* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download The Liver
Survey
Document related concepts
Transcript
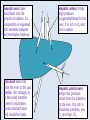
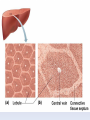
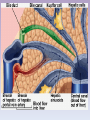
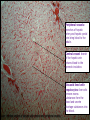
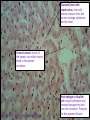
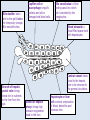
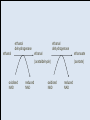
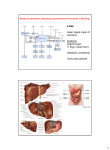
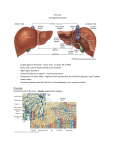
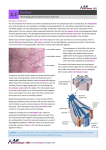
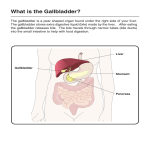
The Liver A2 Biology Liver... • The liver is a large active organ in the abdominal cavity. It has numerous functions, some important ones are: regulation of blood sugar production of and regulation of lipid synthesis of plasma proteins transamination to produce non-essential amino acids – deamination – detoxification – – – – • Before considering the production of urea and detoxification in detail, you need to know a little about the structure and histology of the liver • The liver is found in the upper right of the abdominal cavity, just below the diaphragm. It is made of several lobes and has four connections: – bile duct – hepatic artery – hepatic portal vein – hepatic vein Hepatic vein takes blood back into the general circulation. Its composition is regulated with excesses reduced and shortages made up. Bile duct takes bile from the liver to the gall bladder (for storage) or to the small intestine where it neutralises excess stomach acid and emulsifies lipids. Hepatic artery brings high pressure oxygenated blood to the liver. It is rich in O2 and low in waste. Hepatic portal vein brings low pressure blood from the intestine to the liver. It is rich in dissolved nutrients, low O2 and high CO2. • Liver has four connections: – hepatic artery • brings high pressure oxygenated blood from the aorta. – hepatic portal vein • brings nutrient rich blood from the gut • blood has already passed through the capillaries of the small intestine – at a much lower pressure than the blood of the hepatic artery – partially deoxygenated – hepatic vein • returns blood to the general circulation – bile duct • takes bile from the liver to the gall bladder for temporary storage Histology of the liver... • The liver is made up of 100 000 or so lobules – cylindrical structures – at their centre is a branch of the hepatic vein – at the outside are branches of • the hepatic artery • hepatic portal vein • Blood flows from the outer to the central vessel – through blood-filled channels or sinusoids • lined with liver cells called hepatocytes – hepatocytes regulate the composition of the blood • remove excess substances from the blood and • secrete materials into it which are in short supply or have been made by the liver • Sinusoids are in rows that radiate out from the centre – hepatocytes are only ever one or two cells thick • diffusion path is short. • Bile canaliculi are present – blind-ending channels – also lined by hepatocytes • secrete bile into the channel • flows away from the centre of the lobule to a branch of the bile duct at the periphery. • Sinusoids have large phagocytic Kupffer cells – capture and engulf any bacteria that they encounter • gut contains large numbers of bacteria and could enter the circulation via the hepatic portal vein – also destroy old red blood cells – produce waste bilirubin from haemoglobin • red-brown pigment excreted in bile Peripheral vessels: branches of hepatic artery and hepatic portal vein bring blood to the lobule. Central vessel: branch of the hepatic vein returns blood to the general circulation. Sinusoid lined with hepatocytes: liver cells remove excess substances from the blood and secrete shortage substances into the blood. Liver: injected section of lobules with central and peripheral vessels. Sinusoid lined with hepatocytes: liver cells remove excesses from and secrete shortage substances into the blood. Central vessel: branch of the hepatic vein which returns blood to the general circulation. Liver: detail of central vessel and hepatocytes. Macrophage or Kupffer cell: engulfs pathogens and removes damaged red cells from the circulation. Produces the bile pigment bilirubin. Bile ductile: takes bile to the gall bladder for temporary storage. Bile emulsifies fats. Branch of hepatic portal vein: brings blood rich in nutrients to the liver from the gut. Kupffer cell or macrophage: engulfs bacteria and old or damaged red blood cells. Bile canaliculus: a blind ending canal into which bile is secreted by the hepatocytes. Blood sinusoid: a blood-filled space lined with hepatocytes. Central vessel: takes blood to the hepatic vein to be returned to the general circulation. Branch of hepatic artery: brings high pressure oxygenated blood to the liver. Hepatocyte or liver cell: controls composition of blood, detoxifies and produces bile. Formation of urea by liver... • Excess amino acids cannot be stored in the body – have about the same energy as carbohydrates – extremely wasteful if they were excreted • Instead, they are deaminated by the liver – amino group is removed to produce ammonia – leaves an organic acid • respired or used to make carbohydrates and fats • Ammonia is very soluble and highly toxic – converted to urea via the ornithine cycle • sometimes called the ornithine-citrulline cycle • energy-dependent reactions add it to CO2 to make urea NH2 COOH Amino acid – excess cannot be stored, so it is deaminated in the liver 2NH3 + Ammonia CO2 Carbon dioxide COOH Organic acid – can be respired or converted to lipid and carbohydrate CO(NH2)2 Urea + + NH3 Ammonia – converted to urea for excretion H2O Water NH3 CO2 Ornithine cycle: H2O The ornithine cycle is an energy-consuming process that converts toxic NH3 into urea. In the cycle, TWO molecules of Citrulline Ornithine NH3 NH3 are added to CARBON DIOXIDE to produce urea. Urea is still soluble, but is less Arginine H2O toxic than ammonia. It is secreted into the blood by the HEPATOCYTES (liver cells) and CO(NH2)2 H2O transported to the KIDNEY for excretion. • The resulting urea is excreted – in solution – in urine – via the kidney • Not all animals use urea as their main nitrogenous excretory product – fish and aquatic animals • often use ammonia • can be diluted so not toxic – birds, terrestrial reptiles and insects • often excrete a uric acid paste • to conserve water Role of the liver in detoxification... • The liver detoxifies many substances – For example, alcohol, drugs, antibiotics and hormones – converts them to harmless substances or – excretes them into the bile. • Much of the detoxification takes place on the smooth endoplasmic reticulum in the hepatocytes. Alcohol detoxification... • Alcohol is toxic and is broken down by the liver. – involves the conversion of ethanol into ethanal and – then to ethanoate – ethanoate then enters Krebs cycle to produce energy and ATP • Ethanol contains a lot of energy – can be a significant energy intake for some individuals – pure alcohol contains 29kJ g-1 • Detoxification is summarised on the next slide: ethanol ethanol dehydrogenase ethanal dehydrogenase ethanal (acetaldehyde) oxidised NAD reduced NAD oxidised NAD ethanoate (acetate) reduced NAD Alcohol abuse... • If large quantities of alcohol are consumed on a regular basis, the liver can be damaged • It can cause – fatty liver – hepatitis and – cirrhosis • Explain or comment upon the following observations: Q: The conversion of ethanol to ethanoate needs a supplyoxidised NAD. Other processes also need a supply of NAD, e.g. oxidation of fatty acids. Why does excessive alcohol consumption lead to a condition known as fatty liver? • The supply of available NAD is used for detoxification of the alcohol so it is not available for other aspects of metabolism, including the oxidation of fatty acids. Fatty acids then accumulate. • Also, ethanoate – is fed into Krebs cycle where it is oxidised – less need for oxidation of fatty acids to provide energy – can be used to produce fatty acids The fat that accumulates in ‘fatty liver’ is stored in the hepatocytes. What effect might this have on hepatocyte function? • Fat is stored in droplets – cells swollen – disrupts normal cell functions – particularly intracellular transport • Condition is reversible What is cirrhosis of the liver and what are its effects on liver function? (you might want to consider lobule structure, blood supply, effect on specific aspects of metabolism, e.g. conversion of ammonia to urea and detoxification of hormones) • Hepatocytes damaged and replaced by fibrous, collagen-rich tissue. • Liver cells regenerate – but normal lobule structure lost – poor blood supply to hepatocytes so • Liver function declines – ammonia not converted to urea, so increased toxicity – hormones not detoxified, so effective concentration increases