* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Cone Beam Computed Tomography for Adaptive
Survey
Document related concepts
Transcript
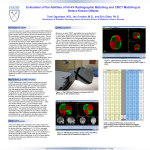
Journal of Medical and Biological Engineering, 34(4): 377-385 377 Cone Beam Computed Tomography for Adaptive Radiotherapy Treatment Planning Kavitha Srinivasan1,* Mohammad Mohammadi1,2 Justin Shepherd2 1 School of Chemistry and Physics, University of Adelaide, Adelaide, SA 5005, Australia Department of Medical Physics, Royal Adelaide Hospital, Adelaide, SA 5005, Australia 2 Received 21 Nov 2012; Accepted 23 Jan 2013; doi: 10.5405/jmbe.1372 Abstract Cone beam computed tomography (CBCT) images obtained from linac-based kV imagers are typically used for image-guided radiotherapy, in particular to perform three-dimensional image matching. CBCT image sets can also be used for adaptive radiotherapy where the treatment plan is modified on the basis of periodic imaging throughout the treatment course. CBCT images provide both anatomical information and Hounsfield unit (HU) values, which are required for dose calculations. This study evaluates treatment plans based on CBCT datasets calibrated using the Catphan 504 phantom to investigate the feasibility of using CBCT for adaptive replanning. The CBCT images were acquired from a Varian On-Board Imager system. Conventional planning CT (PCT) images obtained from a Philips Brilliance Big Bore CT scanner were used as reference images. The HU-density calibration curves of CBCT were obtained using a Catphan 504 phantom and a CIRS density phantom and compared with the clinical PCT calibration curve (obtained using the CIRS density phantom). Treatment plans created using the different calibration curves were compared. Identical targets were delineated on CBCT and PCT images on four different-sized phantoms and planar dose maps were generated. The dose-volume histograms of PCT- and CBCT-based plans were compared and evaluated by gamma analysis. To extend the study to a typical clinical situation, two prostate cases were included. The dose distribution comparison between PCT- and CBCT-based plans for patients yielded similar results to those obtained using phantoms. The study also analyzed the effect of phantom dimensions on HU values and its impact on dose calculations. The isodose distributions computed based on PCT and CBCT using the Catphan calibration curve agree to within ± 1% compared to that based on CBCT using the density phantom calibration curve. However, for phantoms of larger diameter, there is a pronounced discrepancy in the 50% and 60% isodose lines, with the dose difference being about ± 3%. For phantoms whose thickness is less than the cone beam scan length (16 cm) and for phantoms whose diameter is less than that of the calibration phantom, the variation in HU values is high. The effect of a change in radial diameter has a larger impact on dose calculations. This study shows that the CIRS density phantom is not suitable for CBCT calibration and that individual calibration curves obtained using phantoms of appropriate dimensions should be used for planning individual treatment sites. Keywords: Cone beam computed tomography (CBCT), Catphan, Adaptive radiotherapy (ART), Hounsfield unit (HU) 1. Introduction Modern linear accelerators typically have a range of imaging options for image-guided radiotherapy (IGRT). Kilovoltage imagers for improved patient set-up are now commonly used to perform cone beam computed tomography (CBCT) scans for three-dimensional (3D) matching. Linear accelerators with CBCT have been applied to adaptive radiotherapy (ART), where the CBCT dataset is used to adapt the patient treatment plan based on current patient anatomy. * Corresponding author: Kavitha Srinivasan Tel: +61-8-83138353; Fax: +61-8-83134380 E-mail: [email protected] CBCT allows the monitoring of anatomical deformations (weight loss, tumour regression) during the course of radiotherapy treatment, making it a powerful tool for improving patient positioning at the time of treatment and for improved target localization throughout the treatment course [1,2]. Use of CBCT for on-line IGRT applications has been shown to improve the accuracy of radiotherapy treatment at various treatment sites by determining and correcting patient set-up errors down to sub-pixel accuracy [3]. In addition, CBCT datasets can be used for treatment planning and dose calculations [4] if the Hounsfield unit (HU) information provided is reliable and accurate. For accurate dose calculations, knowledge of the relationship between HU and electron density is essential. CBCT images include a larger amount of scatter compared to 378 J. Med. Biol. Eng., Vol. 34 No. 4 2014 that in fan beam CT images [5,6], resulting in a larger variation in HU values, which limits the HU calibration accuracy and reliability [7,8]. Thus, to date treatment plans based on planning CT (PCT) image sets (fan beam geometry) are still superior to those based on CBCT image sets [9]. The magnitude of the scattered radiation in CBCT depends on the size of the scanned object [6,7,10] and hence soft tissue contrast becomes dependent on object size. In addition, limited gantry rotation speed and large field-of-view (FOV) in a single rotation pose problems for image quality. Many methods have been developed to improve the image quality of CBCT [11-14]. It was reported that the number of projections (400-700) from cone beam geometry is insufficient for image reconstruction, leading to variations in HU values [4]. Apart from the geometrical limitations, the Feldkamp algorithm (FDK) used for cone beam reconstruction has the limitation of approximating the line integrals and hence the image quality degrades as the plane moves away from the central axis [15]. This leads to image artifacts such as streaks, rings, cupping, and beam hardening, which degrade image quality [10,15] and reduce soft tissue contrast. Despite these drawbacks, many studies have investigated the use of CBCT datasets for dose calculations [4,7,10,16,17]. It was found that the difference in dose can vary from 3-4% between CBCT- and PCT-based treatment plans using Catphan calibration curves [7,10,16,17], with the largest difference (14.5%) observed for head and neck patients [4]. For bone inhomogeneities, the difference in dose goes up to 20% for two different beam energies [16]. Other approaches for using CBCT datasets generate specific HU-density tables [4]. HU values of PCT have been mapped with CBCT geometry using pixel correction strategies from look-up tables [8,11] or based on rigid registration algorithms [14]. Several scatter correction methods have been developed [18-24] in order to make CBCTbased dosimetry reliable. CBCT datasets have also been applied to adaptive plans to reduce the planning and target margins during the course of treatment [25-28]. The first clinical results of ART applied to prostate cancer showed that a CBCT-based adaptive plan found to reduce the dose to the rectum significantly [25]. The feasibility of CBCT ART for muscle-invasive bladder cancer was determined and compared with conventional radiotherapy [26]. It was found that the volume of irradiated normal tissue was significantly smaller (29% less than conventional) without reducing the clinical target volume. Hawkins et al. [27] investigated the potential reduction in normal tissue irradiation (lungs and heart) for treatment of esophageal cancer for the adaptive plan. A novel re-optimization technique was demonstrated for prostate IMRT plans and it was found that a plan solution can be achieved within 2 min [29] and that it is feasible to use CBCT for online ART [30]. The present study investigates the use of a Varian Onboard Imager (OBI) for ART. Phantoms with various dimensions are used, and the variation in HU values along the phantom Z axis is compared. Parameters that affect the stability of the HU values and their impact on dose calculations are investigated. The dosimetric accuracy of kV-CBCT-based dose calculations is evaluated by extending the study to two clinical situations. The relationship between HU values, scanned object dimensions, and the dose is studied. 2. Materials and methods 2.1 Varian OBI This study used the Varian OBI (Varian Medical Systems, Palo Alto, CA, USA), which has an integrated linac at 90 ° with respect to the treatment beam. Three modes of imaging are available in Varian OBI, namely kV radiography, CBCT, and fluoroscopy. The OBI consists of a kV X-ray source (0.4- and 0.8-mm focal spots) and a kV amorphous silicon digital imaging detector, which faces the X-ray source. For reconstruction diameters of up to 24 cm, a full fan mode is used, where the beam central axis passes through the detector center in order to acquire full projections of the entire object in a single rotation. A total of 360 projections during the 200° gantry rotation are obtained in full fan acquisition. Imaging in full fan mode uses 100 kVp, 20 mA, and 20 ms. For larger reconstruction diameters (up to 45 cm), the CBCT acquisition is switched to half fan mode, in which the detector is offset by 14.8 cm to acquire 655 projections during 360 ° gantry rotation. In this mode, one half of the projections are obtained from one half fan projections and the other half is obtained from the other half fan projections from the other direction. Imaging in half fan mode uses 125 kVp, 80 mA, and 13 ms. A bow-tie filter is added to the kV source while scanning. The CBCT version used is 2.1 and the OBI version is 1.5. 2.2 Planning CT A Philips Brilliance Big Bore CT scanner (Philips Medical Systems, Cleveland, OH, USA) version 2.2 was used in this study to acquire reference CT images. It is a 16-slice helical scanner that has an 85-cm-diameter bore and modulates the tube current during the scan based on patient anatomy. Table 1 shows the scan protocols for CBCT and PCT for the head and body scans used here. The slice thickness can be selected based on the study and depends on which collimation aperture and resolution mode are chosen. There are several filters, including standard, high resolution, and ultra-high resolution, available for each resolution mode to optimize image quality. Depending on the FOV and resolution mode, the pixel resolution is Table 1. Image acquisition parameters for CBCT and PCT for head and body scans. Parameter Scan mode Bow-tie filter X-ray voltage (kVp) X-ray current (mA) Exposure time* (ms) SID (cm) Number of projections Detector configuration (cm2) Field of view (cm2) CBCT Head Body Full Half 100 125 20 80 20 13 150 150 360 655 30 × 40 30 × 40 25 × 25 45 × 45 PCT Head Body --90 120 250 133 800 750 16 × 1.5 16 × 1.5 25 × 25 35 × 35 * Exposure time for CBCT is per projection and that for PCT is per rotation CBCT-Based Treatment Planning determined by choosing the size of the matrix, which can be 512 × 512, 768 × 768, or 1024 × 1024. 2.3 Treatment planning system The treatment planning system (TPS) used was Pinnacle³ (ADAC Laboratories, Milpitas, CA, USA) version v.8.0m. Collapsed cone convolution (CCC) is the model-based algorithm [31] used in this study for dose calculations. It has built-in tissue heterogeneity corrections, handles 3D anatomical information, and allows accurate dose calculations in heterogeneous conditions. 2.4 Phantoms and Patients The Catphan 504 phantom (The Phantom Laboratory, NY, USA) uses tissue substitute materials and is cylindrical, with a 20-cm diameter and a 20-cm thickness. It has several modules. The module used in this study (CTP404) contains inserts of different densities. The CIRS density phantom model 062 (CIRS Tissue Simulation Technology, Norfolk, VA, USA) uses water and tissue equivalent epoxy materials. It is a homogeneous ellipsoidal phantom (33 cm × 5 cm × 27 cm) with 17 small cylindrical parts that can be separated out. The dense bone insert in this phantom is represented by hydroxyapatite, whose mineral composition is similar to that of animal bones. It has a removable central circular section that enables this phantom to be used for both the head and the abdomen. Other homogeneous phantoms were also studied to evaluate HU uniformity: a water phantom (8 cm thick and 25 cm in diameter), a Varian Norm phantom for head scans (made of polyethylene 27 cm thick and 25 cm in diameter) and a Varian Norm phantom for body scans (made of polyurethane 28 cm thick and 45 cm in diameter). Two prostate patients were selected for evaluating CBCTbased dose calculations. Both patients had similar dimensions, with an anterior-posterior separation of 21 cm and a lateral separation of 34 cm. 2.5 Image acquisition Initially images of the above-mentioned phantoms were acquired from two CT volume imaging systems: the PCT as a reference and the CBCT (from Varian OBI). Both systems were operated under similar scanning conditions (tube voltage, tube current, and phantom positioning). Once the images were acquired, they were imported into Pinnacle³ TPS for HUdensity calibration. 2.6 HU calibration Dose distributions were calculated based on the density distribution of the irradiated tissue. Since a CT scanner measures attenuation coefficient values and hence HU values, a calibration function must be derived to determine the physical densities. In order to obtain a calibration curve for a CT scanner, the CIRS density phantom, which is specifically manufactured to obtain a precise relationship between CT numbers and electron densities, was used. Since the volumetric imaging of CBCT includes large fields of view, the use of the thin CIRS 379 density phantom for CBCT calibration leads to more scatter contribution compared to PCT. Hence, this study uses both the density phantom and the Catphan for CBCT calibration and compares these with the PCT calibration to evaluate a suitable CBCT calibration curve for treatment planning. Central slices from the density phantom and from the CTP 404 module of Catphan were selected in Pinnacle3 and the circular regions of interests were drawn to measure the average HU values of each tissue insert. Once the HU values were measured, they were plotted against the known physical density of the tissue inserts for both PCT and CBCT data. Thus, the HU values in each voxel of the reconstructed image were calibrated to the relative physical density for tissue inhomogeneities. 2.7 Dose calculations and evaluations A planning target volume (PTV) of same size (3cm diameter) and shape was contoured in both PCT and CBCT datasets to ensure similar planning conditions for comparison purposes. The PTV for the Catphan, water, and Norm body phantoms (polyurethane) were chosen to be at the center of the phantoms. For the density phantom, the PTV is the breast equivalent insert material (physical density = 0.99 g/cc) at the periphery of the phantom. To calculate the dose distributions in the region of interest, a single 6-MV photon beam with a field size of 10 × 10 cm2 was generated using the source to axis distance (SAD) technique for PCT and CBCT data. The resultant dose distributions and the plot of cumulative dosevolume histograms (DVHs) that summarizes the radiation distribution within the volume of interest were obtained and compared. Planar dose distributions of various phantoms obtained from Pinnacle³ were imported into MapCHECK™ (SUN NUCLEAR Corporation, Melbourne, FL, USA) in order to compare and analyze the PCT and CBCT dose distributions quantitatively. The comparisons were made using a density phantom calibration curve (curve 1) and a Catphan calibration curve (curve 2). The gamma analysis method [32] with a dose difference threshold of 3% and distance-to-agreement (DTA) criterion of 3 mm was used to compare the CBCT dose distributions with that obtained using PCT. To evaluate CBCT-based dose calculation, two prostate patients were recruited. The patients were CT-scanned and the images were transferred to the Pinnacle3 TPS. The target region included the prostate gland with a margin of 6 mm. Femoral heads were included as organs at risk during planning. Static plans using five 6-MV photon beams of equal weighting with gantry angles of 0 °, 55 °, 130 °, 230 °, and 310 ° were adopted for the two cases. CBCT images were acquired with the patient in the treatment position. The images were saved to the record and verify (R&V) system and then analyzed. The PCT- and CBCT- based treatment plans were compared under conditions similar to those for the phantoms. The variation in HU values along the Z axis (thickness of the phantom) is of more concern when dose delivery is based on 3D dose distributions. Therefore, Z profiles of HU were studied for three different phantoms. The HU profiles along the thickness of the homogeneous phantoms were extracted using 380 J. Med. Biol. Eng., Vol. 34. No. 4 2014 ImageJ software (National Institutes of Health) from PCT and CBCT data and compared. The variation in HU values through the slices of the phantom was determined and the difference in percentage HU variation as a function of phantom dimensions (thickness and radial diameter) was examined. that of the calibration phantom, the HU variation is high even for small differences. 3. Results 3.1 HU calibration The relationship between HU values and physical density was established for PCT and CBCT using the density phantom and the Catphan. Routine planning was performed using a CT calibration curve obtained using the CIRS density phantom (i.e., the reference curve). The calibration curve for PCT and CBCT obtained using the density phantom (curve 1) and for CBCT obtained using the Catphan (curve 2) is shown in Fig. 1. Error bars in HU are the standard deviation of the values within the inserts of the phantom. The results show that curve 2 is closer to the PCT curve, with agreement in HU values for densities up to 1 g/cc, whereas curve 1 has much reduced values of HU, agreeing only up to 0.5 g/cc. Figure 2. Scan along the thickness of phantom (Z axis). (a) (b) (c) Figure 3. HU profiles along the thickness of (a) water phantom, (b) Norm head phantom, and (c) Norm body phantom superimposed on their corresponding XZ orthogonal views. Figure 1. Calibration curves for PCT and CBCT. 3.2 HU profiles and dependence on object size The HU profiles of different-sized homogeneous phantoms were measured along the thickness of the phantoms (Z axis) (Fig. 2) and compared in order to verify image uniformity. Figure 3 shows the HU profiles of the water phantom (8.8 cm thick), Norm head phantom (15.8 cm thick), and Norm body phantom (28 cm thick). The HU profile of the water phantom exhibits large fluctuation with reduced HU values along the periphery. With an increase in the thickness of the phantoms (Norm head and body phantoms), the HU fluctuation is significantly reduced (Figs. 3(b) and 3(c)), leading to flatter profiles. The HU profiles were dependent on scanned object size and showed minimum percentage of variation for scanned phantoms whose dimensions are larger compared to the calibration phantom. Figure 4 shows that when the thickness of the object is less than the scanning length (standard cone beam scan length = 16 cm), the scatter contribution leads to high HU variation. Similarly, when the diameter of the object is less than Figure 4. HU dependence on phantom dimensions, along thickness (L) and along Radial diameter (D) of phantom. CBCT-Based Treatment Planning 381 3.3 Dose evaluations - DVHs and gamma maps The isodose lines were calculated using a single 6-MV 10 × 10 cm2 photon beam. The dose distributions in the axial slice of the density phantom, water phantom, Catphan, and Norm body phantom obtained when irradiating an identical spherical target with a 3-cm diameter and of similar volume delineated in PCT and CBCT images are shown in Fig. 5. The dosimetry results were evaluated qualitatively for each study using DVHs, which are shown in Fig. 6. The results show that the dose distribution obtained from CBCT using the Catphan calibration curve (curve 2) agrees well with that of PCT compared to using density phantom calibration curve (curve 1). To further evaluate the results quantitatively, the planar dose distributions in each phantom obtained from PCT and the corresponding slice from CBCT were extracted and compared by gamma analysis. Gamma analysis with the routine clinical threshold levels of 3% and 3 mm was utilized using MapCHECK™. The results are shown in Fig. 7. In the 4window comparison panel of MapCHECK™ software, the dose distributions obtained from PCT and CBCT are in the top two panels. In the lower-left panel, the comparison dose map (a) (b) (c) (a1) (a2) (b1) (b2) (d) Figure 6. DVH comparison of PTV for (a) density phantom, (b) water phantom, (c) Catphan phantom, and (d) Norm body phantom obtained with PCT and CBCT using density phantom calibration curve (curve 1) and Catphan calibration curve (curve 2). (c1) (c2) (d1) (d2) Figure 5. Dose distributions on an axial slice of (a) density phantom, (b) water phantom, (c) Catphan phantom, and (d) Norm body phantoms acquired using PCT (a1, b1, c1 and d1) and CBCT (a2, b2, c2 and d2). (PCT-CBCT) based on gamma analysis indicates the measured dose points that failed the criteria in red and blue for values above and below the criteria, respectively. In the lower-right panel, depth-dose curves along the high-dose profile region between the compared sets are compared. The gamma analysis comparison shows a dose discrepancy within ± 1% using the Catphan calibration curve (curve 2). The same procedure was adopted for the other four phantoms. The overall results show that curve 2 is in better agreement with PCT. For the Norm body, there is a shift in the isodose lines that causes variations in dose of up to 5% (figure not shown). However, the dose discrepancy is reduced to within 3% (Fig. 7(c)) by using the Catphan calibration curve. J. Med. Biol. Eng., Vol. 34 No. 4 2014 382 Figure 8 shows PCT and CBCT axial slices of the two prostate studies with isodose curves embedded on it. A comparison of DVHs of the prostate and femoral heads is presented in Fig. 9. The gamma analysis with 3%/3mm criteria for both the patients (Figs. 10(a) and 10(b)) show 100% pass when the Catphan calibration curve was used, with dose differences within ± 1% . The dose agreement is still clinically acceptable (98% pass) even with 2%/2.5 mm criteria. (a) (b) (a1) (a2) (b1) (b2) Figure 8. Dose distributions superimposed on PCT and CBCT axial slices of patient 1 (a1 and a2) and patient 2 (b1 and b2) for prostate cases using five photon beams. The blue and pink shaded regions are the PTVs and the organ at risk (OAR) is contoured in orange and purple in patient 1 and 2, respectively. (c) (a) (d) (b) Figure 7. Dose distribution, gamma map, and dose profile comparisons for (a) density phantom, (b) Catphan phantom, (c) Norm body phantom, and (d) water phantom obtained using Catphan calibration curve. Figure 9. DVH comparison of PTV and femoral heads for two prostate patients (a and b) obtained with PCT and CBCT using density phantom calibration curve (curve 1) and Catphan calibration curve (curve 2). CBCT-Based Treatment Planning (a) (b) Figure 10. 4-panel dose distribution comparison window from MapCHECK software. The upper two windows show the dose distribution charts from PCT and CBCT, the lower-left window shows the gamma comparison map, and the lower-right window shows the dose profile comparisons for (a) patient 1 and (b) patient 2. 4. Discussion In this study, CBCT HU calibration curves were obtained using the CIRS density phantom (curve 1) and the Catphan 504 phantom (curve 2) and compared with the PCT calibration curve. The CBCT density phantom calibration curve (curve 1) was found to diverge from the corresponding PCT curve, showing reduced values of HU due to a large scatter contribution from CBCT. The density phantom, which is designed for fan beam CT, is very thin (5 cm) compared to the large FOV of CBCT. This causes a greater amount of scattered radiation to reach the OBI flat panel detector. As a result, the HU values are reduced and the noise level is increased, degrading image quality. Comparing the PCT and CBCT calibration curves derived from the density phantom (curve 1), the HU values agree up to ~0.5 g/cc. The deviation in HU linearity for curve 1 is greater than that for curve 2. Since the HU calibration on the Varian OBI was performed using the Catphan phantom, the CBCT 383 calibration curve obtained using Catphan (curve 2) agrees well with the PCT curve for the low-density region up to 1 g/cc (water), after which the values gradually reduce and diverge from the PCT curve. This reduction in HU values is due to the contribution of scattered radiation around high-density materials. However, the variations in HU values are within the typical HU value tolerance of ± 40. Thus, curve 2 is more reliable than curve 1 for treatment planning based on CBCT datasets. The variation in HU values was determined as a function of thickness (in Z direction) and the diameter of the scanned object to study the impact of phantom (scanned object) dimensions on HU. Figure 3(a) shows the HU profile along the thickness of the water phantom. There is a large variation in HU values, with higher values at the center and lower values towards the periphery. This difference in HU values is suggestive of the “capping” artifact caused due to overcorrection for beam hardening effects. This artifact reduces the reconstructed image quality, leading to poor low-contrast resolution. When the thickness of the phantom is increased (Figs. 3(b) and 3(c)), the HU profiles become flatter. When the thickness of the scanned object is less than that of the calibration phantom (Catphan length = 20 cm), there is about 8-10% variation in HU (Fig. 4). However, this variation has little impact on the resulting dose calculation (as was the case for the water phantom with a dose discrepancy within 1%). When the diameter of the scanned object is larger than that of calibration phantom, although HU values are stable (Fig. 3(c)), there is a maximum dose discrepancy of 3% (as was the case for the Norm body phantom). Thus, the diameter of the object has a larger impact on dose calculations. This shows that HU values depend on phantom geometry and hence appropriate HU-density curves are required for specific anatomical sites. Different phantoms with the size of the scanned object (anatomical site) are required in order to use different calibration curves for different clinical studies. The Catphan calibration curve (curve 2) was used for several phantom studies to investigate various situations that limit the use of CBCT datasets in clinical treatment planning. It is worth mentioning that the HU calibration curves for PCT and CBCT were identical in previous studies [7,10,17], which indicates the possibility that higher-density materials (scatter component) were not included in the calibration. In clinical cases, the calibration curve is only useful when inhomogeneities are included. The dose calculated using CBCT curve 1 and curve 2 calibration curves was evaluated using gamma analysis and compared with PCT datasets to study the status of Varian OBI CBCT for treatment planning without correcting for HU values. The doses agreed well (within ± 1%) with that of PCT if the CBCT Catphan calibration curve (curve 2) was utilized for dose computations. However, there was a maximum dose discrepancy of 3% (Fig. 7(c)) on the Norm body phantom with a diameter twice as large as that of the calibration phantom. The reason is, in order to cover large FOVs, half fan acquisition mode was adopted. In this mode, the detector is offset to the center of rotation to cover the large volume. As a consequence, the central part of the phantom is scanned over a complete 360 ° rotation while the peripheral parts are scanned only over a 180 ° J. Med. Biol. Eng., Vol. 34 No. 4 2014 384 half-rotation. This resulted in an artifact in the images of the Norm body phantom (Fig. 3(c)), leading to underestimation of the overall HU values during cone beam reconstruction. This relative variation in HU values when compared to those obtained with PCT causes a shift in the isodose curves, resulting in pronounced variation (± 3%) in the dose distributions when compared to those obtained with PCT. In the patient studies, the resultant dosimetric deviations were found to be ± 5% in the high-gradient dose region for both the cases when the density phantom calibration curve (curve 1) was used. The discrepancy was reduced by using the Catphan calibration curve (curve 2). This further confirms that the use of suitable calibration curves results in better dose agreement. Thus, for major clinical treatment sites such as the prostate, lung, and head and neck, at least three different CBCT calibrations curves based on dimensions of that region are required for planning the corresponding anatomical site. [6] [7] [8] [9] [10] [11] [12] 5. Conclusion [13] In order to use CBCT image sets for dose calculations, reliable HU-density calibration is required. This study showed that the density phantom used for PCT calibration is not appropriate for CBCT dose calculations. Treatment plans created with CBCT images using calibration curves derived from the Catphan (curve 2) agreed well with PCT plans. However the dose distributions of plans created from CBCT images were found to depend on the calibration phantom dimensions. This indicates the need for calibration phantoms that match the size of the treatment site to be imaged (e.g., prostate). When CBCT HU calibration curves that are appropriate for a particular treatment site are used for planning, CBCT can potentially be used for ART. Acknowledgements This work was supported by the University of Adelaide funded by the Australian Postgraduate Award and by Royal Adelaide Hospital. [14] [15] [16] [17] [18] [19] [20] References [1] [2] [3] [4] [5] M. F. Steinke and E. Bezak, “Technological approaches to in-room CBCT imaging,” Australas. Phys. Eng. Sci. Med., 31: 167-179, 2008. J. Chang, K. M. Yenice, A. Narayana and P. H. Gutin, “Accuracy and feasibility of cone-beam computed tomography for stereotactic radiosurgery setup,” Med. Phys., 34: 2077-2084, 2007. D. Létourneau, L. H. Kim, M. Oldham, J. W. Wong, D. Lockman, L. Watt, A. Martinez, G. Hugo, P. Y. Chen and D. Yan, “Cone-beam-CT guided radiation therapy: A model for on-line application,” Radiother. Oncol., 75: 271-278, 2005. A. Richter, Q. Hu, D. Steglich, K. Baier, J. Wilbert, M. Guckenberger and M. Flentje, “Investigation of the usability of conebeam CT data sets for dose calculation,” Radiat. Oncol., 3: 42, 2008. M. B. Sharpe, D. J. Moseley, T. G. Purdie, M. Islam, J. H. Siewerdsen and D. A. Jaffray, “The stability of mechanical calibration for a kV cone beam computed tomography system integrated with linear accelerator,” Med. Phys., 33: 136-144, 2006. [21] [22] [23] [24] [25] J. Siewerdsen and D. Jaffray, “Cone-beam computed tomography with a flat-panel imager: magnitude and effects of x-ray scatter,” Med. Phys., 28: 220-231, 2001. Y. Yang, E. Schreibmann and T. Li, “Evaluation of on-board kV cone beam CT (CBCT)-based dose calculation,” Phys. Med. Biol., 52: 685-705, 2007. T. Tucking, S. Nill and U. Oelfke, “Dose calculation on linac integrated KV-cone beam CT,” Radiother. Oncol., 81: S26, 2006. T. Lo, Y. Yang, E. Schreibmann, T. Li and L. Xing, “Mapping electron density distribution from planning CT to cone-beam CT (CBCT): a novel strategy for accurate dose calculation based on cbct,” Int. J. Radiat. Oncol. Biol. Phys., 63: S507, 2005. S. Yoo and F. Yin, “Dosimetric feasibility of cone-beam CTbased treatment planning compared to CT-based treatment planning,” Int. J. Radiat. Oncol. Biol. Phys., 66: 1553-1561, 2006. T. Depuydt, P. Slagmolen, F. Van den Heuvel and J. Hrbacek, “Cone-beam CT Hounsfield unit correction method and application on images of the pelvic region,” Radiother. Oncol., 81: S29, 2006. D. Letourneau, R. Wong and D. Moseley, “Online planning and delivery technique for radiotherapy of spinal metastases using cone-beam CT: image quality and system performance,” Int. J. Radiat. Oncol. Biol. Phys., 67: 1229-1237, 2007. O. Morin, J. Chen, M. Aubin, A. Gillis, J.-F. Aubry, S. Bose, H. Chen, M. Descovich, P. Xia and J. Pouliot, “Dose calculation using megavoltage cone-beam CT,” Int. J. Radiat. Oncol. Biol. Phys., 67: 1201-1210, 2007. M. van Zijtveld, M. Dirkx and B. Heijmen, “Correction of conebeam CT values using a planning CT for derivation of the “dose of the day”,” Radiother. Oncol., 85: 195-200, 2007. R. Schulze, U. Heil, D. Gross, D. Bruellmann, E. Dranischnikow, U. Schwanecke and E. Schoemer, “Artefacts in CBCT: a review,” Dentomaxillofac. Radiol., 40: 265-273, 2011. J. Hatton, B. McCurdy and P. B. Greer, “Cone beam computerized tomography: the effect of calibration of the Hounsfield unit number to electron density on dose calculation accuracy for adaptive radiation therapy,” Phys. Med. Biol., 54: N329-N346, 2009. S. Padmanaban, V. Nagarajan and P. Sukumar, “A study on evaluation of kV cone beam CT image based treatment planning using anthromorphic phantom,” J. Med. Biol. Eng., 31: 429-435, 2010. R. Ning, X. Tang and D. Conover, “X-ray scatter correction algorithm for cone beam CT imaging,” Med. Phys., 31: 11951202, 2004. G. Poludniowski, P. M. Evans, V. N. Hansen and S. Webb, “An efficient Monte Carlo-based algorithm for scatter correction in keV cone-beam CT,” Phys. Med. Biol., 54: 3847-3864, 2009. J. Rinkel, L. Gerfault, F. Esteve, and J. M. Dinten, “A new method for x-ray scatter correction: first assessment on a conebeam CT experimental setup,” Phys. Med. Biol., 52: 4633-4652, 2007. J. H. Siewerdsen, M. J. Daly, B. Bakhtiar, D. J. Moseley, S. Richard, H. Keller and D. A. Jaffray, “A simple, direct method for x-ray scatter estimation and correction in digital radiography and cone-beam CT,” Med. Phys., 33: 187-197, 2006. J. H. Siewerdsen, D. A. Jaffray, S. Richard, D. J. Moseley and B. Bakhtiar, “The influence of antiscatter grids on soft-tissue detectability in cone-beam computed tomography with flat-panel detectors,” Med. Phys., 31: 3506-3520, 2004. L. Zhu, J. Wang and L. Xing, “Noise suppression in scatter correction for cone-beam CT,” Med. Phys., 36: 741-752, 2009. L. Zhu, Y. Q. Xie, J. Wang and L. Xing, “Scatter correction for cone-beam CT in radiation therapy,” Med. Phys., 36: 2258-2268, 2009. J. Nijkamp, F. J. Pos, T. T. Nuver, R. de Jong, P. Remeijer, J.-J. Sonke and J. V. Lebesque, “Adaptive radiotherapy for prostate cancer using kilovoltage cone-beam computed tomography: first clinical results,” Int. J. Radiat. Oncol. Biol. Phys., 70: 75-82, 2008. CBCT-Based Treatment Planning [26] F. Foroudi, J. Wong, T. Kron, A. Rolfo, A. Haworth, P. Roxby, J. Thomas, A. Herschtal, D. Pham, S. Williams, K. H. Tai and G. Duchesne, “Online adaptive radiotherapy for muscle-invasive bladder cancer: results of a pilot study,” Int. J. Radiat. Oncol. Biol. Phys., 81: 765-771, 2011. [27] M. A. Hawkins, C. Brooks, V. N. Hansen, A. Aitken and D. M. Tait, “Cone beam computed tomography-derived adaptive radiotherapy for radical treatment of esophageal cancer,” Int. J. Radiat. Oncol. Biol. Phys., 77: 378-383, 2010. [28] N. Burridge, A. Amer, T. Marchant, J. Sykes, J. Stratford, A. Henry, C. McBain, P. Price and C. Moore, “Online adaptive radiotherapy of the bladder: small bowel irradiated-volume reduction,” Int. J. Radiat. Oncol. Biol. Phys., 66: 892-897, 2006. [29] Q. J. Wu, D. Thongphiew, Z. Wang, B. Mathayomchan, V. Chankong, S. Yoo, W. R. Lee, and F. F. Yin, “On-line reoptimization of prostate IMRT plans for adaptive radiation therapy,” Phys. Med. Biol., 53: 673-691, 2008. 385 [30] G. X. Ding, D. M. Duggan, C. W. Coffey, M. Deeley, D. E. Hallahan, A. Cmelak and A. Malcolm, “A study on adaptive IMRT treatment planning using kV cone-beam CT,” Radiother.Oncol., 85: 116-125, 2007. [31] A. Ahnesjo, “Collapsed cone convolution of radiant energy for photon dose calculation in heterogeneous media,” Med. Phys., 16: 577-592, 1989. [32] D. A. Low, W. B. Harms, S. Mutic and J. A. Purdy, “A technique for the quantitative evaluation of dose distributions,” Med. Phys., 25: 656-661, 1998.