* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Medicines Optimisation PPT
Survey
Document related concepts
Transcript
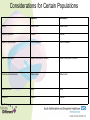
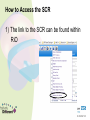
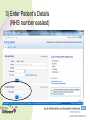
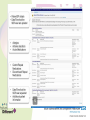
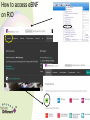
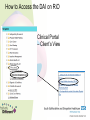
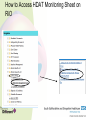
Medicines Optimisation Training Objectives • • • • • • • What is Medicines Optimisation? Nice Guidance MHRA – yellow card reporting Summary Care Records Consultation Skills and Shared Decision Making Hot Topics Patient Group Directions Medicines Code (and related SOPS) • See Medicines Code for further information around Medicines Optimisation and medicine related issues Intranet Staff Policies • Trust formulary: www.sssftformulary.nhs.uk Definition A person-centred approach to safe and effective medicines use to ensure people obtain the best possible outcomes from their medicines Ensuring medicines are: • Clinically appropriate • Safe and effective Goals for the patient: • Improved outcomes • Adherence • Improved medicines safety The RIGHT patients get the RIGHT medication at the RIGHT time at the RIGHT dose and in the RIGHT form Group Work What might you need to consider when choosing a medication for the following: • ‘Average’ patient • Patient of low weight • Woman of child bearing age/Breastfeeding/pregnant woman • Elderly • Child/teenager • Patient with a physical health problem (diabetes, overweight, high blood pressure) NICE GUIDANCE Medicines Optimisation: the safe and effective use of medicines to enable the best possible outcomes Guideline Development Group: • • • • • Nurses Doctors Pharmacists Public involvement Industry Multi Disciplinary Approach • 8 recommendations of which 3 have been identified as priority for implementation 1) Systems for identifying, reporting and learning from medicines-related patient safety incidents How do we do this within our Trust? • Safeguard reporting system • Report on Rio with incident number (serious incidences scan PDF onto RiO) • Helps to improve learning from medicines related patient safety incidents • (Ward pharmacist receives notification can help support any training/learning needs) Adverse Drug Reactions (ADRs) Patient takes a penicillin tablet starts to develop a rash and having trouble breathing dial 999 Patient has an adverse drug reaction Patient is admitted to acute DGH for treatment and returns to ward when better ? Medicines and Healthcare products Regulatory Agency (MHRA) • Regulates medicines, medical devices and blood components for transfusion in the UK • Yellow card scheme – system for recording adverse incidents with medicines and medical devices in the UK • The yellow card scheme is vital in helping the MHRA monitor the safety of all healthcare products in the UK • This ensures that all products are acceptably safe for patients and users When to Report? • For established medicines and vaccines report all serious suspected ADRs (even if the effect is well recognised) • For new medicines and vaccines (▼) – ALL suspected ADRs should be reported How to Report • Through the Yellow Card website (https://yellowcard.mhra.gov.uk) • Send a Yellow Card report by post (download from MHRA website) • By writing to FREEPOST YELLOW CARD • By emailing [email protected] • Phone – 08081003352 (10.00 – 14.00 Mon – Fri only) What to Report • Suspect Drug (route, dose, dates of administration) • Suspect Reaction (what actually happened) • Patient Details (sex, age, patient’s weight, patient initials, local identification number) • Reporter Details • If known – other drugs taken, allergy status and any other relevant information Would you contact the MHRA for the following? a) Oculogyric crisis with haloperidol? b) Pruritus with vortioxetine (▼)? c) Suspected tardive dyskinesia with mirtazapine? 2) Medicines – Related communication systems when patients move from one setting to another 3) Medicines Reconciliation What percentage of patients have an error or unintentional change to their medicines when moving from one care setting to another? Up to 70% How can we, as a Trust, help to reduce this? Summary Care Records • Free (online) access to information about patient’s medication, their allergies and any adverse reactions to medication (24 hours a day, 365 days a year) • Reduces the time, effort and resources needed to obtain patients’ information directly from their GPs • All medical staff, all nurses (including community MH nurses, community LD nurses, children’s nurses, nursery nurses), inpatient admin, community admin, medical secretaries and pharmacy staff now have access to the SCR This is a real step forward for Medicines Reconciliation as it has been shown that using the SCR reduced the time, effort and resources needed to obtain patients’ information directly from their GP with a 45% reduction in phone calls to GP surgeries from the hospital How to Access the SCR 1) The link to the SCR can be found within RiO 2) Click the link 3) Enter Patient’s Details (NHS number easiest) 4) In the Top Right Hand Corner – will confirm if patient has an SCR or not. Click on view SCR Be wary of: • When SCR was last updated • Patients who have not been taking all their medicines when they were at home • ‘Medicines’ that patients don’t consider to be medicines eg OTC/herbal/homeopathic • Any medication that patients may have left at home • Etc! Discharge • Currently discharge summary written by junior doctor and posted to GP • In the future - pharmacy will be ensuring that a copy of the discharge prescription is put in with the discharge medication with a view to the patient taking this to the GP • In the future – a copy of the discharge prescription will be faxed to the GP from the ward • CPN will attend the discharge meeting and will be notified of any changes to medication • When patient obtains their next supply of medication from their GP the CPN will reconcile this supply against the discharge summary 4) Medication Review 5) Self-management plans 6) Patient decision aids used in consultations involving medicines Choice and Medication Website 7) Clinical decision support 8) Medicines – related models of organisational and cross-sector working Making the Patient the Centre of the Consultation and Shared Decision Making Why is it important that we get this right? • Estimated that between 30 -50% medicines prescribed for long term illnesses are not taken as directed • 30-66% non adherence in patients with severe depression • 30 – 65% non adherence in patients with bipolar disorder • 40 – 50% non adherence in patients with schizophrenia • NHS invests and spends a lot of money on medicines • Overall NHS expenditure on medicines in 2013-2014 was £14.4bn • Research has improved our knowledge – but adherence rates do not seemed to have changed over the last 4 decades At any one time what is the cost of medication lying unused around people’s houses: a) £300 million b) £90 million c) £50 million Shared decision-making is an essential part of evidence-based medicine, seeking to use the best available evidence to guide decisions about the care of the individual patient, taking into account their needs, preferences and values Why do you think patients are non adherent with their medicines? What can we do to help support adherence? • Lack of insight • Attitudes towards and previous experiences of medication • Co-morbidity and symptom severity • Level of social and family support • Social isolation • Strength of therapeutic alliance between patient and their doctor (healthcare professional) • Patient feels better • • • • Side effects Insufficient efficacy Drug/alcohol abuse Irregular daily routines (shift work, unemployment) • Dietary/religious (etc) beliefs • Cost of prescription* • Intentional vs non intentional adherence * https://www.gov.uk/get-a-ppc Importance of taking the medicine Concerns • Important that we talk to our patients to understand their beliefs and concerns about their treatment and find out what they wish their medicines to achieve for them Health Coaching Model • Not telling patients how to behave – but helping patients to identify what outcomes they want and what methods for achieving these • Encouraging the patient to be an active participant in their own care 1) Find Out What the Patient knows What do you know? Have you been told about your condition? 2) Find Out about the Patient’s beliefs and concerns What benefit do you think this medicine will give you? What, if anything, are your worries about this medicine? (Use of Drug Attitude Inventory) 3) Ask what the Patient wants the Medicine to Achieve for Them What would you like your medicine to allow you to do? 4) Help the Patient decide whether they want to take their medicine This helps the patient to ‘own’ their decision to take their medicine (rather than us assuming they will) 5) Encourage the Patient to Consider the Practicalities of taking their Medicine Help the patient to plan how to take their medicine every day and how they’ll monitor their own adherence and medicine effectiveness ‘What Matters to You?’ Rather than ‘What is the Matter?’ No Decision About Me Without Me Consultation Skills needed: • • • • • • Welcoming Listening Be aware of body language Reflecting back Appropriate use of questions Empathy • Support a patient in taking responsibility for taking their medicine • Enable a patient to integrate taking a medicine into his/her lifestyle Better Adherence Remember! The Best Outcomes in many conditions are from a combination of : • Self-help Risk reduction, self-management • Help from others Support, psychotherapy, education • Medication To control symptoms Self-help Help from others Medication 3 supports – fairly stable with care 2 supports – can be done but one wobble and you could be struggling 1 support – can be done with a lot of hard work but one wobble and you could be really struggling Hot Topics • eBNF, Drug Attitude Inventory, High Dose Antipsychotics and Formulary • Drug Driving Rules • Sleep (Hypnotic Prescribing Guidelines) • Physical Health • Smoking and Medication • Sodium Valproate • CQC How to access eBNF on RiO How to Access the DAI on RiO Clinical Portal – Client’s View How to Access HDAT Monitoring Sheet on RiO How to Access the Formulary on RiO New Drug Driving Rules • From 2/3/15 new law introduced around driving after taking certain drugs in England and Wales • It is (already) an offence to drive whilst impaired due to illegal or legal drugs (section 4 of RTA 1988) • This new law refers to driving, attempting to drive or being in charge of a vehicle with a specified controlled drug in the body in excess of a specified limit These ‘specified controlled drugs’ can be (broadly) split into 2 groups First Group • ‘Zero tolerance’ group • Consists of commonly abused drugs • Low limits have been set • • • • • • • Cannabis (THC) MDMA (ecstasy) Ketamine Methylamphetamine Cocaine LSD Heroin/diamorphine Second Group • Mainly licensed medicines that have a high potential to be abused. • Specified limits have been set at a higher level than the first group • This means that people taking the medication within the therapeutic range are unlikely to test positive • Morphine, other opiate/opioid based medication (eg codeine, tramadol or fentanyl) • Diazepam, clonazepam, flunitrazepam, lorazepam, oxazepam, temazepam (medication used to treat anxiety or sleep disorder) • Methadone • Amphetamine • Roadside drug screening devices to be developed that will use saliva to identify if the person driving has taken a listed drug (or one that may be metabolised into one of these drugs) • Following a positive screening result the person can be requested to provide a blood sample (for evidential purposes) to enable prosecution ‘Statutory Medical Defence’ (For people who test positive) Entitled to raise ‘statutory medical defence’ if: • The drug was lawfully prescribed, supplied, or purchased over-the-counter, for medical or dental purposes; and • The drug was taken in accordance with advice given by the person who prescribed or supplied the drug, and in accordance with any accompanying written instructions (so far as the latter are consistent with any advice of the prescriber) Notes • May be helpful to advise patients to keep some evidence on themselves when driving to be able to prove that they are legally taking the medication • If police are satisfied that the driver is taking the medicine on appropriate advice then will not prosecute NB • It remains the responsibility of the driver to consider whether they think their driving is, or might be, impaired (eg by feeling sleepy) • It will still remain an offence to drive if driving is impaired by drugs Responsibilities Patient: • To decide whether they consider their driving is impaired Prescriber: • To provide patients with advice/information around medications that may cause drowsiness and thus might impair driving https://www.gov.uk/drug-driving-law Sleep What can help to ensure a restful night’s sleep? Sleep Hygiene • Establish a regular routine eg getting up at the same time each day • Say ‘no’ to naps • Daily exercise (but nb! Not within 4 hours before going to bed) • Don’t drink tea/coffee within 4 hours of going to bed • Avoid alcohol and smoking – both are stimulants (? Avoid smoking within 6 hours of going to bed) • Comfort (bedroom not too hot or cold) • Avoid using televisions or computer monitors prior to sleep • Don’t eat a big meal or spicy foods just before bedtime • Aromatherapy • Use anxiety management/relaxation techniques • Go to bed to sleep • Etc If all else fails …get up and go and do something else in another room Insomnia – facts and figures • Sleep is a vital biological process • People with insomnia have been shown to have higher rates of mental health problems, drug and alcohol abuse, cardiac morbidity, healthcare utilisation and to be at increased risk of accidents and overall mortality • Remember there is a variation in people’s sleep patterns • Quality of sleep important – not actual time spent sleeping Non – Pharmacology Strategies • Should be discussed first • Psychological therapies more effective in the long term compared to hypnotic medication alone • Cause of insomnia should be determined (and treated) Medications that can cause Sleep Disturbance • Antidepressants (SSRIs, venlafaxine, bupropion, duloxetine and MAOIs) • Antiepileptics (lamotrigine and phenytoin) • Antihypertensives (beta blockers, calcium channel blockers) • Antipsychotics (aripiprazole, flupentixol) • Hormones (corticosteroids, thyroid hormones) • NSAIDs • Stimulants: (methylphenidate, modafinil) • Sympathomimetics: (salbutamol, salmeterol, theophylline, pseudoephedrine) • Others: (baclofen, trihexyphenidyl, dantrolene, antimuscarinics, tizanidine) When Should the Use of Hypnotics be considered and what precautions are necessary when using them? Hypnotics • Management of severe insomnia interfering with normal daily life • Short periods of time (4 weeks usually including any tapering off) • Long term prescribing = off license • Reason must be documented in patient’s progress notes (if prescribing more than 4 weeks) • First choice (within SSSFT) is zopiclone • Second choice is temazepam • It is recommended that switching from one hypnotic should only occur if a patient experiences adverse effects • Use of sedating antihistamines, antidepressants and antipsychotics not recommended Considerations for Certain Populations Zopiclone Temazepam Elderly Reduce dose Reduce dose Respiratory disease Caution Caution Respiratory depression Contra-indicated Contra-indicated Hepatic impairment Reduce dose (avoid if severe) Reduce dose (avoid if severe) Renal impairment (severe) Reduce dose Reduce dose Addiction Prone Avoid Avoid Clozapine Caution Caution Administration • Should not be routinely offered (if on PRN) • Only offer if attempts have been made to relax and sleep • Should only be administered after 11pm • Avoid giving in early hours of the morning – ‘hangover effect’ patient may not get up and engage in therapeutic activities Do we (as a Trust) do this? We should NEVER develop a newly dependent patient by virtue of a hospital admission Physical Health • Why the concern? • People with a serious mental health illness die an average of 15-20 years earlier than the rest of the population • People with a serious mental illness at increased risk of a range of physical illnesses/conditions – respiratory disease, coronary heart disease, diabetes, high blood pressure, stroke (etc) • Mental Health Taskforce – ‘The Five Year Forward View for Mental Health’ February 2016 • The Kings Fund – ‘Bringing together Physical and Mental Health’ March 2016 • New models of care • Integrated approach • Reduced life expectancy among people with severe mental health illness largely attributable to poor physical health • Many contributing factors – one of them being medication • Champion for physical health in mental health services and vice versa Smoking and Medication • Cigarette smoking can interact with some medications • Polycyclic aromatic hydrocarbons in cigarette smoke that stimulate production of enzymes which results in some medications being metabolised faster • As majority of interactions are not due to the nicotine (in cigarettes) this problem does not occur when using NRT • Beware if a patient stops/starts smoking Physical Health Medication • • • • Warfarin Theophylline Insulin ? Beta blockers Psychotropic Medication • • • • • • • • Chlorpromazine Clozapine Olanzapine Haloperidol Fluphenazine Duloxetine Fluvoxamine Methadone Valproate • Sodium valproate and valproic acid (epilepsy) • Semi sodium valproate (mood stabiliser) Known to cause teratogenic side effects: Increased risk of congenital malformation • Woman not on valproate • Woman on valproate Developmental Disorders • Exposure to valproate in utero can have an adverse effect on mental and physical development • Up to 30-40% experience delays in their early development such as talking and walking later, lower intellectual abilities, poor language skills (speaking and understanding) and memory problems Toolkit • February 2016 – launch of a new ‘toolkit’ to ensure female patients are better informed about the risks of taking valproate medicines during pregnancy. https://www.gov.uk/government/publications/ toolkit-on-the-risks-of-valproate-medicinesin-female-patients Checklist and important discussion points for prescribers and patients Credit card sized information leaflet Patient booklet Healthcare professional booklet Need to consider: • Risk vs benefit • Pregnant – planned? - unplanned? • Child bearing age/not of child bearing age? • (Use of reliable contraception if the woman is of childbearing age) CQC • Omitted/Delayed Doses • RT • Lithium red top alert (9/8/16) – poor blood test monitoring in relation to lithium management E-Learning Module In order to obtain the Medicines Optimisation Competency an e-learning module on Medicines Management also needs to be undertaken This can be accessed via: [email protected] (Any problems contact Sharon Dennison) Patient Group Directions PGDs Patient Group Directions (PGDs) • A PGD is a written instruction for the supply and/or administration of a named licensed medication for a defined medical condition to a group of patients that fit the criteria laid out in the PGD. • It allows specified healthcare professionals to supply and/or administer medicine directly to a patient without the patient needing to see a prescriber. • Important to remember that it is a ‘direction’ – by writing a PGD you are not prescribing What Do I need to Do to be able to use a PGD to Administer Medication? • Complete the PGD part of the Medicines Optimisation Training initially on starting with the Trust and then on a 3 yearly basis • Work through and complete the PGD Resource pack • Once completed contact your line manager (who will assess you to confirm competency) • Line manager should then assess nursing staff yearly (? At annual appraisal) to ensure continual competence Complete the front page of each PGD that you are able to use The original will be kept in the PGD folder on the ward A photocopy will be kept in your personnel file N.B. PGDs vary between clinical settings. • Check trust website • • • • • • Nurses (Inpatients) Nurses (Inpatients, specific areas (EDU) Nurses (Crisis Team) Nurses (Sub Misuse) Nurses (GUM) Nurses (Outpatient specific areas eg Drug and Alcohol) Etc! When to Use a PGD For short term conditions e.g • Short term pain relief • Short term relief of constipation • Short term relief of indigestion • Short term relief of anxiety or agitation When should a PGD NOT be Used • PGDs are NOT suitable for chronic disease management (Long term pain management, long term insomnia, long term anxiety etc) • PGDs cannot be used to alter a prescribed dose • PGDs cannot cover repeat prescribing • If any of the exclusion criteria in the PGD are fulfilled then that PGD cannot be used and a prescriber must be consulted (and if necessary come out and prescribe the medication) • Staff employed directly by SSSFT can use PGDS. (If you are doing a bank shift on another ward as long as you are signed off for a PGD on your base ward then you can also write that same PGD on a different ward) • Staff who are NOT directly employed by SSSFT must not write PGDs How To Use a PGD to Administer Medication Inpatient • Peptac • Nurse who writes the PGD should also administer the first dose • Any subsequent doses that are administer can only be done by PGD trained nursing staff • Need to document on RiO that the patient has had a medication using a PGD for a certain condition and document the PGD number Community • Different paper work • Crisis one book for supplying and one book for administering (controlled drug book) • Amounts are tallied each time a PGD is administered This presentation only gives an overview Healthcare Professionals need to familiarise themselves with the Competency Based Assessment (which is adapted from the National Prescribing Centre) and the framework within this. There should be a PGD Learning Resource Pack on each ward. Thanks for listening Any Questions?