* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download pericarditis
Survey
Document related concepts
Transcript
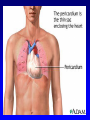
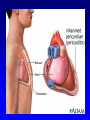
Pericardial Disease By Dr. Muhammad Aftab Shah Senior Registrar Cardiology KEMU/Mayo Hospital, Lahore. 1 Pericardial Disease • • • • • Acute Pericarditis Chronic Relapsing Pericarditis Constrictive Pericarditis Cardiac Tamponade Localized and Low Pressure Tamponade • Restrictive Cardiomyopathy 2 Pericardial Anatomy • Two major components – serosa (viceral pericardium) mesothelial monolayer facilitate fluid and ion exchange – fibroa (parietal pericardium) fibrocollagenous tissue • Pericardial Fluid – 15 - 50 ml of clear plasma ultrafiltrate • Ligamentous attachments – to the sternum, vertebral column, diaphragm 3 9/98 medslides.com 4 Pericardial Physiology • not needed to sustain life • physiologic functions – limit cardiac dilatation – maintain normal ventricular compliance – reduce friction to cardiac movement – barrier to inflammation – limit cardiac displacement 5 Pericardial Inflammation pathogenesis • Contiguous spread – lungs, pleura, mediastinal lymph nodes, myocardium, aorta, esophagus, liver • Hematogenous spread – septicemia, toxins, neoplasm, metabolic • Lymphangetic spread • Traumatic or irradiation 6 9/98 medslides.com 7 Pericardial Inflammation pathology • inflammation provokes a fibrinous exudate with or without serous effusion • the normal transparent and glistening pericardium is turned into a dull, opaque, and “sandy” sac • can cause pericardial scarring with adhesions and fibrosis 8 PERICARDITIS 9 Acute Pericarditis common causes • Outpatient setting – usually idiopathic – probably due to viral infections – Coxsackie A and B (highly cardiotropic) are the most common viral cause of pericarditis and myocarditis – Others viruses: mumps, varicellazoster, influenza, Epstein-Barr, HIV 10 Acute Pericarditis common causes • Inpatient setting T = Trauma, TUMOR U = Uremia M = Myocardial infarction (acute, post) Medications (hydralazine, procain) O = Other infections (bacterial, fungal, TB) R = Rheumatoid, autoimmune disorder Radiation 11 Acute Pericarditis Diagnostic Clues • History sudden onset of anterior chest pain that is pleuritic and substernal • Physical exam presence of two- or three-component rub • ECG most important laboratory clue 12 Chest Pain History pericarditis vs infarction • Common characteristics – retrosternl or precordial with raditaion to the neck, back, left shoulder or arm • Special characteristics (pericarditis) – more likely to be sharp and pleuritic – with coughing, inspiration, swallowing – worse by lying supine, relieved by sitting and leaning forward 13 Heart Murmurs of Pericarditis • Pericardial friction rub is pathognomic for pericarditis • scratching or grating sound • Classically three components: – presystolic rub during atrial filling – ventricular systolic rub (loudest) – ventricular diastolic rub (after A2P2) 14 Acute Pericarditis ECG features • ST-segment elevation – reflecting epicardial inflammation – leads I, II, aVL, and V3-V6 – lead aVR usually shows ST depression • ST concave upward – ST in AMI concave downward like a “dome” • PR segment depression (early stage) • T-wave inversion – occurs after the ST returns to baseline 15 16 17 18 Acute Pericarditis Management • Treat underlying cause • Analgesic agents – codeine 15-30 mg q 4-6 hr • Anti-inflmmatory agents – ASA 648 mg q 3-4 hrs – NSAID (indomethacin 25-50 mg qid) – Corticosteroids are symptomatically effective , but preferably avoided 19 Types of Effusive Fluid • serous – transudative - heart failure • suppurative – pyogenic infection with cellular debris and large number of leukocytes • hemorrhagic – occurs with any type of pericarditis – especially with infections and malignancies • serosanguinous 20 Dignostic Evaluation • Chest x-ray – usually requires > 200 ml of fluid – cannot distinguish between pericardial effusion and cardiomegly • Echocardiography – standard for diagnosing pericardial effusion – convenient, highly reliable, cost effective – false positives (M-mode)- left pleural effusion, epicardial fat, tumor tissue, pericardial cysts 21 Noncompressing Effusion • asymptomatic unless they are large enough to compress adjacent organs – – – – – – – dysphagia cough dyspnea hoarseness hiccups abdminal fullness nausea 22 Cardiac Tamponade • Decompensated cardiac compression from increased intracardaic press 23 Cardiac Tamponade • Early stage – mild to moderate elevation of central venous pressure • Advanced stage – intrapericardial pressure ventricular filling, stroke volume – hypotension – impaired organ perfusion 24 Beck’s Triad • Described in 1935 by thoracic surgeon Claude S. Beck • 3 features of acute tamponade – Decline in systemic arterial pressure – Elevation in systemic venous pressure (e.g. distended neck vein) – A small, quiet heart 25 Cardiac Tamponade Bedside Diagnosis • Elevated jugular venous pressure • Paradoxical pulse 26 Pulsus Paradoxus • an exaggerated drop in blood pressure with inspiration (>10mmHg) • tamponade without pulsus – atrial septal defect – aortic insufficiency – LVH with LVEDP • pulsus without tamponade – COPD, RV infarct, pulmonary embolism 27 Echocardiography • Pericardial effusion – highly reliable • Cardiac tamponade – RA and RV diastolic collapse – reduced chamber size – distension of the inferior vena cava – exaggerated respiratory variation of the mitral and tricuspid valve flow velocities 28 Pericardiocentesis • Diagnostic tap – usually not indicated – rarely have positive cytology or infection that can be diagnosed • Therapeutic drainage – indicated for significant elevation of the central venous pressure 29