* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download hernias - FK UWKS 2012 C
Survey
Document related concepts
Transcript
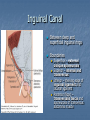
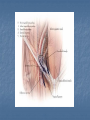
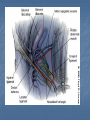
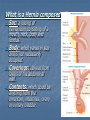
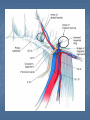
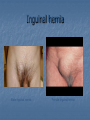
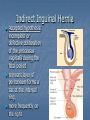
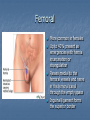
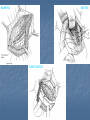
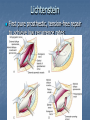
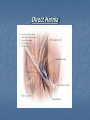
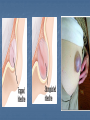
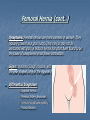
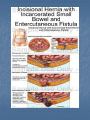
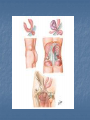
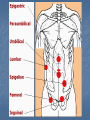
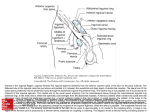
Introduction Protrusion of the peritoneum or preperitoneal fat through an abnormal opening in the abdominal wall Presents as a bulge Peritoneal contents may be trapped in “sac” Asymptomatic bulge most common Symptoms Physical effects of sac and contents on surrounding tissues Obstruction and/or strangulation of hernia sac contents Epidemiology 700,000 hernia repairs year Inguinal hernias -75% of all hernias 2/3 Indirect, remainder are direct Incisional hernias – 15 to 20% Umbilical and epigastric – 10% Femoral – 5% Epidemiology Prevelance of hernias increases with age Most serious complication – strangulation 1 to 3% of groin hernias Femoral – highest rate of complications 15% to 20% recommended all be repaired at time of discovery Anatomy Areas of Natural Weakness Used with permission from the American College of Surgeons Anatomy Inguinal ligament (Poupart’s) – inferior edge of external oblique Lacunar ligament – triangular extension of the inguinal ligament before its insertion upon the pubic tubercle conjoined tendon (510%)- Internal oblique fuses with transversus abdominis aponeurosis Cooper’s Ligament formed by the periosteum and fascia along the superior ramus of the pubis. Inguinal Canal Between deep and superficial inguinal rings Boundaries Superifical – external oblique aponeurosis Superior – internal and transversus Inferior – shelving edge of inguinal ligament and lacunar ligament Posterior (floor) – transversalis fascia and aponeurosis of transversus abdominis muscle Components of Hesselbach’s triangle include which of the following anatomic landmarks? A. B. C. D. E. Pectineal ligament Lateral border of the rectus sheath Cooper’s ligament Inguinal ligament Inferior epigastric vessels Hernia Diathesis Varies with age Pediatric: congenital remnant Adult Tissue weakness Burst strength < abdominal wall tension Varies with gender Hernia Diathesis Pediatric: major risk is premature birth Adult Obesity Previous abdominal surgery Pregnancy Abrupt abdominal wall exertion What is a Hernia composed of? 1. Sac: a folding of peritoneum consisting of a mouth, neck, body and fundus. 2. Body: which varies in size and is not necessarily occupied. 3. Coverings: derived from layers of the abdominal wall. 4. Contents: which could be anything from the omentum, intestines, ovary or urinary bladder. A sliding inguinal hernia on the left side is likely to involve which of the following? A. B. C. D. E. Jejunum composing the posterior wall of the sac Ovary and fallopian tube in a female infant Omentum Sigmoid colon composing the posterior wall of the sac Cecum composing the anteromedial wall of the sac Terminology Pantaloon – direct and indirect components Richter’s – contains antimesenteric portion of small bowel Sliding – involves visceral peritoneum of an organ , i.e. bladder, ovary Littre’s – hernia contains Meckel’s diverticulum Petit – hernia at inferior lumbar triangle Grynfelt – hernia at superior lumbar triangle Clinical Evaluation: History Demographics Age Gender Presentation of bulge When, where, how Activities that make it better or worse Discomfort vs. pain Signs/symptoms of bowel obstruction Clinical Evaluation: History Surgery: previous repairs/operations Review of factors related to increased intra-abdominal pressure Chronic cough Constipation Straining to urinate Clinical Evaluation: Location Groin: 75% Inguinal Femoral Anterior abdominal wall: 25% Umbilical Epigastric Spigelian Incisional Hernia Pathology Contents of hernia sac Bowel (small and large, appendix) Incarceration of portion of bowel wall: Richter’s hernia: Strangulation occurs without obstruction Omentum, bladder, ovary, fallopian tubes Sac wall may be formed by large bowel, bladder, or the ovary/tube: Sliding hernia Hernia Pathology Fascial defect may exist without peritoneal hernia sac Preperitoneal abdominal wall contents may protrude through fascial defect Preperitoneal fat Lymph node Hernia Pathology Incarceration: contents of hernia sac not reducible into peritoneal cavity Acute: fascial margins trap contents Chronic: contents adhesed in sac Strangulation: incarceration with compromise of blood supply Narrow neck at greatest risk: indirect inguinal, femoral, and umbilical Hernia Repair Indications Asymptomatic prevent visceral incarceration and/or strangulation Symptomatic, non-obstructed Treat discomfort from bulge Prevent incarceration/strangulation Visceral obstruction/strangulation Release obstruction/manage viscera Prevent recurrence Groin Hernia Men : Women 25 : 1 Right : Left 2 : 1 Femoral Women > Men Strangulation risk > inguinal Inguinal Indirect : Direct 2 : 1 Most common in men and women Groin Hernia Inguinal: relationship of sac to inguinal canal determines external bulge Movement from internal ring to scrotum Bilateral hernias: direct 4x indirect Indirect vs. direct hernia is intraoperative diagnosis, not clinical diagnosis Femoral: relationship of sac to inguinal ligament determines external bulge Groin Hernia: Inguinal Adults Weakness of transversalis fascia Indirect: sac is lateral to inferior epigastric vessels Direct: sac is medial to inferior epigastric vessels Pantaloon: both indirect and direct Pediatric: patent processus vaginalis Inguinal hernia Male inguinal hernia Female inguinal hernia Groin Hernia: Differential Diagnosis Tendonitis Muscle tear Lymph node Lipoma Varicose vein Hydrocele Epididymitis Spermatocele Groin Hernia Management Most hernias: ambulatory OR Local/regional/general anesthesia Prohibitive operative risk: truss Groin Hernia Management Acute incarceration Reduction (taxis) Distal traction and gentle milking Caution: reduction en masse Successful reduction shows visually Urgent elective repair if reduced Groin Hernia Management Emergent repair Irreducible acute incarceration Strangulation Fluid, electrolyte resuscitation Groin Hernia Surgical Classification (Nyhus) I: Indirect hernia w/normal internal ring 2: Indirect hernia w/enlarged internal ring 3a: Direct inguinal hernia 3b: Indirect hernia with weak floor 3c: Femoral hernia 4: All recurrent hernias Direct Inguinal Hernia Direct Inguinal Hernia Medial to the inferior epigastric artery and vein, and within Hesselbach's triangle acquired weakness in the inguinal floor Indirect Inguinal Hernia Accepted hypothesis: incomplete or defective obliteration of the processus vaginalis during the fetal period remnant layer of peritoneum forms a sac at the internal ring more frequently on the right Femoral More common in females Up to 40% present as emergencies with hernia incarceration or strangulation Passes medial to the femoral vessels and nerve in the femoral canal through the empty space Inguinal ligament forms the superior border Groin Hernia Surgery: Open Indirect sac: high ligation Men: ligation at internal ring Women: ligation/excision of round ligament with closure of internal ring Cord lipoma: excision Operative Bassini Shouldice McVay Lichtenstein Preperitoneal Laparoscopic Bassini (early 20th Century) Shouldice (1930s) Transversus abdominis to Thompson’s ligament and internal oblique musculoaponeurotic arches or conjoined tendon to the inguinal ligament Multilayer imbricated repair of the posterior wall of the inguinal canal McVay (1948) Edge of the transversus abdominis aponeurosis to Cooper’s ligament; incorporate Cooper’s ligament and the iliopubic tract (transition suture) BASSINI MCVAY SHOULDICE Lichtenstein First pure prosthestic, tension-free repair to achieve low recurrence rates Groin Hernia Surgery: Open Inguinal floor: tension-free repair with mesh Anterior plug and patch Anterior patch Posterior patch (Stoppa) Groin Hernia Surgery Open tissue repair for risk of infection (example: strangulated hernia) Laparoscopic Indications Recurrent hernia Bilateral hernias Must be able to tolerate general anesthesia More expensive Groin Hernia Repair Complications Recurrence Tissue repair: 1.3—25% Tension-free mesh: 0.5—5% Greatest risk is repair of previous hernia at same location Groin Hernia Repair Complications Chronic groin pain: up to 30% Numbness over base of scrotum Groin Hernia Repair Complications Wound Infertility Hematoma: 1.0% Infection: 1.3% Seroma Injury to vas deferens Ischemic orchitis is uncommon Urinary retention Other Hernias Umbilical Hernia Fascial defect at the umbilicus with peritoneal sac covered by skin External bulge at the umbilicus or periumbilically depending on subcutaneous migration of sac Exam: External bulge at or adjacent to the umbilicus Pediatric Umbilical Hernia Present in 10-30% of babies 80% close spontaneously by age 2 Indications for primary suture repair Hernia present after ages 2-4 Large (5 cm) defect at age 1 Adult Umbilical Hernia Increased intra-abdominal pressure Pregnancy Obesity Ascites Differential diagnosis (rare) Embryologic remnants Metastatic cancer Adult Umbilical Hernia Symptoms relate to cosmesis, traction on the sac, or trapped contents Omentum Small or transverse colon Acute incarceration: reduction en masse problematic Adult Umbilical Hernia Repair Assess contents and manage appropriately based on viability Open hernia repair < 1 cm defect: primary suture repair > 1 cm defect: mesh repair lowers recurrence Laparoscopic hernia repair: size of access ports often > hernia incision Adult Umbilical Hernia Repair Risks Recurrence Umbilical necrosis Injury to sac contents Hematoma Infection Epigastric Hernia Fascial defect in supraumbilical linea alba Most < 1 cm 20% with multiple defects Beware diastasis recti Men: Women 2:1 Epigastric midline junction of the aponeuroses (linea alba) between the xiphoid process and umbilicus Paraumbilical hernia epigastric hernia that borders the umbilicus Estimated frequency 35% More common in Males 3:1 20% may be multiple Epigastric Hernia Contents Incarcerated preperitoneal fat or falciform ligament Peritoneal sac Repair Open repair similar as for umbilical hernia Must palpate or visualize entire supraumbilical linea alba Laparoscopic approach is suboptimal Spigelian Hernia Defect through transversus abdominus and internal oblique muscles Occurs at junction of arcuate line and linea semilunaris Fascial defect 1-2 cm Covered by external oblique aponeurosis Spigelian Hernia occurs along the semilunar line, which traverses a vertical space along the lateral rectus border where more than 90% of spigelian hernias are found Spigelian Hernia Clinical Swelling in middle to lower abdomen lateral to rectus muscle Usually reducible Up to 20% present with incarceration Tx: surgical Mesh not required Recurrence is uncommon Spigelian Hernia Presentation Lower abdominal swelling lateral to rectus Focal discomfort/pain May require imaging studies for diagnosis Ultrasound or CT Repair: open or laparoscopic, on-lay mesh Incisional Hernia Bulge in region of scar from surgery or penetrating trauma Chronic wound failure Up to 20% of abdominal incisions Subcutaneous sac may be more complex Multi-loculated Contents adhesed within sac Incisional Hernia: Risk Factors Previous incisional hernia repair Obesity Smoking Chronic lung disease Diabetes Malnutrition Wound infection Incisional Hernia Repair Fix conditions that promoted hernia occurrence Open repair Primary suture: < 52% recurrence Mesh: < 24% recurrence Incisional Hernia Repair Complex open repairs Stoppa mesh repair Component separations repair Laparoscopic repair Multiple fascial defects detected Large on-lay intraperitoneal mesh 5 cm marginal overlap Incisional Hernia Complications of repair Recurrence Seromas Injury to sac contents Bleeding Infection Review Pediatric hernias Inguinal Umbilical Adult hernias Groin Inguinal Femoral Umbilical Epigastric Spigelian Incisional Points to Remember Hernias represent fascial defects with protrusion of a peritoneal sac or preperitoneal fat Asymptomatic bulge most common Hernia risk is related to visceral obstruction or strangulation Tension-free repair with mesh produces lowest recurrence rates Summary Etiology, pathology, clinical evaluation, and treatment of abdominal wall hernias including inguinal, femoral, umbilical, epigastric, Spigelian, and incisional hernias Scenario Direct Hernia Indirect inguinal hernia Direct inguinal hernia Relation to epigastric vessels Lataral medial Processus vaginalis Present Absent Causes congenital Acqiured Individual hernias 1. Direct & indirect Inguinal hernia. 2. Femoral hernia. 3. Umbilical hernia & paraumbilical hernia. 4. Incisional hernia. 5. Epigastric hernia. 6. Rare external Hernias. Femoral Hernia Femoral Hernias occur just below the inguinal ligament, when abdominal contents pass through a naturally occurring weakness called the femoral canal. The Femoral canal : The most medial structure in the femoral sheath,. extending from the femoral ring to the saphenous opening. 1.25cm x 1.25cm. Contains fat, lymph vessels and the lymph node of cloquet. Femoral Hernia (cont..) Symptoms: Femoral hernias are more common in women, They typically present as a groin lump. They may or may not be associated with pain, a femoral hernia has often been found to be the cause of unexplained small bowel obstruction. Signs: an absent Cough impulse, with a more globular lump than the pear shaped lump of the inguinal hernia. Differential Diagnoses: Inguinal Hernia. Femoral Artery Aneurism. Femoral Lymphadenopathy. Psoas Abscess. Umbilical & paraumbilical Hernia A. Umbilical Hernia: Seen in infants & children. Effecting boys more than girls. tend to resolve without any treatment by around the age of 5 years. Obstruction and strangulation of the hernia is rare. Babies are prone to this malformation because of the process during fetal development by which the abdominal organs form outside the abdominal cavity, later returning into it through an opening which will become the umbilicus. B. Paraumbilical Hernia: Affects adults. The defect is either supra or infraumbilical through the linea alba. The female to male ratio is 20:1. May contain omentum, small intestine or transverse colon. Etiology: 1. 2. 3. Obesity. Flabbiness of the abdominal muscles. Multiparity. Clinical Features: Clolicky pain and/or irreducibilty due to omental adhesions. Incisional Hernia Definition: An incisional hernia occurs when the area of weakness is the result of an incompletely healed surgical wound. These can be among the most frustrating and difficult hernias to treat. It can occur at any incision, but tend to occur more commonly along a straight line from the sternum breastbone straight down to the pubis, and are more complex in these regions. Hernias in this area have a high rate of recurrence. Causes: Any reasons leading to an icrease in intraabdominal pressure postoperatively such as: chronic cough, vomitting, infection, malnutrition diabetes, steroid treatment or a tension closure done during the previous operation. Clinical Features: Swelling at the incisional site +/- pain. Ventral wall (Incisional) Highest incidence in midline and transverse incisions Up to20% after laparotomy 1/3 present in 5-10 years postoperatively Risk factors obesity, DM, ascites, steroids, smoking malnutrition, wound infection Technical aspects of wound closure Type of incision Excessive tension (prone to fascial disruption) Epigastric Hernia Due to a defectin the linea alba between the xiphoid process and the umbilicus Starts as a protrusion of the extraperitoneal fat at the site where a small vessel pierces the lina alba and as it enlarges it drags a pouch of peritoneum after it. Clinical Features: Swelling +/- pain similar to a peptic ulcer pain. Rare external Hernias Since many organs or parts of organs can herniate through many orifices, it is very difficult to give an exhaustive list of hernias, with all synonyms and eponyms. But her are Other hernial types and unusual types of visceral hernias: 1. Spiglian Hernia: Occurs at the spaces of the semilunar line and the lateral edge of the rectus muscle (inferior to the arcuate line). The posterior rectus sheath jis weak thus leading to the protrusion. Preoperative diagnosis is diffucult & only correct in 50% of the patients. u/s & c.t are helpful tools in the diagnosis Depending on the size of the defect, treatment varies from suture approximation to using a mesh. Rare hernias (cont..) 2. Lumbar Hernias: In the lumbar region, in the form of a broad bulging hernia, that are not vulnerable to incarceration. Devided into: A. Petit’s hernia: which occurs in the inferior lumbar triangle. B. Grynfeltt’s Hernia: which occurs in the superior lumbar triangle and is less common that Petit’s. Lumbar Acquired lumbar hernias – Contains to anatomic triangles, inferior and superior lumbar triangles back or flank trauma, poliomyelitis, back surgery, and the use of the iliac crest as a donor site for bone grafts Grynfelt’s Petit’s Strangulation is rare Soft swelling in lower posterior abdomen Rare hernias (cont..) 3. Obturator Hernia: The obturator canal is covered by a membrane pierced by the obturator nerve and vessels. Any enlargement in the canal or weakness in the membrane may lead to herniation of the intetines. Because of differences in anatomy, it is much more common in women than in men. It often presents with bowel obstruction. The Howship-Romberg sign is suggestive of an obturator hernia, exacerbated by thigh extension, medial rotation and adduction. It is characterized by lancilating pain in the medial thigh/obturator distribution, extending to the knee; caused by hernia compression of the obturator nerve. Obturator Rare form of hernia Protrusion of intra-abdominal contents through obturator foramen F:M ratio 6:1 The obturator foramen is formed by the ischial and pubic rami obturator vessels and nerve lie posterolateral to the hernia sac in the canal Small bowel is the most likely intraabdominal organ to be found in an obturator hernia Obturator 4 cardinal signs : intestinal obstruction (80%) Howship-Romberg sign (50%) –History of repeated episodes of bowel obstruction that resolve quickly and without intervention Palpable mass (20%) Tx: Sugical Repair Sciatic Via greater or lesser sciatic notch greater sciatic notch is traversed by the piriformis muscle, and hernia sacs can protrude either superior or inferior to this muscle suprapiriform defect 60% Infrapiriform 30% subspinous (through the lesser sciatic foramen) 10% EXAMINATION: Hernias must be examined with the patient standing and in supine Always examine both groins. INSPECTION: Visible swelling. (site, size and shape) Visible cough impulse. Easily reducible Reappear on straining, standing or coughing Elucidate Fothergill and Carnet signs. PALPATION: Examine as a mass and then Palpable cough impulse Reduce Occlusion test Three Finger test ( Zimman’s test) Examination also asses the following: Position Temperature Tenderness Shape Size Tension Composition Expansile cough impulse Reducible. PERCUSSION AND AUSCULTATION: Bowel sound. Treatment Most abdominal hernias can be surgically repaired. Uncomplicated hernias are principally repaired by herniorrhaphy. a Herniorrhaphy (Hernioplasty) is a surgical procedure for correcting hernia, which can be devided into four techniques: Groups 1 and 2: open "tension" repair: in which the edges of the defect are sewn back together without any reinforcement or prosthesis. In the Bassini technique, the conjoint tendon (formed by the distal ends of the transversus abdominis muscle and the internal oblique muscle) is approximated to the inguinal canal and closed. [4] Although tension repairs are no longer the standard of care due to the high rate of recurrence of the hernia, long recovery period, and post-operative pain, a few tension repairs are still in use today. Treatment (cont..) Group 3: open "tension-free" repair: Almost all repairs done today are open "tension-free" repairs that involve the placement of a synthetic mesh to strengthen the inguinal region. This operation is called a 'hernioplasty'. The meshes used are typically made from polypropylene or polyester. The operation is typically performed under local anesthesia, and patients go home within a few hours of surgery, often requiring no medication beyond aspirin or acetaminophen. Recurrence rates are very low - one percent or less, compared with over 10% for a tension repair Treatment (cont..) Group 4: laparoscopic repair "Lap" repairs are also tension-free, although the mesh is placed within the preperitoneal space behind the defect as opposed to in or over it. It is further sub-devided into: T.A.P.P repair (transabdominal preperitoneal) T.E.P repair (totally extraperitoneal) It has no proven superiority to the open method other than a faster recovery time and a slightly lower post-operative pain score. laparoscopic surgery, though, requires general anesthesia, more expensive and consumes more O.R. time than open repair and carries a higher risk of complications, and has equivalent or higher rates of recurrence compared to the open tension-free repairs.