* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Survey
Document related concepts
Transcript
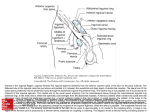
5-year DDS Program General Surgery Department of Surgery University School of Medical Science POZNAN, POLAND Chairman: prof. Dr hab. n.med. Waclaw Majewski Hernias NMS Surgery: Bruce E.Jarrell, R.Anthony Carabasi, Lippincott Williams & Wilkins Suggested textbook: Historical Perspective • 15th century Castration with wound cauterization or hernia sac debridement • recommended a truss Father of Modern Inguinal Hernia Repair EDUARDO BASSI NI 1844-1924 Nuovo metodo operativo per la cura dell'ernia inguinale, 1889 Hernia • latin for rupture • an abnormal protrusion of an organ or tissue through a defect in its surrounding walls • the most common herniae develop in the abdomen when a weakness in the abdominal wall evolves into a localized hole, or "defect", through which adipose tissue, or abdominal organs covered with peritoneum, may protrude What is a Hernia composed of? 1.Sac: a folding of peritoneum consisting of a mouth, neck, body and fundus 2.Body : which varies in size and is not necessarily occupied 3.Coverings: derived from layers of the abdominal wall 4.Contents: which could be anything from the omentum, intestines, ovary or urinary bladder Epidemiology • 600,000 hernia repairs yearly in the USA • Inguinal hernias – 75-80% of all hernias – 4/5 Indirect, remainder are direct • Incisional hernias – 8-10% • Umbilical and epigastric – 3-5% • Femoral – 5% Epidemiology • Prevelance of hernias increases with age • Most serious complication – strangulation – 1-3% of groin hernias • Femoral – highest rate of complications (strangulation) 15% to 20% – recommended all be repaired at time of discovery Anatomy inguinal canal • Between deep and superficial inguinal rings • Boundaries – Superifical – external oblique aponeurosis – Superior – internal and transversus – Inferior – shelving edge of inguinal ligament and lacunar ligament – Posterior (floor) – transversalis fascia and aponeurosis of transversus abdominis muscle Anatomy The inguinal canal contains: • the spermatic cord (M) and round ligament of the uterus (F) • Spermatic cord – – – – – – – Cremasteric muscle fibers Testicular vessels Genital branch of genitofemoral nerve Vas deferens Cremasteric vessels Veins: pampiniform plexus Processus vaginalis: an evagination of peritoneum Anatomy Hesselbach's triangle Boundaries: Medial: Rectus abdominis muscle medially Inferiorly: Inguinal ligament Laterally: Inf. Epigastrics Anatomy • Inguinal ligament (Poupart’s) – inferior edge of external oblique • lacunar ligament (Gimbernat’s) – triangular extension of the inguinal ligament before its insertion upon the pubic tubercle • conjoined tendon (510%)- Internal oblique fuses with transversus abdominis aponeurosis • Cooper’s Ligament formed by the periosteum and fascia along the superior ramus of the pubis. Terminology • Reducible – can be replaced within surrounding musculature • Incarcerated – cannot be reduced • Strangulated – compromised blood supply to its contents Terminology • Pantaloon – direct and indirect inguinal hernia components • Richter’s – contains antimesenteric portion of small bowel • Sliding – involves visceral peritoneum of an organ i.e. bladder, ovary • Littre’s – hernia contains Meckel’s diverticulum • Petit – hernia at inferior lumbar triangle • Grynfeltt – hernia at superior lumbar triangle Groin Hernias • Indirect Inguinal • Direct Inguinal • Femoral Inguinal Hernia • classified as congenital vs. acquired • commonly thought that repeated increases in intra-abdominal pressure contribute to hernia formation • collagen formation and structure deteriorates with age, and thus hernia formation is more common in the older individual Clinical Presentation • Groin bulge • Often asymptomatic • Dull feeling of discomfort or heaviness in the groin • Focal pain – raise suspicion for incarceration or strangulation • Symptoms of bowel obstruction Diagnosis • Physical Exam • 74.5% sensitive and 96.3% specific • examine the patient in the standing and supine positions • difficult to distinguish direct and indirect on exam on alone Diagnosis • Radiologic Investigations – Herniography • Suspected hernia, but clinical dx unclear • Procedure done under flouroscopy following injection of contrast medium • Frontal and oblique radiographs are taken with and without increased intraabdominal pressure – Ultrasonography – MRI – CT Right direct inguinal hernia Left indirect inguinal hernia Direct Inguinal Hernia • Medial to the inferior epigastric artery and vein, and within Hesselbach's triangle • acquired weakness in the inguinal floor Indirect Inguinal hernia • Abdominal contents protrude through internal inguinal ring • 5 to 10 times more common in men Indirect Inguinal Hernia • Accepted hypothesis: incomplete or defective obliteration of the processus vaginalis during the fetal period • remnant layer of peritoneum forms a sac at the internal ring • more frequently on the right Femoral • More common in females • Up to 40% present as emergencies with hernia incarceration or strangulation • Passes medial to the femoral vessels and nerve in the femoral canal through the empty space • Inguinal ligament forms the superior border • Requires palpation of the femoral canal just below the inguinal ligament in the upper thigh Treatment • Non-Operative – Observation – Trusses can provide symptomatic relief • Hernia control in ~30% of patients Operative • • • • • • Bassini Shouldice McVay Lichtenstein Preperitoneal Laparoscopic • Bassini (early 20th Century) – Transversus abdominis to Thompson’s ligament and internal oblique musculoaponeurotic arches or conjoined tendon to the inguinal ligament • Shouldice (1930s) - multilayer imbricated repair of the posterior wall of the inguinal canal uses the transversalis fascia, which is divided longitudinally and imbricated upon itself in two layers; the internal oblique muscle and conjoint tendon are then sutured to the reflection of the inguinal ligament in two layers (total four suture lines). • McVay (1948) - Edge of the transversus abdominis aponeurosis to Cooper’s ligament; incorporate Cooper’s ligament and the iliopubic tract (transition suture) • Lichtenstein • First pure prosthestic, tension-free repair to achieve low recurrence rates • Lichtenstein • The mesh is sutured to the aponeurotic tissue overlying the pubic bone medially, continuing superiorly along the transversus abdominis or conjoined tendon. The inferolateral edge of the mesh is sutured to the iliopubic tract or the shelving edge of the inguinal ligament to a point lateral to the internal inguinal ring. Neo-ring created. The ilioinguinal nerve and genital branch of the genitofemoral nerve are placed with the cord structures and are passed through this newly fashioned internal inguinal ring. Prosthetic Repair • Polypropylene mesh most common and preferred – allows for a fibrotic reaction to occur between the inguinal floor and the posterior surface of the mesh, thereby forming scar and strengthening the closure of the hernia defect • Polytetrafluoroethylene (PTFE) mesh – often used for repair of ventral or incision hernias in which the fibrotic reaction with the underlying serosal surface of the bowel is best avoided Laparoscopic repair Surgical Complications • • • • • • Recurrence Infection Neuralgia Bladder injury Testicular injury Vas Deferens injury Other Hernias Umbilical Incidence • Reported 3-8% • several times greater in Black children • more common in premature children all races • Most close spontaneously by age 2 or 3 • Acquired rather than congenital in adults • Female to male ratio 10:1 Epigastric • midline junction of the aponeuroses (linea alba) between the xiphoid process and umbilicus • Paraumbilical hernia epigastric hernia that borders the umbilicus • Estimated frequency 35% • More common in Males 3:1 • 20% may be multiple Epigastric • Clinical – Often asymptomatic, incidental finding – If symptomatic, vague abdominal pain above the umbilicus exacerbated by standing or coughing; relieved in supine position – Severe pain secondary to incarceration/strangulation o preperitoneal fat (often no peritoneal sac) or omentum – Exam: palpate small, soft, reducible mass superior to the umbilicus – RARE to have strangulated bowel • Treatment – like umbilical hernia – Excise fat and sac, close primarily Obturator • • • • • • Rare form of hernia Protrusion of intra-abdominal contents through obturator foramen F:M ratio 6:1 The obturator foramen is formed by the ischial and pubic rami obturator vessels and nerve lie posterolateral to the hernia sac in the canal Small bowel is the most likely intraabdominal organ to be found in an obturator hernia Obturator – 4 cardinal signs : • intestinal obstruction (80%) • Howship-Romberg sign (50%) – pain along the obturator nerve (mid-anterior thigh) • Palpable mass (20%) – Treatment - Sugical Repair Spigelian Hernia • occurs along the semilunar line, which traverses a vertical space along the lateral rectus border Spigelian Hernia • Clinical – Swelling in middle to lower abdomen lateral to rectus muscle – Usually reducible – Up to 20% present with incarceration • Treatment: surgical – Mesh not required – Recurrence is uncommon Lumbar • Acquired lumbar hernias – back or flank trauma, poliomyelitis, back surgery, and the use of the iliac crest as a donor site for bone grafts • Contains to anatomic triangles, inferior and superior lumbar triangles – Grynfeltt’s – Petit’s • Strangulation is rare • Soft swelling in lower posterior abdomen Sciatic • Via greater or lesser sciatic notch • greater sciatic notch is traversed by the piriformis muscle, and hernia sacs can protrude either superior or inferior to this muscle • suprapiriform defect 60% • Infrapiriform 30% • subspinous (through the lesser sciatic foramen) 10% Ventral wall (Incisional) • • • • Highest incidence in midline and transverse incisions Up to 20% after laparotomy 1/3 present in 5-10 years postoperatively Risk factors – obesity, DM, ascites, steroids, smoking malnutrition, wound infection • Technical aspects of wound closure – Type of incision – Excessive tension (prone to fascial disruption)