive cancer. HPV infection
is a cause of nearly all cases of cervical cancer. However, most infections do not cause disease.
Most HPV infections in young women are temporary and have little long-term significance. Seventy percent of
infections are gone in one year and ninety percent in two years. However, when the infection persists in 5% to 10% of
infected women there is high risk of developing precancerous lesions of the cervix, which can progress to invasive
cervical cancer. This process usually takes 10–15 years, providing many opportunities for detection and treatment of the
29
pre-cancerous lesion. Progression to invasive cancer can be almost always prevented when standard prevention
strategies are applied, but the lesions still cause considerable burden necessitating preventive surgeries, which do in
many cases involve loss of fertility.
In more developed countries, cervical screening using a Papanicolaou (Pap) test or liquid-based cytology is used to
detect abnormal cells that may develop into cancer. If abnormal cells are found, women are invited to have a
colposcopy. During a colposcopic inspection, biopsies can be taken and abnormal areas can be removed with a simple
procedure, typically with a cauterizing loop or, more commonly in the developing world by freezing (cryotherapy).
Treating abnormal cells in this way can prevent them from developing into cervical cancer.
Pap smears have reduced the incidence and fatalities of cervical cancer in the developed world, but even so there were
11,000 cases and 3,900 deaths in the U.S. in 2008. Cervical cancer has substantial mortality in resource-poor areas;
worldwide, there are an estimated 490,000 cases and 270,000 deaths each year.
HPV vaccines (Cervarix and Gardasil), which prevent infection with the HPV types (16 and 18) that cause 70% of
cervical cancer, may lead to further decreases.
http://drddp.wordpress.com/
30