* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Bariatric Surgery Basics
Survey
Document related concepts
Thrifty gene hypothesis wikipedia , lookup
Abdominal obesity wikipedia , lookup
Epidemiology of metabolic syndrome wikipedia , lookup
Obesity and the environment wikipedia , lookup
Diet-induced obesity model wikipedia , lookup
Cigarette smoking for weight loss wikipedia , lookup
Transcript
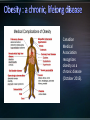
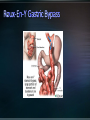
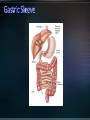
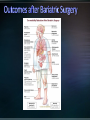
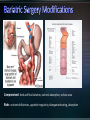
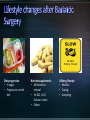
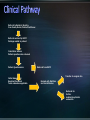
Obesity: prevalence, influences and challenges Canadian Medical Association recognizes obesity as a chronic disease (October 2015). 4-fold increase in morbid obesity over the last 20 years Source: Katzmarzyk PT, Mason C. Prevalence of class I, II and III obesity in Canada. CMAJ. 2006 Jan 17;174(2):156-7. 80-90% of patients with T2DM overweight or obese* Some antihyperglycemic therapies contribute to weight gain Higher BMI increases mortality Modest weight loss (5-10% total body weight) can improve metabolic parameters *Wing RR. Weight loss in the management of type 2 diabetes. In: Gerstein HC, Haynes B editor(s). Evidence-Based Diabetes Care. Ontario, Canada: B.C. Decker, Inc, 2000:252–76. Interdisciplinary weight management programs to prevent weight gain and achieve and maintain a lower, healthy body weight (Grade A, Level 1A). Recognize the effect of anti-hyperglycemic agents on body weight. (Grade D, consensus). Bariatric surgery may be considered when lifestyle interventions are inadequate in achieving healthy weights in patients with type 2 diabetes and class II or III obesity (Grade B, Level 2). *A.Sharma and D. Lau (2013). Weight Management in Diabetes. Can J Diabetes 37: S82-S86. Weight management is not a simple equation Goals around weight management: - Preventing weight gain - Preventing weight regain - Understanding best weight Weight Management Strategies Age ≥ 18 years Body Mass Index (BMI) ≥ 40 BMI ≥ 35 with significant co-morbidities Heart disease, Type 2 diabetes, Hypertension, Sleep Apnea, GERD History of prior weight management attempts Motivation and engagement in lifestyle modifications * Ontario Bariatric Network Active substance use, including nicotine and alcohol, <6 months prior to surgery. Medical or surgical conditions that may make surgery a high risk to perform. Severe or poorly controlled current psychiatric illness or undertreated symptoms. * Ontario Bariatric Network NSAIDS are contraindicated for gastric bypass Significantly increased risk of GI bleeding Avoidance (pre / post op) : nicotine, caffeine Potential detrimental effect on anastomoses and GI lining Weight loss 52-77% excess body weight loss maintained at 10 yrs All cause mortality lowered 29-40% CAD 49%, cancer 60% Diseases improved or remission (60-80%) Diabetes, lipids, BP, liver disease, MSK pain Sleep apnea resolves 95% Improved Quality of Life TD Adames et al. (2007). Long-term mortality after gastric bypass surgery. N Engl J Med. 357: 753-761. Impressive outcomes: Metabolic – STAMPEDE trial of 150 moderately obese patients showed that 42% of patients with RNY had A1C < 6% compared to 12% of a medical therapy group Metabolic outcomes are independent of weight loss Reduced truncal fat and increased beta cell function Improved insulin sensitivity Reduction / elimination of medications: insulin, oral antihyperglycemics, antihypertensives, statins ALL surgeries have a risk of death Studies show 0.2-2.0% mortality for RYGB <2 deaths per 100 operations The most common causes of death: Pulmonary embolism (blood clot in the lung) Leak in staple lines made during surgery Early complications Nausea / Vomiting Diarrhea / Dumping Heart and lung problems Blood Clots Stricture Blockage Leaks Infection Organ failure Death Later complications Constipation Nutrient deficiencies Protein malnutrition Hair loss Gallbladder disease Mental health problems Higher incidence of post prandial hypoglycemia post bariatric surgery Can occur months to years after surgery Causes related to rapid transit of food between stomach and small intestine Carbohydrates absorbed much quicker producing an acute spike in glucose provoking a strong hyperinsulinemia. Responsive to dietary modification with small frequent low carb meals Some patients require medical therapy such as acarbose to reduce carbohydrate absorption More severe cases require partial pancreatectomy. Lifestyle and weight management • Understanding influences on weight management • Encourage awareness and application of healthy behaviours • Building confidence in managing lifestyle change • Accepting best weight Emotions & Coping Strategies Sleep Biology, hormones + more Medications Weight loss and weight cycling Mental Health Portion Management Understanding nutrients and Inadequacies Disorganized eating Environments: family, work, social Beverage Consumption Planning and Goal Setting Plate method Nutrient Supplements Mindful Eating Physical Activity Balanced plate Balanced plate after bariatric surgery Compromised: food and fluid volumes, nutrient absorption, surface area Risks: nutrient deficiencies, appetite irregularity, disorganized eating, absorption Diet progression • 5 stages • Progress to normal diet Nutrient supplements • Multivitaminmineral • Vit B12, Vit D, Calcium citrate • Others Lifelong lifestyle • Mindful • Coping • Accepting Ideal Body Weight Desired Body Weight Best Weight Weight will continue to change through the course of our life. Bariatric Surgery shows the greatest total weight loss even over years of follow-up. Manage Stress Journaling Problem Solving/Goal Setting Selfmonitoring Mindfulness Motivational Techniques Social support Wadden TA, Foster GD Med Clin North Am 2000: 84(2) 441-461, vii. Review Supported by the Ministry of Health and LongTerm Care and South East Local Health Integration Network Only bariatric assessment service between Ottawa and Toronto Means easier access to care closer to home Committed to providing patient and family centered care for obese and morbidly obese patients Provide pre-surgical assessment and post surgical follow-up services Surgeries performed at Toronto East General Hospital and St. Michael’s Hospital Medical Lead Program Manager 2 Nurse Practitioners 1 Registered Nurse 3 Registered Dietitians (1 FT, 0.8 FT, 0.5 PT) 2 Social Workers 3 Medical Secretaries / Data Coordinators Referral to Bariatric Registry from Family Doctor/Nurse Practitioner Referral received by RATC Package mailed to patient Orientation Session Patient questionnaire returned Patient Questionnaire Initial Assessment Baseline Bloodwork Tests ordered as applicable Deferred from RATC Transfer to surgical site Booked with Dietitian and Social Worker Referred for further medical/psychiatric evaluation Required attendance at orientation session Patient to make informed decision about continuing the process Pre-operatively patients assessed by each member of the team Required to complete tests relevant to their pre-surgical screening Follow-up includes multiple visits with team members starting at 1 week post-operatively Follow-up at 1,3,6,9, and 12 months Support groups offered bi-weekly Annual follow-up for 5 years Glycemic Optimization Clinic: Provides support to pre-op bariatric candidates with elevated blood glucose levels Endocrinologist and CDE support once weekly Surgical/General Medicine Clinic: Dr. Robertson providing consultation to complex bariatric surgical patients once monthly Sleep Apnea Assessment/ Respirology clinic Dr. Aaron Aggarwal providing support for preoperative bariatric patients requiring sleep study assessment Internal Medicine Clinic • Clinics run weekly • Optimize patients’ chronic health conditions Ontario Bariatric Network (OBN) : http://www.ontariobariatricnetwork.ca/ Public Health Agency of Canada (2011). Obesity in Canada. Accessed at https://secure.cihi.ca/free_products/Obesity_in_canada_2011_en.pdf Mechanick et al (2013) Clinical practice guidelines for the Perioperative Nutritional, Metabolic and Nonsurgical support of the bariatric surgical patient. Surgery for Obesity and Related Diseases. 9: 159-191. Isom et al (2014). Nutrition and Metabolic Support Recommendations for the Bariatric Patient. Accessed online at www.ncp.sagepub.com Ontario Bariatric Network www.ontariobariatricnetwork.ca Canadian Obesity Network www.obesitynetwork.ca